Bone Fractures: Types, Symptoms, Causes & Treatment
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. Raghuram - Orthopaedic Consultant, Trauma, Shoulder and Knee Arthroscopic Surgeon, Hip and Knee Joint Replacement Specialist
Overview |
Epidemiology |
Types |
Pathophysiology |
Symptoms |
Causes |
Risk Factors |
Complications |
Diagnosis |
Treatment |
Prevention |
Colles Fracture vs Smith Fracture |
Sprain vs Fracture |
FAQs |
When to consult a Doctor
Fracture definition
A fracture is a break in a bone that is either partial or complete. It occurs when the force applied to the bone is stronger than the bone's strength. In most cases, fractures can occur because of injuries like falls, accidents, repetitive stress, direct blows or diseases like osteoporosis that make bones weaker. Common symptoms include sudden pain, swelling, deformity, inability to move the affected area, and bruising. The diagnosis is based on a person's medical history and physical examination. Imaging tests such as X-rays, CT scans, or MRIs confirm the diagnosis. If untreated, complications can include delayed or non-healing, infection, joint stiffness, deformity (malunion), and loss of function.
An orthopaedic surgeon (orthopedist), trauma surgeon, emergency medicine doctor, or musculoskeletal specialist trained in managing bone injuries can accurately diagnose a fracture and provide appropriate treatment, including fracture reduction, immobilization, or surgery when required.
Fracture meaning
The word fracture is derived from the Latin word:
- “Fractura’’ refers to a “breach, break, cleft’’
So, "fracture" means "a break in a bone," which is the main sign of the condition: a disruption in the bone's continuity caused by trauma, excessive force, stress, or an underlying bone disease.
Fracture Epidemiology
Fracture epidemiology worldwide
The Global Burden of Disease study reflects that the number of fractures worldwide is increasing. In 2021, there were 17. 279 crores new cases, and this number is expected to continue rising as the population ages. The number of prevalent cases reported was about 45.331 crores. Overall, age-adjusted rates are declining, but fractures of the lower extremities, pelvis, and femur are increasing.
Fracture epidemiology in India
Based on data up to early 2025, the epidemiology of fractures in India, encompassing both incidence and prevalence, exhibits a distinct profile relative to Western countries, marked by a significant prevalence of trauma among young, working-age males, coupled with a swiftly increasing occurrence of fragility fractures in the older population.
Types of Fractures
There are different types of fractures based on the pattern, cause, and severity of the bone break. This helps clinicians make accurate diagnoses and treatment. The following are the different types of fractures:
On the basis of:
Etiology
- Traumatic fracture
- Pathological fracture
- Stress fracture/hairline fracture
Skin Involvement (Communication)
- Closed fracture
- Open fracture
Pattern/Configuration
1. Simple fracture
- Transverse fracture
- Oblique fracture
- Spiral fracture
2. Multifragmentary
- Wedge (partial articular, complete articular, or extra-articular fracture)
- Complex (comminuted) fracture
- Segmental fracture
3. Other patterns
- Avulsion fracture
- Compression fracture
- Greenstick (pediatric) fracture
Alignment
- Nondisplaced fracture
- Displaced (Translation, angulation, rotation, shortening)
Location (by bone/anatomic segment)
1. Upper bone fracture
- Clavicle fracture
- Proximal humerus fracture
- Distal radius fracture (e.g., Colles fracture)
2. Lower bone fracture
- Femoral neck fracture
- Shaft fracture
- Tibial plateau fracture
- Ankle (bimalleolar) fracture
3. Axial fracture
- Spine (compression/burst) fracture
- Pelvis (acetabular) fracture
Special/pediatric fractures
- Plastic deformation fracture
- Buckle/torus fracture
Eponyms fractures
- Monteggia fracture
- Galeazzi fracture
Etiology
Fractures can occur for several reasons, including physical trauma or weakened bones from disease or repeated stress.
