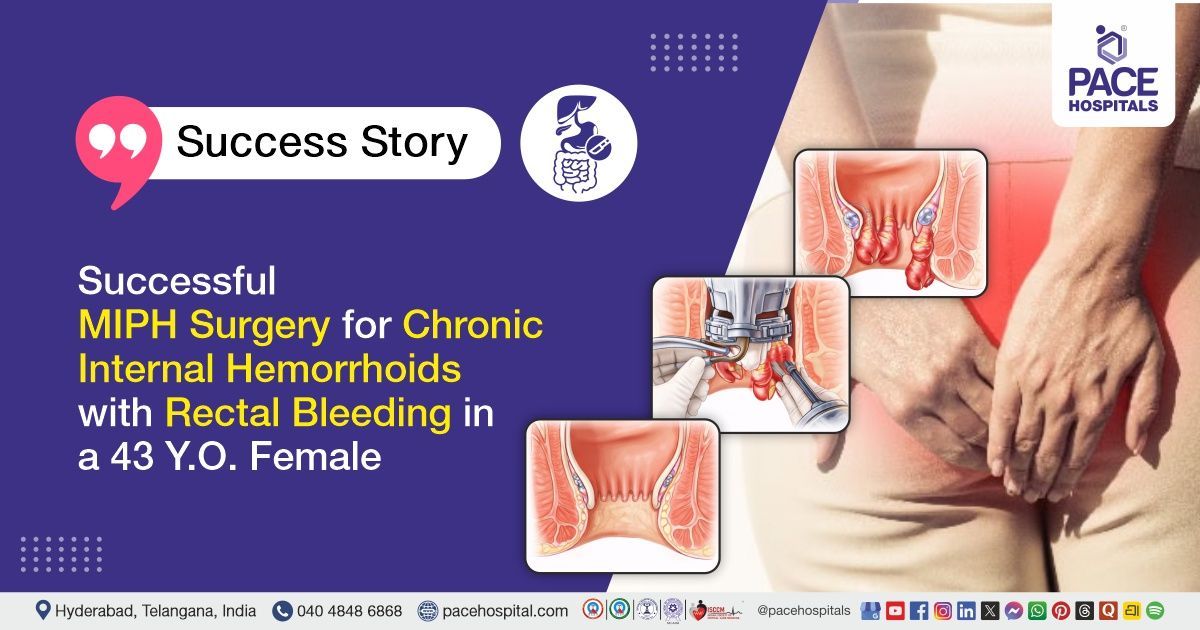
Successful MIPH Surgery for Chronic Internal Hemorrhoids with Rectal Bleeding in a 43 Y.O. Female
PACE Hospitals
PACE Hospitals’ expert gastroenterology team successfully performed Minimally Invasive Procedure for Hemorrhoids (MIPH) on a 43-year-old female with internal hemorrhoids, with the aim of reducing prolapsed hemorrhoidal tissue, controlling bleeding, and relieving symptoms such as pain and discomfort while preserving normal anal function.
Chief Complaints
A 43-year-old female patient with a body mass index (BMI) of 21 presented to the Gastroenterology Department at PACE Hospitals, Hitech City, Hyderabad, with chief complaints of bleeding per rectum for the past 5 years. She had previously undergone a hemorrhoidectomy, and for the past 1 year she experienced recurrent bleeding per rectum associated with lower abdominal pain and perianal swelling.
Past Medical History
The patient was a known case of systemic hypertension and was on regular medication. She had a past surgical history of cholecystectomy and hemorrhoidectomy.
On Examination
On examination, the patient was conscious, coherent and oriented. Vital signs revealed elevated blood pressure, while pulse rate, temperature, and oxygen saturation were within normal limits. On systemic examination, the per abdomen examination was soft and non-tender, with no palpable masses or organomegaly. Other systemic findings were within normal limits, with the notable abnormality being uncontrolled systemic hypertension at presentation.
Diagnosis
Following the clinical assessment, the Gastroenterology team conducted a comprehensive evaluation of the patient’s long-standing rectal bleeding, abdominal discomfort, and perianal swelling, along with a detailed review of her medical and surgical history.
Clinical examination and proctoscopic evaluation suggested prolapsed internal hemorrhoids, consistent with the patient’s symptoms of bleeding per rectum and perianal swelling. Further assessment, along with the patient’s history of previous hemorrhoidectomy, supported the presence of recurrent hemorrhoidal disease.
