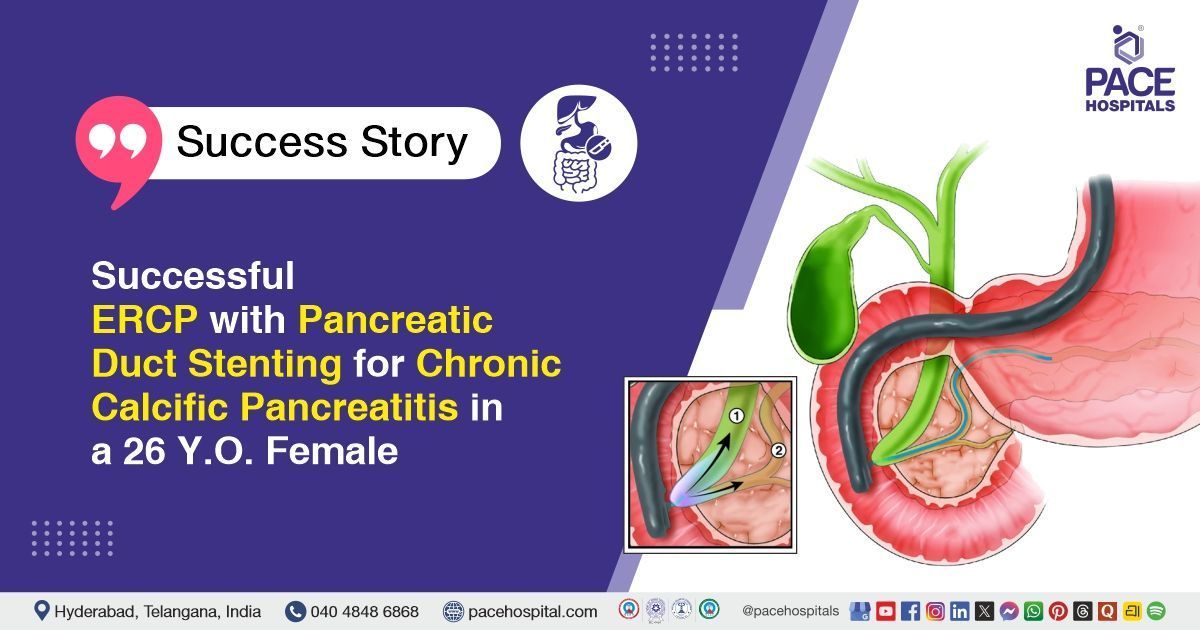
Successful ERCP with Pancreatic Duct Stenting for Chronic Calcific Pancreatitis in a 26 Y.O. Female
PACE Hospitals
PACE Hospitals’ expert gastroenterology team successfully performed Endoscopic Retrograde Cholangiopancreatography (ERCP), Pancreatic Duct (PD) Stenting, Endoscopic Ultrasound (EUS), and Sphincterotomy in a 26-year-old female with chronic calcific pancreatitis, hyperparathyroidism, and hypertriglyceridemia. The procedure was aimed at relieving pancreatic duct obstruction, removing intraductal stones, reducing abdominal pain, and improving pancreatic drainage.
Chief Complaints
A 26-year-old female patient with a body mass index (BMI) of 17 presented to the Gastroenterology Department at PACE Hospitals, Hitech City, Hyderabad, with one month of epigastric and peri-umbilical pain, accompanied by oily stools and unintended weight loss.
Past Medical History
The patient had a history of Type 3c diabetes mellitus secondary to chronic pancreatitis and no known drug or food allergies. She had no history of previous deliveries or surgical procedures related to fertility or sterilization.
On Examination
On general examination, the patient was conscious, coherent and oriented, with stable vitals. General physical examination was normal. Abdominal examination revealed a soft, non-distended abdomen with mild tenderness in the epigastric region, no palpable masses, and no organomegaly. Bowel sounds were present and normal. Cardiovascular and respiratory system examinations were normal. No peripheral edema or lymphadenopathy was noted.
Diagnosis
Following the clinical assessment, the Gastroenterology team conducted a comprehensive review of the patient’s medical history and abdominal symptoms.
Imaging studies, including magnetic resonance cholangiopancreatography (MRCP) and contrast-enhanced computed tomography (CECT) abdomen, demonstrated multiple calculi within the pancreatic duct along with ductal dilation, confirming the presence of chronic calcific pancreatitis. Laboratory investigations revealed hypertriglyceridemia, elevated parathyroid hormone levels, high hemoglobin A1C (HbA1C) and features of Type 3C diabetes mellitus. No acute systemic complications were noted.
Based on the confirmed diagnosis, the patient was advised to undergo Chronic Calcific Pancreatitis Treatment in Hyderabad, India, under the expert care of the Gastroenterology Department.
Medical Decision Making (MDM)
After a detailed consultation with consultant gastroenterologists, Dr. Govind Verma, Dr. M Sudhir, and Dr. Padma Priya, and cross consultation with endocrinologist Dr. Tripti Sharma a comprehensive evaluation was performed to determine the most appropriate diagnostic and therapeutic approach. Considering the patient’s history of chronic calcific pancreatitis, intermittent epigastric pain, steatorrhea, weight loss, hypertriglyceridemia, hyperparathyroidism, and Type 3C diabetes mellitus, an optimal treatment strategy was formulated.