- Traumatic fracture: A break in a bone caused by a physical force from outside the body, like a fall, a car accident, or a direct blow. When the force applied is stronger than the bone's strength, this happens in a normal, healthy bone.
- Pathological fracture: A fracture that happens in a bone that is already weak because of diseases like osteoporosis, infection, or cancer. It can happen with little or no trauma because the bones are less strong.
- Stress fracture /hairline fracture: A small crack in a bone that happens when it is put under too much mechanical stress or overused. It is often seen in athletes or people who suddenly start working out more.
Skin involvement (communication)
When a fracture affects the skin, it is very important to assess the severity and plan treatment, influencing both infection risk and the healing process.
- Closed fracture: The bone is broken, but the skin that covers it is still intact and not exposed to the outside environment. There is no way for the fracture site to communicate with the external environment.
- Open fracture: The broken bone is connected to the external environment by a wound in the skin. It has a high risk of infection and requires immediate treatment by a healthcare professional.
Pattern/configuration
Simple fracture
A simple fracture, or closed fracture, is a break in a bone where the skin over the break stays intact, and there is no connection between the break and the external environment.
- Transverse fracture: The line of the fracture goes across the long axis of the bone. It usually occurs when something hits it directly or bends it.
- Oblique fracture: The line of the fracture goes across the bone at an angle. A force that is not directly applied at an angle is usually what causes it.
- Spiral fracture: The fracture line goes around the bone because of a twisting action. It is often associated with injuries caused by bone twisting.
Multifragmentary
When a bone breaks into several pieces, it is called a multifragmentary fracture. These pieces can form complicated or segmental patterns, which can make the bone less stable and slow healing.
- Wedge (partial articular, complete articular, or extra-articular fracture): The bone is broken into three pieces, with a triangular wedge piece in between the main pieces. Depending on the type of fracture, it could affect the articular or extra-articular areas.
- Complex (comminuted) fracture: The bone is broken into many pieces, usually more than three. It occurs when a lot of energy is involved, and it is usually unstable.
- Segmental fracture: Two separate fracture lines separate a piece of bone. This results in a free bone fragment with a disrupted blood supply.
Other patterns
Other patterns of fractures can occur when bones are pulled apart suddenly or when pressure causes bones to collapse.
- Avulsion fracture: A tendon or ligament pulls a piece of bone off during a sudden, strong contraction. It usually happens where muscles or ligaments are strongly attached.
- Compression fracture: This occurs when a bone fractures under pressure, typically in the vertebral bodies. It is often linked to osteoporosis or injuries from axial loading.
- Greenstick (pediatric) fracture: An incomplete fracture in which one side of the bone bends and the other side breaks. It occurs in children because their bones are still growing and are flexible.
Alignment
Alignment in fractures refers to the broken bone pieces being lined up in relation to each other. This affects the fracture's stability and its treatment.
- Nondisplaced fracture: A nondisplaced fracture means the bone pieces remain in their normal anatomical position even though they are broken. The alignment stays the same, and the fracture may be stable.
- Displaced fracture: The bone pieces are not in their normal position because they have moved. Sliding (translation), bending (angulation), twisting (rotation), or overlapping (shortening) can all be components of displacement and are usually less stable and often require reduction (realignment).
Location (by bone/anatomic segment)
Upper bone fracture
Upper bone fractures, like those of the clavicle, proximal humerus, and distal radius, are common injuries that can occur due to a fall or injury. They often need careful treatment to heal properly and restore mobility.
- Clavicle fracture: A broken collarbone usually happens when an individual falls on their shoulder or outstretched hand. It most often happens in the middle of the shaft. It causes pain, swelling, and deformity over the collarbone and is usually treated conservatively.
- Proximal humerus fracture: Fracture of the upper end of the humerus near the shoulder, often seen in the elderly after falls or in high-energy trauma. It is categorized by displaced segments (head, tuberosities (refers to a rounded, usually prominent projection or bump on a bone, typically serving as a site for muscle or ligament attachment), and shaft) and may affect shoulder mobility.
