Vasculitis: Symptoms, Causes & Treatment
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. Shweta Bhardwaj - Consultant Rheumatologist and Clinical Immunologist
Overview | Prevalence | Types | Symptoms | Causes | Risk Factors | Complications | Diagnosis | Treatment | Prevention | Vasculitis vs Vasculopathy | FAQs | When to consult a Doctor
Vasculitis definition
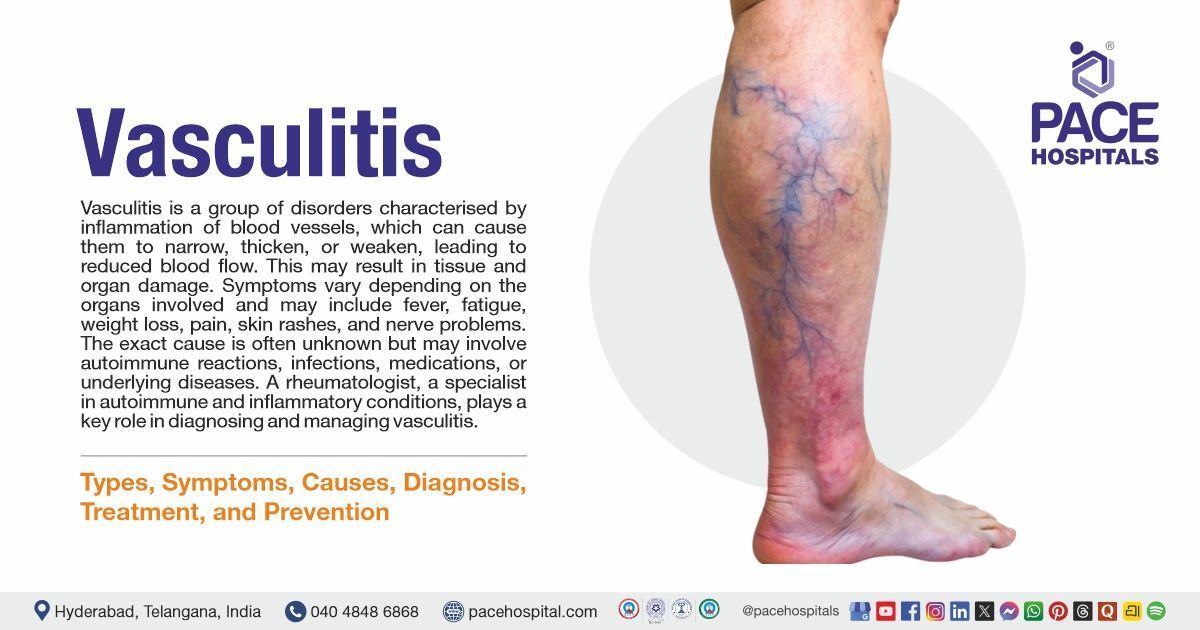
Vasculitis is a group of disorders in which blood vessels become inflamed, leading to thickening, weakening, narrowing, or scarring of their walls. This inflammation reduces blood flow and can damage vital organs and tissues. The condition may affect arteries, veins, or capillaries of any size, leading to symptoms such as fever, fatigue, weight loss, muscle or joint pain, skin rashes, and nerve problems.
The cause of vasculitis is often unknown, but it may occur due to autoimmune reactions, infections, certain medications, or cancers. In some cases, it develops secondary to other autoimmune diseases like rheumatoid arthritis or lupus. Complications may depend on which organs are affected and can include organ failure, stroke, alveolar haemorrhage, aneurysms, or tissue death due to poor blood supply.
A
rheumatologist, a doctor specialised in autoimmune and inflammatory diseases, can accurately diagnose and provide the correct treatment for vasculitis.
Vasculitis meaning
The word vasculitis is derived from Latin and Greek.
- “Vasculum,” meaning small vessel or blood vessel
- “-itis,” which means inflammation.
Therefore, vasculitis literally means “inflammation of the blood vessels.”
Vasculitis Prevalence
Vasculitis prevalence Worldwide
Vasculitis as a group affects approximately 3.8–4.0 per lakh persons worldwide, with individual vasculitides remaining rare. Prevalence rates vary by subtype and region, for example, antineutrophil cytoplasmic antibody (ANCA)-associated vasculitides (AAV) have a prevalence of about 18.7–21.0 per 100,000 in some populations, while giant cell arteritis (GCA) is estimated at 10–22 per 100,000 in people aged ≥50 years (highest in Scandinavia). Geographic, ethnic, and age-related factors affect disease incidence, with higher rates observed in certain populations, such as Northern Europeans in the case of giant cell arteritis.
Vasculitis prevalence in India
In India, vasculitis remains uncommon but shows regional variation among subtypes with possible underdiagnosis due to limited awareness. ANCA-associated vasculitis accounts for about 0.001% (or roughly 1 per 100,000) of hospital admissions, indicating its rarity. Takayasu arteritis occurs more commonly in Indian and other Asian populations than in Western countries. In northern India, the incidence of Kawasaki disease in children under five years old ranges from 4.5–9 cases per 100,000, indicating an increasing awareness of the condition. Rheumatoid vasculitis continues to be a notable concern in South Indian rheumatoid arthritis patients despite global declines.
