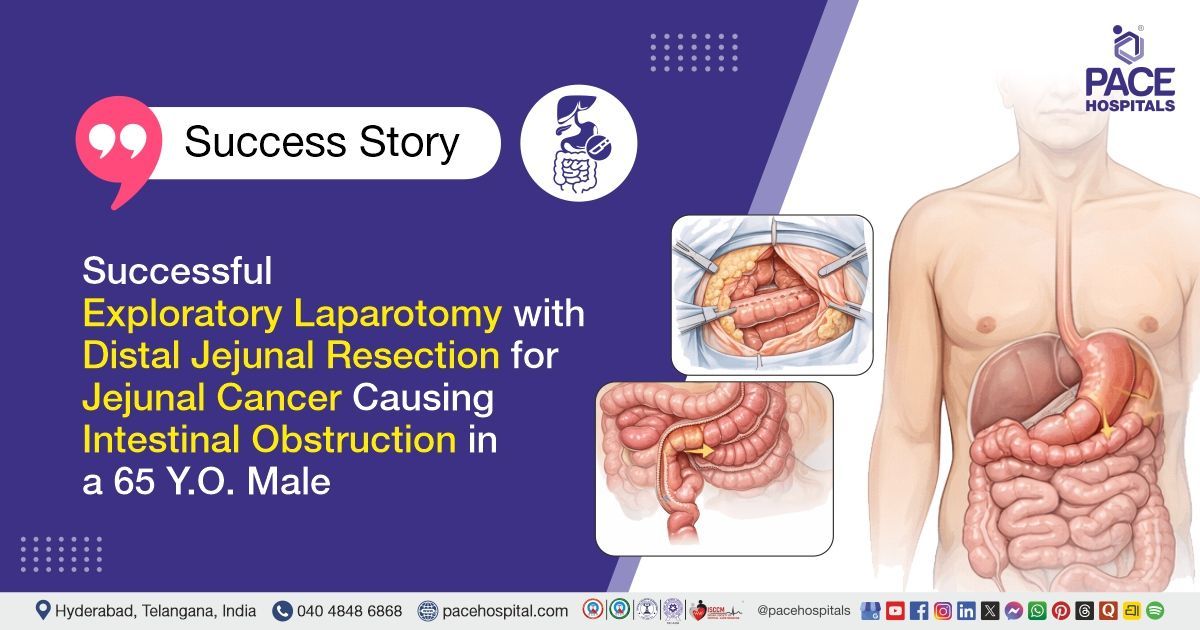
Successful Exploratory Laparotomy with Distal Jejunal Resection for Jejunal Cancer Causing Intestinal Obstruction in a 65 Y.O. Male
PACE Hospitals
PACE Hospitals’ expert Surgical Gastroenterology team successfully performed an Exploratory Laparotomy with Distal Jejunal Resection, side-to-side anastomosis, and Omentectomy on a 65-year-old male patient diagnosed with acute intestinal obstruction secondary to a malignant distal jejunal stricture. The aim of the procedure was to relieve the obstruction, remove the malignant segment of the intestine, restore intestinal continuity, and prevent further complications related to the disease.
Chief Complaints
A 65-year-old male patient with a body mass index (BMI) of 17 presented to the Surgical Gastroenterology Department at PACE Hospitals, Hitech City, Hyderabad, with chief complaints of vomiting and postprandial abdominal discomfort for the past three months. He experienced bilious, non-projectile vomiting occurring 3–4 times per week, typically aggravated after food intake and relieved spontaneously. He also reported persistent postprandial discomfort, leading to a predominantly liquid and pureed diet.
Past Medical History
The patient had no known prior medical comorbidities such as diabetes mellitus, hypertension, cardiac disease, or chronic respiratory illness. There was no history of similar gastrointestinal complaints in the past. He had not undergone any previous abdominal surgeries and had no significant past hospitalizations except for two recent admissions in the last three months for the same presenting complaints. There was no history suggestive of chronic medication use, malignancy, or other systemic illnesses prior to the onset of the current condition.
On Examination
On examination, the patient had poor nutritional status and appeared mildly dehydrated. He was conscious, coherent, and oriented, and was hemodynamically stable. Abdominal examination revealed distension with visible fullness. On palpation, the abdomen was soft with mild diffuse tenderness and no palpable mass. There were no signs of guarding or rigidity. Bowel sounds were exaggerated, suggestive of intestinal obstruction. There was no clinical evidence of ascites. Examination of other systems, including cardiovascular, respiratory, and central nervous systems, was normal.
Diagnosis
Upon admission to PACE Hospitals, the patient was thoroughly evaluated by the Surgical Gastroenterology team. He presented with recurrent episodes of bilious, non-projectile vomiting and persistent postprandial abdominal discomfort for three months, which were aggravated after food intake and led to a predominantly liquid and pureed diet. The clinical presentation, along with progressive symptoms and nutritional compromise, was suggestive of an underlying small bowel obstruction.
The patient underwent further diagnostic evaluation. Contrast-enhanced CT (CECT) of the abdomen revealed dilated proximal bowel loops with a transition point at the mid to distal jejunum, suggestive of small bowel intussusception with a possible pathological lead point and multiple deposits suspicious for metastasis. Routine laboratory investigations were also performed, which showed abnormalities consistent with anemia and poor nutritional status, while other parameters were largely within acceptable limits.
Based on the confirmed diagnosis, the patient was advised to undergo
Acute Intestinal Obstruction Treatment in Hyderabad, India, secondary to a malignant distal jejunal stricture, under the expert care of the Surgical Gastroenterology Department, to relieve obstruction, remove the diseased segment, and prevent further complications.
