Successful Sentinel Pile Excision for Chronic Anal Fissure with Bleeding
PACE Hospitals
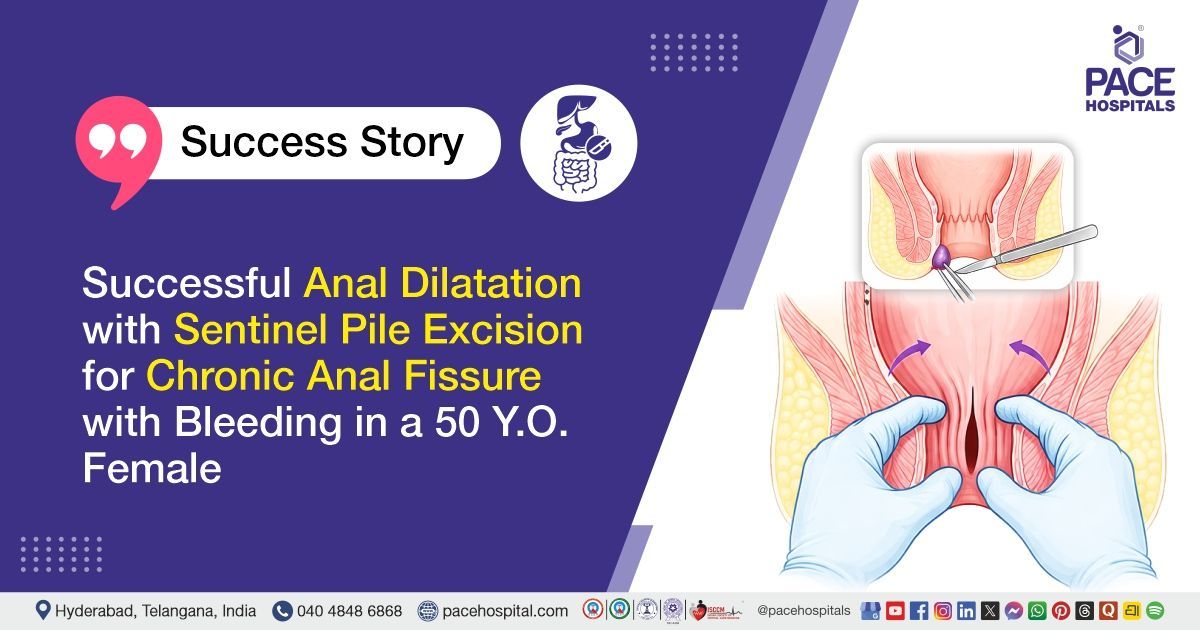
PACE Hospitals’ expert Surgical Gastroenterology team successfully performed manual anal dilatation with sentinel pile excision on a 50-year-old female patient diagnosed with chronic fissure in ano. The aim of the procedure was to relieve anal sphincter spasm, reduce pain during defecation, improve blood flow to promote fissure healing, remove the associated sentinel pile, and prevent recurrence.
Chief Complaints
A 50-year-old female patient with a body mass index (BMI) of 19 presented to the Surgical Gastroenterology Department at PACE Hospitals, Hitech City, Hyderabad, with a history of painful defecation, bleeding per rectum, and intermittent constipation for the past two years. The pain was sharp in nature and occurred during defecation. The bleeding was noted as streaks smearing the stool. She had been on medical treatment for these symptoms, with only partial relief.
Past Medical History
The patient had no known comorbidities such as diabetes mellitus, hypertension, or other chronic systemic illnesses. She had no history of prior perianal surgeries or similar anorectal conditions. She was not on any long-term medications and had no significant past medical history contributing to her present condition.
On Examination
On examination, the patient was conscious, coherent, and oriented, and was hemodynamically stable. General physical examination revealed no significant abnormalities, and there was no pallor, icterus, cyanosis, clubbing, or pedal edema. Abdominal examination showed a soft, non-tender abdomen with no palpable masses or organomegaly, and bowel sounds were normal. Perianal examination (under anesthesia findings) revealed a chronic anal fissure in the posterior midline at the 6 o’clock position with an associated sentinel skin tag, along with increased anal sphincter tone prior to dilatation. No other anorectal abnormalities were noted.
Diagnosis
Upon admission to PACE Hospitals, the patient was thoroughly evaluated by the Surgical Gastroenterology team. She presented with a history of painful defecation, bleeding per rectum, and intermittent constipation for the past two years, with pain being sharp in nature and occurring during defecation. The bleeding was described as streaking the stool and was associated with significant discomfort. The patient had been on conservative medical management earlier, with only partial symptomatic relief.
