NAFLD and NASH - Symptoms, Causes, Differences and Treatment
PACE Hospitals
About Liver
The liver is the largest full internal organ in the body. It is located under the rib cage in the upper right part of the abdomen. Although it varies in size with age, body size and shape, sex and disease state, it is roughly the size of a soccer ball in most adults. The liver has several important functions, such as:
- Works as a blood filter
- Metabolizes nutrients and other substances such as drugs
- Stores energy
- Synthesizes proteins essential for the function of our body, such as those which advise the blood to clot when we bleed.
Although the liver is a very resilient organ that has the ability to repair itself, it is susceptible to damage from many sources including viruses, toxins, inherited conditions, and even our own immune system.
NAFLD full form - Non Alcoholic Fatty Liver Disease
What is NAFLD?
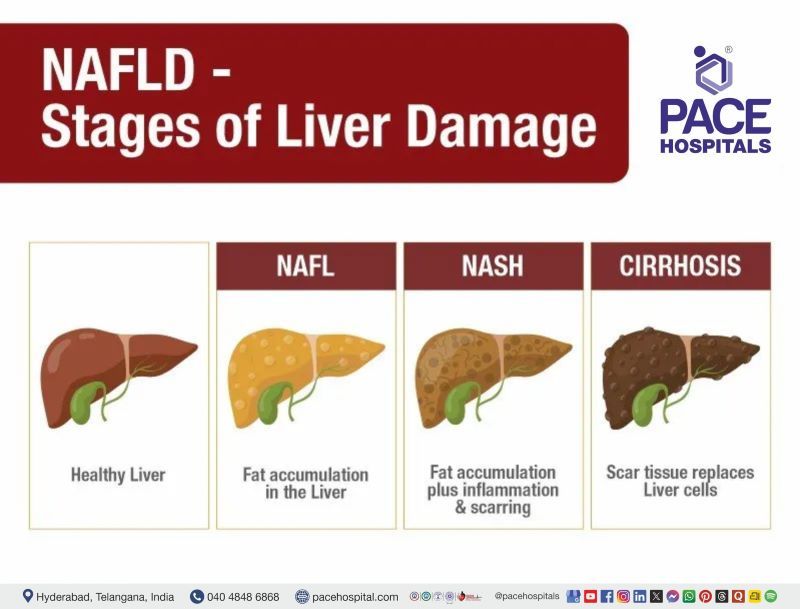
Non-alcoholic fatty liver disease (NAFLD) is a condition characterized by an accumulation of fat in liver cells (hepatocytes). Excess fat in the liver can lead to significant damage over the years. There are two types of NAFLD:
- Non-alcoholic fatty liver (NAFL)
- Non-alcoholic steatohepatitis (NASH)
NAFL (Non-alcoholic fatty liver) - It is a benign condition and in this fat is accumulated in the liver that can cause inflammation of liver but not a progressive damage or complications of the liver. This may result in abdominal discomfort or pain due to an enlarged liver (hepatomegaly).
NASH (Non-alcoholic steatohepatitis) – It is a malignant condition and in this fat is accumulated in the liver can cause scarring of liver, liver fibrosis and liver damage further it can cause cirrhosis of liver (also called as end-stage liver disease), further cirrhosis of the liver may lead to liver cancer.
Many people typically develop any type of NAFLD with having no symptoms; most of the time it is diagnosed by a healthcare professional or doctors by doing investigations for abnormal laboratory results or imaging test of the abdomen for unrelated problems.
In order to help people with this condition, doctor identify people those who all are at risk and offers advice on how to manage the condition before significant liver damage occurs. NAFLD is a condition that can be treated and often managed with lifestyle changes.
Prevalence of NAFLD (Nonalcoholic fatty liver disease)
Only a few researchers took a part and studied the prevalence of NAFLD in urban-rural regions of India. From the very limited data, NAFLD prevalence in India ranges vary from 8% to 54%. As per the studies urban population reported higher prevalence than the rural population. Due to very limited data and different regions, it is very difficult to define prevalence of NAFLD in India.
