Hepatomegaly: Symptoms, Causes & Treatment
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. Govind Verma - Senior Consultant Gastroenterologist & Hepatologist
Hepatomegaly definition
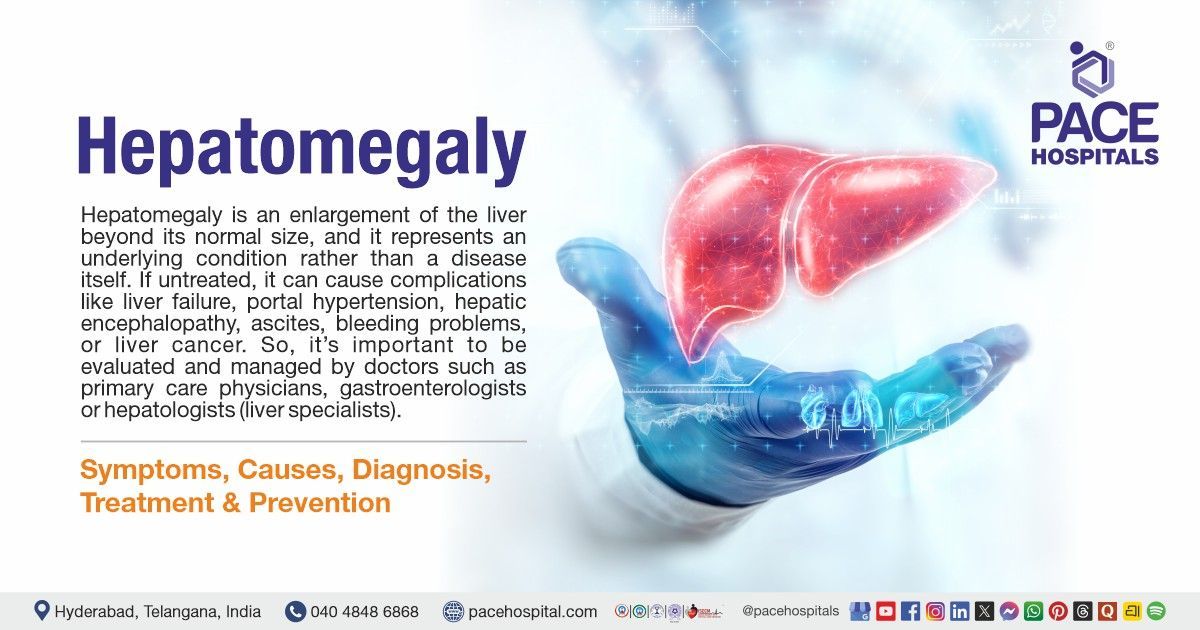
Hepatomegaly means an enlarged (swollen) liver beyond its normal size, and it is usually a sign of another underlying problem rather than a disease by itself. Some people have no symptoms, but others may feel abdominal fullness or pain, tiredness, nausea, vomiting, or notice yellowing of the skin and eyes (jaundice).
Clinicians diagnose it through a physical exam, blood tests, scans like ultrasound/CT/MRI, and sometimes a liver biopsy to evaluate the underlying causes. Common causes include liver diseases (like hepatitis, fatty liver, or cirrhosis), alcohol consumption, carcinoma spread, heart failure, infections, or metabolic disorders. If untreated, it can lead to serious complications like liver failure, portal hypertension, ascites (fluid in the abdomen), hepatic encephalopathy, bleeding issues, or liver cancer. So it’s important to be evaluated and managed by doctors such as primary care physicians, gastroenterologists or hepatologists (liver specialists).
Hepatomegaly meaning
The word hepatomegaly is derived from the two Greek words
- “Hepar” or hepato, meaning "liver"
- “Megas” meaning “enlargement” or “large”
Hepatomegaly is a medical term defined as “enlargement of the liver”.
Hepatomegaly Prevalence
Hepatomegaly prevalence worldwide
Hepatomegaly is not a disease in itself, but rather a sign of other liver diseases. Because of this, there is no specific worldwide prevalence estimate for hepatomegaly as a standalone condition. As of 2019, pooled analyses of studies show that nonalcoholic fatty liver disease (NAFLD), which is a common cause of hepatomegaly, affects about 32% of adults worldwide. This number is even higher among men (40%) and is worsening over time. There haven't been any recent articles that give a specific number for hepatomegaly, which shows that there is a lack of comprehensive global surveillance research.
