Bone Cancer: Symptoms, Causes & Treatment
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. Ramesh Parimi, Senior Consultant – Surgical Oncology, Specialist in Cancer Surgery
Bone cancer definition
Bone cancer refers to a rare type of cancer in which abnormal cells grow uncontrollably in the bones, forming malignant tumors. It is also called osseous cancer. These tumors can weaken the bones, cause pain, and may spread to other parts of the body.
Bone cancer is associated with symptoms like persistent bone pain, swelling, fractures, weight loss, tiredness, and reduced mobility. It generally develops due to genetic factors, prior exposure to radiation, or as a secondary cancer that spreads from other organs. Although bone cancer is a serious condition, various treatments such as surgery, radiation therapy, chemotherapy, and targeted therapy can help manage the disease. Treatment helps to relieve symptoms, slow cancer progression, and improve patient outcomes.
Diagnosis and treatment are managed by an
oncologist or orthopaedic oncologist. Imaging studies, biopsies, and laboratory tests are used to determine the type, location, and extent of the cancer.
Bone cancer meaning
Bone cancer is medically referred to as “osseous cancer”. The term osseous comes from the Latin word osseus, meaning “made of bone” or “bony.” The word cancer originates from the Latin cancer, meaning “crab,” a term used by early physicians because the swollen veins surrounding tumors resembled a crab’s legs. Thus, bone cancer literally refers to a malignant tumor arising from bone tissue.
Bone Cancer Statistics
Bone cancer statistics in the world
Primary bone malignancies are extremely rare, estimates around approximately 0.2% of all cancers worldwide. The main types include osteosarcoma, chondrosarcoma, and Ewing sarcoma. The global yearly incidence is less than one case per 100,000 people. In 2021, more than 600,000 persons worldwide were diagnosed with malignant bone and articular cartilage cancer. In the United States, the incidence is roughly one per 100,000 people per year, with 3,700-3,800 new cases reported each year and a lifetime risk of about 0.1%. Secondary (metastatic) bone malignancies are much more prevalent and are reported separately.
Bone cancer statistics in India
Primary bone cancers are rare in India, accounting for approximately 0.5–1% of all registered malignancies, according to data from the National Cancer Registry Programme (NCRP). Ewing sarcoma accounts for 15-25% of all primary bone sarcomas in children and adolescents, and it is more common among Indian and Asian populations than in Western countries.The age-standardized incidence rate of primary bone cancer is very low, typically 0.1–0.3 cases per lakh population per year with a peak incidence in the 10–19-year age group.
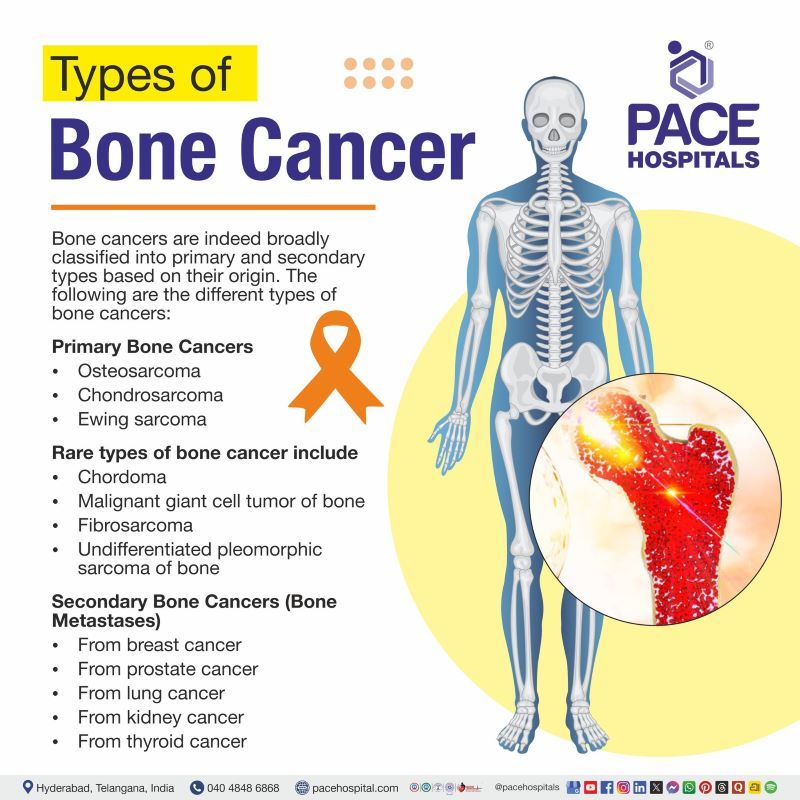
Types of Bone Cancer
Bone cancers are indeed broadly classified into primary and secondary types based on their origin. Primary bone cancers originate directly in the bone tissue itself, such as osteosarcoma or chondrosarcoma, while secondary bone cancers, which are more common, result from metastasis to the bone from primary cancers arising in other organs, such as breast, prostate, or lung.