- Distal radius fracture (Colles fracture): A fracture of the distal end of the radius usually occurs during a fall on an outstretched hand. A Colles fracture occurs when the distal fragment moves backwards, causing a "dinner fork" deformity.
Lower bone fracture
Fractures of the lower body, such as those of the femoral neck, shaft, tibial plateau, and ankle, are common injuries that can occur for a variety of reasons. They can cause severe pain and difficulty with movement.
- Femoral neck fracture: Older adults often break their femoral necks because of osteoporosis or a fall from low energy. It can impair blood flow to the femoral head, leading to complications such as avascular necrosis.
- Shaft fracture: A fracture that happens along the diaphysis (shaft) of long bones like the femur or tibia, usually because of a high-energy injury. These fractures usually involve significant movement and pain and require stabilization.
- Tibial plateau fracture: A fracture of the upper surface of the tibia that affects the knee joint, usually caused by axial loading or trauma. It can cause joint instability and cartilage damage, and it needs to be carefully aligned with the body.
- Ankle (bimalleolar) fracture: A fracture that affects both the medial and lateral malleoli of the ankle, which usually happens when the ankle twists. This kind makes the ankle unstable and usually needs surgery to fix it properly.
Axial fracture
Axial fractures, which can be either compression or burst types, are serious injuries that affect the spine and pelvis. They are often caused by high-impact forces or by conditions that weaken bones, such as osteoporosis.
- Spine (compression/burst) fracture: When axial load causes vertebral bodies to collapse, this is called a compression fracture. This happens a lot in people with osteoporosis. Burst fractures are worse because they break up the vertebral body and may affect the spinal cord.
- Pelvis (acetabular) fracture: Fracture of the acetabulum (hip socket) is usually caused by high-energy trauma such as car accidents. It affects the hip joint's stability and may require surgery.
Special/pediatric fractures
Pediatric fractures frequently differ from adult fractures, necessitating specialized care due to the unique bone flexibility and growth patterns in children.
- Plastic deformation fracture: Children can have an incomplete fracture, in which the bone bends without breaking. This is because the bone is flexible. It might not show up well on an X-ray, but if left untreated, it can cause functional deformity.
- Buckle (torus) fracture: A stable incomplete fracture caused by compression that makes one side of the cortex bulge. A common injury in children usually heals well with just immobilization.
Eponyms fractures
Eponymous fractures are named after people who first described or characterized them. These names often point to specific injury patterns that require quick, specialized treatment.
- Monteggia fracture: Fracture of the proximal ulna accompanied by dislocation of the radial head at the elbow joint. It usually occurs when it falls onto an outstretched hand or is hit directly, and it needs to be treated immediately.
- Galeazzi fracture: A break in the distal or middle third of the radius and a dislocation of the distal radioulnar joint. Most of the time, it occurs during the fall on an outstretched hand, and surgery is often required to fix it.
Pathophysiology of Fracture
Fractures occur when excessive force breaks a bone, changing its structure and starting the body's natural healing process. Here are the steps involved in the mechanism of fractures:
Initial injury: A fracture starts with an injury that cracks or breaks a bone, which can also injure nearby blood vessels. This causes the area to bleed, forming a hematoma (blood clot) that serves as a temporary scaffold for healing.
Inflammatory stage: Inflammation starts in the first few days after injury. Immune cells arrive at the fracture site to clean up dead bones and other debris. As the hematoma is resolved, it can cause swelling, pain, and redness. Some of the bones near the break dissolve slightly, making the fracture line visible on X-rays.
Reparative Stage: In the next few weeks (2-6 weeks), new blood vessels grow into the hematoma, making a soft cartilage callus across the break. This turns into a stronger woven bone callus that fills the gap. To protect this delicate new tissue, it is important to keep it immobilized (like a cast).
Remodelling Stage: Over months to years, the big callus turns into strong, normal bone that resembles the original structure. Extra bones are removed, and the area becomes stronger from daily use and stress.