Hepatomegaly prevalence in India
There isn't a specific number for how common hepatomegaly is in the general population because it is usually reported as a clinical sign rather than a separate condition. These articles talk about underlying causes like viral hepatitis. They note that hepatitis B (HBsAg prevalence 3–4%, affecting 4 crores carriers) and hepatitis C (1% population prevalence) are both common and cause liver enlargement, but they don't give any direct statistics on hepatomegaly. There haven't been any recent articles that give a clear national prevalence rate for hepatomegaly itself. This shows that there is a lack of aggregated data, even though there is extensive detailed information on viral hepatitis.
Hepatomegaly Pathophysiology
The following are the steps involved in pathophysiology of hepatomegaly which include:
- Infiltrative processes: The accumulation of substances like glycogen, lipids, iron, or lysosomal materials (for example, in storage diseases like Gaucher or mucopolysaccharidoses) induces hepatocytes develop, which leads to organomegaly (enlargement of liver).
- Congestive mechanisms: When blood can't flow out of the veins (like in heart failure or hepatic vein thrombosis), the sinusoids become enlarged and blood pools, which stretches the liver capsule.
- Inflammatory responses: Infections (e.g., hepatitis viruses, cytomegalovirus) or toxins cause damage to hepatocytes, swelling, and an increase in inflammatory cells, which leads to liver enlargement.
- Neoplastic infiltration: Malignant cells (e.g., leukemia, lymphoma, metastases) supplant normal parenchyma or disrupt its structural integrity, leading to nodular or diffuse enlargement.
- Metabolic overload: Conditions like hemochromatosis or Wilson's disease cause too much iron or copper to build up in the body. This damages liver cells, causes fibrosis (scarring), and creates regenerative nodules, resulting in hypertrophy (liver cells grow abnormally).
Hepatomegaly Symptoms
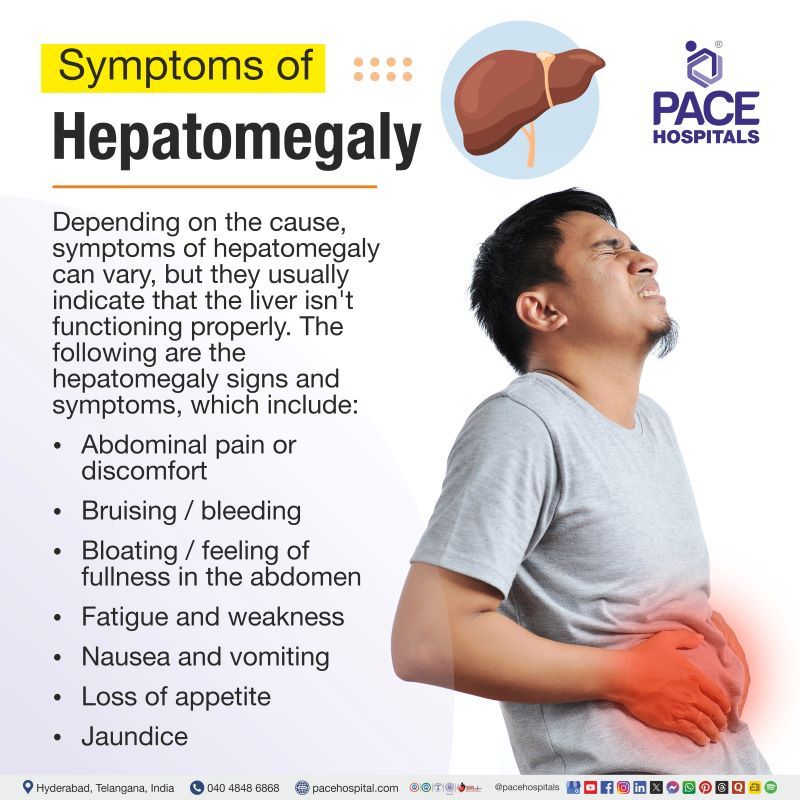
Depending on the cause, symptoms of hepatomegaly can vary, but they usually indicate that the liver isn't functioning properly or is putting too much pressure on other organs. Mild hepatomegaly is often asymptomatic (absence of symptoms).
