Esophagitis - Symptoms, Causes, Diagnosis, Treatment & Prevention
PACE Hospitals
Esophagitis definition
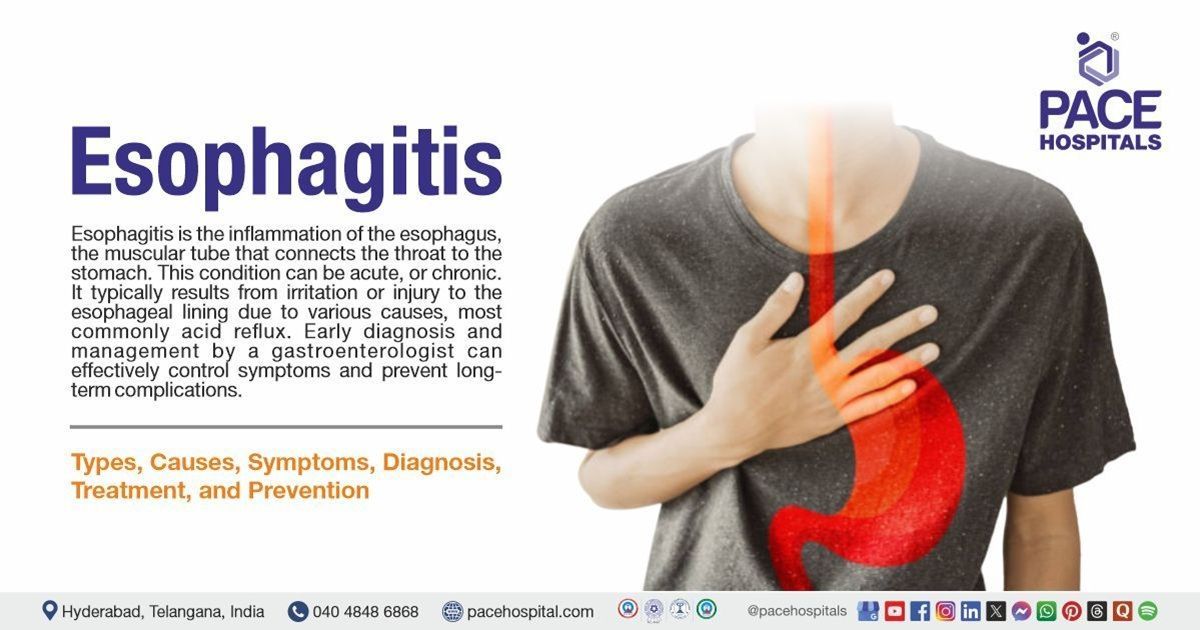
Esophagitis is the inflammation of the esophagus, the muscular tube that connects the throat to the stomach. This condition can be acute(short-term), developing suddenly, or chronic, persisting over a long period of time. It typically results from irritation or injury to the esophageal lining due to various causes, most commonly acid reflux.
Common symptoms include heartburn, chest pain, and painful swallowing. The condition can range from mild cases that may resolve on their own or with treatment to severe cases that can lead to serious complications such as Barrett’s esophagus, necrosis, perforation, or stricture formation. Early diagnosis and management by a gastroenterologist can effectively control symptoms and prevent long-term complications.
Esophagitis meaning
The word "esophagitis" is of Greek origin. It is formed from the Greek root "esophag-" referring to the esophagus (the tube that connects the throat to the stomach), combined with the suffix "-itis," which means inflammation. Hence, "esophagitis" literally means inflammation of the esophagus. The term is used in medical language to describe inflammation or injury to the esophageal mucosa caused by various conditions such as acid reflux, infections, allergies, or medications.
Esophagitis Prevalence
Esophagitis prevalence in the world
Esophagitis prevalence varies by type. Eosinophilic esophagitis (EoE) affects about 40 per 100,000 people globally, with higher rates in high-income countries and males. Its prevalence has elevated from 8 to over 70 per 100,000 between the late 20th century and 2022. GERD, the leading cause of esophagitis, affects around 14% of the global population (over 100 crore people). Esophagitis from infections or medications is less common. Overall, its prevalence is influenced by region, income level, and healthcare access.
