Cranioplasty Surgery, Procedure and Cost
PACE Hospitals offers advanced cranioplasty surgery in Hyderabad, India, focusing on the reconstruction and restoration of skull defects caused by trauma, prior brain surgery, congenital conditions, or infections. Our expert neurosurgeons perform titanium mesh cranioplasty, autologous cranioplasty, and other advanced techniques to restore skull integrity, protect the brain, and improve both function and appearance.
With a strong emphasis on precise diagnosis, customized surgical planning, and patient-focused care, we ensure safe outcomes, faster recovery, and improved neurological and cosmetic results for enhanced quality of life.
Book an Appointment for Cranioplasty Surgery
Cranioplasty Surgery Appointment
Why Choose PACE Hospitals for Cranioplasty Procedure?
Expert Neurosurgeons Specializing in Safe Cranioplasty for Skull Reconstruction & Trauma Repair
Minimally Invasive Cranioplasty procedure with Advanced Materials, Small Incisions & Faster Recovery
Transparent Cranioplasty Surgery with Insurance & Cashless Options
Cranioplasty Surgery
A cranioplasty surgery is a common neurosurgical procedure performed to repair or reconstruct defects or deformities in the skull, often resulting from injury (traumatic brain injury), surgery (previous brain surgery), or congenital abnormalities. The procedure involves the use of various materials, such as autologous bone grafts, metal plates, or synthetic materials, to improve the appearance of the skull and restore the integrity in both cosmetic and functional aspects.
Cranioplasty procedure is typically performed by neurosurgeons. These healthcare professionals are trained to evaluate, examine and manage conditions involving the brain and skull, including the reconstruction of cranial defects following trauma, surgery, or congenital abnormalities.
In more complex cases-especially those requiring customized implants or cosmetic considerations-a multidisciplinary team may be involved. This can include craniofacial or plastic surgeons, radiologists, and rehabilitation specialists. However, the primary responsibility for the procedure and decision-making lies with the neurosurgeon.
Types of Cranioplasty
Different types of Cranioplasty that are categorized by the material used to repair the skull defects are mentioned below:
- Autologous Bone Cranioplasty
- Alloplastic Cranioplasty
- Titanium Mesh Cranioplasty
- Polyetheretherketone (PEEK) Cranioplasty
- Polymethyl Methacrylate (PMMA) Cranioplasty
- Custom 3D-Printed Cranioplasty Implants
Autologous Bone Cranioplasty (Using Patient’s Own Bone)
Autologous cranioplasty utilizes the patient's own bone flap, usually preserved after decompressive craniectomy, for skull reconstruction. It is preferred due to excellent biocompatibility and cost-effectiveness. But certain risks include bone resorption and infection. Various preservation techniques and timing influence outcomes, with long-term success reported in multiple studies.
Alloplastic Cranioplasty (Using Synthetic Materials)
Alloplastic cranioplasty is done using synthetic materials when autologous bone is unavailable or unsuitable. These cranioplasty materials are chosen for their structural durability, customizability, and biocompatibility. Major common synthetic options include:
- Titanium Mesh Cranioplasty: Titanium is strong and highly biocompatible, making it one of the most popular choices for mesh implants in cranioplasty. It provides excellent skull protection with a low risk of infection and implant rejection. Its mesh design allows for flexible contouring to fit the cranial defect precisely.
- Polyetheretherketone (PEEK) Cranioplasty: Polyetheretherketone (PEEK) is a good durable, lightweight polymer known for its excellent biocompatibility. Often custom-made using 3D printing, PEEK implants offer precise anatomical fitting and radiolucency, making them suitable for complex skull reconstructions with minimal risks and outcomes.
- Polymethyl Methacrylate (PMMA) Cranioplasty: PMMA is an acrylic polymer widely used for cranioplasty implants due to its customizability and ease of molding feature. While effective, PMMA implants may have a higher risk of infection compared to titanium or PEEK and require careful surgical technique.
Custom 3D-Printed Cranioplasty Implants
Cranioplasty 3D printing technology allows the creation of patient-specific implants that fit precisely to the skull defect. Using 3D reconstruction from CT scans, these implants offer improved anatomical accuracy and better cosmetic outcomes. It is commonly made from materials like titanium or PEEK, 3D-printed cranioplasty implants reduce surgical time, enhance recovery, and lower complication rates. This advanced method makes cranioplasty more efficient and personalized.