The following are the different types of bone cancers:
Primary Bone Cancers
- Osteosarcoma
- Chondrosarcoma
- Ewing sarcoma
- Chordoma
- Malignant giant cell tumor of bone
- Fibrosarcoma
- Undifferentiated pleomorphic sarcoma of bone
Secondary Bone Cancers (Bone Metastases)
- From breast cancer
- From prostate cancer
- From lung cancer
- From kidney cancer
- From thyroid cancer
Primary Bone Cancers
- Osteosarcoma: The most common primary bone malignancy, arising from bone-forming cells. It typically affects children and adolescents, often around the long bones near the knees, and is highly aggressive with a tendency to metastasize to the lungs.
- Chondrosarcoma: It is a malignant tumor that originates from cartilage-producing cells, usually seen in adults. It commonly affects the pelvis, femur, and shoulder girdle and is often resistant to chemotherapy and radiotherapy.
- Ewing sarcoma: It is a highly aggressive malignant tumor mostly affecting children and young adults. It usually arises in the diaphysis of long bones or the pelvis and may extend into soft tissue, with a high risk of metastasis.
- Chordoma: A rare, slow-growing tumor derived from notochord remnants, usually occurring in the sacrum or skull base. It can be locally destructive and difficult to fully remove surgically.
- Malignant giant cell tumor of bone: Malignant giant cell tumour of bone is a rare and aggressive type of giant cell tumour. It can occur on its own or as a result of the malignant transformation of a previously benign tumor. It usually affects the ends of long bones in young people and has the potential to metastasis.
- Fibrosarcoma: A malignant tumor originating from fibrous connective tissue in bone. It is rare, usually occurs in adults, and can be locally aggressive with potential for metastasis.
- Undifferentiated pleomorphic sarcoma of bone: A rare, high-grade malignant tumor lacking specific differentiation. It mostly affects adults and can grow rapidly, and cause aggressive invasion of surrounding bone and soft tissue.
Secondary Bone Cancers (Bone Metastases)
- Breast cancer: It is a leading cause of bone metastases, frequently producing osteolytic or mixed lesions, commonly affecting the pelvis, spine and ribs, causing pain, fractures and other skeletal complications.
- Prostate cancer: Prostate cancer frequently spreads to bone, usually producing osteoblastic (bone-forming) lesions, commonly in the spine and pelvis, contributing to skeletal morbidity.
- Lung cancer: Lung cancer often metastasizes to bone, especially in the advanced stages of the disease. It usually causes osteolytic lesions in the spine, ribs, pelvis, and long bones like the femur, which raises the risk of pathological fractures.
- Kidney cancer: Renal cell carcinoma frequently develops aggressive osteolytic bone metastases, which are usually painful and can affect the spine and long bones. These lesions are connected with a higher risk of fracture and hemorrhage.
- Thyroid cancer: Less common, but advanced thyroid cancers, especially follicular types, can spread to bone, forming osteolytic lesions, usually in the spine and long bones.