Esophagitis prevalence in India
The prevalence of erosive esophagitis in India is approximately 52% (95% CI: 44%–59%) among patients undergoing endoscopy for GERD symptoms, making it one of the highest rates globally. GERD prevalence in the general Indian population ranges from 7.6% to 30%, with erosive esophagitis seen in a smaller subset of symptomatic patients. Key risk factors include age, obesity, diabetes, and hiatal hernia, while Helicobacter pylori infection shows a protective effect.
Types of Esophagitis
There are different types of esophagitis, each with distinct causes, characteristics, and treatments. The following are different types of esophagitis:
- Reflux esophagitis
- Eosinophilic esophagitis
- Drug-induced esophagitis (Pill esophagitis)
- Infectious esophagitis
- Radiation esophagitis
Reflux esophagitis
Frequent and excessive reflux of stomach contents into the esophagus can damage the mucosa. This is mainly due to decreased lower esophageal sphincter (LES) tone and increased transient relaxations. Large hiatal hernias further reduce LES pressure, increasing reflux risk. Impaired esophageal peristalsis or reduced saliva also weakens protective mechanisms, leading to reflux esophagitis.
Eosinophilic esophagitis
The exact pathogenesis of eosinophilic esophagitis (EoE) is not fully understood. However, strong evidence indicates it is an allergic condition activated by sensitisation to food or airborne allergens. Key inflammatory mediators involved include eotaxin, interleukin-5 (IL-5), and STAT6. In some cases, symptoms partially improve with acid suppression therapy, reccomending that acid reflux may also play a contributing role.
Drug-induced esophagitis (Pill esophagitis)
Medication-induced esophagitis occurs from direct irritation and disruption of the esophageal mucosal barrier. Longterm or prolonged contact between the medication and the esophageal lining can lead to localized injury. Acidic drugs may cause caustic damage due to their low pH when dissolved. At the same time, hyperosmolar agents can lead to tissue and vascular injury by drawing water out of cells and damaging the mucosa.
Infectious esophagitis
Infectious esophagitis can be caused by bacteria, viruses, or fungi. It occurs primarily in immunocompromised individuals and is rare in healthy patients. Causative organisms include Candida species, herpes simplex virus (HSV), and cytomegalovirus (CMV).
Radiation esophagitis
Radiation-induced esophagitis involves DNA damage and cell death caused by high-energy electrons and oxygen-free radicals. Acute injury leads to epithelial cell destruction and impaired regeneration, with higher doses causing widespread mucosal loss. Chronic injury involves small vessel ischemia, driven by endothelial inflammation, fibrosis, and smooth muscle proliferation. Over time, this can result in strictures, ulcers, fistulas, and even perforation.
Corrosive esophagitis
Corrosive esophagitis is a serious inflammation of the esophagus caused by ingestion of caustic substances, such as strong acids or alkalis found in household cleaners or detergents. These chemicals can severely damage the esophageal lining, resulting in pain, difficulty swallowing, and potentially life-threatening complications.

Esophagitis Symptoms
Esophagitis can cause a range of symptoms. The Following are the signs and symptoms of esophagitis:
- Difficulty swallowing (dysphagia)
- Painful swallowing (odynophagia)
- Heartburn or a burning sensation in the chest
- Sensation of food stuck in the esophagus
- Acid reflux or regurgitation
- Sore throat
- Hoarseness or voice changes
- Chest pain, especially worsened by eating
- Nausea and vomiting
- Abdominal pain
- Decreased appetite or weight loss
- Cough or chronic throat clearing
- In infants and children: feeding difficulties, irritability, or failure to thrive

Esophagitis Causes
Esophagitis is commonly caused by acid reflux from the stomach, known as GERD, which irritates the esophageal lining. It can also result from eosinophilic esophagitis, an allergic and autoimmune condition. The following are the causes of esophagitis:
- Alcohol use
- Cigarette smoking
- Medical procedures, such as radiation therapy
- Allergies, often to foods
- Infections that weaken the immune system
- Medications, including nonsteroidal anti-inflammatory drugs (NSAIDs) or other irritant medications, can also contribute to esophagitis.