The following are the hepatomegaly signs and symptoms, which include:
- Abdominal pain or discomfort
- Bruising/bleeding
- Bloating/feeling of fullness in the abdomen
- Fatigue and weakness
- Nausea and vomiting
- Loss of appetite
- Jaundice
- Dark urine and pale stools
- Itchy skin (pruritus)
- Enlarged spleen (splenomegaly)
Abdominal pain or discomfort: When the liver gets enlarged, it stretches the capsule that surrounds it, which can cause pain or discomfort in the right upper abdomen. This symptom could mean there is something wrong with the liver, and it should be checked out by a doctor.
Bruising/bleeding: People with liver disease and hepatomegaly may bruise or bleed easily because their damaged liver can't make enough clotting factors or platelets, which causes bleeding that isn't normal. When liver function gets worse, it's common to bruise and bleed easily, especially in chronic liver diseases like cirrhosis.
Bloating/feeling of fullness in the abdomen: When the liver gets larger, it takes up more space in the abdominal cavity, which puts pressure on the stomach and makes it feel full or bloated even after small meals. People often say they feel "bloating or fullness in the belly" when their liver gets bigger.
Fatigue and weakness: Fatigue and weakness are common signs of hepatomegaly because when the liver doesn't work properly, it can make it harder for the body to make energy and keep its metabolism going, which makes people feel tired and weak all over. People with liver diseases that cause the liver to grow bigger often report these symptoms. They may also have other systemic problems, such as losing weight and anorexia (not feeling like eating).
Nausea and vomiting: Hepatomegaly can cause nausea and vomiting because liver diseases often affect digestion and appetite, which can irritate the stomach and make it harder for the body to get rid of toxins. Along with fever and abdominal pain, nausea and vomiting are common signs of liver enlargement and hepatitis.
Loss of appetite: People with hepatomegaly lose their appetite (anorexia) because their liver isn't working properly, which makes them feel sick and less hungry. Liver diseases often cause a lack of appetite and weight loss as general systemic symptoms because the liver isn't working properly and is inflamed.
Jaundice: Jaundice is when the skin and white part of the eyes turn yellow because there is too much bilirubin in the blood. This usually means that the liver isn't working right or that the bile duct is blocked. It is a clinical sign that is often linked to liver diseases like hepatitis or cirrhosis.
Dark urine and pale stools: When the liver or bile duct doesn't work appropriately, bile can't get to the intestines. Instead, excess bilirubin is excreted in urine, which makes it dark, and bile pigments are missing, which makes stools pale or clay-colored. These colour changes may mean that bile isn't flowing properly or that the liver isn't working properly. They may also be linked to conditions like jaundice and hepatomegaly.
Itchy skin (pruritus): Itching is a common sign of liver and bile flow problems. It happens when bile salts build up in the blood and irritate skin nerves, causing generalized itching without a rash. Cholestasis (impairment or blockage of bile flow from the liver) and other liver diseases are often associated with this symptom, which can cause itching ranging from mild to severe.
Enlarged spleen (splenomegaly): Splenomegaly is an abnormal enlargement of the spleen. It often happens with liver diseases like hepatomegaly because of shared blood flow and portal hypertension. It can make the stomach feel full or hurt, and it can be linked to infections, blood problems, or liver problems.
Hepatomegaly Causes and Risk Factors
Many factors can cause hepatomegaly, such as infections, metabolic disorders, cancers, and systemic diseases that make the liver inflamed, congested, or infiltrated.
