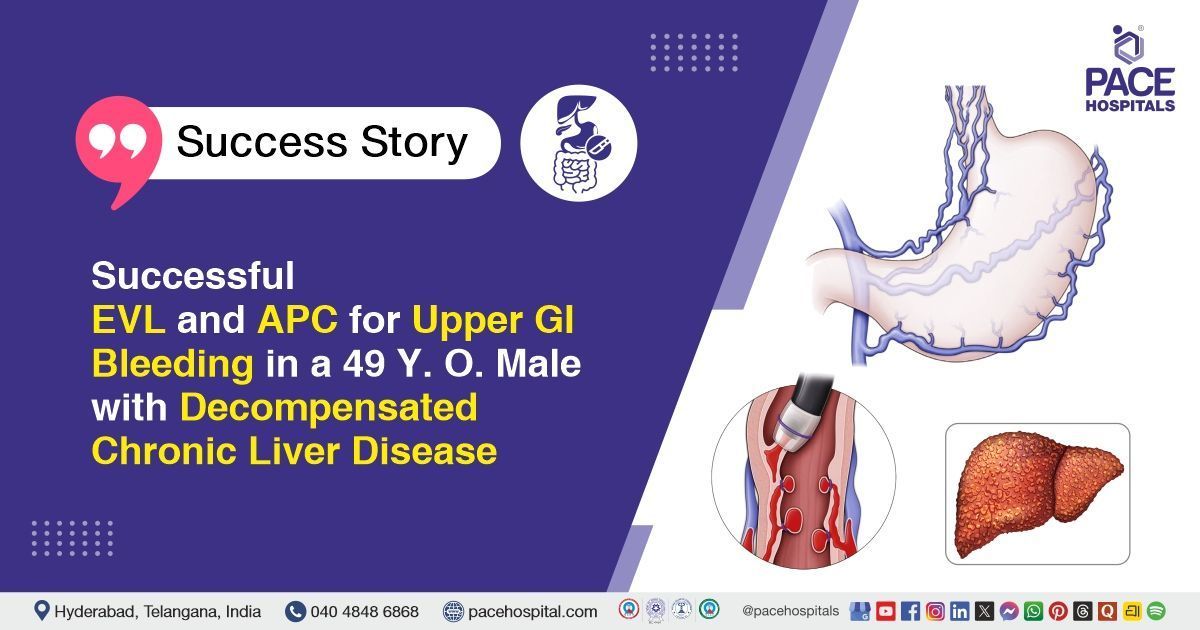
Successful EVL & APC for Upper GI Bleeding in a 49 Y.O. Male with Decompensated Chronic Liver Disease
PACE Hospitals
PACE Hospitals’ expert Gastroenterology team successfully performed Diagnostic and Therapeutic Endoscopy, including Endoscopic Variceal Ligation (EVL) and Argon Plasma Coagulation (APC), on a 49-year-old male patient diagnosed with decompensated chronic liver disease with portal hypertension (etiology: MASLD), Child-Pugh B (score 8), MELD-Na 14, who presented with upper gastrointestinal bleeding due to esophageal varices and a duodenal ulcer. The aim of the procedures was to identify the source of bleeding, achieve effective hemostasis, prevent rebleeding, and stabilize the patient’s condition.
Chief Complaints
A 49-year-old male patient with a body mass index (BMI) of 21 presented to the Gastroenterology Department at PACE Hospitals, Hitech City, Hyderabad, with complaints of black-colored stools for two days, one episode of hematemesis (blood vomiting), and epigastric pain associated with nausea for three days.
Past Medical History
The patient was a known case of decompensated chronic liver disease (DCLD) with portal hypertension, who had a prior history of large esophageal varices for which he had undergone endoscopic variceal ligation (EVL) twice previously. He had experienced previous episodes of upper gastrointestinal bleeding. There was no documented history of diabetes mellitus, hypertension, chronic kidney disease, or coronary artery disease.
On Examination
On general examination, the patient was conscious, coherent, and oriented. Pallor was present. There was no icterus or pedal edema. Vital signs were stable. Systemic examination revealed a soft, non-tender abdomen with no organomegaly appreciated clinically. Cardiovascular examination showed normal heart sounds with no added sounds. Respiratory system examination revealed bilaterally normal vesicular breath sounds. Central nervous system examination was within normal limits.
Diagnosis
Upon admission to PACE Hospitals, the patient was thoroughly evaluated by the Gastroenterology team. The patient was presented with complaints of black-coloured stools for two days, one episode of hematemesis, and epigastric pain associated with nausea for three days. He was a known case of portal hypertension with a prior history of large esophageal varices for which endoscopic variceal ligation had been performed earlier.
The patient underwent a detailed diagnostic evaluation. Emergency upper gastrointestinal endoscopy revealed esophageal varices with post-ligation scarring and ulcers, portal hypertensive gastropathy, altered blood in the stomach, and a duodenal ulcer. Ultrasound abdomen showed features suggestive of chronic liver disease with splenomegaly and bilateral mild pleural effusion. Routine laboratory investigations, including complete blood picture, liver function tests, renal function tests, and coagulation profile, were performed and revealed significant anemia, leukocytosis (high white blood cell count) thrombocytopenia, deranged liver function parameters, and coagulopathy, consistent with decompensated chronic liver disease and active upper gastrointestinal bleeding.