Vasculitis Types
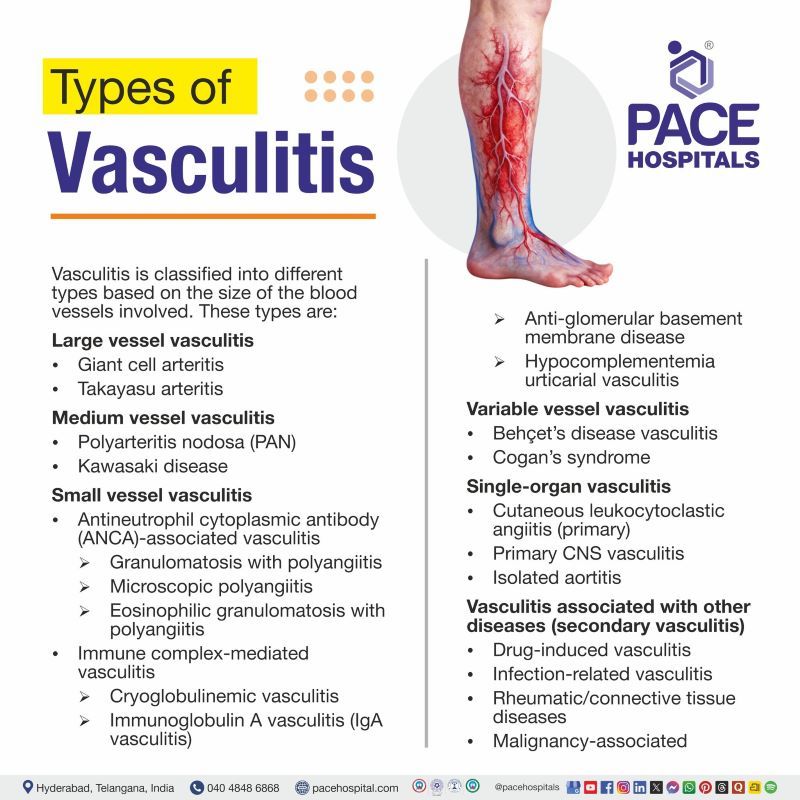
Vasculitis disease is classified mainly based on the size of the affected blood vessels: large, medium, or small. Understanding the types of vasculitides helps doctors identify specific disease patterns, guide investigations, and choose appropriate treatment strategies. The Chapel Hill classification of vasculitis categorises different types. The vasculitis classification is as follows:
- Large vessel vasculitis
- Giant cell arteritis
- Takayasu arteritis
- Medium vessel vasculitis
- Polyarteritis nodosa (PAN)
- Kawasaki disease
- Small vessel vasculitis
- Antineutrophil cytoplasmic antibody (ANCA)-associated vasculitis
- Granulomatosis with polyangiitis
- Microscopic polyangiitis
- Eosinophilic granulomatosis with polyangiitis
- Immune complex-mediated vasculitis
- Cryoglobulinemic vasculitis
- Immunoglobulin A vasculitis (IgA vasculitis)
- Anti-glomerular basement membrane disease
- Hypocomplementemia urticarial vasculitis
- Variable vessel vasculitis
- Behçet’s disease vasculitis
- Cogan’s syndrome
- Single-organ vasculitis
- Cutaneous leukocytoclastic angiitis (primary)
- Primary CNS vasculitis
- Isolated aortitis
- Vasculitis associated with other diseases (Secondary vasculitis)
- Drug-induced vasculitis
- Infection-related vasculitis
- Rheumatic/connective tissue diseases
- Malignancy-associated
Large vessel vasculitis
This type primarily affects the aorta and its major branches, leading to reduced blood flow to large areas of the body.
- Giant cell arteritis: This affects individuals over the age of 50. It mainly involves the arteries of the head, particularly the temporal arteries. Symptoms include headache, scalp tenderness, jaw pain, and vision problems.
- Takayasu arteritis: Usually affects young women and involves the aorta and its main branches. It can cause arm or leg weakness, unequal blood pressure between arms, and organ damage due to restricted blood flow.
Medium vessel vasculitis
This form targets medium-sized arteries that supply organs such as the kidneys, heart, and intestines.
- Polyarteritis nodosa (PAN): It causes inflammation of medium-sized arteries, leading to reduced blood flow and organ damage. It can damage skin, kidneys, nerves and digestive tract.
- Kawasaki disease primarily affects children under 5 years old and causes inflammation of the coronary arteries. It presents with fever, rash, swollen lymph nodes, and redness in the eyes.
Small vessel vasculitis
This category includes diseases that affect small arteries, such as arterioles, capillaries, and venules. This group is further divided into ANCA-associated vasculitis and immune complex vasculitis.
ANCA-associated vasculitis (AAV)
This type is associated with antineutrophil cytoplasmic antibodies (ANCA) that target white blood cells, leading to inflammation of blood vessels.
- Granulomatosis with polyangiitis: This involves inflammation of small blood vessels in the respiratory tract and kidneys.
- Microscopic polyangiitis: This type generally affects capillaries and small arteries in the lungs and kidneys.
- Eosinophilic granulomatosis with polyangiitis (EGPA): This is associated with asthma, elevated eosinophil counts, and organ involvement.
Immune complex–mediated vasculitis
These kinds are caused by the deposition of immune complexes on vessel walls, which trigger inflammation.
- Cryoglobulinemic vasculitis: This is caused by abnormal proteins (cryoglobulins) in the blood, often seen in patients with hepatitis C.
- Immunoglobulin A (IgA) vasculitis: This is the most common vasculitis that affects children after infections.
- Anti-glomerular basement membrane (Anti-GBM) disease: The immune system attacks the basement membrane in the kidneys and lungs.
- Hypocomplementemic urticarial vasculitis: This is characterised by recurring hives (urticaria) and low complement levels in blood; it can affect skin, joints, kidneys, and lungs.
Variable vessel vasculitis
This type affects vessels of any size (large, medium, or small) and can involve both arteries and veins. The pattern and severity vary from person to person, depending on the organ systems involved.
- Behçet’s disease vasculitis: This is a chronic, relapsing form of vasculitis that can affect both arteries and veins of all sizes. It commonly causes mouth and genital ulcers, skin lesions, and uveitis (inflammation of the eye).
- Cogan’s Syndrome: A rare autoimmune disorder affects the eyes and inner ear, resulting in vision and hearing loss.