- Chronic vomiting
- Lying down after eating a large meal
- Obesity
Esophagitis Risk Factors
Various factors contribute to the development and progression of esophagitis. Recognizing the risk factors is crucial for early diagnosis, effective treatment, and prevention of complications associated with esophageal inflammation and damage. Risk factors of esophagitis include:
- Smoking: It damages the esophageal lining and weakens the lower esophageal sphincter (LES), promoting acid reflux.
- Alcohol consumption: It irritates esophageal mucosa and can reduce LES pressure.
- Diet (coffee, chocolate, fatty, or spicy foods): These foods can relax the LES or irritate the esophageal lining, elevating the risk of acid reflux and inflammation.
- Pregnancy: Hormonal changes and pressure from the growing uterus can relax the LES and promote reflux.
- Obesity: Increases abdominal pressure, pushing stomach contents into the esophagus.
- Older age: Age-related weakening of esophageal muscles and slower healing make the esophagus more vulnerable to injury.
- Use of NSAIDs and other irritant drugs (e.g., nitrates, beta blockers): These medications can irritate or weaken the esophageal lining.
- Improper pill intake: Swallowing pills without enough water or lying down immediately can cause them to lodge in the esophagus, leading to localized injury.
- Radiation therapy to the chest: It can damage the esophageal mucosa and blood vessels, leading to acute or chronic inflammation.
- Spinal cord injury: May impair the nerve signals responsible for proper esophageal motility and swallowing, increasing the risk of reflux or pill-related injury.
- Scleroderma: An autoimmune condition that stiffens the esophagus and reduces motility, making reflux more likely.
- Multiple food allergies: Increase the risk of eosinophilic esophagitis, an allergic form of esophagitis triggered by certain foods.
Esophagitis Complications
Untreated or chronic (long-term) esophagitis can result in several significant complications affecting the esophagus and, sometimes, beyond. The following are the complications of esophagitis:
- Esophageal stricture: Scarring can cause narrowing of the esophagus, resulting in difficulty swallowing and increased risk of food impaction.
- Ulceration: Chronic inflammation can lead to the development of ulcers, which are breaks in the lining of the oesophagus. These may bleed or become infected.
- Bleeding: Erosions or ulcers can cause gastrointestinal bleeding, which may present as vomiting blood or black, tarry stools.
- Perforation: Severe inflammation may lead to tearing or perforation of the esophageal wall, a medical emergency.
- Barrett's esophagus: Long-term acid exposure can transform the cells lining the lower esophagus (Barrett’s esophagus). This condition increases the risk of esophageal adenocarcinoma.
- Esophageal cancer: Chronic esophagitis, especially when associated with Barrett’s esophagus, increases cancer risk in the esophagus.
- Aspiration and pneumonitis: Poor esophageal motility due to stricture or severe inflammation may allow gastric contents to be aspirated into the lungs, potentially causing pneumonitis or worsening asthma.
- Malnutrition and weight Loss: Difficulty swallowing can lead to reduced food intake, malnutrition, and unintended weight loss.
- Other respiratory complications: Inflammation can spread, resulting in laryngitis, cough, and hoarseness.
Esophagitis Diagnosis
Esophagitis diagnosis depends on history and clinical exam, with endoscopy and biopsy needed to identify subtypes. Mild acid reflux cases may avoid initial endoscopy unless treatment fails. Medication-induced esophagitis often doesn't require immediate endoscopy. The following diagnostic tests are used for esophagitis:
- Medical history
- Physical examination
- Laboratory tests
- Complete blood count (CBC)
- Eosinophil Count
- IgE Levels (Immunoglobulin E)
- HIV or Immunocompromised Status
- Biopsy
- Esophageal Sponge Test
- Imaging studies
- Barium swallow (X-ray series)
- Esophageal pH testing
- Upper endoscopy (Esophagogastroduodenoscopy)
Esophagitis Treatment
Treatment of esophagitis targets the underlying cause, such as acid reflux, infection, medication, or allergies. Managing the root issue helps to relieve symptoms and heal the esophageal lining. The following are the treatment options for esophagitis:
- Non-pharmacological options
- Pharmacological therapy
- Surgical management
Non-Pharmacological Options
- Lifestyle and diet modifications
- Weight management
Pharmacological therapy
- Proton pump inhibitors (PPIs)
- H2-receptor antagonists
- Steroids
- Monoclonal antibodies
- Antimicrobials
- Antacids
- Analgesics
Surgical management
- Fundoplication
- Endoscopic dilation
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support

Prevention of Esophagitis
Effective prevention strategies focus on minimizing irritation and inflammation of the esophageal lining. Important preventive measures include:
- Dietary modifications: The intake of spicy, fatty, and acidic foods needs to be limited. Caffeine, chocolate, and mint have also been associated with increased reflux symptoms. Individuals with food sensitivities or allergies are advised to avoid known allergens such as milk, eggs, nuts, soy, and wheat.