Fracture Symptoms
Recognizing the early bone fracture symptoms, such as pain, bruising, and limited movement, can help prevent complications. The following are the signs and symptoms of a fracture:
Rib fracture symptoms
- Severe chest pain
- Pleuritic pain (pain on deep breathing)
- Tenderness over the affected area
- Swelling or bruising(contusion)
- Difficulty in breathing
- Crepitus (crackling sensation)
- Coughing pain
Fractured ankle symptoms
- Inability to bear weight, visible deformity
- Limited movement
- Localized swelling, discoloration/tenderness
Fractured finger symptoms
- Finger deformity, numbness
- Difficulty moving, stiffness/redness/warmth
- Localized pain, swelling/bruising/tenderness
Hip fracture symptoms
- Inability to bear weight or stand
- The leg appears shortened/externally rotated
- Groin pain radiating to the thigh, bruising
Stress fracture symptoms
- Pain worsening with activity
- Point tenderness on weight-bearing
- Localized aching/swelling
Fractured knee symptoms
- Inability to straighten/extend leg
- Deformed kneecap appearance
- Pain on knee movement, swelling
Fractured wrist symptoms
- Bent wrist deformity
- Finger numbness/tingling
- Stiffness, tenderness/bruising
Skull fracture symptoms
- Clear fluid leak
- Battle's sign (indicates basilar fracture)
- Headache, nausea, confusion
Spinal fracture symptoms
- Sudden back pain with nerve symptoms
- Bowel/bladder dysfunction
- Weakness/tingling sensation in limbs
Clavicle fracture symptoms
- Shoulder drooping/grinding sensation
- Arm movement difficulty
- Visible bump at the collarbone
Compression fracture symptoms
- Sudden onset of back pain
- Height loss/kyphosis
- Abdominal discomfort
Femoral neck fracture symptoms
- Inability to stand (shortened leg)
- Groin/thigh pain on rotation
- External rotation deformity
Pelvic fracture symptoms
- Severe pain
- Immobility
- Bruising and swelling
- Numbness or tingling
- Signs of internal injury
Tibia fracture symptoms
- Severe pain and tenderness
- Swelling and bruising
- Inability to bear weight
- Deformity
- Limited knee motion
- Skin breakdown
- Numbness or tingling
Rib fracture symptoms
Severe chest pain: Pain is sharp and worsens with breathing, coughing, or movement. It is usually only in the area where the rib broke.
Pleuritic pain (pain on deep breathing): Taking a deep breath makes the pain worse because it moves the ribs. This could cause shallow breathing.
Tenderness over the affected area: Pain in the injured area is severe when the rib is touched or pressed, indicating that there is damage to the bone and the tissues around it.
Swelling or bruising (contusion): On the chest, swelling or discoloration of the soft tissues can be seen. It might occur due to damage to the underlying tissue and bleeding.
Difficulty in breathing: The patient may feel breathless because their chest can't expand fully due to pain. It can increase the risk of lung problems.
Crepitus (crackling sensation): During movement or touching it, individuals might hear or feel a grating sound. It looks like the ends of the bones are rubbing against each other. It is rare for simple fractures.
Coughing pain: Pain makes it hard to cough normally, resulting in mucus buildup in the lungs.
Fractured ankle symptoms
Inability to bear weight, visible deformity: Severe ankle fractures make it impossible to stand or walk because they hurt and make the ankle unstable. In some cases, the ankle may look misshapen if the bones are displaced.
Limited movement: Pain, swelling, and joint damage from the fracture make it hard to move the ankle.
Localized swelling, discoloration/ tenderness: Swelling and bruising occur when blood leaks under the skin, and tenderness happens when the area around the fracture becomes inflamed.
Fractured finger symptoms
Finger deformity, numbness: A broken finger might look bent or misshapen, and if the nerves are involved, it may feel numb or tingly.