Based on clinical assessment and imaging findings, including magnetic resonance cholangiopancreatography (MRCP) and contrast-enhanced computed tomography (CECT) abdomen, showing multiple intraductal calculi with dilated main pancreatic duct and features of chronic calcific pancreatitis, it was determined that ERCP with pancreatic duct stenting, Endoscopic Ultrasound (EUS), balloon sweeps, and sphincterotomy was identified as the most suitable therapeutic intervention to relieve ductal obstruction, clear pancreatic calculi, and reduce the risk of further pancreatic injury.
The patient and her family members were counselled regarding the diagnosis, planned procedure, associated risks, post-procedure care, and its potential to relieve symptoms, improve pancreatic drainage, and enhance quality of life.
Surgical Procedure
Following the decision, the patient was scheduled to undergo ERCP with Pancreatic Duct Stenting, Endoscopic Ultrasound (EUS), Balloon Sweeps, and Sphincterotomy in Hyderabad at PACE Hospitals under the expert supervision of the Gastroenterology Department.
The following steps were carried out during the procedure:
- Pre-Procedure Preparation: The patient was evaluated for fitness for endoscopic intervention, including assessment of vital signs, blood sugar control, and coagulation status. Informed consent was obtained after explaining the procedure, potential risks, and expected benefits. The patient was positioned in the left lateral decubitus position, and intravenous sedation and analgesia were administered.
- Endoscopic Ultrasound (EUS) Evaluation: A linear echoendoscope was introduced orally to perform EUS of the pancreas. Detailed visualization of the main pancreatic duct, intraductal calculi, and ductal dilation was carried out. The EUS provided precise localization of ductal obstruction and stones, guiding the approach for selective pancreatic duct cannulation.
- ERCP and Pancreatic Duct Cannulation: Following EUS evaluation, ERCP was performed. A duodenoscope was advanced to the second part of the duodenum (D2), and selective pancreatic duct cannulation was achieved using a guidewire and cannula. Contrast injection under fluoroscopy outlined the pancreatic duct, confirming the presence of intraductal calculi and ductal dilation.
- Sphincterotomy and Duct Clearance: A pancreatic sphincterotomy was performed at the ductal orifice to facilitate access to the pancreatic duct. Multiple balloon sweeps were performed to extract stones and debris. Fluoroscopic imaging confirmed complete clearance of the pancreatic duct and restoration of unobstructed ductal flow.
- Stent Placement: A 5 Fr × 7 cm plastic stent was deployed into the pancreatic duct to maintain ductal patency and support drainage. Correct stent placement was confirmed fluoroscopically, completing the therapeutic intervention.
Postoperative Care
The patient’s postoperative period was uneventful. She was closely monitored for vital signs, fluid balance, and signs of abdominal pain or complications. Supportive care was provided to maintain hydration and nutritional status. Measures were taken to prevent infection, manage pain, and ensure optimal pancreatic function. The patient was also monitored for blood sugar levels and metabolic parameters, given her underlying diabetes and hypertriglyceridemia. Overall, she remained hemodynamically stable and was discharged in stable condition.
Discharge Medications
Upon discharge, the patient was prescribed medications to prevent and treat infection, manage pain as needed, and support pancreatic enzyme supplementation for digestion. She was also advised to undergo therapy to protect the gastric lining, correct vitamin deficiencies, and improve bone health. Blood sugar management was continued to maintain glycemic control. Additionally, treatment to manage lipid levels and reduce cardiovascular risk was continued.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms such as fever, abdominal pain, or vomiting.
Review and Follow-up Notes
The patient was advised to return for a follow-up visit with the Gastroenterologist in Hyderabad at PACE Hospitals after one week.
Conclusion
This case highlights a young female with chronic calcific pancreatitis, type 3C diabetes, and hyperparathyroidism, presenting with abdominal pain and weight loss. She underwent ERCP with pancreatic duct stenting, EUS, and sphincterotomy without complications. The postoperative course was uneventful, and she was discharged in stable condition with medications for ongoing management.
Hypertriglyceridemia as a Critical Trigger for Acute and Chronic Pancreatitis
Severe hypertriglyceridemia can precipitate acute or chronic pancreatitis, posing high risk for systemic inflammation and multi-organ dysfunction. Clinical features include epigastric pain, nausea, vomiting, and steatorrhea, often accompanied by markedly elevated triglycerides and abnormal lipid profiles. Early interventions and strict dietary modifications are critical to reduce complications and prevent rapid deterioration.
Comprehensive care involves fluid resuscitation, pain control, pancreatic enzyme supplementation, and long-term lipid management. A gastroenterologist / gastroenterology doctor plays a key role in timely diagnosis, procedural interventions, and coordinating multidisciplinary follow-up with endocrinology and nutrition specialists to reduce recurrence risk and preserve both pancreatic and metabolic function.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868