- Eating habits: Chewing food thoroughly and taking small bites reduces mechanical irritation. Consumption of food needs to be avoided close to bedtime. Soft-textured foods may be beneficial for individuals experiencing swallowing difficulties.
- Medication practices: Oral medications need to be taken with a full glass of water and remain in an upright position for at least 30 minutes after ingestion. Medications need not be taken while lying down or immediately before sleep.
- Lifestyle measures: Avoidance of alcohol and tobacco is recommended, as both substances can irritate the esophagus. Maintaining a healthy body weight and engaging in regular physical activity are beneficial in reducing reflux-related symptoms.
- Timing of meals: It is advisable to avoid lying down or going to bed within three hours after eating. Post-meal bending, or strenuous activity, also needs to be minimised to prevent reflux.
- Sleep positioning: Reducing reflux at night can be achieved by raising the head of the bed by 6 to 8 inches. Instead of stacking pillows, which are usually ineffectual, bed risers or a wedge are recommended.
- Allergy management: It is important to identify and remove food allergens under medical supervision in cases of eosinophilic esophagitis. Dietary modification needs to be based on allergy testing or a physician-guided elimination diet.
Difference Between Reflux esophagitis and GERD
Reflux esophagitis Vs GERD
Reflux esophagitis and GERD (gastroesophageal reflux disease) are closely related but distinct. GERD refers to the chronic backflow of stomach acid into the esophagus, However reflux esophagitis describes the inflammation and tissue damage in the esophagus resulting from that acid exposure. Essentially, reflux esophagitis is a potential complication of GERD. Below are some of the parameters that help in differentiating Reflux esophagitis and GERD:
| Parameters | Reflux esophagitis | GERD |
|---|---|---|
| Definition | A chronic condition where stomach acid frequently flows back into the esophagus. | Inflammation of the esophageal lining caused by acid reflux. |
| Causes | Acid reflux can exist without visible damage. | A result of GERD with visible esophageal damage. |
| Symptoms | Heartburn, regurgitation, and chest discomfort can occur, sometimes without visible injury. | Similar symptoms but confirmed with mucosal injury on endoscopy. |
| Severity | It can range from mild to severe, with or without complications. | Indicates a complication or more advanced stage of GERD. |
| Treatment | Lifestyle changes, PPIs, antacids. | Similar treatment often requires more prolonged or more aggressive therapy. |
Difference Between Esophagitis and Barrett's esophagus
Esophagitis Vs Barrett's esophagus
Esophagitis and Barrett's esophagus are related but distinct. Esophagitis is the inflammation of the esophageal lining, often caused by GERD. Barrett's esophagus is a complication of chronic esophagitis where the regular lining changes to an intestinal-type lining, increasing the risk of cancer. Below are some of the parameters that help in differentiating Esophagitis and Barrett's esophagus:
| Parameters | Esophagitis | Barrett's esophagus |
|---|---|---|
| Definition | Esophagitis is defined as Inflammation of the esophageal lining the tube that carries food from the mouth to the stomach. | A condition where the normal squamous cells of the esophagus are replaced by columnar cells (intestinal metaplasia). |
| Causes | There are several types of esophagitis, each with different underlying causes, most commonly due to acid reflux, infections, medications, or allergies. | Long-term, chronic GERD and acid exposure. |
| Risk | It can lead to complications like ulcers or strictures. | Considered a precancerous condition, increases the risk for esophageal adenocarcinoma. |
| Symptoms | Heartburn, chest pain, and painful or difficult swallowing. | Often asymptomatic, may have GERD symptoms. |
| Treatment | Depends on cause: PPIs, antifungals, steroids, etc. | Long-term acid suppression (PPIs), regular surveillance endoscopy, and possibly ablation . |
Frequently Asked Questions (FAQs) on Esophagitis
How to cure esophagitis?