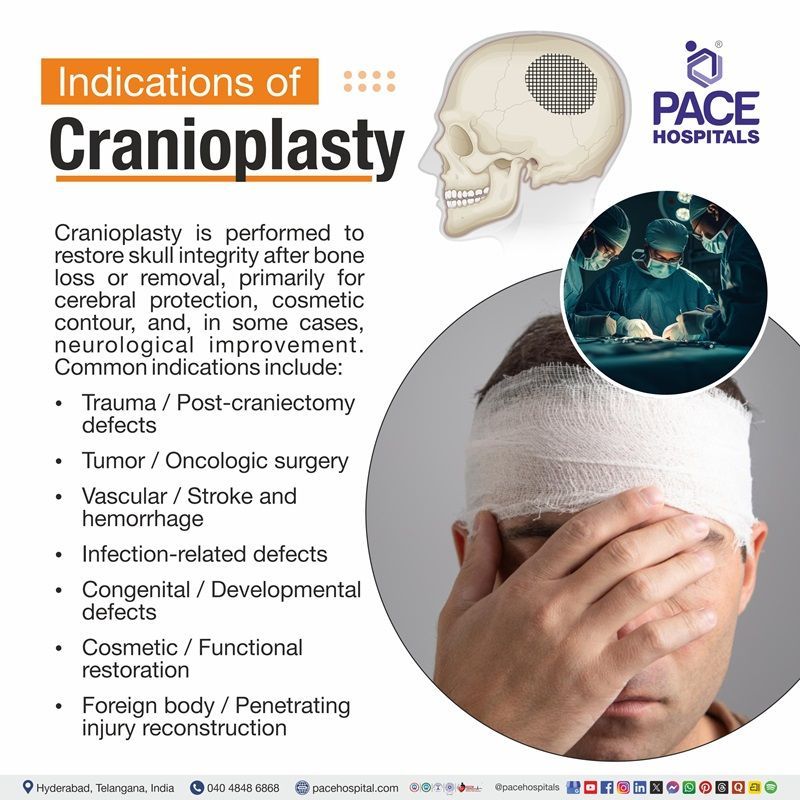
Cranioplasty Indications
Cranioplasty surgery is performed to restore skull integrity after bone loss or removal - primarily for cerebral protection, cosmetic contour, and, in selected patients, neurological improvement (e.g., “syndrome of the trephined”). The most common trigger is a prior decompressive craniectomy for trauma or stroke; other causes include tumor surgery, infection, congenital defects, and penetrating injuries. The following are the detailed conditions that can come under the cranioplasty surgery indications:
- Trauma / post-craniectomy defects
- Tumor / Oncologic surgery
- Vascular / Stroke and hemorrhage
- Infection-related indications
- Congenital / Developmental defects
- Cosmetic / Functional restoration
- Foreign body / Penetrating injury reconstruction
Trauma / post-craniectomy defects
After decompressive craniectomy for traumatic brain injury (TBI), cranioplasty is performed once swelling subsides to protect the brain, restore skull contour, and potentially improve cognition and motor function. Traumatic cranial defects, such as depressed fractures or bone loss from injuries, are repaired by closing skull gaps created during life-saving surgery.
Tumor / Oncologic surgery
Cranioplasty replaces bone removed for tumor resection (benign or malignant) to restore cranial protection and appearance.
Vascular / Stroke and hemorrhage
Reconstruction follows craniectomy for malignant ischemic stroke or hemorrhage once the patient stabilizes.
Infection-related indications
Delayed cranioplasty occurs after removal of infected bone flaps post-craniotomy infection, once infection is cleared.
Congenital / Developmental defects
Certain congenital cranial defects or deformities are reconstructed to protect the brain and improve cosmetic contour, distinct from craniosynostosis correction.
Cosmetic / Functional restoration
Cranioplasty helps to correct visible skull deformities, improves psychosocial well-being, and may enhance neurological function by normalizing cerebrospinal fluid dynamics, alleviating "syndrome of the trephined."
Foreign body / Penetrating injury reconstruction
Skull reconstruction follows the extraction or stabilization of intracranial foreign bodies after penetrating injuries when clinically safe.