Difficulty moving, stiffness/redness/warmth: Pain and swelling make it hard to move, and inflammation can make the area around the injured finger red and warm.
Localized pain, swelling/bruising/ tenderness: Pain is immediate and gets worse when touched or moved. Swelling and bruising are caused by bleeding and tissue damage.
Hip fracture symptoms
Inability to bear weight or stand: People who have hip fractures often can't stand or walk because of the pain and instability of their bones.
The leg appears shortened/externally rotated: The injured leg may look shorter and turned outward because the muscle is pulling on the broken bone.
Groin pain radiating to the thigh, bruising: Pain usually starts in the groin or hip and can move to the thigh. Bruising can occur due to internal bleeding.
Stress fracture symptoms
Pain worsens with activity: The pain from a stress fracture usually starts mild and gets worse when individuals do things that put stress on the bone. Pain may also occur at rest or during everyday activities as the injury worsens.
Point tenderness on weight-bearing: When touched or pressed, patients often feel a sharp pain in a specific area of the bone. This pain worsens during strenuous physical activities, such as walking or running.
Localized aching/swelling: stress fracture causes dull, aching pain in the affected area. This pain may get worse over time. There is often swelling around the painful area, especially after activity.
Fractured knee symptoms
Inability to straighten/extend leg: If the kneecap (patella) or the muscles and tendons around it are injured, it can be hard to extend the leg fully. This makes it hard or painful to straighten the knee.
Deformed kneecap appearance: A broken bone may cause the patella to move out of place, making the knee look unusual or uneven. Severe fractures can cause a visible gap or misalignment.
Pain on knee movement, swelling: When a bone breaks, it triggers inflammation that worsens pain during movement and leads to significant swelling around the joint. After an injury, fluid often builds up.
Fractured wrist symptoms
Bent wrist deformity: A broken wrist, especially a distal radius fracture, can make the wrist look bent or displaced (the classic "dinner fork" deformity). This means that the bones are misplaced.
Finger numbness/tingling: If bones move or swell, they can press on nearby nerves, causing the fingers to feel numb, tingly, or less sensitive.
Stiffness, tenderness/bruising: Soft-tissue damage around the fracture causes stiffness, pain, and bruising from blood pooling beneath the skin, resulting in restricted movement.
Skull fracture symptoms
Clear fluid leak: If clear fluid leaks from the nose or ears, it may indicate cerebrospinal fluid (CSF) leakage, which can signal a serious basilar skull fracture.
Battle's sign (indicates basilar fracture): Battle's sign, which is bruising behind the ears, is a sign of internal bleeding and is a key sign of a basilar skull fracture.
Headache, nausea, confusion: These signs happen because of brain damage or involvement, and they could mean a concussion or a more serious traumatic brain injury.
Spinal fracture symptoms
Sudden back pain with nerve symptoms: It is the most common sign of a vertebral fracture. It usually occurs in one area and worsens during movement or standing. If the spinal cord or nerves are compressed, neurological symptoms such as weakness or radicular pain can occur.
Bowel/bladder dysfunction: Loss of control over bowel or bladder function indicates potential spinal cord involvement and severe neurological injury. This occurs when the nerve pathways that control the pelvic organs are damaged or compressed.
Weakness/tingling sensation in limbs: Fractures of the spine can put pressure on nerves, leading to weakness, numbness, or even paralysis of limbs. The level and severity of spinal cord involvement determine neurological deficits.
Clavicle fracture symptoms
Shoulder drooping/grinding sensation: The shoulder droops because the clavicle is no longer supporting it, leading to pain and structural damage. When bones move, they may make a grinding (crepitus) sound.
Arm movement difficulty: Moving the arm makes the pain worse because the clavicle prevents the shoulder from moving too much. Patients frequently refrain from utilizing the affected arm due to pain and restricted mobility.
Visible bump at the collarbone: A displaced fracture can make the clavicle look bent or bumpy. This occurs because the bone moves and the area around the fracture swells.