The following are the causes and risk factors of hepatomegaly:
- Alcohol abuse
- Primary liver cancer (hepatocellular cancer)
- Diabetes
- Autoimmune hepatitis
- Metastatic cancer (cancer that spreads to the liver)
- Congestive heart failure
- Glycogen storage disease
- Amyloidosis
- Hepatitis A
- Hepatitis B
- Hepatitis C
- Leukemia/lymphoma infiltration
- Nonalcoholic fatty liver disease (NAFLD) is associated with obesity
Alcohol abuse: Taking too much alcohol can damage liver cells and cause liver disease, which can make the liver swell (hepatomegaly). Long-term heavy drinking can lead to liver swelling and conditions like fatty liver, alcoholic hepatitis, and cirrhosis.
Primary liver cancer (hepatocellular cancer): Primary liver cancer (hepatocellular carcinoma) starts in liver cells (hepatocytes) and often happens in people who have chronic liver damage from cirrhosis or hepatitis infections. This causes tumours to grow in the liver. The tumour can make the liver larger (hepatomegaly) and cause symptoms like abdominal pain, jaundice, and weight loss as it grows.
Diabetes: Diabetes, particularly type 2 diabetes, can result in hepatic steatosis, associated with the accumulation of fat in the liver, which causes liver enlargement and damage. High blood sugar for a longer duration can also damage the liver and other internal organs, which raises the risk of liver disease and hepatomegaly.
Autoimmune hepatitis: It is a long-term liver disease that causes inflammation and possibly enlargement of the liver. It happens when the body's immune system attacks liver cells. Autoimmune hepatitis can progress to cirrhosis or liver failure if untreated.
Metastatic cancer (cancer that spreads to the liver): Metastatic cancer is a type of cancer that spreads from its original site. (Primary) site to other organs, like the liver, where it can grow new tumours and make the liver bigger. Cancer cells move through the blood or lymphatic system and grow in the liver, which causes secondary liver cancer (liver metastases).
Congestive heart failure: When someone has congestive heart failure/heart failure, blood backs up into the hepatic veins. This raises the pressure in the veins and causes the liver to become congested and enlarged (congestive hepatomegaly). If chronic congestion persists, it can damage the liver, leading to jaundice, hepatocyte injury, and even fibrosis.
Glycogen storage disease: It is a genetic metabolic disorder characterized by defective enzymes that lead to excessive glycogen accumulation in the liver, resulting in hepatomegaly (liver enlargement). Hepatomegaly and metabolic problems occur when liver cells store excess glycogen and fat. This makes the liver work less well.
Amyloidosis: It is associated with abnormal proteins called amyloid that build up in organs like the liver, making them larger and impairing their function. In amyloidosis, a physical examination may reveal hepatomegaly, characterized by a swollen liver or spleen resulting from amyloid protein accumulation.
Hepatitis A: It is a virus that makes the liver swell and become inflamed, which can make it larger (hepatomegaly). The hepatitis A virus mainly spreads through food or water that has been contaminated, resulting in inflammation and damage to the liver.
Hepatitis B: It is a virus that attacks the hepatic cells and can cause liver inflammation that lasts for a short time or a long time. This can damage the liver and cause it to enlarge (hepatomegaly). Cirrhosis or liver cancer can happen as a result of chronic hepatitis B, which makes the liver enlarged.
Hepatitis C: It is a liver disease that happens when the hepatitis C virus damages and inflames liver tissue. This can cause the liver to enlarge (hepatomegaly). If chronic hepatitis C remains untreated, it can lead to cirrhosis, liver failure, or liver cancer, which can make the liver grow bigger.
Leukemia/lymphoma infiltration: Leukemia and lymphoma can result in hepatomegaly due to the infiltration and accumulation of malignant (cancerous) blood or lymphoid cells within liver tissue, causing liver enlargement. These blood cancers are known to cause an enlarged liver.
Nonalcoholic fatty liver disease (NAFLD) is associated with obesity: Obesity, specifically abdominal obesity, is a major risk factor for nonalcoholic fatty liver disease (NAFLD). Too much body fat makes the liver more insulin-resistant and promotes inflammation, leading to fat accumulation and liver enlargement. NAFLD affects about 60–90% of obese people, which shows that obesity is a major cause of fatty liver and hepatomegaly.