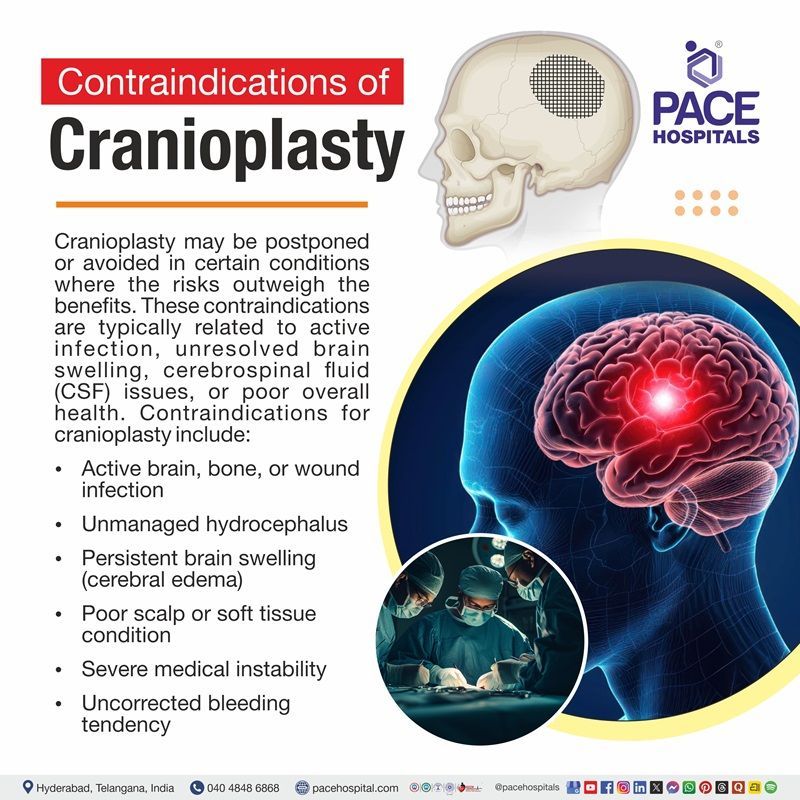
Cranioplasty Contraindications
Cranioplasty may be avoided or delayed in certain conditions where the risk of surgery is higher than the expected benefit. These contraindications are mainly accompanied by and related to active infection, unresolved brain swelling, disturbed cerebrospinal fluid dynamics, or poor overall surgical readiness. Contraindications for cranioplasty include:
- Active brain, bone, or wound infection
- Unmanaged hydrocephalus
- Persistent brain swelling (cerebral edema)
- Poor scalp or soft tissue condition
- Severe medical instability
- Uncorrected bleeding tendency
Active brain, bone, or wound infection
Cranioplasty is usually postponed when there is an active infection involving the brain, skull bone, or surgical wound. Reconstructing the skull in the presence of infection can increase the chance of implant contamination, wound breakdown, and serious postoperative complications. Infection is treated first, and reconstruction is considered only after the infection is adequately controlled.
Unmanaged hydrocephalus
Hydrocephalus is one of the main reasons to delay cranioplasty. If cerebrospinal fluid pressure is not properly controlled, the reconstructed bone or implant may not sit well, and the risk of complications can increase. In many patients, hydrocephalus needs to be treated first, often with CSF diversion, before cranioplasty is planned.
Persistent brain swelling (cerebral edema)
Cranioplasty is generally avoided when the brain is still swollen. Replacing the skull too early in the setting of ongoing cerebral edema can worsen pressure effects and may lead to poor neurological outcomes. Surgery is usually delayed until swelling has subsided and the brain condition is more stable.
Poor scalp or soft tissue condition
If the scalp is fragile, poorly healed, scarred, ulcerated, or unable to provide adequate coverage, cranioplasty may need to be postponed. Weak soft tissue coverage increases the risk of wound dehiscence, implant exposure, and infection. In such cases, the scalp condition may need correction before definitive skull reconstruction.
Severe medical instability
Patients who are medically unstable may not tolerate another major neurosurgical procedure safely. Cranioplasty is often delayed until the patient's general condition improves and perioperative risks are better controlled. This is especially important in patients recovering from severe brain injury or prolonged ICU care.
Uncorrected bleeding tendency
A bleeding disorder or uncorrected coagulopathy can increase the risk of excessive bleeding during and after cranioplasty. Before surgery, coagulation problems are usually corrected to reduce the risk of hematoma, wound complications, and reoperation. Until then, cranioplasty may be deferred. This is a standard surgical precaution reflected in neurosurgical perioperative practice.
Cranioplasty Benefits
Cranioplasty is more than a cosmetic repair of skull defects. It restores cranial protection, improves cerebral physiology, enhances neurological recovery, and positively impacts quality of life. The following are the key benefits of cranioplasty:
- Cerebral protection
- Neurological improvement
- Cerebrospinal Fluid and Hemodynamic Restoration
- Psychological and Cosmetic Benefits
- Reduced Dependency and Improved Quality of Life
Cerebral protection
Cranioplasty helps to get back the skull's barrier function, protecting the brain from trauma, external pressure, and atmospheric influences. This mechanical protection is required for safeguarding the brain post-craniectomy
.
Neurological improvement
Cranioplasty often leads to enhancement in coordination, motor function, memory, and concentration. These neurological benefits are partly attributed to the normalization of cerebral blood flow and cerebrospinal fluid (CSF) dynamics after skull reconstruction. Symptoms such as fatigue, dizziness, headache, and cognitive decline frequently improve postoperatively.
Cerebrospinal Fluid and Hemodynamic Restoration
Cranioplasty normalizes CSF circulation and intracranial pressure regulation, which helps to reduce complications like post-craniectomy hydrocephalus. Studies show increased cerebral blood flow to both ipsilateral and contralateral hemispheres following cranioplasty, contributing to better cerebral hemodynamics.