Depending on the cause, treatment may involve lifestyle modifications such as raising the head when sleeping, losing weight, and avoiding trigger foods, as well as proton pump inhibitors (PPIs) or H2-blockers to lower acid. While eosinophilic varieties may need topical steroids or food avoidance, infectious forms are treated with specialised antibiotic drugs. In order to treat esophagitis caused by medication, it is advised to stop using the offending medication. Maintaining recovery and preventing issues requires routine monitoring and follow-up.
How long does esophagitis last?
Most cases resolve within 3–6 weeks with prompt, appropriate therapy, including acid suppression and dietary changes. Mild cases can improve within 1–3 weeks, while more severe or chronic esophagitis, due to long-term acid reflux, allergies, or persistent injury, may require more extended or ongoing treatment. Strict adherence to prescribed medication and medical recommendations is necessary for complete healing and to prevent relapse or complications.
Can esophagitis cause swollen lymph nodes?
Though rarely, severe esophagitis, particularly if due to infection or significant inflammation, can result in swollen lymph nodes as part of the body's immune response. However, lymphadenopathy is not a classical symptom of reflux, allergic, or erosive esophagitis. Persistent or substantial lymph node swelling needs prompt evaluation for other causes, such as infection, malignancy, or other inflammatory diseases.
How to cure reflux esophagitis?
Treatment for reflux esophagitis involves lowering stomach acid with proton pump inhibitors (PPIs) or H2-receptor blockers, as well as altering lifestyle choices such as avoiding heavy meals, stopping smoking, raising the head of the bed, and decreasing weight. Eliminating fatty, acidic, or spicy foods is one way to help. In order to reduce symptoms and promote mucosal healing, surgical procedures like fundoplication might be required if medication is ineffective.
Can esophagitis cause death?
Death from esophagitis is highly uncommon, especially with modern treatment. Complications such as esophageal perforation, severe bleeding, or infection (mediastinitis, sepsis) may rarely become life-threatening if left untreated. Chronic esophagitis increases long-term cancer risk, which can be fatal if undetected and untreated. Early diagnosis, effective management, and ongoing monitoring prevent nearly all fatal outcomes related to esophagitis.
Can esophagitis cause cancer?
Prolonged and severe esophagitis, particularly from chronic gastroesophageal reflux, increases the risk of Barrett's esophagus, a precancerous condition that can progress over the years to esophageal adenocarcinoma. However, with timely therapy, lifestyle changes, and routine monitoring, malignant transformation is uncommon and usually preventable. It is standard practice to suggest surveillance endoscopy for those who are more susceptible.
Can H. pylori cause esophagitis?
Helicobacter pylori is not a typical cause of esophagitis and, in some cases, may even offer mild protection against reflux-related esophageal injury by reducing gastric acid output. Predominantly, H. pylori results in gastritis or ulcers. The majority of esophagitis arises from reflux, pill injury, infection, or allergy. Testing and therapy need to target the identified etiology.
Is eosinophilic esophagitis deadly?
Eosinophilic esophagitis is not considered deadly but can severely affect swallowing and quality of life, leading to symptoms like food impaction and strictures. Rare, severe events may occur, for example, complete food blockages, but fatal outcomes are exceedingly rare. Management includes dietary changes, topical steroids, and endoscopic dilation if necessary. Early and sustained therapy is essential for preventing complications.
What is meant by erosive esophagitis?
Erosive esophagitis means there is visible damage (ulcers or erosions) to the esophageal lining, most commonly from persistent acid exposure. It is more severe than non-erosive esophagitis, poses a higher risk for complications like strictures or Barrett's esophagus, and usually presents with more significant symptoms like pain, bleeding, and trouble swallowing. Diagnosis is generally established on
endoscopy.