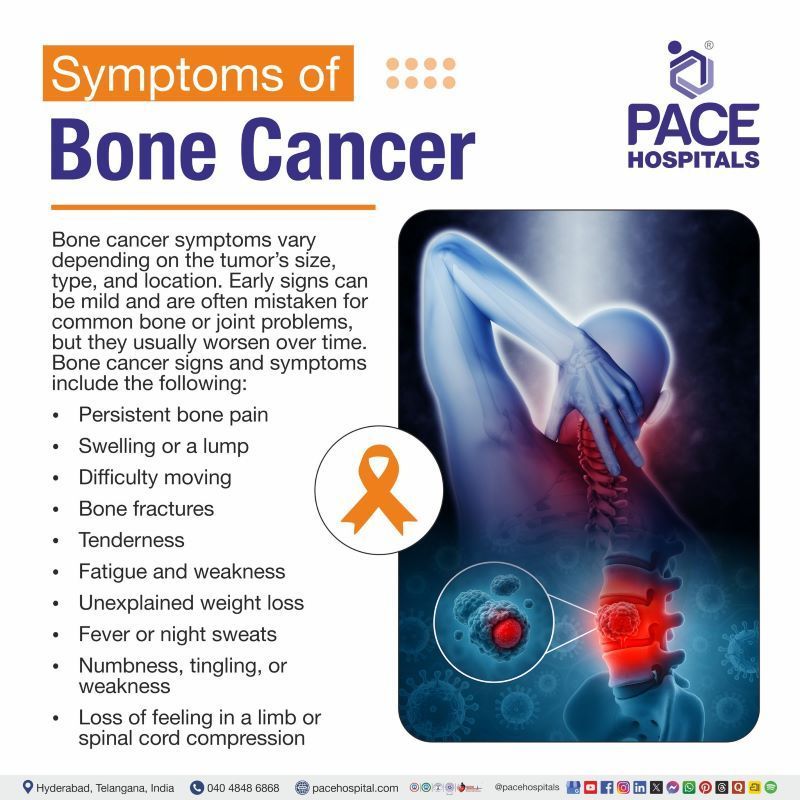
Bone Cancer Symptoms
Bone cancer symptoms vary depending on the tumor’s size, type, and location. Early signs can be mild and are often mistaken for common bone or joint problems, but they usually worsen over time. Bone cancer signs and symptoms include the following:
- Persistent bone pain
- Swelling or a lump
- Difficulty moving
- Bone fractures
- Tenderness
- Fatigue and weakness
- Unexplained weight loss
- Fever or night sweats
- Numbness, tingling, or weakness
- Loss of feeling in a limb or spinal cord compression
Note: Not everyone with these symptoms has bone cancer, but persistent or unexplained symptoms need to be checked by a doctor.
Persistent bone pain: This is the most common symptom. The pain may start mildly and come and go, but it usually becomes constant over time and may worsen at night or during physical activity.
Swelling or a lump: Swelling or a noticeable lump may develop near the affected bone or joint. This usually appears after pain has started and may feel firm or tender to the touch.
Difficulty moving: If the cancer is present near a joint, it can cause stiffness and restrict movement. This may lead to limping or reduced use of the affected limb.
Bone fractures: Bone cancer can weaken the bone structure, making it more likely to break with minor injury or normal activity. Such fractures may occur suddenly after months of pain.
Tenderness: The affected area may feel sore or painful when touched due to inflammation or tumor growth within the bone.
Fatigue and weakness: Cancer can cause ongoing tiredness and weakness that does not improve with rest. This happens because the body uses extra energy to fight against the disease.
Unexplained weight loss: Cancer can alter the body's metabolism, result into weight loss even without any alterations in diet or physical activity.
Fever or night sweats: Some people may experience low-grade fever or excessive sweating at night as a response to cancer-related inflammation.
Numbness, tingling, or weakness: Tumors near nerves, especially in the spine, can press on them, leading to altered sensation or muscle weakness.
Loss of feeling in a limb or spinal cord compression: Advanced tumors in the spine may compress the spinal cord, leading to loss of sensation, weakness, or problems with movement and coordination.

Bone Cancer Causes
The exact cause of bone cancer remains largely unknown and is believed to be multifactorial. Several genetic, environmental, and clinical factors are thought to contribute to malignant transformation of bone tissue.
The following are the causes of bone cancer:
- Genetic mutations
- Inherited genetic factors
- Environmental factors
Genetic mutations: Genetic mutations are changes in genes that control cell proliferation, division, and DNA repair. When these genes are changed, normal bone, cartilage, or musculoskeletal cells may proliferate uncontrolled, resulting in cancer.
Inherited genetic factors: Some individuals inherit genetic mutations that increase their risk of developing bone cancer. These inherited conditions are rare but significantly raise susceptibility to certain types of bone tumors. It includes Li-Fraumeni syndrome, hereditary retinoblastoma, and Rothmund-Thomson syndrome.
Environmental factors: Environmental exposures can increase the risk of bone cancer. The most well-established factor is high-dose ionizing radiation, especially during childhood. Bone cancer may develop years after radiation exposure.