Psychological and Cosmetic Benefits
Restoration of the skull contour through cranioplasty surgery improves visible deformities, which significantly enhance psychological well-being, including self-esteem, social reintegration, and overall quality of life. The cosmetic aspect remains an important consideration for patient satisfaction beyond functional recovery.
Reduced Dependency and Improved Quality of Life
Some evidence demonstrates that cranioplasty reduces long-term disability and dependency, enabling many patients to resume daily activities and, in some cases, return to work. Improved cerebral protection and neurological function contribute to enhanced rehabilitation potential.
Need More Clarity on Skull Reconstruction Surgery?
Get a free second opinion from experienced neurosurgeons.
At PACE Hospitals, we are committed to providing our patients with the best possible care, and that includes offering second medical opinions with super specialists for treatment or surgery. We recommend everyone to get an expert advance medical second opinion, before taking decision for your treatment or surgery.
Cranioplasty Procedure Steps
The neurosurgery team follows the steps below for performing cranioplasty:
Before Cranioplasty surgery
- Pre-operative evaluation & imaging: Before undergoing cranioplasty, patients are carefully assessed for neurological status, scalp and soft-tissue condition, history of prior infections, and the presence of shunts. Imaging, such as Computed Tomography (CT) or Magnetic Resonance Imaging (MRI), is performed to evaluate defects and residual brain swelling. The timing of surgery is often individualized, though many centers consider 3–6 months after decompressive craniectomy as appropriate.
- Risk discussion & consent: The patients and families are counseled on the objectives of surgery, which include restoring brain protection, improving skull contour, and potentially enhancing neurological recovery. They are also informed about possible risks, such as infection, hematoma, hydrocephalus, bone flap resorption, implant failure, and seizures.
- Infection screening & wound readiness: The surgical team ensures that the scalp and surrounding soft tissues are healthy before proceeding. Surgery is postponed if there is evidence of active infection or poor wound healing capacity.
- Cranioplasty Material planning: A decision is made between using the patient’s preserved bone flap or an artificial implant such as Polymethyl Methacrylate (PMMA), Polyetheretherketone (PEEK), or titanium. This choice depends on the important factors including the size of the defect, the condition of stored bone, and patient-specific considerations.
- Anesthesia planning: Cranioplasty surgery is performed under general anesthesia. Enhanced recovery protocols are planned, which may include multimodal pain management, strategies for reducing nausea, early mobilization, and venous thromboembolism prophylaxis according to neurosurgical guidelines.
- Antibiotic prophylaxis: To reduce the risk of infection, peri-operative antibiotics are administered in line with neurosurgical standards and adjusted according to the patient’s allergy profile and institutional policy.
During Cranioplasty surgery
- Anesthesia & positioning: Cranioplasty is performed under general anesthesia, with the patient being positioned to provide optimal exposure of the cranial defect. Careful padding protects pressure points, and lines and monitors are secured to prevent injury during surgery.
- Incision and exposure: The previous scalp incision is reopened when feasible or new scalp flaps are designed for robust, well-vascularized coverage. Buccal and temporalis muscles are elevated carefully to preserve tissue blood supply and avoid devascularization, all done in careful manner.
- Dural & epidural preparation: Adhesions between dura and bone edges are lysed, bleeding is controlled, and a clean epidural plane is created to reduce hematoma formation post-surgery.
- Implant/bone-flap preparation: Autologous bone is inspected for viability, with nonviable edges debrided and contouring performed for optimal fit. Alloplastic implants such as PMMA, PEEK, or titanium are patient-specific or shaped intraoperatively, fixed with plates and screws to ensure flush contour and stability.
- Watertight dural management as needed: Cerebrospinal fluid leaks are repaired, and dural augmentation is performed when necessary to reduce the risk of postoperative fluid collections.
- Hemostasis & drains: Meticulous hemostasis is achieved, and subgaleal or epidural drains are placed as indicated to minimize hematoma and seroma formation.
- Layered closure: Muscle, fascia, and skin layers are carefully re-approximated and closed in a tension-free manner to provide well-perfused coverage over the implant, promoting optimal healing.
After Cranioplasty surgery
- Immediate monitoring: After cranioplasty, patients are closely observed for neurological status, wound condition, and drain output. Postoperative imaging, such as CT scans, is obtained if clinically indicated to assess for hematoma or implant malposition.
- Pain control & Enhanced recovery after surgery (ERAS) care: Multimodal analgesia is employed to manage postoperative pain effectively. Early mobilization is encouraged as part of enhanced recovery after surgery (ERAS) protocols to promote healing and reduce complications.