Non Alcoholic Fatty Liver Disease - NAFLD Causes
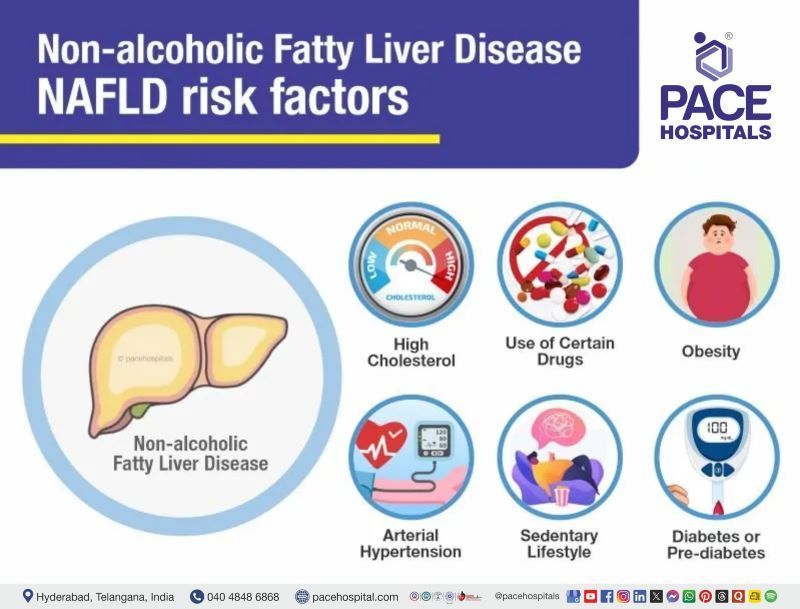
Non-alcoholic fatty liver disease (NAFLD) is not a condition that can be passed on (i.e., it does not spread from person to person). In fact, it occurs most often in people who have one or more of the following risk factors:
- Obesity
- Diabetes or prediabetes
- High cholesterol
- Arterial hypertension
- Sedentary lifestyle
- Use of certain drugs
The medical researchers still do not know the exact reason why NAFLD affects some people with the conditions listed above, but not others.
It is also poorly understood why in some people fat accumulates in the liver without causing significant damage (benign steatosis), while in other people it causes significant damage (non-alcoholic steatohepatitis - NASH).
Since the prevalence of this condition is increasing in INDIA, if you have one or more of the risk factors for the disease, it may be reasonable to discuss with your Hepatologist (Liver Specialist Doctor) whether you need evaluation or not. However, there are no specific-accepted guidelines for who should be further investigated for this condition, other than those with unexplained abnormalities in liver enzymes.
Non Alcoholic Fatty Liver Disease - NAFLD Symptoms
Many people with NAFLD do not have any symptoms, but in those who do, these are usually non-specific such as:
- Mild fatigue
- Discomfort or pain in upper right abdomen
Nonalcoholic Steatohepatitis – NASH Symptoms
Over the years, the presence of fat can trigger inflammation of the liver, which can lead to the formation of scar tissue. In an advanced state, the amount of scar tissue in the liver can reach a level called cirrhosis of the liver, which refers to the precise appearance of the scar tissue, liver fibrosis and its degree. In patients with NASH and cirrhosis of the liver can eventually lead to the appearance of signs and symptoms such as:
- Increased fatigue
- Buildup of fluid in the abdomen (ascites)
- Confusion (encephalopathy)
- A decreased or loss of appetite
- Bleeding easily or bruising (Ecchymosis)
- Nausea (an uneasiness of the stomach)
- Edema (Swelling in your feet, ankles or feet)
- Unexplained weight loss
- Yellow discoloration in the skin and eyes (jaundice)
- Esophageal varices - enlarged or swollen veins in the esophagus that can cause vomiting of blood, bloody or black tar-like stool
The goal of screening for NAFLD is to ensure adequate surveillance, offer treatment advice and decrease the chances of complications such as cryptogenic cirrhosis, hepatic transaminases, and cryptogenic hepatocellular carcinoma (HCC - common type of primary liver cancer).