Bone Cancer Risk Factors
Risk factors for bone cancer are conditions that raise a person's chance of developing the disease. Some factors, such as genetics and age, cannot be changed, while others, like previous radiation exposure, can potentially be treated or avoided. Risk factors of bone cancer include:
- Genetic factors
- Previous radiation exposure
- Bone disorders
- Age
- Rapid bone growth
- Family history
- Gender
Genetic factors: Certain inherited conditions like Li-Fraumeni syndrome or hereditary retinoblastoma, increase the risk of developing bone cancer. These genetic mutations can disrupt normal cell growth and repair in bones. As a result, affected individuals have a higher chance of malignant bone changes.
Previous radiation exposure: Exposure to high-dose radiation, especially during childhood, can damage bone cells and increase the risk of cancer later in life. The risk is greater when radiation is applied near growing bones or given repeatedly. This exposure can trigger abnormal cell growth and malignancy over time.
Bone disorders: Bone conditions like Paget's disease of bone or fibrous dysplasia result in abnormal bone growth, making bones more susceptible to cancer. Chronic changes in bone structure and cell turnover can create an environment favourable for malignancy. Individuals with these disorders are at increased long-term risk.
Age: The risk of bone cancer varies with age. Osteosarcoma is most common in children and adolescents, while chondrosarcoma occurs more often in adults over 40 years of age. These age-related patterns reflect variations in bone growth and cellular activity over time.
Rapid bone growth: Periods of fast bone growth, such as during puberty, are associated with an increased risk of abnormal changes in bone cells. Rapid cell division can make DNA errors more likely. These errors may accumulate, raising the chance of cancerous transformation.
Family history: A family history of hereditary cancer syndromes or bone cancer increases the risk of developing the disease. This risk is influenced by both shared genetics and environmental factors. Individuals with impacted relatives should be especially concerned about bone health.
Gender: Males have a slightly higher risk of developing bone cancer compared to females. Hormonal differences and patterns of bone growth may partly explain this. This makes monitoring and awareness particularly important in males.
Complications of Bone Cancer
Bone cancer can cause substantial local and systemic complications arising from tumor growth, osteolysis (bone destruction), and effects on surrounding tissues. These complications frequently impair mobility, cause severe symptoms, and adversely affect prognosis. The complications include:
- Pathological fractures
- Tumor recurrence
- Distant metastasis
- Pain and functional impairment
- Treatment-related complications
Pathological fractures: Cancer weakens the structural integrity of bones, making them more prone to fractures even with minor injury. These fractures commonly occur in the spine, pelvis, femur, or upper limbs. Pathogenic fractures restrict movement, cause sharp pain, and usually need surgery to stabilise.
Tumor recurrence: Despite adequate treatment, such as surgery, chemotherapy, or radiotherapy, bone tumors can recur at the original site. Local recurrence frequently needs more intensive therapy, increases morbidity, and is related to a lower long-term survival.
Distant Metastasis: Certain bone cancers, like osteosarcoma and Ewing sarcoma spread to the lungs or other organs. Metastasis significantly worsens the prognosis and complicates treatment planning.
Pain and functional impairment: Long-term pain is caused by tumor-related bone destruction, joint involvement, and nerve compression. This can impair limb function, limit normal tasks, and lower overall quality of life.
Treatment-related complications: Therapies used to treat bone cancer may produce complications. Surgical operations can result in infection, delayed wound or bone healing, limb length discrepancy, or loss of function. Systemic side effects of chemotherapy and radiotherapy include tiredness, immunosuppression, and damage to adjacent healthy tissues, all of which can have an impact on recovery and long-term outcomes.
Bone Cancer Diagnosis
Bone cancer diagnosis is primarily based on clinical evaluation, including medical history and physical examination, to assess bone involvement and related features. Below are the steps involved in the diagnosis of bone cancer:
- Medical history
- Physical examination
- Laboratory Tests
- Blood tests
- Complete blood count (CBC)
- Alkaline phosphatase (ALP)
- Serum calcium
- Other relevant markers
- Imaging Tests
- X-ray (initial investigation)
- Computed tomography (CT) scan
- Magnetic resonance imaging (MRI)
- Bone scan (radionuclide scintigraphy)
- Positron emission tomography (PET) scan
- Ultrasound (USG)
- Biopsy
- Needle biopsy
- Core needle biopsy
- Fine-needle aspiration
- Open (surgical) biopsy
- Staging Tests
- CT scan of the chest (lung metastases)
- PET scan or bone scan (distant spread)
- MRI for local staging
Bone Cancer Treatment
Bone cancer treatment involves a combination of approaches to control the tumor, relieve symptoms, and improve quality of life. The following are the bone cancer treatment options:
- Non-pharmacological management
- Physical rehabilitation
- Palliative care
- Supportive care (nutritional and psychological support)
- Lifestyle modifications, exercise, and physiotherapy
- Pharmacological management
- Chemotherapy
- Targeted therapy/ immunotherapy
- Radiation therapy
- Pain and symptom management (analgesics, bone-modifying agents)
- Anti-inflammatory drugs and other adjunct medications
- Surgical management
- Limb-salvage surgery
- Amputation
- Bone reconstruction (grafts, endoprosthesis)
- Metastasis resection and diagnostic biopsy procedures
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support
Bone Cancer Prevention
While most bone cancers cannot be completely prevented, certain measures may help reduce the risk and promote early detection. The following are the preventive measures for bone cancer:
- Avoid unnecessary radiation exposure
- Manage underlying bone disorders
- Genetic counseling
- Healthy lifestyle choices
- Early detection of symptoms
- Regular follow-up for high-risk groups
Avoid unnecessary radiation exposure: High doses of radiation, especially during childhood, can increase the risk of developing bone cancer. Limiting exposure to X-rays, CT scans, and radiation therapy unless medically necessary can help reduce this risk.