Single-Organ Vasculitis (SOV)
It is characterized by inflammatory involvement limited to a single organ or tissue without evidence of systemic vasculitis and need careful evaluation and follow-up to exclude evolution into a generalized vasculitic disorder.
- Cutaneous leukocytoclastic angiitis (primary): It is a small-vessel vasculitis limited to the skin, showing neutrophil-predominant inflammation with nuclear debris (leukocytoclasia) in dermal vessels. It generally appears as palpable purpura on the lower legs and can be idiopathic (unknown) or triggered by drugs, infections, or other factors, with idiopathic cases often resolving on their own.
- Primary CNS vasculitis: It is also called primary angiitis of the central nervous system (PACNS). This rare inflammatory disorder is confined to the brain and spinal cord vasculature without systemic involvement. It presents with focal neurologic deficits, headaches, cognitive changes, or seizures, and the diagnosis relies on imaging and sometimes biopsy.
- Isolated aortitis: Isolated aortitis is inflammation of the aortic wall without involvement of other organs or evidence of systemic vasculitis. It may be discovered incidentally on imaging or present with symptoms related to aneurysm or dissection, and histologically resembles large-vessel vasculitis while remaining confined to the aorta.
Vasculitis Associated with Other Diseases (Secondary Vasculitis)
It occurs due to external factors, infections, immune-mediated diseases, or malignancy, with vascular inflammation developing as a result of an underlying condition rather than as a primary disorder.
- Drug-induced vasculitis: A vasculitic reaction triggered by medications, ranging from small-vessel cutaneous leukocytoclastic vasculitis to ANCA-associated forms. Common culprits include antibiotics, NSAIDs, antithyroid drugs, and others, likely mediated by immune complex deposition or aberrant immune activation.
- Infection-related vasculitis: Infections can provoke vasculitic inflammation either by direct invasion of vessel walls or through immune complex formation, agents like hepatitis B and C, bacterial pathogens, and others are well-recognized triggers, and infection-associated vasculitis can involve small to large vessels.
- Rheumatic/connective tissue disease-associated vasculitis: Autoimmune connective tissue disorders like systemic lupus erythematosus (SLE), rheumatoid arthritis, and other CTDs can cause secondary vasculitis, usually affecting small vessels but potentially any vessel size, leading to skin lesions, neuropathy, and organ dysfunction.
- Malignancy-associated vasculitis: Malignancy-associated vasculitis can occur with certain cancers, such as hematologic malignancies or solid tumors, as a paraneoplastic phenomenon. It may lead to immune complex formation or tumor-associated antigens causing vessel inflammation, and its presentation can mimic other forms of vasculitis.
Secondary vasculitis
This type of vasculitis is triggered by another medical condition.
- Associated with systemic disease: This type occurs as a complication of another autoimmune or connective tissue disease (rheumatoid arthritis (RA), systemic lupus erythematosus (SLE), or sarcoidosis).
- Vasculitis associated with other diseases: Certain infections (like hepatitis B, hepatitis C, or HIV) and malignancies (especially lymphomas) can trigger immune complex formation that leads to inflammation and damage of the blood vessels. This immune-mediated injury can result in systemic vasculitis.
- Drug-induced vasculitis: Some medications (such as antibiotics, anti-thyroid drugs, and certain diuretics) can trigger immune reactions that lead to inflammation of small or medium vessels.
Vasculitis Symptoms
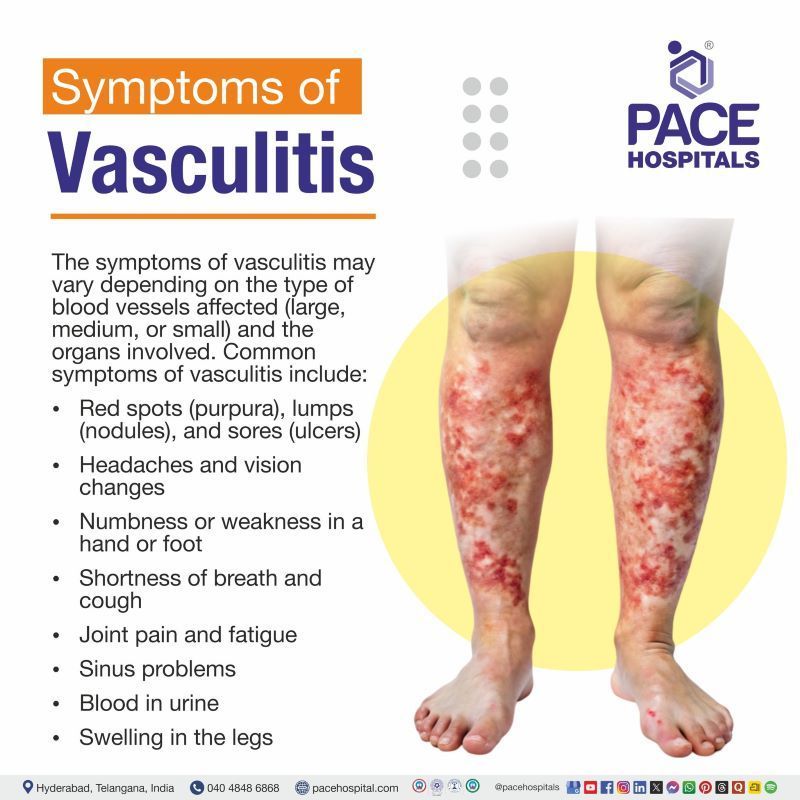
The symptoms of vasculitis may vary depending on the type of blood vessels affected (large, medium, or small) and the organs involved. However, most forms share common signs of vasculitis, including inflammation and reduced blood flow. The common symptoms include:
- Red spots (purpura), lumps (nodules), and sores (ulcers)
- Headaches and vision changes
- Numbness or weakness in a hand or foot
- Shortness of breath and cough
- Joint pain and fatigue
- Sinus problems
- Blood in urine
- Swelling in the legs
Red spots (purpura), lumps (nodules), and sores (ulcers): Inflammation of small or medium-sized blood vessels in the skin may cause leakage of blood, producing red or purple spots referred to as purpura. Deeper vessel involvement may result in the formation of firm, painful nodules, while severe vascular damage can reduce oxygen delivery to tissues, resulting in slow-healing sores or ulcers.