Risk Factors of NAFLD - Non Alcoholic Fatty Liver Disease
There are many health conditions that can increase risk of NAFLD / NASH that includes:
- Abdominal obesity (excessive fat around the abdomen & stomach)
- Sleep apnea (breathing repeatedly stops and starts during sleep)
- Metabolic syndrome (high blood sugar, high blood pressure, excess body fat around the waist and abnormal cholesterol levels)
- High levels of cholesterol or triglycerides in the blood
- Polycystic ovary syndrome (PCOS)
- Type 2 diabetes
- Hypothyroidism (underactive thyroid)
- Hypopituitarism (deficiency of the pituitary hormones)
People those who are having any of the above-mentioned risk factors should go for liver function tests once in a year. To differentiate between NAFL and NASH, doctors may advise blood test, imaging tests and / or liver biopsy.
Complication of NAFLD - Nonalcoholic Fatty Liver Disease
NAFLD complications depends upon its type of condition, such as:
- In NAFL (Nonalcoholic Fatty Liver) people don’t develop any complications of liver
- In NASH (Nonalcoholic Steatohepatitis) people may develop complications of liver that includes end-stage liver disease (ESLD), cirrhosis of the liver, hepatic encephalopathy, liver fibrosis, ascites, esophageal varices and liver cancer.
People with NAFLD are at higher risk of developing certain health condition, such as:
- Type 2 diabetes
- Cardiovascular disease (CVD) - affecting the blood vessels or heart
- Metabolic syndrome (high blood sugar, high blood pressure, excess body fat around the waist and abnormal cholesterol levels)
Diagnosis of NAFLD and NASH
Initial stage it’s difficult to find out the NAFLD and NASH because of no symptoms. Usually, many patients fortuitously reported with liver problem while doing medical tests for other disease, medical ailments or conditions.
Doctors may advise some of these tests to identify severity of NAFLD / NASH.
Blood Tests: Doctors may advise these blood tests to identify NAFLD / NASH:
- CBP (Complete blood picture)
- Liver function tests
- Viral load tests and Genotype test for chronic viral hepatitis
- Genetic & Serology testing for celiac disease
- Hemoglobin A1C (HbA1c) test
- Lipid profile (for cholesterol and triglycerides levels)
- FibroTest and APRI (AST-to-Platelet Ratio Index)
Diagnostic imaging procedures:
- Abdominal Ultrasound
- Computerized tomography (CT) scan or Magnetic resonance imaging (MRI)
- Transient elastography (FibroScan)
Liver biopsy: It’s a type of liver tissue examination procedure in which a needle is used to remove a small piece of liver tissue for examination under a microscope, is the gold standard for diagnosing non-alcoholic fatty liver disease. Although currently the only way to confirm a diagnosis, in practice a combination of blood tests and imaging is usually sufficient to make the diagnosis in more than one patient.
The role of liver biopsy in the diagnosis of NAFLD, mainly NASH remains important in some circumstances, especially if the diagnosis is questionable. In addition, the biopsy can determine if there is scar tissue in the liver and its extent, if so.
Quantification is the process of determining the amount of scar tissue (fibrosis) in the liver; in the past, a liver biopsy was the only technique used. Normal tissue without scarring is found at stage 0. An increasing amount of scar tissue in the liver in combination with a change in its appearance increases the classification at a higher stage.
- Stage 1 is represented by a minimal amount of scar tissue
- Stage 4 refers to cirrhosis.
Although a biopsy is a safe procedure, it is invasive and therefore carries risks, including bleeding and pain after the procedure. Other than its invasive nature, one of the disadvantages of this procedure is that it only takes a sample from a very small section of a large organ and is therefore susceptible to sampling error.
Investigations
When a person is diagnosed with non-alcoholic fatty liver disease, it is important that they see a hepatologist doctor who has specialized knowledge in this area. It could be a nurse, a family doctor or a specialist (hepatologist or gastroenterologist doctor) who will undertake the initial investigations to ensure that the diagnosis is certain and to rule out other liver diseases that may coexist. Much of this information can be obtained from a physical examination, blood test, imaging of the abdomen and Liver tissue examination.