Manage underlying bone disorders: Conditions like Paget's disease of bone or fibrous dysplasia may increase the likelihood of developing bone cancer. Regular monitoring and proper medical management of these disorders can help lower the risk.
Genetic counseling: Individuals with inherited cancer syndromes, such as Li-Fraumeni syndrome or hereditary retinoblastoma, have a higher risk of bone cancer. Genetic counseling can provide guidance on risk assessment and early monitoring.
Healthy lifestyle choices: Maintaining a balanced diet, regular physical activity, and avoiding carcinogens like tobacco and excessive alcohol can improve overall bone health and decrease cancer risk.
Early detection of symptoms: Being alert to ongoing bone pain, swelling, or unexplained fractures can help in identifying the condition at an earlier stage. Early diagnosis allows timely treatment, improves outcomes, and may help prevent further cancer progression.
Regular follow-up for high-risk groups: People with rare genetic disorders, significant family history, or a history of therapeutic radiation should have planned clinical follow-up, which may include periodic assessments to detect early changes suggestive of malignancy and allow earlier intervention.
Difference between Bone Cancer and Arthritis
Bone cancer and arthritis are distinct conditions affecting bones and joints, with different causes, symptoms, and treatments. Bone cancer is a malignant tumor that spreads, whereas arthritis is joint inflammation that primarily impairs function and quality of life. The table below highlights the key differences between bone cancer and arthritis:
| Feature | Bone Cancer | Arthritis |
|---|---|---|
| Nature | Malignant tumor originating from bone tissue. It involves the uncontrolled growth of abnormal bone cells that can destroy healthy bone. | Chronic or long-term inflammation of the joints, affecting cartilage, synovium, and surrounding tissues. Non-cancerous, but it can cause permanent joint damage. |
| Symptoms | Persistent bone pain, swelling, lumps or masses, fractures, fatigue, and sometimes fever. Pain may worsen at night and not improve with rest. | Joint pain, stiffness (morning time), swelling, redness, warmth, and reduced range of motion. Pain may improve with rest in osteoarthritis but persists in inflammatory types. |
| Progression | Can grow rapidly, invade surrounding tissues, and metastasize to distant organs like lungs or liver. Advanced stages may cause systemic symptoms such as weight loss or anemia. | It normally advances slowly, mostly impacting joint function. Inflammatory arthritis can flare up, but it rarely spreads outside of the joints. |
| Diagnosis | Requires imaging studies (X-ray, MRI, CT, bone scan) and is confirmed by biopsy. Lab tests may help detect tumor markers or monitor treatment. | Diagnosed through clinical evaluation, blood tests for inflammation or autoantibodies, and imaging studies to assess joint damage. |
| Treatment | Treatment options include surgery, chemotherapy, targeted therapy, immunotherapy and supportive care. Treatment varies according to type, stage, and location. | Medications (NSAIDs, DMARDs, biologics), physical therapy, lifestyle changes, and joint replacement surgery in severe cases. Management is aimed at reducing pain and preserving function. |
Frequently Asked Questions (FAQs) on Bone Cancer
What is bone cancer?
Bone cancer is a malignant tumor that develops in the bone tissue. It can be primary, starting in the bone itself, or secondary (metastatic), spreading to the bone from other parts of the body. The most common primary bone cancers are osteosarcoma, chondrosarcoma, and Ewing sarcoma. Although rare, bone cancer can cause persistent bone pain, swelling, tenderness, fractures with minor injury, and reduced mobility. Early detection and prompt treatment are necessary to prevent complications.