- Antibiotics & wound care: Perioperative antibiotics are continued as per protocol, and standardized incision care- such as gentle cleansing, clot removal, and hair care around the incision - is practiced reducing the risk of surgical site infections.
- Deep Vein Thrombosis (DVT) prophylaxis: Mechanical methods like compression stockings and pharmacologic prophylaxis are applied according to neurosurgical judgment to prevent deep vein thrombosis safely.
- Activity & recovery: Patients are advised a gradual return to self-care and ambulation while avoiding strenuous activities until cleared. Protection of the operative site from trauma is essential, along with education on recognizing signs of infection or fluid collection.
- Follow-up: Drains and sutures are removed per protocol. Patients are monitored for issues such as headaches, seizures, swelling, or neurological changes, and follow-up imaging and clinical review are planned.
Cranioplasty Complications
Cranioplasty, though beneficial for cerebral protection, neurological recovery, and cosmetic restoration, is also associated with a range of complications. These may include problems related to wound healing, infection, implanted material, seizures, and systemic issues. The following are the major complications of cranioplasty:
- Infectious complications
- Wound and healing problems
- Implant-Related problems
- Neurological complications (Hemorrhage and brain edema)
- Seizures/new-onset epilepsy
- Timing-related considerations (early vs. late cranioplasty)
Infectious complications
Surgical site infections (SSIs) are among the most frequent complications and may necessitate prolonged antibiotic treatment or removal of the implant. Bone flap infections or osteomyelitis are particularly seen with autologous bone grafts used in cranioplasty, leading to flap loss.
Wound and healing problems
Wound dehiscence can expose the implant, increasing the chances of infection risks. Skin flap necrosis may develop due to poor blood supply or tension in scalp tissue around the cranioplasty site, sometimes requiring surgical revision. Seromas or hematomas-collections of fluid or blood beneath the scalp flap-are also reported postoperative complications.
Implant-Related problem
Bone flap resorption is common in younger patients undergoing autologous cranioplasty, causing recurrent skull defects and often demanding reoperation. Synthetic implants can loosen or migrate if improperly secured during cranioplasty. Although rare, implant fractures or mechanical failures have been reported with materials like PMMA or titanium mesh. Some patients may develop foreign body reactions to synthetic cranioplasty materials, leading to inflammation.
Neurological complications (Hemorrhage and brain edema)
Postoperative seizures may occur due to cortical irritation or scarring related to cranioplasty. Epidural or subdural hematomas beneath the implant are recognized complications requiring urgent management. Some patients may develop hydrocephalus after cranioplasty, characterized by ventricular enlargement, may necessitate CSF shunting to relieve intracranial pressure.
Seizures/new-onset epilepsy
New seizures after cranioplasty (NOSAC) are documented; rare but severe refractory cases are reported, sometimes associated with drainage/pressure changes or edema.
Timing-related considerations (early vs. late cranioplasty)
Timing-related considerations for cranioplasty remain debated. Some analyses show no significant difference in overall complication rates between early and late cranioplasty. However, early cranioplasty (within 90 days) may be associated with a higher risk of cerebrospinal fluid (CSF)-related complications such as hydrocephalus. Given the mixed evidence, timing decisions should be individualized based on patient factors and clinical context of a person affected by it.
In certain conditions, cranioplasty risks include infection that may require antibiotic treatment, stroke, postoperative blood clots needing drainage, seizures, and clots in the legs, which can rarely travel to the lungs. Additional complications although not directly related to the surgery itself can include pneumonia, heart attack, and urinary infection. Discussing these risks thoroughly with the surgeon is essential before undergoing cranioplasty.
Cranioplasty Surgery Recovery Time
Although recovery times vary depending on individual patient factors, most patients undergo cranioplasty approximately 3 to 6 months after decompressive craniectomy. Early cranioplasty (within 12 weeks) has been shown to be as safe as later procedures, with no significant difference in complication rates based upon some of studies. Postoperatively, neurological improvements and functional recovery often begin within weeks, with benefits extending over months. Early surgery may decrease operative time and support faster neurological recovery. Rehabilitation and neuropsychological improvement continue progressively, with some studies reporting cognitive and motor improvements within 40 days after cranioplasty. Strict individualization of timing based on patient condition is recommended to optimize outcomes.
Questions that the patients can ask the healthcare team about Cranioplasty?
- When can I go home after cranioplasty?
- When do I need to return for follow-up visits?
- What kind of pain or discomfort should I expect after cranioplasty surgery?
- When can I resume my regular daily activities?
- How long is the expected recovery time after cranioplasty?
- What precautions should I take to protect my head after the operation?
- What problems or complications can occur after cranioplasty?
- Will the implant or bone flap be permanent, or could it need replacement?
- When can I safely return to work, exercise, or sports?
- Are there any dietary restrictions after cranioplasty?
- What signs of infection or wound problems should I watch for?