Headaches and vision changes: In large-vessel vasculitides such as giant cell arteritis, inflammation of the arteries in the head and eyes reduces blood flow to the scalp and optic nerve. This causes severe headaches, scalp tenderness, jaw pain, blurred vision, or even sudden vision loss if left untreated.
Numbness or weakness in a hand or foot: Vasculitis affecting small arteries that nourish peripheral nerves can cause nerve injury due to poor blood supply. This leads to numbness, tingling, burning sensations, or weakness in the hands and feet.
Shortness of breath and cough: When vasculitis involves the small blood vessels in the lungs, it can cause inflammation and bleeding in lung tissue. This leads to breathlessness, dry cough, or sometimes coughing up blood, as seen in conditions like granulomatosis with polyangiitis or microscopic polyangiitis.
Joint pain and fatigue: Ongoing inflammation throughout the body can cause joint aching and swelling, as well as a constant feeling of tiredness. Fatigue also results from the immune system's overactivity and reduced oxygen supply to tissues and muscles.
Sinus problems: In some small-vessel vasculitides, like granulomatosis with polyangiitis, inflammation affects blood vessels in the nose and sinuses, leading to chronic sinus pain, nasal congestion, nosebleeds, or sinus infections.
Blood in urine: Inflammation of the kidney’s small vessels (glomeruli) can cause microscopic bleeding, allowing blood and protein to leak into the urine. This sign indicates kidney involvement, a serious complication in ANCA-associated vasculitis.
Swelling in the legs: Reduced kidney function or inflammation of the veins can cause fluid buildup in the lower limbs. Edema (swelling) in the feet and legs is often a sign of impaired circulation or kidney damage due to vasculitis.
Vasculitis Causes
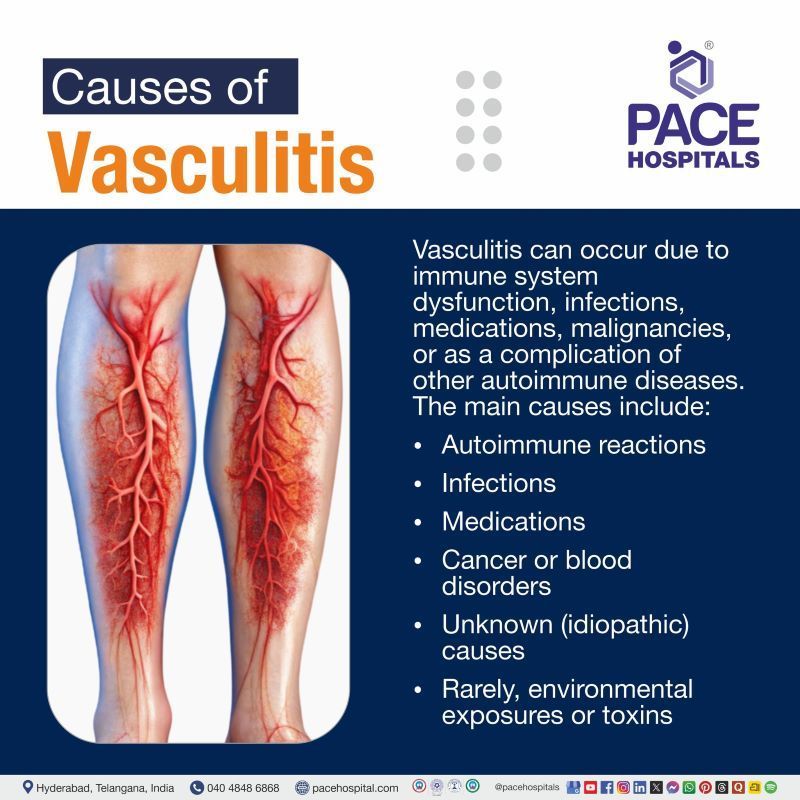
The causes of vasculitis are complex and can differ depending on the type. Vasculitis occurs when the body’s immune system mistakenly attacks blood vessel walls, leading to inflammation, narrowing, or blockage of the vessels. The exact trigger is not always known, but several possible causes include:
- Autoimmune reactions
- Infections
- Medications
- Cancer or blood disorders
- Unknown (idiopathic) causes
- Rarely, environmental exposures or toxins
Autoimmune reactions: In autoimmune vasculitis, the body's immune system mistakenly attacks its own normal blood vessel walls as if they were harmful invaders. This leads to inflammation, narrowing, or blockage of vessels. Autoimmune reactions are common in diseases such as RA, SLE, and systemic scleroderma, where vasculitis occurs as part of the broader immune disorder. Inflammation can affect vessels of any size and, if untreated, lead to organ damage.
Infections: Certain infections, particularly viral infections such as hepatitis B, hepatitis C, varicella-zoster, and HIV, as well as bacterial infections like streptococcal or staphylococcal infections, can act as triggers for vasculitis. The body forms immune complexes (antibody–antigen clusters) while fighting disease, and when these deposit in vessel walls, they cause inflammation and injury. This process, known as immune complex–mediated vasculitis, may affect the skin, kidneys, or nerves.
Medications: Some drugs can cause drug-induced vasculitis as a side effect. The immune system may react abnormally to certain medicines, including antibiotics, diuretics, anti-thyroid drugs, or seizure medications. This hypersensitivity produces inflammation in small or medium vessels, which usually appears as skin rashes, purpura (red patches), or ulcers. Symptoms often resolve after stopping the drug.