Hepatomegaly Complications
Patients with hepatomegaly may experience significant complications, depending upon the underlying liver condition and the extent of liver dysfunction. The following are some of the complications of hepatomegaly:
- Portal hypertension
- Ascites
- Spontaneous bacterial peritonitis
- Progression to cirrhosis and liver failure
- Gastrointestinal bleeding
- Coagulopathy and bleeding tendency
- Hematologic abnormalities
- Endocrine and hormonal disturbances
- Cardiovascular and renal consequences in advanced disease
- Hepatic encephalopathy
- Hepatocellular carcinoma or other liver malignancies in chronic liver disease/cirrhosis.
Portal hypertension: It is characterized by increased pressure within the portal venous system, resulting from increased resistance to portal blood flow, and is frequently associated with chronic liver diseases such as cirrhosis. It can cause serious problems like ascites, variceal bleeding, and hepatic encephalopathy.
Ascites: It is the abnormal buildup of fluid in the peritoneal cavity. This usually happens because of chronic liver disease and portal hypertension, which makes the abdomen swollen and damaged.
Spontaneous bacterial peritonitis: It is a bacterial infection of previously sterile ascitic fluid without a surgically treatable intra-abdominal source, constituting a severe complication of ascites in liver disease.
Progression to cirrhosis and liver failure: Chronic liver injury that results in ongoing hepatomegaly can induce fibrosis and scarring of liver tissue, ultimately advancing to cirrhosis, which disrupts normal liver architecture and function. As cirrhosis gets worse, the liver may not be able to perform important metabolic and detoxification functions, which can lead to liver failure.
Gastrointestinal bleeding: Chronic liver disease can lead to portal hypertension, which can make veins bigger (oesophageal or gastric varices). If these veins burst, they can cause severe upper gastrointestinal bleeding, which can be deadly.
Coagulopathy and bleeding tendency: The liver makes clotting factors, so if it is damaged, it can cause coagulopathy, which makes it hard for blood to clot and can lead to bleeding on its own or excessive bleeding. This tendency to bleed is a known problem that comes with advanced liver disease, like cirrhosis and liver failure.
Hematologic abnormalities: Advanced liver disease with hepatomegaly can lead to bleeding problems such as anaemia (low haemoglobin), leukopenia (low WBC count), and thrombocytopenia (low platelet count) because it impairs the body's ability to make blood cells or causes them to die faster. Liver dysfunction also causes coagulopathy, meaning the liver can't produce enough clotting factors, increasing the risk of bleeding.
Endocrine and hormonal disturbances: Cirrhosis or chronic liver disease can cause problems with the endocrine system, like glucose intolerance, insulin resistance, and thyroid hormone tests that show abnormal results. This is because the liver can't break down hormones properly. Hormonal problems are common, such as hypogonadism (low male hormones) and feminization in men, like gynecomastia (enlargement of breast tissue in males) and problems with periods or getting pregnant in women.
Cardiovascular and renal consequences in advanced disease: Advanced liver disease can lead to cardiovascular changes, such as cirrhotic cardiomyopathy and circulatory dysfunction, because of changes in blood flow and systemic blood vessel dilation, which makes circulation less effective. It can also lead to kidney failure, like in hepatorenal syndrome, where severe liver failure slows blood flow to the kidneys and causes kidney failure to get worse.
Hepatic encephalopathy: It is a neuropsychiatric disorder that arises when liver dysfunction permits the accumulation of toxins in the bloodstream, thereby impairing cerebral function. It can change a person's mental state, making them confused or changing their personality, or even progress to coma if their liver disease is severe or they have liver failure.
Hepatocellular carcinoma or other liver malignancies in chronic liver disease/cirrhosis: Chronic liver disease advances via fibrosis and cirrhosis, with hepatocellular carcinoma (HCC) emerging as a late-stage complication of chronic liver disease/cirrhosis.
Hepatomegaly Diagnosis
To diagnose hepatomegaly, doctors look for signs of liver enlargement and then imaging tests like an ultrasound or a CT scan are used to confirm the size of the liver and evaluate its causes. Liver function tests, which are blood tests, are used to check for liver damage and diseases that are related to it.