Medical Decision Making (MDM)
After a detailed consultation with the consultant Surgical Gastroenterologists, Dr. CH. Madhusudhan and Dr. Prashanth Sangu, Dr. Suresh Kumar S, a thorough evaluation was conducted considering the patient’s complaints, and all relevant laboratory and imaging investigations, including complete blood picture, serum electrolytes, liver and kidney function tests, CECT abdomen, ultrasonography, and histopathology of resected specimens, were reviewed.
Based on the clinical and diagnostic evaluations, it was determined that exploratory laparotomy with distal jejunal resection, side-to-side anastomosis, and omentectomy was identified as the most appropriate intervention to relieve the acute intestinal obstruction, remove the malignant jejunal stricture, manage the patient’s complaints, and prevent potential complications such as bowel perforation, persistent obstruction, or further metastatic spread.
The patient and his family members were counselled regarding the diagnosis, the surgical procedure, associated risks, expected postoperative recovery, dietary modifications, and the potential to improve quality of life.
Surgical Procedure
Following the decision, the patient was scheduled to undergo Exploratory Laparotomy with Distal Jejunal Resection, Side-to-Side Anastomosis, and Omentectomy Surgery in Hyderabad at PACE Hospitals, under the expert care of the Surgical Gastroenterology Department.
The procedure involved the following steps:
- Exploratory Laparotomy: The patient was placed under general anesthesia, and a midline abdominal incision was made to access the abdominal cavity. The abdomen was systematically explored, revealing a hard growth of approximately 4 × 3 cm in the distal jejunum, causing luminal narrowing, multiple metastatic deposits over the mesentery and omentum, and two hard nodules over segment 8 of the liver. No ascites was present, and the proximal jejunum was dilated and thickened.
- Distal Jejunal Resection: The affected segment of the distal jejunum, including the stricture and surrounding tissue, was carefully isolated. The mesenteric vessels supplying this segment were ligated to control bleeding. The diseased jejunal segment was then resected with adequate margins to ensure removal of all malignant tissue.
- Side-to-Side Jejunal Anastomosis: To restore intestinal continuity, the proximal and distal cut ends of the jejunum were aligned side-to-side. A hand-sewn or stapled side-to-side anastomosis was performed to create a wide lumen and prevent postoperative narrowing. The anastomosis was checked for integrity to avoid leakage.
- Omentectomy: The omentum containing metastatic deposits was dissected carefully. All nodular tissue in the omentum was removed while preserving healthy omental tissue. Hemostasis was ensured throughout the procedure to prevent postoperative bleeding.
- Closure and Drain Placement: The abdominal cavity was irrigated and inspected for bleeding or leakage. A drain was placed near the anastomosis to monitor postoperative output, particularly for chyle leak. The abdominal layers were then closed in a standard manner. The patient was transferred to postoperative care, managed with IV fluids, antibiotics, and a chyle diet.
Postoperative Care
The procedure was uneventful, and post-procedure recovery was satisfactory. On postoperative day five, the patient had turbid drain output, and evaluation for chyle leak revealed a triglyceride level of 241 mg/dl. He was managed with a chyle diet, resulting in a gradual decrease in drain output. Histopathology showed moderate-grade bowel cancer (3 cm) that spread through the bowel wall, with cancer spots in nearby tissues (subserosa, omentum, mesentery), spread via lymph/nerves, and a tiny spot at one edge (stage pT4 N0 M1; no cancer in 6 nodes). During his hospital stay, he received treatment for fluid and electrolyte management, infection control, and other supportive care. The patient was discharged in a hemodynamically stable condition with advice for follow-up care.
Discharge Medications
At discharge, the patient was prescribed medications for infection control, acid suppression, pain management as needed, nutritional supplementation, and calcium supplementation to support recovery and maintain overall health.
Advice on Discharge
The patient was advised to follow a chyle diet, including pure medium-chain triglycerides and a protein supplement mixed in water, to be taken every alternate hour to support nutritional needs and promote recovery.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms such as fever, abdominal pain, and vomiting.
Review and Follow-up Notes
The patient was advised to return for a follow-up visit with the Surgical Gastroenterologist in Hyderabad at PACE Hospitals, after 5 days, to review his condition.
Conclusion
This case highlights an acute intestinal obstruction secondary to malignant distal jejunal stricture with mesenteric and omental metastases, managed successfully with exploratory laparotomy, distal jejunal resection, and anastomosis. Postoperative recovery was satisfactory, with a transient chyle leak managed conservatively through dietary modification. The patient was discharged in a hemodynamically stable condition with appropriate supportive care and follow-up instructions.
Acute Jejunal Obstruction Secondary to Malignancy
Acute intestinal obstruction due to malignant jejunal strictures often presents with persistent vomiting, postprandial abdominal discomfort, and gradual intolerance to solid foods. Imaging typically shows proximal bowel dilation, a discrete transition point, and sometimes intussusception or mesenteric/omentum deposits. Management is usually surgical, performed by a surgical gastroenterologist / surgical gastroenterology doctor, involving resection of the obstructed segment with side-to-side anastomosis and possibly omentectomy or nodal sampling.
Postoperative issues like chyle leak are managed with a medium-chain triglyceride (MCT) diet, drainage, and supportive care. Monitoring of nutrition, electrolytes, and infection is crucial during recovery. Prognosis depends on tumor stage, metastasis, and patient condition, and early intervention by a surgical gastroenterology doctor improves symptom relief and quality of life.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868