Non-invasive procedures for liver fibrosis
- Liver biopsy remains the gold standard for quantifying liver disease and is still a good option for many patients. However, health care providers are increasingly using other effective tools to determine the degree of fibrosis in the liver.
- FibroScan is a non-invasive technique used to assess the degree of fibrosis in the liver. This is a technique used to measure liver elasticity which is closely related to the degree of fibrosis in the liver. A probe is placed on the surface of the skin without causing pain, all of which is completed in a few minutes. The section sampled is approximately 100 times larger than that of a typical liver biopsy. This procedure gives a reliable reading in most people.
- FibroTest and APRI (AST-to-Platelet Ratio Index) are non-invasive technique that use calculations based on blood tests to measure the degree of fibrosis in the liver. FibroTest is likely not covered by health insurance plans and will therefore incur personal expenses. APRI is derived from the calculation of a simple equation based on common blood tests.
Regardless of the technique used to estimate the degree of fibrosis, expert interpretation is essential to ensure that the information obtained is useful in making treatment decisions. In addition, a liver biopsy can still provide valuable information regarding disease activity, which non-invasive tools could not.
Nonalcoholic Fatty Liver Disease - NAFLD Treatment
Doctors may advise patients with NAFLD to lose weight by following healthy diet, regular exercise and lifestyle as a 1st line of NAFLD treatment. People who are successful in losing weight equivalent to 3-10% of their total body weight by increasing their activity level and improving their diet are also successful in improving their liver enzymes and reducing the amount of fat accumulated in the liver.
Not all people with nonalcoholic fatty liver disease (NAFLD) will be at risk for developing active liver disease. However, since the management of this condition emphasizes a healthy lifestyle, it may also reduce the risk of developing cardiovascular disease.
- Alcohol: Heavy alcohol consumption is a known risk factor for the accumulation of fat in the liver. More than two drinks per day are generally considered heavy consumption. For a person with established NAFLD, limit ingestion to a maximum of two drinks per day (one drink is 148 mL of wine, 44 mL of spirits or 355 mL of beer) without consuming alcohol every day is a reasonable goal. In fact, complete abstinence from alcohol would be preferable.
- Other medical conditions: As already mentioned, other medical conditions such as high cholesterol, diabetes and high blood pressure increase the risk of developing NAFLD and may make it worse if it is already present. Optimal control of these risk factors is therefore essential for the management of NAFLD. Medicines typically used to treat these risk factors can usually be used safely by people with liver disease; patients should discuss this further with their health care provider.
- Medicines: As per the studies, many drugs, vitamins and supplements for beneficial effects that would be helpful in the management of NAFLD. Unfortunately, to date, no evidence has been found to support their universal and widespread use in people with this condition.
- Diet and lifestyle changes: Although research continues to find drugs that are suitable for widespread use in the management of NAFLD, many well-designed trials have shown that lifestyle changes (exercise and diet) that lead to weight loss are effective in the management of this disease.
The current Medical Society recommend that adults 18 to 64 years of age get at least 150 minutes of moderate to vigorous aerobic physical activity per week in sessions of at least 10 minutes, to achieve health benefits. This is also a reasonable goal for people with non-alcoholic fatty liver disease who are not already physically active at this level.
Limiting the consumption of foods high in fat and sugar, limiting portion sizes, and eating regular, balanced meals. Following the advice of a personal trainer or dietitian can also help you reach your goals.
Nonalcoholic steatohepatitis - NASH Treatment
Although nonalcoholic fatty liver disease is mild, if left untreated it can lead to a much more serious disease state, nonalcoholic steatohepatitis (NASH), which involves inflammation of the liver, scarring of the liver, liver fibrosis, cirrhosis of the liver and liver cancer.
Liver fibrosis can cause advanced scarring (cirrhosis) or cancer of the liver. About 20% of people diagnosed with NASH will develop cirrhosis, a serious problem that can cause many complications. In this condition, patients may require liver transplantations.
The future of non-alcoholic fatty liver disease (NAFLD) lies in raising awareness; it will allow hepatologist to determine which people have this condition in order to treat them.