The following are the steps commonly included in the diagnostic criteria for hepatomegaly:
- Medical history
- Physical examination
- Laboratory tests
- Liver function test (LFT)
- Complete blood count (CBC)
- Viral hepatitis serology
- Coagulation profile (PT/INR)
- Serum electrolytes
- Serum blood glucose
- Autoimmune markers
- Tumor markers
- Imaging studies
- Ultrasound (USG)
- Computed tomography (CT) scan
- Magnetic resonance imaging (MRI)
- Advance tests
- Liver Biopsy or Elastography
Hepatomegaly Treatment
Medical management of hepatomegaly mainly focuses on treating the underlying causes, like infection, metabolic disorder, heart failure, or liver disease, to prevent the liver from getting larger and avoid problems. It also includes things that help, like changing lifestyle, taking medications, and monitoring liver function to make overall liver health better. Hepatomegaly therapy includes:
- Non-pharmacological therapy
- Pharmacological therapy
- Surgical intervention
Non-pharmacological therapy
- Identifying and removing triggers
- Quitting alcohol consumption
- Managing underlying conditions with lifestyle changes
- Losing weight through diet and physical activity
- Following a healthy, balanced diet
- Increasing physical activity/exercise regularly
Pharmacological therapy
- Antiviral therapy for viral hepatitis
- Nucleoside/nucleotide analogues
- Direct-acting antivirals
- Immunomodulatory (interferons) antivirals
- Medications for metabolic or autoimmune liver diseases
- Steroids
- Immunosuppressants
- Drugs for complications or associated conditions
- Diuretics
- Non-selective beta blockers
- Antibiotics
- Laxatives/Ammonia-lowering agents
- Vasoconstrictors
- Avoiding hepatotoxic drugs and substances
Surgical Intervention
- Liver transplant
- Resection or ablation
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support

Hepatomegaly Prevention
Prevention of hepatomegaly means keeping liver diseases and risk factors under control by living a healthy lifestyle, getting vaccinated, staying away from alcohol and drugs that are bad for liver health, and treating metabolic and infectious conditions early. The following measures are commonly recommended to prevent or minimize the development of hepatomegaly:
- Vaccination against hepatitis viruses
- Early testing and treatment of hepatitis B and C
- Avoiding unsafe injections, blood exposure, and high-risk behaviours
- Maintaining safe food and clean water hygiene
- Limiting alcohol consumption and avoiding hepatotoxic drugs/chemicals
- Adopting healthy lifestyle measures
Vaccination against hepatitis viruses: To avoid viral hepatitis infections and lower the risk of chronic liver disease and hepatomegaly complications, it is best to get safe and effective vaccines, especially for hepatitis A and B.
Early testing and treatment of hepatitis B and C: It helps to stop the disease from getting worse because finding it early means getting care and treatment right away, which can stop or slow down liver damage.
Avoiding unsafe injections, blood exposure, and high-risk behaviours: It is very important to use sterile, single-use needles and screened blood because unsafe injections or contaminated blood can spread hepatitis viruses (HBV/HCV), which can cause chronic liver disease and hepatomegaly. Avoiding high-risk behaviours like sharing needles can help stop the spread of blood-borne infections that damage the liver.
Maintaining safe food and clean water hygiene: It is essential to make sure people have access to clean, safe drinking water, good food handling, and good hygiene, which can help stop hepatitis A and E infections, which can cause liver inflammation and make the liver bigger (hepatomegaly).
Limiting alcohol consumption and avoiding hepatotoxic drugs/chemicals: Excessive alcohol intake and toxic drugs or chemicals can directly damage liver cells, leading to inflammation, scarring, and liver failure or cirrhosis. This is why it's important to limit alcohol intake and stay away from hepatotoxic substances.
Adopting healthy lifestyle measures: To prevent the progression of hepatic disease and lower the amount of fat in the liver, it is important to maintain a healthy weight, eat a balanced diet, exercise regularly, manage diabetes/ NAFLD and avoid drinking too much alcohol. This kind of lifestyle change helps to protect the liver and avoid problems that can arise from liver enlargement.