- Do I need to continue taking medications (such as anti-seizure or blood thinners) after surgery?
- Will cranioplasty improve my neurological function or only protect my brain?
- How often will I need follow-up scans or imaging after the procedure?
Difference Between Craniotomy and Cranioplasty
Craniotomy vs cranioplasty
Craniotomy and cranioplasty are two different neurosurgical procedures often performed at separate stages of patient care. A craniotomy involves temporarily removing a bone flap to access the brain for treatment of conditions such as tumors, vascular malformations, or hematomas, and the bone is usually replaced at the end of surgery. In contrast, a cranioplasty is performed to repair a skull defect, most commonly after a previous craniectomy, with the aim of restoring skull protection, cosmetic appearance, and, in many cases, improving cerebral hemodynamics and neurological recovery. Below are some key parameters that differentiate craniotomy from cranioplasty.
| Parameter | Craniotomy | Cranioplasty |
|---|---|---|
| Meaning / Purpose | A craniotomy is a procedure in which a bone flap is temporarily removed to access the brain for operations such as tumor removal, hematoma evacuation, or vascular surgery. | Cranioplasty is the surgical reconstruction of a skull defect (often following a prior craniectomy) to restore protection, contour, and possibly improve cerebral dynamics. |
| Bone flap management | The bone flap is generally replaced at the end of the same operation. | The bone or implant is placed later (or during the same surgery if bone was preserved) to close the defect. |
| Timing in surgical workflow | Usually part of an initial neurosurgical intervention. | Performed as a secondary or delayed reconstruction procedure after brain swelling subsides (i.e. after decompressive craniectomy). |
| Risks / complications | Risks include bleeding, brain injury, infection, CSF leaks, and general surgical risks. | Risks overlap (infection, hemorrhage, implant failure, bone resorption, CSF disturbances) but also include unique challenges of reconstructing skull defects. |
| Relation to craniectomy | Craniotomy sometimes is converted to craniectomy if bone is not replaced (e.g. in swelling) | Directly follows craniectomy in many cases; cranioplasty repairs the defect left by craniectomy. |
| Impact on patient outcome / recovery | The primary goal is immediate intracranial intervention; recovery depends heavily on the underlying brain condition. | Aims to restore skull integrity, improve cerebral hemodynamics, mitigate “syndrome of the trephined,” and possibly aid neurological recovery. |
Craniectomy vs Craniotomy vs Cranioplasty
Craniectomy: A craniectomy resembles a craniotomy in that both involve removing a portion of the skull. However, the key distinction is that in a craniotomy the bone flap is replaced at the end of the procedure, while in a craniectomy the bone is deliberately left out, usually to allow the brain room to swell or to manage increased intracranial pressure.
Craniotomy: A craniotomy is one of the most frequently performed neurosurgical procedures, often carried out to remove brain tumors. It may also be indicated for evacuating a hematoma (blood clot), managing bleeding caused by a cerebral aneurysm, repairing vascular malformations such as arteriovenous malformations, draining abscesses, relieving intracranial pressure, obtaining a brain biopsy, or directly inspecting brain tissue.
Cranioplasty: A cranioplasty is performed to reconstruct or repair a skull defect or irregularity. This is commonly required after head trauma or as a secondary procedure following prior surgeries such as a craniectomy or craniotomy. To restore the skull’s protective barrier and normal contour, the surgeon may use the patient’s preserved bone or an artificial implant made of materials like titanium, PMMA, or PEEK.
Cranioplasty Surgery Cost in Hyderabad, India
The cost of Cranioplasty Surgery in Hyderabad generally ranges from ₹1,50,000 to ₹5,50,000 and above (approx. US $1,805 – US $6,630).
The exact cost of cranioplasty surgery depends on the type of cranioplasty (autologous vs. synthetic materials), the size and location of the skull defect, the complexity of the procedure, and whether additional reconstructive surgery is required. Additional factors include preoperative imaging (CT, MRI), hospital stay duration, ICU care, and postoperative rehabilitation. The use of advanced surgical materials like titanium or custom implants may also influence the cost. Availability of cashless treatment options, TPA corporate tie-ups, and insurance assistance may further affect expenses.
Cost Breakdown According to Type of Cranioplasty Surgery
- Autologous Cranioplasty (Using Patient’s Own Bone Flap) – ₹1,50,000 – ₹3,00,000 (US $1,805 – US $3,610)
- Synthetic Cranioplasty (Using Materials Like Titanium or PEEK) – ₹2,00,000 – ₹4,00,000 (US $2,410 – US $4,820)
- Custom Implant Cranioplasty (3D-Printed or Preformed Implants) – ₹3,00,000 – ₹5,00,000 (US $3,610 – US $6,020)
- Cranioplasty with Additional Reconstructive Surgery (e.g., Facial Reconstruction) – ₹4,00,000 – ₹7,00,000 (US $4,820 – US $8,410)
- Post-Traumatic Cranioplasty (After Severe Head Injury) – ₹2,50,000 – ₹6,00,000+ (US $3,010 – US $7,230+)
Frequently Asked Questions (FAQs) on Cranioplasty
What to expect after cranioplasty?