Cancer or blood disorders: In some cases, vasculitis occurs secondary to cancers, generally blood-related cancers like leukaemia, lymphoma, or myeloma. Cancer cells or abnormal proteins produced in these conditions can damage vessel walls or trigger immune reactions. Additionally, bone marrow disorders can alter blood cell production, increasing inflammation and vessel injury.
Unknown (idiopathic) causes: In many patients, the exact cause of vasculitis cannot be identified. These are called idiopathic cases. They may result from a complex interaction between genetics, environment, infections, and immune system irregularities. Even without a clear cause, the underlying mechanism remains the same: the immune system attacks blood vessels, causing inflammation and tissue damage.
Rarely, environmental exposures or toxins: It can trigger vasculitis by provoking abnormal immune responses that inflame vessel walls. Examples like silica dust (linked to ANCA vasculitis in miners), solvents such as pesticides, benzene, or heavy metals, often via inhalation or skin contact forming immune complexes. This is more common in certain occupations (e.g., farming, mining) but remains uncommon overall, typically contributing to small-vessel types like microscopic polyangiitis.
Risk Factors for Vasculitis
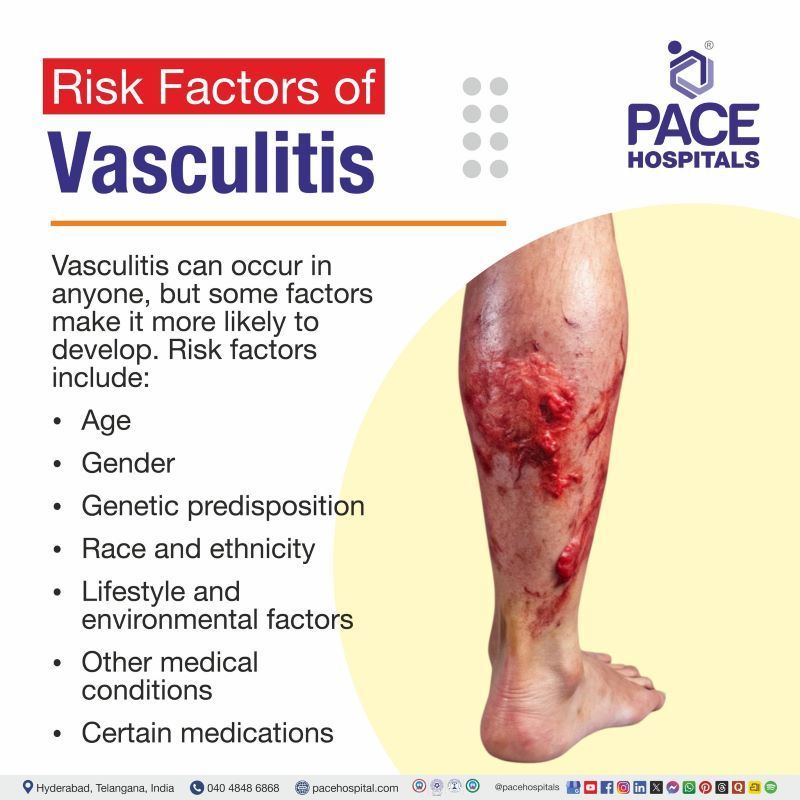
Vasculitis can occur in anyone, but some factors make it more likely to develop. These risk factors affect how the immune system works and how the body responds to triggers, whether they are internal or external. All these factor plays a specific role in increasing vulnerability to vascular inflammation:
- Age
- Gender
- Genetic predisposition
- Race and ethnicity
- Lifestyle and environmental factors
- Other medical conditions
- Certain medications
Age: The likelihood of developing specific types of vasculitis varies with age. For example:
- Kawasaki disease: Mainly affects children under five.
- Giant cell arteritis: This occurs almost exclusively in adults over 50.
- Takayasu arteritis: Most common in women between the ages of 20 and 40.
- Buerger’s disease: Usually affects men younger than age 45 who smoke or have smoked.
Age-related changes in the immune system and blood vessel structure can make older individuals more vulnerable to inflammation and vascular damage.
Gender: Some vasculitides are gender predominant. Giant cell arteritis is more common in women, but Behçet's disease is more common in men, probably due to hormonal and genetic differences influencing immunological responses.
Genetic predisposition: Genetics play a role in determining immune system behaviour. Certain genes, such as HLA-B51, are associated with Behçet’s disease, and other immune-regulating genes can increase the risk of autoimmune vasculitis. A family history of autoimmune or inflammatory disorders may also heighten susceptibility to vasculitis.
Race and ethnicity: Some forms of vasculitis occur more frequently in specific racial or ethnic groups. For example,
- Behçet’s disease: More common in people from the Middle East and Mediterranean regions.
- Giant cell arteritis: More frequent in individuals of Northern European descent.
- Kawasaki disease: More commonly observed among children of Japanese descent.
Such variations are most likely due to a combination of hereditary and environmental factors.
Lifestyle and environmental factors: Environmental exposures, such as smoking, air pollution, or contact with industrial chemicals (such as silica), can trigger or worsen vasculitis by irritating blood vessels and promoting immune activation. Smoking is a strong risk factor, particularly in Buerger's disease, where it causes inflammation and narrowing of small arteries and veins. Chronic stress and poor diet may also indirectly affect immune balance.
Other medical conditions: Individuals with autoimmune diseases such as rheumatoid arthritis, systemic lupus erythematosus, or scleroderma have a higher risk of developing secondary vasculitis due to persistent immune activation. Chronic infections, including hepatitis B, hepatitis C, and HIV, as well as hematologic malignancies like lymphoma, may also cause vascular inflammation through abnormal immune responses or immune complex formation.