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support
Lifestyle modifications to reverse NAFLD
People with Nonalcoholic fatty liver disease (NAFLD) can these steps to control and reverse it that includes:
- Healthy diet – Follow a healthy diet consist of whole grains, fruits, and leafy vegetables, especially rich in vitamin E.
- Weight loss
- Regular exercise and staying active
- Controlling diabetes
- Lower down the cholesterol
- Preventing liver damage
Difference between NAFLD and NASH | NAFLD vs NASH
Non-alcoholic fatty liver (NAFL) and Non-alcoholic steatohepatitis (NASH) are are types of Non alcoholic fatty liver disease NAFLD, indicated by the deposition of fats in liver and can be differentiated based on the damage done to the liver.
| NAFL (Nonalcoholic Fatty Liver) | NASH (Nonalcoholic Steatohepatitis) |
|---|---|
| Non-alcoholic fatty liver (NAFL) is type of NAFLD, happens due to accumulation of fats in liver. | Non-alcoholic steatohepatitis (NASH) is a severe form of NAFLD, associated with high level of fats accumulation in liver accompanied by Hepatitis infection. |
| Non-alcoholic fatty liver (NAFL) is also known as simple fatty liver, and usually it is reversible. | Non-alcoholic steatohepatitis (NASH) can be reversed but depends on its progression. |
| Non-alcoholic fatty liver (NAFL) doesn't cause inflammation and liver cell damage. | Non-alcoholic steatohepatitis (NASH) causes inflammation and liver cell damage due to hepatitis infection, which can lead to liver scarring (fibrosis). |
| Non-alcoholic fatty liver (NAFL) is not progressive in nature, does not lead to any severe complication. | Non-alcoholic steatohepatitis (NASH) can possibly lead to severe complications like Fibrosis, cirrhosis, liver cancer, liver failure. |
| Non-alcoholic fatty liver (NAFL) can be treated by losing 3-5% of body weight. | Inflammations of liver due to Non-alcoholic steatohepatitis (NASH) can be reduced by losing 7-10% of body weight. |
Frequently Asked Questions (FAQs) on NAFLD and NASH
What is NAFLD?
Non-Alcoholic Fatty Liver Disease (NAFLD) now called as Metabolic dysfunction-Associated Steatotic Liver Disease (MASLD) is a condition in which fat is accumulated in the liver of individuals who drink minimal or no alcohol. It is now one of the most common liver disorders worldwide and is closely linked to conditions such as obesity, type 2 diabetes, high cholesterol, and metabolic syndrome. NAFLD can range from simple fatty liver (without damage) to a more serious form called non-alcoholic steatohepatitis (NASH), which leads to inflammation and scarring of the liver. If not managed, it may progress to cirrhosis or liver failure over time.
Is NAFLD fatal?
Non-Alcoholic Fatty Liver Disease (NAFLD) is usually not fatal in its early stages, and many people live with simple fatty liver without any serious complications. However, it can develop into non-alcoholic steatohepatitis (NASH) in certain people, which can result in liver failure, liver cancer, or liver scarring (cirrhosis). The most common cause of death for these patients is heart disease, which is also associated with a higher risk of developing NAFLD. Early diagnosis and management can decrease the risk of severe outcomes.
How to differentiate between NAFLD and NASH?
NAFLD is a broad condition that includes simple fatty liver (NAFL) and the more severe form known as non-alcoholic steatohepatitis (NASH). The liver accumulates fat in NAFL, but there isn't any noticeable inflammation or damage to the liver cells. Fat is present in NASH along with inflammation and damage to the liver, which, over time, can result in cirrhosis and fibrosis. Clinical assessment, blood tests, imaging, and occasionally a liver biopsy to confirm inflammation and scarring provide the basis for differentiation.
How to reverse NAFLD?
NAFLD can often be improved and even reversed in the early stages with healthy lifestyle changes. Liver fat can be reduced by gradual weight loss, regular physical activities, and a balanced diet low in added sugars and saturated fats. Additionally, it is the effective management of associated conditions like diabetes, hypertension (high blood pressure) and high cholesterol. Patients can stop the progression of their illness and help in liver recovery by avoiding alcohol and following the doctor's advice.