Can celiac disease cause esophagitis?
Esophagitis is not commonly caused by celiac disease, but chronic inflammation from gluten sensitivity in susceptible patients can sometimes involve the esophagus. Most esophagitis is related to reflux, infection, or medication injury, but addressing celiac disease with a gluten-free diet may reduce symptom burden and inflammation for some patients. Diagnosis and targeted treatment are based on individual findings.
How long does esophagitis take to heal?
Most patients heal from esophagitis within 3–8 weeks with appropriate therapy, such as proton pump inhibitors and diet modifications. Rapid healing is familiar with early intervention, but severe, chronic, or recurrent esophagitis may need longer or maintenance therapy. Symptom relief may occur in just days, but endoscopic healing often takes several weeks. Follow-up is recommended to confirm complete mucosal recovery and prevent further complications.
How to cure esophagitis naturally?
Natural remedies include avoiding foods that trigger symptoms (spicy, acidic, fatty, caffeinated), losing weight, not eating close to bedtime, and elevating the head when lying down. Drinking water can ease mild symptoms. While these methods can sometimes relieve mild esophagitis, medication is often required for significant or persistent cases, and medical consultation is recommended before relying solely on “natural” treatments for healing.
Can esophagitis go away on its own?
Mild esophagitis can occasionally clear with dietary and lifestyle modifications alone, especially if the trigger is identified and removed quickly. However, most cases need medication to ensure thorough healing and prevent recurrence or complications like bleeding and strictures. Medical assessment and management are best for complete and safe recovery.
How to treat esophagitis pain?
Treatments for esophagitis problems comprise acid-suppressing drugs, including proton pump inhibitors (PPIs), gastrointestinal agents, and H2 blockers, as well as dietary changes like avoiding irritants and eating soft foods. Some people may utilize short-term analgesics or topical anesthetics for extreme pain. For long-term relief and healing, addressing the underlying cause is crucial, and routine follow-up guarantees that no complications arise.
When to consult a doctor for esophagitis?
Recognizing when to consult a doctor for esophagitis is essential in preventing progression and serious damage. The following signs indicate it is time to consult a healthcare professional:
- Symptoms persist for more than a few days or worsen despite self-care
- Severe or prolonged chest pain, especially with sweating or shortness of breath
- Painful or difficult swallowing, or feeling that food is stuck in the throat
- Vomiting frequently, particularly with blood or a dark, coffee-ground appearance
- Unexpected weight loss or loss of appetite
- Symptoms interfering with daily eating or causing significant distress
- Shortness of breath or chest discomfort shortly after meals
- Early evaluation, diagnosis using methods such as endoscopy and biopsy, and appropriate treatment can significantly improve outcomes and reduce the risk of complications.
If these symptoms persist, it is important to consult a esophagitis doctor who can identify the underlying cause of esophagitis and recommend the right treatment plan. Seek emergency medical care if you experience severe chest pain, vomiting blood, or black, tarry stools, which may indicate serious complications such as bleeding or perforation. A general care physician, gastroenterologist, or ENT specialist can provide the best esophagitis treatment to control inflammation, relieve discomfort, and prevent long‑term damage to the esophagus.
What are the key signs of esophagitis, and how can early treatment at PACE Hospitals improve outcomes?
🔥 Warning! Frequent heartburn or chest pain could be more than just discomfort. Early diagnosis can prevent serious esophagus damage.
👨⚕️ Expert tip: Not all swallowing difficulties are normal. If eating feels painful or stuck, PACE Hospitals’ specialists can help find the cause and provide relief.
⚠️ Heads up! Certain medications may harm your esophagus lining if not taken properly. PACE Hospitals advises always swallowing pills with plenty of water.
🛡️ Protect your throat: Simple lifestyle changes like avoiding spicy foods and not lying down right after meals can keep your esophagus healthy. Get personalized advice from PACE experts.
💊 Did you know? Steroids and antibiotics can sometimes irritate your esophagus. Let PACE Hospitals’ medical team guide safe medication use and management.
🕒 Take action early: Ignoring symptoms like sore throat or chronic cough can lead to worsening esophagitis. PACE Hospitals offers timely care for lasting healing.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868