The clinical presentation was suggestive of a chronic anal fissure in ano, likely associated with persistent internal sphincter spasm and formation of a sentinel skin tag due to long-standing disease. Further evaluation and perianal examination confirmed the presence of a chronic fissure in the posterior midline (6 o’clock position) with an associated sentinel pile.
Based on the clinical findings and confirmed diagnosis, the patient was advised to undergo Chronic Anal Fissure Treatment in Hyderabad, India, under the expert care of the Surgical Gastroenterology Department, aimed at relieving sphincter spasm, reducing pain during defecation, promoting healing of the fissure, and preventing recurrence.
Medical Decision Making (MDM)
After a detailed consultation with Dr. CH Madhusudan, Senior Consultant Surgical Gastroenterologist and Liver Transplant Surgeon, along with the team, including Dr. Suresh Kumar S, Consultant Surgical Gastroenterologist, a comprehensive evaluation was carried out considering the patient’s clinical symptoms of long-standing painful defecation, bleeding per rectum, and intermittent constipation, along with all relevant laboratory investigations. The findings were consistent with a diagnosis of chronic anal fissure in ano with associated sentinel pile formation, confirmed on perianal examination.
Based on the clinical presentation and examination findings, it was determined that Manual Anal Dilatation with Sentinel Pile Excision as the most appropriate therapeutic intervention. This decision was made with the intent to relieve internal anal sphincter spasm, reduce pain during defecation, improve local blood flow to facilitate fissure healing, excise the associated sentinel pile, and prevent recurrence of symptoms.
The patient and her family members were counselled regarding the diagnosis, the planned procedure, potential risks and benefits, postoperative care including dietary modifications and sitz bath, expected recovery course, and the importance of follow-up for optimal outcomes.
Surgical Procedure
Following the decision, the patient was scheduled to undergo Manual Anal Dilatation with Sentinel Pile Excision Surgery in Hyderabad at PACE Hospitals, under the expert care of the Surgical Gastroenterology Department.
The procedure involved the following steps:
- Patient Preparation and Positioning: The patient was taken to the operating room after obtaining informed consent and completing pre-anesthetic evaluation. Under appropriate anesthesia, the patient was positioned in the lithotomy position, ensuring proper exposure of the perianal region. Standard aseptic and antiseptic precautions were followed, and the surgical field was draped.
- Examination Under Anesthesia (EUA): A careful perianal examination under anesthesia was performed. A chronic anal fissure was identified in the posterior midline at the 6 o’clock position, along with an associated sentinel skin tag (sentinel pile). No additional anorectal pathology was noted.
- Sentinel Pile Excision: The sentinel pile/skin tag associated with the chronic fissure was carefully grasped and excised using appropriate surgical instruments. Hemostasis was achieved to prevent bleeding, and the excised tissue was managed as per standard protocol.
- Manual Anal Dilatation: Gradual manual anal dilatation was performed in a controlled manner to reduce internal anal sphincter spasm. The anal canal was gently stretched until two fingers could be easily admitted, ensuring adequate relaxation of the sphincter without causing trauma.
- Hemostasis, Final Check, and Completion: The surgical site was thoroughly inspected to ensure no active bleeding or complications. Hemostasis was confirmed, and the area was cleaned and dressed. The procedure was completed successfully and was uneventful, after which the patient was shifted to the recovery room for observation.
Postoperative Care
The procedure was uneventful. Postoperatively, the patient developed headache and vomiting, which were managed conservatively. A neurology opinion was obtained in view of the associated tingling sensation and persistent headache, and appropriate evaluation and recommendations were followed. The patient improved with conservative management and was discharged in a hemodynamically stable condition with the advised postoperative care and follow-up instructions.
Discharge Medications
The patient was discharged with medications prescribed for postoperative care, including agents to prevent infection, reduce pain and inflammation, provide gastric protection, and ensure bowel softening to avoid straining during defecation. Additional supportive medications were advised on an as-needed basis for management of breakthrough pain and associated symptoms.
Advice on Discharge
The patient was advised to follow a high-fiber diet to maintain soft stools and prevent constipation. She was also instructed to take sitz baths three times daily to promote local hygiene, reduce discomfort, and aid in postoperative healing.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms such as Fever, pain, bleeding at the site, vomiting, or chest pain.
Review and Follow-up Notes
The patient was advised to return for a follow-up visit with the
Surgical Gastroenterologist in Hyderabad at PACE Hospitals, after 3 days, to review her condition.