Certain medications:
Some medications can trigger allergic or immune-mediated hypersensitivity reactions. Common causes such as antibiotics, diuretics, and antithyroid drugs, with inflammation mainly affecting small vessels and presenting as red spots, skin rashes, or ulcers.
Vasculitis Complications
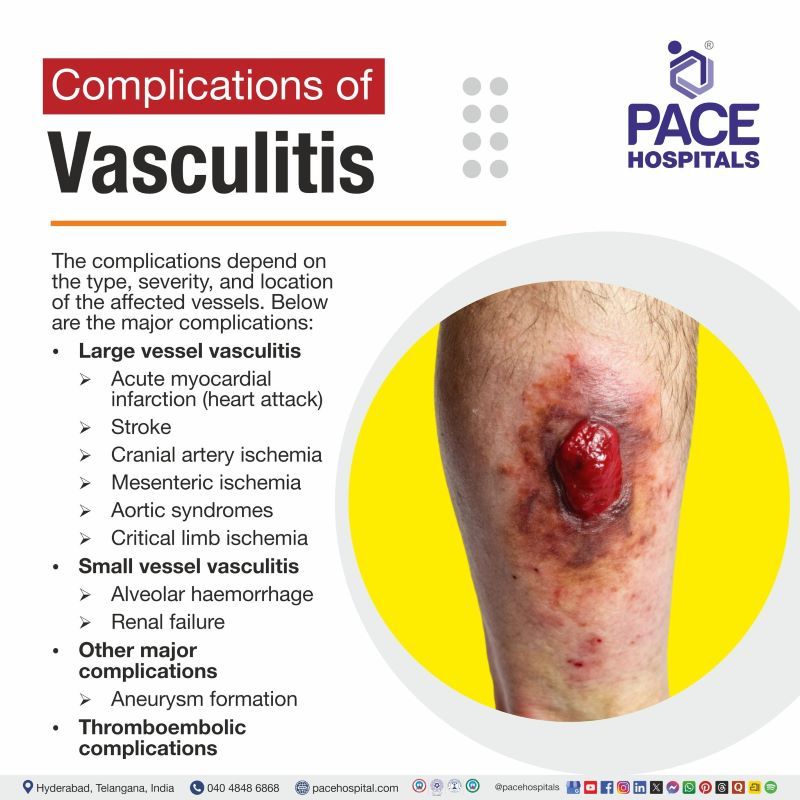
Vasculitis can lead to serious health problems if inflammation damages blood vessels and limits blood flow to vital organs. The complications depend on the type, severity, and location of the affected vessels. Below are the major complications:
- Large vessel vasculitis
- Acute myocardial infarction (heart attack)
- Stroke
- Cranial artery ischemia
- Mesenteric ischemia
- Aortic syndromes
- Critical limb ischemia
- Small vessel vasculitis
- Alveolar haemorrhage
- Renal failure
- Aneurysm formation
- Thromboembolic complications
Large vessel vasculitis complications
Acute myocardial infarction (heart attack)
Inflammation in large arteries such as the aorta or coronary arteries can cause narrowing or blockage, leading to reduced blood flow to the heart muscle. This oxygen shortage results in tissue death and causes a heart attack, a serious complication seen in conditions like Takayasu arteritis or giant cell arteritis.
Stroke
When vasculitis affects the arteries supplying the brain, it can lead to narrowing, blockages, or clot formation. Reduced blood supply leads to ischemic stroke, resulting in sudden weakness, loss of coordination, or paralysis. In some cases, ruptured weakened vessels can cause haemorrhagic stroke.
Cranial artery ischemia
Giant cell arteritis involves arteries in the head and scalp, including those supplying the eyes and brain. The resulting inflammation reduces blood flow, leading to ischemic damage that may cause jaw pain, scalp tenderness, headaches, or sudden vision loss due to optic nerve involvement.
Mesenteric ischemia
Vasculitis involving mesenteric arteries reduces blood flow to the intestines, leading to tissue ischemia, abdominal pain, and potential bowel infarction. If untreated, it may lead to life-threatening intestinal perforation or sepsis.
Aortic syndromes
Chronic inflammation in large-vessel vasculitis can weaken the aortic wall, leading to complications such as aortic aneurysm, aortic dissection, or rupture. These conditions are medical emergencies and may present with chest or back pain, low blood pressure, and circulatory collapse.
Critical limb ischemia
Vasculitis that narrows or blocks arteries in the arms or legs can seriously block the blood flow, causing pain, ulcers, or gangrene in the affected limb. This condition, known as critical limb ischemia, may need urgent medical or surgical intervention to prevent tissue death or amputation.
Small vessel vasculitis complications
Alveolar haemorrhage
In small-vessel vasculitis, inflammation of lung capillaries can cause bleeding into the air sacs (alveoli). This results in coughing up blood, shortness of breath, and low oxygen levels, which can be life-threatening if not promptly treated.
Renal failure
Small-vessel inflammation in the kidney capillaries (glomeruli) leads to glomerulonephritis, causing leakage of blood and protein into urine. Over time, continuous damage results in scarring and kidney failure, requiring dialysis or transplant in severe cases.
Other major complications
Aneurysm formation
Persistent vessel wall inflammation weakens arterial walls, leading to balloon-like bulges (aneurysms). These are common in large- or medium-vessel vasculitis. Aneurysms can rupture suddenly, causing severe internal bleeding and death if not treated in time.
Thromboembolic complications
Damaged and inflamed vessels increase the risk of blood clot formation. These clots can break down and travel through the bloodstream, causing embolism in vital organs such as the lungs (pulmonary embolism) or brain (stroke).