Based on the confirmed diagnosis, the patient was advised to undergo Hemorrhoids Treatment in Hyderabad, India, under the expert care of the Gastroenterology Department.
Medical Decision Making (MDM)
After a detailed consultation with consultant gastroenterologists, Dr. Govind Verma, Dr. M. Sudhir, and Dr. Padma Priya, along with surgical gastroenterologist Dr. Suresh Kumar S, a comprehensive evaluation was performed to determine the most appropriate diagnostic and therapeutic approach. Considering the patient’s history of long-standing bleeding per rectum, lower abdominal pain, perianal swelling, previous hemorrhoidectomy, and systemic hypertension, an optimal treatment strategy was formulated.
Based on clinical assessment and proctoscopic findings confirming internal hemorrhoids, along with laboratory investigations that were within normal limits, it was determined that Minimally Invasive Procedure for Hemorrhoids (MIPH) with stapler hemorrhoidectomy was identified as the most suitable therapeutic intervention to reduce prolapsed hemorrhoidal tissue, control rectal bleeding, relieve symptoms, and minimize postoperative discomfort and recovery time compared to conventional hemorrhoid surgery.
The patient and her family members were counselled regarding the diagnosis, planned procedure, associated risks, and its potential to relieve symptoms and improve quality of life.
Surgical Procedure
Following the decision, the patient was scheduled for Minimally Invasive Procedure for Hemorrhoids (MIPH) with stapler hemorrhoidectomy in Hyderabad at PACE Hospitals, under the expert care of the Gastroenterology Department.
The following steps were carried out during the procedure:
- Proctoscopic Dilatation: The anal canal was gently dilated using a proctoscope to allow adequate visualization and access to the prolapsed internal hemorrhoids.
- Identification of Hemorrhoidal Zone: The dentate line was identified, and the operative field was carefully assessed to determine the level for suture placement above the hemorrhoidal cushions.
- Purse-String Suture Placement: A circumferential purse-string suture was placed approximately 1 cm above the dentate line in the rectal mucosa to lift and reposition the prolapsed hemorrhoidal tissue.
- Stapled Hemorrhoidopexy (MIPH): A circular stapling device was introduced, and stapled hemorrhoidectomy was performed to excise a ring of redundant rectal mucosa and reposition the third-degree hemorrhoidal cushions.
- Hemostasis and Dressing: Hemostasis was confirmed, the surgical site inspected for bleeding, and appropriate dressing was applied to complete the procedure.
Postoperative Care
The patient’s postoperative period was uneventful, and she remained stable throughout her hospital stay. She received supportive care, including hydration, infection prevention, pain management, acid suppression, and bowel regulation. The patient showed symptomatic improvement and was discharged with the prescribed medications.
Discharge Medications
Upon discharge, the patient was prescribed medications for infection prevention, acid suppression, blood pressure control, bowel regulation, pain relief, and symptom management as needed. These therapies are intended to support healing, prevent complications, and ensure comfort during the recovery period.
Advice on Discharge
The patient was advised to avoid constipation and straining during bowel movements.
Dietary Advice
The patient was advised to follow a high-fiber, low-salt diet to promote bowel regularity and support overall health.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms such as fever, abdominal pain, bleeding per rectal or vomiting.
Review and Follow-up Notes
The patient was advised to return for a follow-up visit with the Gastroenterologist in Hyderabad at PACE Hospitals after 5 days and review with the surgical gastroenterologist after 5 days.
Conclusion
This case highlights a patient with internal hemorrhoids and systemic hypertension who underwent a successful Minimally Invasive Procedure for Hemorrhoids (MIPH). The procedure and postoperative period were uneventful, with symptomatic improvement. The patient was discharged in stable condition with advice on bowel care, dietary modifications, and scheduled follow-up.
Comprehensive Approach to Advanced Hemorrhoids
Advanced hemorrhoids require precise surgical intervention to alleviate symptoms and prevent complications. Minimally invasive stapler hemorrhoidectomy achieves this while minimizing pain and hospitalization. Optimizing bowel habits, diet, and comorbidity management is essential for successful recovery. A gastroenterologist/gastroenterology doctor plays a key role in guiding the procedure, monitoring postoperative progress, and managing associated comorbidities.
Postoperative care also includes monitoring for bleeding, ensuring proper wound healing, and managing any discomfort effectively. Multidisciplinary follow-up ensures sustained symptom relief, early identification of complications, and reduces the risk of recurrence. Patient education on lifestyle modifications and adherence to follow-up schedules further enhances long-term outcomes.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868