After cranioplasty, patients are closely monitored for neurological signs, wound healing, and possible complications (e.g., infection, hematoma, CSF collections). Many patients show improvements in motor, cognitive, and language function over the months following the surgery, especially if surgery is done early and conditions are optimal. However, cranioplasty carries a nontrivial rate of complications; in one single-center series, about 10.3% of patients had postoperative infection, and other risks included minor complications and hydrocephalus.
Which Is the best hospital for Cranioplasty Surgery in Hyderabad, India?
PACE Hospitals, Hyderabad, is a trusted centre for advanced neurosurgery and cranial reconstruction procedures, including cranioplasty surgery.
We have highly experienced neurosurgeons, craniofacial surgeons, anesthesiologists, and rehabilitation teams who follow evidence-based protocols to perform cranioplasty surgeries with a focus on functional and aesthetic recovery. Whether the procedure is autologous or synthetic, our experts ensure minimal invasiveness, effective healing, and optimal results.
We mange complicated cases and have excellent facilities including state-of-the-art modular operation theatres, advanced imaging systems (CT, MRI), 3D printing technologies, and titanium implants, PACE Hospitals ensures precise and patient-centred cranioplasty surgery.
Can cranioplasty improve brain function?
Yes, several studies have found improvements in brain functioning through correct brain movement, cognition, and overall function following cranioplasty, which is most likely due to improved intracranial physiology once the skull is rebuilt. Gains typically take months to manifest, and the outcome is determined on the underlying brain injury and following recovery.
What Is the cost of Cranioplasty Surgery at PACE Hospitals, Hyderabad?
At PACE Hospitals, Hyderabad, the cost of cranioplasty surgery typically ranges from ₹1,80,000 to ₹5,00,000 and above (approx. US $2,170 – US $6,020), making it a cost-effective and competitive option for cranial reconstruction in Hyderabad. However, the final cost depends on:
- Type of cranioplasty (autologous vs. synthetic vs. custom implants)
- Size and location of the skull defect
- Complexity of the procedure (whether additional facial reconstruction is needed)
- Need for preoperative imaging (CT, MRI) and 3D modelling
- Duration of hospital stay and postoperative care
- Specialist consultations and follow-up care
For standard cranioplasty procedures, costs remain toward the lower end, while custom implants or complex surgeries may fall toward the higher range.
After a detailed neurological and craniofacial evaluation, our specialists provide a transparent cost estimate tailored to the patient’s needs and recovery goals.
How long does recovery take, and when can a person get back to normal activities after cranioplasty?
Recovery from cranioplasty is gradually observed process. However, many patients can resume mild activities within weeks, but full recovery may take many months, depending on the primary brain damage, comorbidities, and other therapy demands. To guarantee safe progress, the surgical team will provide personalized counsel on exercise, employment, and driving, as well as plan follow-up appointments.
Can cranioplasty be done in children?
Yes, cranioplasty surgery is also performed in children, but pediatric cases require special planning and additional care because bone resorption is more frequent, and skull growth must be considered carefully. Synthetic implants are sometimes favored to lessen complications, and long-term follow-up is necessary.
Looking for the best Cranioplasty Surgery Hospital Near Me?
If you’re searching for the top cranioplasty surgery hospital near me in areas like HITEC City, Madhapur, Kondapur, Gachibowli, Kukatpally, or KPHB, it is important to choose a hospital with experienced neurosurgeons and advanced cranial reconstruction technologies.
Effective cranioplasty surgery requires:
- Accurate diagnosis with imaging (CT, MRI) and 3D modelling
- Advanced surgical techniques with minimal tissue disruption
- Use of high-quality implants (titanium, PEEK, or custom-made implants)
- Postoperative care and rehabilitation to support recovery
At PACE Hospitals, Hyderabad, patients receive comprehensive care with cutting-edge technologies and specialized care to restore both function and aesthetics after cranial injury or surgery.
What is cranioplasty?
Cranioplasty is the surgical reconstruction of a defect or deformity in the skull vault, using either the patient’s own bone flap or artificial materials (metal, plastic, composite) to restore protection, contour, and normal intracranial dynamics. In patients who previously underwent decompressive craniectomy, cranioplasty aims not only to repair the skull but also to improve cerebral blood flow, cerebrospinal fluid regulation, and potentially neurological function.
Can nerves get damaged after cranioplasty surgery?