Vasculitis Diagnosis
The diagnosis of vasculitis is usually made through a detailed clinical evaluation. A rheumatologist may ask about symptoms and medical history before performing a thorough physical examination to look for signs of blood vessel inflammation or organ involvement. The following tests are commonly recommended to help confirm the diagnosis and determine the type of vasculitis:
- Medical history
- Physical examination
- Laboratory examinations
- Complete blood count (CBC)
- Inflammatory markers (ESR and CRP)
- Kidney function tests
- Liver function tests (LFTs)
- Serologic tests for viral hepatitis
- Antineutrophil cytoplasmic antibodies (ANCA)
- Autoimmune markers (rheumatoid factor and antinuclear antibodies)
- Urinalysis with urinary sediment
- Immunologic tests
- Complement levels
- Immunoelectrophoresis
- Imaging studies
- Chest X-ray or high-resolution computed tomography (HRCT)
- Computed tomography of sinuses
- Vascular imaging:
- MRI / MR angiogram
- CT angiogram
- Vascular ultrasound
- Positron emission tomography (PET)
- Tissue biopsy
Vasculitis Treatment
The treatment of vasculitis aims to suppress vascular inflammation, prevent further tissue injury, and induce and maintain remission, while minimising treatment-related toxicity. Vasculitis management strategies are guided by the type of vasculitis (large-, medium-, or small-vessel involvement), disease severity, and the presence of organ-threatening or life-threatening manifestations. Treatment options of vasculitis include the following:
Non-pharmacological management
- Multidisciplinary care
- Lifestyle modifications
- Patient education
- Regular exercise
- Weight management
Pharmacological management
- Corticosteroids
- Immunosuppressants / immunomodulators
- Biologics/ targeted therapies
- Adjunctive /symptomatic therapy
- Anticoagulants/ antiplatelet therapy
Surgical intervention
- Angioplasty and stenting of stenotic vessels
- Reconstructive vascular surgery with graft implantation
- Endoscopic management
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support
Vasculitis Prevention
Some types of vasculitides cannot be prevented because they result from autoimmune disorders. However, depending on the cause of the vasculitis, it is possible to prevent certain types from flaring up. The helpful tips to prevent vasculitis are:
- Ensuring a healthy lifestyle
- Avoiding smoking
- Managing weight
- Treating underlying conditions
- Getting routine vaccination
- Ensuring proper monitoring of flare-ups
- Exercising regularly
Ensuring a healthy lifestyle: Taking a healthy diet which are rich in fruits, whole grains, vegetables, and lean protein promotes immune system balance and reduces chronic inflammation. Adequate rest, hydration, and stress management (through meditation or relaxation techniques) also lowers immune overactivation, lowering the risk of vessel inflammation and damage.
Avoiding smoking: Smoking damages the blood vessel walls, increases oxidative stress, and promotes inflammation. It also worsens circulation and may trigger autoimmune reactions. Quitting smoking helps maintain vessel integrity and reduces the risk of flare-ups or complications in people predisposed to vasculitis.
Managing weight: Excess body weight is linked to systemic inflammation and poor circulation. Obesity increases stress on the heart and blood vessels and increases the risk of related conditions like hypertension and diabetes, which can aggravate vasculitis. Maintaining a healthy body mass index (BMI) minimises these inflammatory triggers.
Treating underlying conditions: It helps prevent vasculitis by reducing inflammation and protecting blood vessels. Proper management of autoimmune diseases (like lupus or RA) and infections (such as hepatitis B or C) prevents immune overactivity that can damage vessel walls.
Controlling high blood pressure (High BP) is important because it reduces stress on blood vessels, while managing high cholesterol prevents plaque buildup and inflammation. Together, these measures help maintain healthy circulation and lower the risk of vasculitis flare-ups.
Getting routine vaccinations: Certain infections (e.g., hepatitis B, hepatitis C, influenza) are known triggers for vasculitis. Keeping vaccinations up to date helps prevent these infections, thereby reducing the risk of infection-induced vessel inflammation.
Ensuring proper monitoring of flare-ups: Regular medical check-ups allow early detection of symptoms such as unexplained rashes, fatigue, or joint pain. Prompt administration of medication (commonly corticosteroids or immunosuppressants) are used to prevent the inflammation from causing vascular damage or organ involvement.
Exercising regularly: Regular physical activity boosts blood flow, strengthens the cardiovascular system, and lowers systemic inflammation. Exercise also helps regulate blood pressure and stress, both of which can impact immunological function and vascular health.
Difference between Vasculitis and Vasculopathy
Vasculitis vs vasculopathy
Vasculitis and vasculopathy are both caused by abnormal blood vessels and might show with comparable clinical symptoms such as tissue ischemia, skin sores, or organ malfunction. But their underlying systems and pathogenic processes are fundamentally distinct. Recognising the difference between these two conditions is important for proper diagnosis and treatment. Below are the key differences between vasculitis and vasculopathy:
| Parameters | Vasculitis | Vasculopathy |
|---|---|---|
| Definition | Inflammatory destruction of blood vessel walls due to immune-mediated inflammation. | Non-inflammatory vascular injury resulting from occlusion, thrombosis, embolism, or vascular occlusion without vessel wall inflammation. |
| Pathogenesis | Caused by immune complex deposition, autoimmune reaction, or direct endothelial injury → inflammation and necrosis of the vessel wall. | Caused by coagulopathy, thrombophilia, vascular occlusion, or endothelial dysfunction without immune inflammation. |
| Inflammation | Present – vessel wall infiltrated by neutrophils, lymphocytes, or eosinophils. | Absent – minimal or no inflammatory infiltrate in the vessel wall. |
| Vessel wall damage | Due to inflammatory destruction. | Due to ischemic or thrombotic occlusion, not primary inflammation. |
| Clinical features | Painful, purpuric, or ulcerative skin lesions; may have systemic symptoms (fever, arthralgia, organ involvement). | Usually livedo reticularis, ulcers, or necrosis; no systemic inflammatory features. |
| Treatment | Immunosuppressive/anti-inflammatory therapy (e.g., corticosteroids, immunomodulators). | Anticoagulant/antiplatelet therapy; treat underlying coagulopathy. |
Frequently Asked Questions (FAQs) on Vasculitis
What is vasculitis?