Compression fracture symptoms
Sudden onset of back pain: Compression fractures often cause sudden back pain, even if there hasn't been any major trauma (especially in people with osteoporosis). Pain is localized and intensifies with standing or ambulation, worsening on standing and improving on lying down.
Height loss/kyphosis: Repeated vertebral collapse results in height loss and kyphosis, or forward spinal curvature. This deformity is caused by weakened vertebral bodies being pushed together.
Abdominal discomfort: Spinal deformity can compress the abdominal contents, leading to pain or early satiety. Pain that makes it hard to move around can also cause constipation and stomach problems.
Femoral neck fracture symptoms
Inability to stand (shortened leg): Patients frequently cannot bear weight due to intense hip pain and instability. Displaced fractures often cause the limb to shorten due to muscle pull.
Groin/thigh pain on rotation: The pain is in the groin or thigh and gets worse when you move your hip, especially when you turn it. This is because the hip joint and its surrounding structures are involved.
External rotation deformity: Muscle forces acting on the broken femur often cause the affected leg to lie externally rotated. This deformity is a typical clinical indication of displaced femoral neck fractures.
Pelvic fracture symptoms
Severe pain: When a bone is broken, such as with a pelvic fracture, there is usually severe pain at the point of injury. This is a common sign of a bone fracture.
Immobility: Difficulty moving or bearing weight on a bone fracture is common, and with a pelvic fracture, it may be very difficult or impossible to stand or walk.
Bruising and swelling: Broken bones often result in bruising, swelling, or tenderness at the injury site as blood and fluids accumulate.
Numbness or tingling: Pelvic fractures often cause nerve problems in this region, leading to changes in sensation, such as numbness or tingling.
Signs of internal injury: Although not specific, a severe pelvic fracture often results in internal bleeding or other internal injuries, and this is a sign of internal injury, which is a criterion for urgent medical treatment due to life-threatening complications.
Tibia fracture symptoms
Severe pain and tenderness: A fractured tibia causes pain, swelling, and tenderness around the injury site, and it can worsen with movement, indicating damage to the bone and surrounding soft tissues.
Swelling and bruising: The lower leg often swells and bruises due to bleeding under the skin from the fracture, making the shin appear larger and discolored.
Inability to bear weight: Individuals may find it very painful or impossible to put weight on the leg or walk normally after a tibia break.
Deformity: A broken tibia can make the leg look twisted, bent, shortened or abnormal, and in severe cases, a bone fragment may even stick out.
Limited knee motion: The injury can make it difficult to move leg or bend knee properly, reflecting pain and disruption of normal joint motion.
Skin breakdown: If the fracture is severe, a bone may protrude through the skin, or there may be a significant wound where the bone is visible.
Numbness or tingling: Although less common, a fracture may injure nearby nerves such that the leg, foot or toes feel numb, tingling, or burning in the affected limb.

Causes of Fracture
To keep bones strong and healthy and prevent injuries, it is essential to understand the causes of bone fractures, which may occur from sudden trauma to underlying health conditions that can vary widely and impact people of all ages. The following are the causes of bone fractures:
Pathological fracture causes/compression fracture causes
- Bone diseases
- Bone tumors
- Infections or metabolic disorders
Causes of femur fracture/hip fracture
- Low bone density
- High-energy trauma
Stress fracture causes/femoral neck fracture causes
- Repetitive mechanical stress (overuse)
- Imbalance in bone remodelling
- Normal stress on weakened bones
Causes of Clavicle fracture
- Fall onto the lateral shoulder
- Direct trauma to the clavicle
- Fall on outstretched hand
Causes of tibia fracture
- Low-energy torsional forces
- Indirect trauma
- High-energy direct trauma
Causes of pelvic fracture
- Falls from height
- Lateral compression injury
Oblique fracture cause
- Angled force on bone
A transverse fracture causes
- Direct perpendicular trauma
- Bending forces
An avulsion fracture causes
- Sudden muscle contraction
- Sports injuries/rapid acceleration
Basilar skull fracture causes
- High-velocity blunt trauma
- Penetrating trauma
Bimalleolar fracture causes
- Twisting injury of the ankle
- Eversion/external rotation trauma
- A fall or misstep causing sudden ankle stress
Pathological Fracture Causes/compression fracture causes
Pathological fractures occur when a disease weakens the normal structure of bones, making them prone to fracture even with minimal stress. These fractures are not the result of trauma but rather of preexisting bone pathology, which includes:
Bone diseases: Osteoporosis and metabolic disorders make bones weaker and less dense, which makes them more likely to break under low stress.