Is bone cancer curable?
Bone cancer is curable in some circumstances. If diagnosed early, osteosarcoma and Ewing sarcoma can be treated with surgery and chemotherapy. Low-grade chondrosarcoma can be cured if the tumor is totally excised after surgery. Advanced or metastatic bone tumors, on the other hand, are typically incurable, with treatment focusing on disease control, symptom management, and quality of life. Early diagnosis and coordinated care are important for attaining the best potential results.
Can bone marrow edema be cancer?
Bone marrow edema is not a type of cancer; it shows excess fluid within the bone marrow visible on MRI, which is commonly caused by trauma, arthritis, or inflammation. In rare cases, edema can accompany tumors or bone cancers, but the edema is a sign of an underlying condition rather than cancer. A complete clinical evaluation is needed to rule out serious causes.
What causes bone cancer?
The exact cause of most primary bone cancers is unknown. Still, risk factors include genetic predispositions like Li Fraumeni and retinoblastoma syndromes, prior high-dose radiation, and certain benign bone conditions. These factors may disrupt normal cell regulation and lead to malignant transformation of bone cells.
How to avoid bone cancer?
There is no guaranteed way to prevent bone cancer due to its often idiopathic nature. Minimising unnecessary radiation exposure, monitoring existing bone disorders, and providing genetic counselling for high-risk individuals may help reduce risk. Maintaining overall bone health and reporting persistent bone symptoms early can aid in earlier diagnosis.
Is bone cancer genetic?
Some bone cancers are associated with inherited genetic syndromes like Li Fraumeni and hereditary retinoblastoma, which involve mutations in tumor suppressor genes. These conditions increase susceptibility, but most bone cancers occur sporadically without a clear hereditary pattern.
How does bone cancer occur?
Bone cancer occurs when normal bone cells undergo changes that make them grow uncontrollably. These cancerous cells form a tumor that can damage nearby bone and sometimes spread to other parts of the body. Early detection and treatment are very important.
What are the symptoms of bone marrow cancer?
Bone marrow cancers such as multiple myeloma can cause bone pain, anemia, and increased susceptibility to fractures, hypercalcemia, and impaired renal function. Systemic symptoms such as unexplained weight loss and frequent infections, as malignant cells disrupt normal marrow function.
Is bone cancer common?
No, primary bone cancers are very rare, accounting for less than about 0.2% of all malignancies worldwide. They are far less common than secondary (metastatic) bone involvement from cancers of the breast, prostate, or lung.
Is bone cancer dangerous?
Bone cancer can be severe and life-threatening, particularly if it has spread (metastasised) beyond the bone. It can damage bone structure, lead to pathological fractures, and compromise organ function. Early intervention improves outcomes, but severe disease frequently necessitates intensive treatments.
Can a bone cyst be cancerous?
Most bone cysts are benign and not cancerous, but certain cysts or lesions can transform into malignant tumors in rare cases. Imaging and biopsy are needed to distinguish benign cysts from malignant bone lesions.
Where does bone cancer usually start?
Primary bone tumors usually develop in the long bones of the arms and legs, specifically around growth plates such as the distal femur, proximal tibia, and proximal humerus. Different subtypes have a preference for specific bone areas.
How fast does bone cancer spread?
The rate of spread depends on the cancer type and aggressiveness, some, such as Ewing sarcoma, can grow rapidly, while others may be slower. Metastatic spread, particularly to lungs or other bones, worsens prognosis and may occur earlier in more aggressive forms.
When to consult a doctor for bone cancer?
Consult a doctor for bone cancer if bone pain, inflammation, or lumps persists for few weeks, worsens over time, or affect with daily activities. Signs that need attention include:
- Persistent or worsening bone pain at night
- Swelling or a noticeable lump over a bone
- Unexplained fractures even from minor injuries
- Tiredness, fever, or unexplained weight loss
- Reduced movement or difficulty using a limb
If these symptoms continues, it is important to consult an orthopedic oncologist, general care physician, or oncologist who can evaluate the cause and recommend the proper diagnostic tests and treatment plan. Seek emergency medical attention if there is sudden severe pain, numbness, weakness, or loss of function in a limb, which could suggest rapid tumor growth or nerve compression. An orthopedic oncologist, general physician, or oncologist can provide the best bone cancer treatment to control the disease and prevent complications.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868