Conclusion
This case highlights a chronic fissure in ano managed successfully with manual anal dilatation and sentinel pile excision. The procedure was uneventful, and the postoperative course remained stable with conservative management of transient symptoms. The patient showed good clinical recovery and was discharged in a hemodynamically stable condition. She was advised of dietary modifications, a sitz bath, and regular follow-up for further evaluation.
Chronic Anal Fissure Managed by a Surgical Gastroenterologist
Chronic anal fissure is a painful anorectal condition primarily caused by persistent internal anal sphincter spasm, leading to reduced blood flow and impaired healing. In this case, a surgical gastroenterologist / surgical gastroenterology doctor opted for a sphincter-relaxing approach through manual anal dilatation combined with sentinel pile excision to address the underlying pathology. The procedure helps break the cycle of pain, spasm, and ischemia, thereby promoting effective fissure healing and symptom relief.
Excision of the sentinel pile improves local hygiene and removes chronically inflamed tissue associated with long-standing disease. Postoperative recovery is generally smooth when constipation is well controlled through dietary modifications and stool softening measures. Sitz baths further aid in reducing local inflammation and enhancing patient comfort during the healing phase. Overall, this case demonstrates the effectiveness of targeted surgical gastroenterology intervention in managing chronic fissure in ano and preventing recurrence.
Frequently Asked Questions (FAQs)
Is manual anal dilatation an effective treatment for chronic fissure in ano?
Manual anal dilatation can help in some cases by relaxing the tight muscle around the anus. This reduces pain and allows the fissure to heal better. It is usually done when medicines do not give enough relief. The procedure is simple, and many patients feel better after it. However, it is not used as often now because other treatments give more reliable results.
When is sentinel pile excision recommended along with fissure treatment?
Sentinel pile excision is done when there is a small skin tag near the fissure. This tag can cause discomfort and make cleaning difficult. Removing it helps the area heal better and reduces irritation. It is commonly done in long-standing fissure cases. The doctor decides this after examining the area.
How long does it take to recover after anal dilatation and fissure surgery?
Most patients start feeling better within 1 to 2 weeks. Pain and discomfort slowly reduce during this time. Complete healing may take around 3 to 4 weeks. Daily activities can usually be resumed within a few days. Eating properly and keeping stools soft helps in faster recovery.
What is the success rate of manual anal dilatation in chronic fissure cases?
Many patients get good relief from pain after this procedure. It helps the fissure heal by reducing muscle tightness. But in some cases, the fissure can come back again. Results are better when proper care is taken after the procedure. Nowadays, other treatments are preferred as they give more consistent results.
Can a chronic fissure in ano come back after surgical treatment?
Yes, it can come back if proper care is not followed. Constipation and straining are the main reasons for recurrence. Keeping stools soft by eating fiber-rich food and drinking enough water helps prevent this. Regular follow-up is useful to catch early signs. Long-term care is important to avoid the problem again.
What precautions are required after fissure surgery to prevent recurrence?
Eating a fiber-rich diet and drinking plenty of water is very important. This helps avoid constipation and reduces strain during bowel movements. Taking warm sitz baths can give relief and help healing. Keeping the area clean is also necessary. Regular check-ups help ensure everything is healing well.
How does manual anal dilatation compare with lateral internal sphincterotomy?
Manual dilatation is a simple method and does not involve cutting the muscle. However, the results are not always consistent. Lateral internal sphincterotomy is more effective and has a lower chance of recurrence. That is why it is more commonly used now. The choice depends on the patient’s condition and the doctor’s advice.
What type of diet helps in faster healing after fissure surgery?
Foods rich in fibre, like fruits, vegetables, and whole grains, are very helpful. Drinking enough water keeps stools soft and easy to pass. Avoiding spicy and junk foods can reduce irritation. Light and simple meals are better during recovery. A good diet plays a big role in healing.
When can normal bowel habits return after fissure surgery?
Bowel movements usually become normal within a few days. Some discomfort may be felt during the first few times. Medicines and a proper diet make passing stools easier. Within 1 to 2 weeks, things generally return to normal. Avoiding straining is important during this period.
What complications should be monitored after an anal dilatation procedure?
Some pain or mild bleeding can happen after the procedure. In a few cases, there may be difficulty in controlling gas for a short time. Headache or vomiting can occur if spinal anesthesia was used. Fever or increasing pain should not be ignored. If anything unusual is noticed, medical advice should be taken early.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868