While nerve injury is not always explicitly emphasized in cranioplasty post-surgery, manipulation of scalp, pericranial, and temporalis muscles (which contain nerve branches) may contribute to soft tissue or muscular injury, especially during flap elevation or fixation. One known issue after cranial surgeries (craniotomy or cranioplasty) is temporal hollowing, which may be due to atrophy or denervation of the temporalis muscle (nerve, vessel, or direct injury) after surgery, affecting facial contour.
Can a person get swelling on the face after cranioplasty surgery?
Yes, soft tissue swelling over or around the incision site is common postoperatively because of surgical manipulation, edema, and vascular response in scalp/flap tissues may be observed after cranioplasty surgery. Although not always phrased as "facial swelling," wound and subgaleal swelling are well documented as postoperative phenomena. In some reports, the manipulation of the temporalis muscle and adjacent tissues during cranioplasty can contribute to changes in contour, soft-tissue depression or bulging, which might be noticeable in the face or temple region.
When to do cranioplasty?
Cranioplasty is usually performed 3 to 6 months after decompressive craniectomy, once brain swelling has subsided and the wound is healthy. Earlier surgery may help neurological recovery but can increase infection risk, while delayed surgery reduces infection risk but may lead to bone resorption or more scarring. The exact timing should be individualized based on the patient’s condition and surgical safety.
Why is cranioplasty performed after a decompressive craniectomy?
After a craniectomy, the skull has an opening that protects the brain less well and can disturb normal pressure/flow inside the head. Cranioplasty closes that opening, restoring the skull's barrier and often improving symptoms linked to "sinking skin flap" physiology. But, several reviews emphasize benefits in protection, contour, and potential improvements in cerebral physiology and function.
What cranioplasty materials are used for the repair?
If the original bone flap is available and acceptable, it may be used; otherwise, neurosurgeons use modern implants such as titanium or high-grade polymers tailored to your skull. The choice is based on defect size, infection risk, cosmetic goals, and your medical status, with several series outlining the benefits and drawbacks of each alternative.
Will the face or scalp look swollen or different after surgery?
Some swelling around the incision and nearby facial areas is common early on and typically settles with healing. A known longer-term issue after some cranial surgeries is temporal hollowing (a contour depression near the temple) from muscle/bone changes; surgeons use techniques to minimize it, and reconstructive options exist if needed.
Can nerves be injured during cranioplasty?
Cranioplasty involves lifting and repositioning scalp and muscle, which contain small sensory and motor nerve branches. Certain meticulous technique aims to protect these structures, but temporary numbness or contour changes (e.g., related to temporalis muscle handling) can occur and usually improve; targeted techniques can further reduce risk and any other related complications.
How long will a patient stay in the hospital after cranioplasty?
Most patients remain hospitalized for a few days after cranioplasty to allow close monitoring of neurological function, wound healing, and potential complications. In some series, length of stay is extended in cases with comorbidities or if complications like infection or hydrocephalus develop.
Does a person need rehabilitation after cranioplasty?
Rehabilitation is often recommended after cranioplasty, particularly for patients with neurological deficits from their original injury. Studies report that motor and cognitive improvements may continue for months after skull reconstruction, and structured rehabilitation enhances recovery.
Is Cranioplasty Surgery Covered by Insurance at PACE Hospitals?
Yes, cranioplasty surgery is generally covered under most health insurance policies at PACE Hospitals, subject to policy terms and approval. Since cranioplasty is a medically necessary procedure for conditions like traumatic brain injury or congenital defects, it is typically included under neurological and surgical coverage in private insurance and corporate health plans.
At PACE Hospitals, patients can benefit from:
- Cashless hospitalization facilities with empaneled insurance providers
- Assistance from a dedicated insurance and TPA coordination team
- Pre-authorization support and documentation guidance
- Transparent cost estimates before admission
- Support for government health schemes where applicable
Coverage depends on pre-existing condition clauses, sum insured limits, surgical coverage, and policy inclusions. Patients are encouraged to share insurance details in advance so the hospital’s insurance desk can verify eligibility and streamline approvals.
Why choose PACE Hospitals?
- A Multi-Super Speciality Hospital.
- NABH, NABL, NBE & NABH - Nursing Excellence accreditation.
- State-of-the-art Liver and Kidney transplant centre.
- Empanelled with all TPAs for smooth cashless benefits.
- Centralized HIMS (Hospital Information System).
- Computerized health records available via website.
- Minimum waiting time for Inpatient and Outpatient.
- Round-the-clock guidance from highly qualified super specialist doctors, surgeons and physicians.
- Standardization of ethical medical care.
- 24X7 Outpatient & Inpatient Pharmacy Services.
- State-of-the-art operation theaters.
- Intensive Care Units (Surgical and Medical) with ISO-9001 accreditation.