Vasculitis is a group of rare conditions, also called angiitis, in which blood vessels become inflamed, leading to thickening, narrowing, or weakening of their walls. This can reduce blood flow and damage organs or tissues. It may affect small, medium, or large blood vessels anywhere in the body. The cause can be autoimmune reactions, infections, medications, or underlying diseases.
What are the symptoms of vasculitis?
Symptoms of vasculitis depend on the organs and blood vessels affected, but commonly include fatigue, fever, loss of appetite, and weight loss. Many patients develop skin rashes, red or purple spots, joint pain, or muscle aches. If internal organs are involved, there may be numbness, breathing difficulty, abdominal pain, or kidney problems, including blood in the urine.
How to prevent vasculitis?
There is no proven way to prevent vasculitis, but specific measures can reduce risk.
- Maintaining a healthy immune system through balanced nutrition, regular exercise, stress control, and avoiding smoking helps protect blood vessels.
- Managing chronic conditions such as diabetes or hepatitis, getting vaccinated, and avoiding unnecessary medications that can trigger immune reactions are also helpful.
- Regular medical checkups support early detection and management to prevent complications.
What is medium vessel vasculitis?
Medium-vessel vasculitis is a group of disorders characterized by inflammation of medium-sized arteries that supply blood to major organs and body regions such as the kidneys, intestines, and limbs. Diseases such as polyarteritis nodosa and Kawasaki disease are included in this category, where vascular inflammation leads to vessel narrowing or damage, resulting in reduced blood flow, tissue ischemia, pain, weakness, and organ dysfunction.
Is vasculitis contagious?
No. Vasculitis is not contagious; it cannot be passed from person to person. It is a result of the body’s immune system attacking its own blood vessels (in many cases) or being triggered by other underlying causes, not due to a transmissible infection.
Which specialists can diagnose vasculitis?
Because vasculitis can affect many organs and mimic other conditions, diagnosis often involves multiple specialists. A rheumatologist (immune/autoimmune disorders) is usually central. Depending on what organs are involved, you might also see a nephrologist (kidneys), pulmonologist (lungs), dermatologist (skin), neurologist (nerves/brain), ophthalmologist (eyes) or cardiovascular specialist (blood vessels).
Does leukocytoclastic vasculitis go away?
Yes, in most cases of idiopathic leukocytoclastic vasculitis (about 90%), the condition resolves spontaneously within weeks to months. Around 30% of patients may experience extracutaneous involvement, which can complicate the course of the disease. While many cases are self-limiting, and treatment such as oral corticosteroids or steroid-sparing immunosuppressive agents, is considered for more severe or persistent disease to manage symptoms and prevent complications.
Who is most at risk for vasculitis?
People are most at risk for vasculitis when certain medical, genetic, or environmental factors increase the chance of abnormal immune-system activity. Studies show that risk is higher in older adults, people with autoimmune diseases (like rheumatoid arthritis or lupus), chronic infections (hepatitis B or C), certain genetic backgrounds (e.g., HLA types), smokers, and individuals taking specific medications. Exposure to toxins and having a family history of autoimmune disorders also increase susceptibility.
What is vasculitis of the kidneys?
Vasculitis of the kidneys occurs when inflammation affects the small or medium blood vessels inside the kidneys. This decreases blood flow and damages kidney function. Symptoms may include swelling, dark or bloody urine, high blood pressure, or fatigue. It is linked to autoimmune diseases, such as ANCA-associated vasculitis.
Is ANCA vasculitis hereditary?
ANCA-associated vasculitis is generally not considered hereditary. ANCA vasculitis is an autoimmune disease where the immune system mistakenly attacks blood vessels. While genetic factors may influence susceptibility, ANCA vasculitis usually occurs randomly and is not directly passed down from parent to child in a clear hereditary pattern.
What organs are affected by vasculitis?
Vasculitis are the inflammation of blood vessels, and depending on which vessels are affected, many organs may be involved. Commonly affected organs include the skin, kidneys, lungs, eyes, nerves, and joints. If blood vessels supplying an organ become narrowed, blocked or weakened, that organ may suffer damage from reduced blood flow or bleeding.
What is autoimmune vasculitis
This is a condition in which the immune system mistakenly attacks the body's own blood vessels, leading to inflammation. This leads to swelling and damage to blood vessel walls, which can impair blood flow and affect organ function. The exact cause is unclear but involves immune system dysfunction.
Are there conditions that can mimic the presentation of vasculitis?
Yes, many other conditions can mimic vasculitis in presentation (i.e., look like it) yet are different in cause and treatment. These include infections, drug reactions, coagulation disorders, malignant conditions, and even vascular-blockage disorders. Because misdiagnosis can lead to inappropriate therapy, doctors often must rule out these mimics.
When to consult a doctor for vasculitis?
Consult a doctor for vasculitis if symptoms such as persistent fatigue, unexplained fever, or unusual skin rashes (especially red or purple spots) occur. Signs that indicate a need for medical assistance are:
- Unexplained weight loss or night sweats
- Joint or muscle pain that doesn’t improve
- Numbness, weakness, or tingling in the limbs
- Blood in urine or dark-coloured urine
- Breathlessness, chest pain, or coughing up blood
If these symptoms persist, it is best to see a vasculitis doctor for an accurate diagnosis and treatment. Seek emergency care if there is sudden vision loss, severe headache, chest pain, or signs of kidney failure, as these may indicate serious complications. A rheumatologist can provide the right vasculitis treatment to manage symptoms and reduce risks.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868