Based on the confirmed diagnosis, the patient was advised to undergo Esophageal Varices and Duodenal Ulcer Treatment in Hyderabad, India, under the expert care of the Gastroenterology Department, with the aim of controlling bleeding, stabilizing the condition, and preventing
Medical Decision Making (MDK)
After a detailed consultation with the consultant gastroenterologists, Dr. Govind Verma, Dr. Padma Priya, and Dr. M. Sudhir, a thorough evaluation was conducted considering the patient’s complaints of black-colored stools, one episode of hematemesis, epigastric pain, and nausea, with a history of decompensated chronic liver disease with portal hypertension. All relevant laboratory, imaging, and endoscopic investigations were reviewed.
Based on clinical and endoscopic findings, which included large esophageal varices with oozing and a duodenal ulcer (Forrest Ib), it was determined that therapeutic endoscopy with Esophageal Variceal Ligation (EVL) and Argon Plasma Coagulation (APC) was identified as the most appropriate intervention to control active bleeding, prevent further gastrointestinal hemorrhage, and stabilize the patient’s condition.
The patient and his family members were counselled regarding the diagnosis, the procedure, associated risks, and its potential to control bleeding, relieve symptoms, and improve quality of life.
Surgical Procedure
Following the decision, the patient was scheduled to undergo Esophageal Variceal Ligation (EVL) and Argon Plasma Coagulation (APC) in Hyderabad at PACE Hospitals under the expert care of the Gastroenterology Department.
The following steps were done during the procedure:
- Preparation and Sedation: The patient is assessed for fitness, kept fasting, and given intravenous sedation for comfort. Continuous monitoring of vital signs is done throughout. The patient is positioned in the left lateral decubitus position to allow safe endoscope insertion.
- Diagnostic Endoscopy: A flexible endoscope is inserted through the mouth to examine the esophagus, stomach, and duodenum. Varices, post-ligation changes, and the duodenal ulcer are identified. Any active bleeding or high-risk lesions are noted to guide therapy.
- Esophageal Variceal Ligation (EVL): Varices are suctioned into a ligation cap and elastic bands are deployed at their base. This compresses the veins, stopping bleeding and promoting scarring. Multiple varices can be treated in the same session if required.
- Argon Plasma Coagulation (APC): The duodenal ulcer is treated with ionized argon gas and electrical energy. This coagulates the ulcer surface, sealing small vessels and reducing bleeding risk. The energy is controlled to prevent damage to surrounding tissue.
- Completion of Procedure: After ligation and coagulation, the mucosa is reassessed for bleeding or injury. The endoscope is withdrawn carefully. The procedure is concluded once hemostasis and variceal management are confirmed.
Postoperative Care
The procedure was uneventful. Subsequently, the patient received one unit of packed red blood cell (PRBC) transfusion and oral iron supplementation. Following this, his condition improved symptomatically, with no further drop in hemoglobin or episodes of melena. Supportive therapy for gastric protection was continued for three days, after which the patient was deemed stable and discharged with appropriate medical advice.
Discharge Medications
Upon discharge, the patient was prescribed medications for gastric acid suppression, antifungal therapy, mucosal protection, bowel regulation, gastroprotection and ulcer healing, vitamin D supplementation, blood pressure control, and liver support.
Emergency Care
The patient was informed to contact the emergency ward at PACE hospitals in case of emergency or having any symptoms like fever, vomiting and abdominal pain.
Review and Follow-up Notes
The patient was advised to return for a follow up visit with the Gastroenterologist in Hyderabad at PACE Hospitals after one week.
Conclusion
This case highlights a patient with decompensated chronic liver disease and upper gastrointestinal bleeding successfully managed with endoscopic therapy, blood transfusions, and supportive care. The patient’s symptoms improved, hemoglobin stabilized, and no further bleeding occurred. He was discharged stable with medications for gastric protection, liver support, and nutritional supplementation, with follow-up advised.
Advanced Portal Hypertension with Acute Variceal Hemorrhage
Acute variceal bleeding in the context of chronic liver disease is a life-threatening complication that requires prompt management by a gastroenterologist / gastroenterology doctor. Clinical features such as hematemesis, melena, and hemodynamic instability, combined with lab abnormalities like anemia, thrombocytopenia, and coagulopathy, indicate significant systemic involvement. Endoscopic interventions, including EVL and APC, are essential to control bleeding and reduce recurrence risk.
Comprehensive care involves blood transfusions, infection prevention, acid suppression, and liver-supportive therapy. Monitoring for complications such as rebleeding, hepatic encephalopathy, and electrolyte imbalances is critical. A gastroenterologist ensures timely interventions and long-term follow-up to improve survival and quality of life in such complex liver disease cases.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868