Difference between Hepatomegaly and Fatty Liver
Hepatomegaly vs fatty liver
The medical terminology for an enlarged liver is hepatomegaly. Fatty liver is a condition in which excessive fat accumulates (builds up) in the liver. It may or may not cause hepatomegaly. Below are the key differences between hepatomegaly and fatty liver.
| Features | Hepatomegaly | Fatty liver |
|---|---|---|
| Definition | It is defined as an enlarged liver beyond its normal size. | Fatty liver is a type of metabolic dysfunction-associated steatotic liver disease (MASLD) that is characterized by more than 5% hepatic steatosis, and associated risk factors include obesity, type 2 diabetes, or dyslipidemia. It can be as mild as simple steatosis or as severe as metabolic dysfunction-associated steatohepatitis (MASH). |
| Nature | Hepatomegaly is not a disease, but it is a sign of many different health problems, such as infections, tumours, metabolic disorders, and heart failure. | Hepatic steatosis (>5% fat in liver cells) is the main cause of MASLD, and it can progress from simple steatosis (which is usually not harmful) to MASH (which features inflammation, liver cell damage, and possible fibrosis). |
| Causes | There are many types of infections, parasites, tumours, anaemias, heart failure, and storage diseases. | Primarily metabolic: obesity, diabetes, high lipids; fat accumulation not related to alcohol. |
| Symptoms | Hepatomegaly remains asymptomatic when it is mild, but often exerts symptoms like abdominal pain or discomfort, bloating, jaundice, weakness, nausea, easy bruising, and itchy skin. | Often asymptomatic, mild symptoms include abdominal pain, fatigue and advanced symptoms include jaundice, leg swelling, abdominal swelling(ascites), itchy skin, unexplained weight loss, and |
| Relationship | Hepatomegaly can result from MASLD (especially MASH, which causes liver swelling), but also from many other conditions. MASLD/MASH may cause hepatomegaly, but diagnosis requires steatosis plus metabolic criteria, not just enlargement. | It may cause mild hepatomegaly, but fat content alone does not define fatty liver; the liver's size also matters. |
Frequently Asked Questions (FAQs) on Hepatomegaly
What is hepatomegaly?
An enlarged liver is called hepatomegaly. This means that the liver grows larger than it should. It's not a disease itself, but it is a sign of a health problem that could be anything from a mild infection to severe liver disease or heart failure. Some symptoms include tiredness, stomach pain, or jaundice.
What is mild hepatomegaly?
Mild hepatomegaly means the liver is slightly larger or swollen than normal and usually detected on physical examination or imaging, such as ultrasound. This is often an early sign of stress on the organ, not a disease. Fatty liver disease, drinking too much alcohol, hepatitis, or congestion are all common causes. It usually doesn't show any symptoms, but it can cause mild pain in the upper right abdomen or tiredness.
What are the symptoms of an enlarged liver?
Hepatomegaly is frequently asymptomatic (symptoms not present), particularly in the initial stages, with symptoms emerging from the underlying cause (e.g., liver disease, heart failure) such as pain, discomfort, pale/clay-colored stools, easy bruising/bleeding, or a feeling of fullness in the upper right abdomen. Common signs include tiredness/fatigue, weakness, jaundice (yellowing of the skin and eyes), nausea, and unexplained weight loss. It can also cause swelling in the abdomen (ascites), itchy skin, and urine that is darker than normal.
What is hepatomegaly with fatty liver?
Hepatomegaly with fatty liver means that the liver is too big (hepatomegaly) because there is too much fat in the liver cells (steatosis). This condition, which is often linked to obesity, diabetes, and metabolic syndrome, means that the liver is under stress and is swelling beyond its normal size. It can often be reversed by changing diet, exercise, and way of life.
Is hepatomegaly serious?
Hepatomegaly (enlarged liver) should be taken seriously because it may indicate a liver or systemic disease. Severity depends on the cause. It says that an enlarged liver could be a sign of serious problems or worsening liver damage, and that a doctor should evaluate it to identify the cause and preserve liver function.
Why does leukemia cause hepatomegaly?