Is NAFLD hereditary?
No, NAFLD is not directly inherited, but genetics can enhance a person’s risk of developing the condition. The way the body stores and breaks down fat in the liver can be affected by specific inherited genes. Fatty liver disease may be more likely to develop if there is a family history of NAFLD, obesity, or type 2 diabetes. But a lot of its development is influenced by lifestyle factors like weight, diet, and exercise.
Can NAFLD lead to cirrhosis?
Yes. Non-alcoholic fatty liver disease can progress over time to a severe form called non-alcoholic steatohepatitis (NASH), which causes liver inflammation and damage. This ongoing injury can lead to fibrosis (scarring) and eventually cirrhosis, which is permanent liver damage. Not everyone with NAFLD develops cirrhosis, but the risk increases if the condition is not managed.
Can NAFLD be prevented?
Yes. Healthy lifestyle choices can prevent non-alcoholic fatty liver disease (NAFLD). Maintaining regular physical activity, eating a well-balanced diet, managing portion sizes, and maintaining a healthy body weight help reduce the risk. Other important factors include preventing excessive weight gain and controlling diseases like diabetes and cholesterol. By taking these steps, the risk of fatty liver disease can be considerably reduced.
Is non alcoholic fatty liver disease common?
Yes. Non-alcoholic fatty liver disease (NAFLD) is the most common chronic liver condition worldwide. NAFLD affects a large proportion of adults, particularly in people with type 2 diabetes, obesity, or metabolic syndrome. It is increasingly seen in both adults and children due to rising rates of overweight and sedentary lifestyles. Many people may have NAFLD without symptoms and may not realise they have it.
What foods should be avoided in NAFLD?
People with NAFLD are advised to limit foods high in added sugars, such as sugary drinks, sweets, and refined carbohydrates. Foods like saturated fats and trans fats (processed fats), including fried foods, processed snacks, and red or processed meats, should also be reduced. High-salt and highly processed foods may worsen metabolic health and liver fat. A healthy, balanced diet, such as vegetables, fruits, lean protein and whole grains, helps liver health.
What causes non alcoholic fatty liver disease?
NAFLD is mainly caused by the body storing too much fat in the liver due to metabolic problems. The most common causes include obesity, type 2 diabetes, insulin resistance, high triglycerides and high cholesterol. Unhealthy diet (high in sugar, refined carbohydrates, and saturated fats) and lack of physical activity also contribute. Genetics and certain medical conditions can also lead to an increased risk. These factors lead to fat buildup in the liver even in people who do not drink alcohol.
Can stress cause NAFLD?
Non-alcoholic fatty liver disease is not directly caused by stress. However, long-term stress can result in unhealthy behaviors that raise the risk of NAFLD, such as poor dietary habits, lack of exercise, weight gain, and poor management of diabetes or cholesterol. Stress can also worsen insulin resistance, which leads to the deposition of fat in the liver. Improved liver health is supported by stress management and a healthy lifestyle.
How to know if NAFLD is getting worse?
NAFLD may worsen silently, but certain changes may be a sign of progression. There may be persistent right-upper abdominal pain, weakness, increasing fatigue, or unexpected weight loss. Warning signs in advanced stages include easy bruising, jaundice (yellowing of the skin or eyes), and swelling of the legs or abdomen. To identify progression early, routine liver health monitoring and medical follow-up are essential.
Can NAFLD lead to vitamin deficiencies?
Vitamin deficiencies usually do not occur in early-stage NAFLD. However, the liver might not properly process and store nutrients if the disease worsens and results in cirrhosis or advanced liver damage. Deficiencies in specific vitamins, particularly fat-soluble vitamins like A, D, E, and K, may result from this. Complications can be reduced with a proper diet and routine checkups with a physician.
Is dark urine a sign of NAFLD?
Dark urine is not usually a sign of early NAFLD. Most people with non-alcoholic fatty liver disease have no symptoms in the early stages. However, in advanced liver disease or cirrhosis, dark urine may occur due to jaundice (a buildup of bilirubin). If dark urine is noticed along with yellowing of the eyes or skin, medical evaluation is recommended.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868