Leukemia causes hepatomegaly, or an enlarged liver, mostly because leukemic (WBC) cells invade the liver tissue. When abnormal white blood cells made in the bone marrow move through the bloodstream, they can get stuck in the liver and spleen, causing them to swell. This buildup, along with increased extramedullary hematopoiesis (blood cell production outside the marrow) and possible blood flow obstruction, results in liver enlargement.
Is hepatomegaly fatal?
Hepatomegaly (an enlarged liver) is not fatal in itself; it can be a sign of other health problems like infections, metabolic disorders, or cancer. Most of the cases reflect that death can happen because of amyloidosis (buildup of amyloid proteins in the organs) or metastases (cancer that spreads throughout the body) that cause liver failure, not just because the liver gets enlarged. The prognosis (mortality risk) depends on early diagnosis and prompt treatment of the root cause.
What is the meaning of hepatomegaly?
The term hepatomegaly comes from Greek words. "Hepar" (or hepato-) means liver, and "megas" means large or enlargement, so hepatomegaly literally means "enlargement of the liver."
What are the causes of hepatomegaly?
Hepatomegaly (enlarged liver) can occur when the liver becomes inflamed, congested, or infected. Some examples of this are metabolic dysfunction-associated steatotic liver disease (MASLD), hepatitis, drinking too much alcohol, heart failure, and infections like malaria or infectious mononucleosis (caused by Epstein-Barr virus), cirrhosis, malignancies, or storage disorders. It often indicates a serious underlying condition that needs to be evaluated by a doctor.
What does it feel like when the liver is enlarged?
An enlarged liver usually doesn't show any signs, especially if it's not too bad. When noticeable, it may feel like a dull ache, fullness, discomfort, or pressure in the upper right abdomen; it may also feel tired, and it may present as nausea, vomiting, fatigue, or jaundice, depending on severity and cause. If these signs don't go away, consult a doctor immediately, as they may indicate other problems.
Can hepatomegaly go away on its own or be reversed?
Yes, hepatomegaly (an enlarged liver) can often be reversed or go away, especially if it is identified early and the underlying cause is treated. The liver can heal and grow back healthily by making changes in lifestyle, like eating a healthy diet, losing weight, exercising, and avoiding alcohol, which can reverse mild to moderate cases, especially fatty liver disease.
Does an enlarged liver cause weight gain?
An enlarged liver (hepatomegaly) does not directly cause weight gain, but it can contribute to weight gain when liver disease causes fluid to build up in the abdomen (ascites) or swelling elsewhere in the body. For example, cirrhosis can cause fluids to build up in the abdomen and legs, which can make the body look heavier and cause weight gain due to fluid retention instead of fat gain.
What is the difference between hepatomegaly and fatty liver?
An enlarged liver (hepatomegaly) is a sign of an underlying issue in which the liver exceeds its normal size. Fatty liver (hepatic steatosis) is a specific condition characterised by fat buildup in liver cells. A fatty liver is a common reason for an enlarged liver, but not all fatty livers are enlarged, and not all enlarged livers are caused by fat.
Can exercise be recommended in hepatomegaly?
Yes, exercise is a good way to manage liver enlargement (hepatomegaly) if it is caused by fatty liver or metabolic liver disease. It is recommended that doing aerobic exercise regularly (like walking, biking, or swimming) and resistance training can help lose weight, make the body more sensitive to insulin, and stop fat from building up in the liver, which can help stop liver disease from getting worse.
When to consult a doctor for hepatomegaly?
Consult a doctor for hepatomegaly if there is persistent pain or abdominal discomfort, unexplained fatigue, jaundice (yellowing of the skin or eyes), or swelling in the abdomen. See a doctor right away. Here are some signs that you need immediate medical attention:
- Unexplained weight loss or loss of appetite
- Feeling sick, throwing up, or having trouble digesting food
- Dark urine, pale stools, or skin that itches
- Bloating in the stomach or an enlarged spleen
If these symptoms persist, it's best to see a hepatologist (liver specialist) for an accurate diagnosis and treatment. Seek emergency medical attention if severe stomach pain, a fever, bloody vomit, or sudden confusion is experienced by the individual, as these may signal complications of liver failure. A general physician or hepatologist can provide the right hepatomegaly treatment to manage symptoms and reduce long-term risks.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868