Bone tumors: Both primary bone tumours and metastatic cancer deposits make unusual lesions in bone that make it weaker, which can cause fractures with little or no trauma.
Infections or metabolic disorders: Chronic bone infections (osteomyelitis) or metabolic disorders (e.g., hyperparathyroidism) disrupt normal bone remodelling and compromise bone tissue, increasing the risk of abnormal fractures.
Causes of femur Fracture/hip Fracture
Femur fractures, particularly in older people, typically result from a combination of bone fragility and mechanical force, whereas in younger individuals, severe trauma is more common. The following are the causes of femur and hip fractures:
Low bone density: Osteoporosis and other conditions make it harder for the femur to absorb force, so a fall from standing height can break the hip.
High-energy trauma: In younger people or in situations with a lot of force (such as car accidents or falls from a height), the femur or hip region can break because the external forces are too strong for the bones to withstand.
Stress fracture causes / Femoral Neck Fracture
Stress and femoral neck fractures occur when bones get microdamage faster than they can heal. The following are the causes of stress and femoral neck fracture:
Repetitive mechanical stress (overuse): Long-distance running and other activities put stress on the femoral neck repeatedly, which causes microfractures that eventually turn into a stress fracture.
Imbalance in bone remodeling: If bone resorption occurs faster than formation (due to training load, hormonal imbalance, or nutrition), existing microdamage can't be repaired effectively, which can lead to stress fractures.
Normal stress on weakened bones: If osteoporosis or another disease weakens the bone, even normal daily activities can cause a fracture because the bone can't handle normal mechanical loads.
Causes of clavicle Fracture
Most of the time, a collarbone fracture occurs because of direct mechanical trauma to the shoulder area. The following are the causes of clavicle (collarbone) fractures:
Fall onto the lateral shoulder: The most common way this occurs is during a fall onto the outer shoulder, which transmits force directly to the clavicle, resulting in a clavicle (collarbone) fracture.
Direct trauma to the clavicle: A strong hit or blow to the collarbone (like in a sports collision or contact injury) can break the bone.
Fall on outstretched hand: When an individual falls, the force that travels up the arm can push the shoulder upward, potentially breaking the clavicle.
Causes of tibia fracture
Low- and high-energy trauma can cause tibia shaft fractures. Some of the most common causes of tibia fractures are:
Low-energy torsional forces: A twisting or rotational force on the lower leg can break bones, especially when someone falls or twists their leg, which can cause fractures along the tibial shaft.
Indirect trauma: Indirect force (such as twisting while the foot is planted) can cause spiral fracture patterns with little external force.
High-energy direct trauma: High-impact events, such as car crashes or falls from a height, can put significant stress on the shin, leading to comminuted or wedge fractures of the tibia and damage to the surrounding soft tissues.
Causes of pelvic fracture
The pelvis is shaped like a strong ring; it usually takes a lot of force to break it, including the following causes:
Falls from height: When someone falls from a height and lands on their feet, buttocks, or side, the force travels up their legs and into the pelvic ring, resulting in a pelvic bone fracture.
Lateral compression injury: When some unusual activity hits the side of the pelvis, like in a car accident, it pushes the pelvis inward, breaking and compressing the pelvic bones. These patterns are most common in high-energy trauma, but they can also occur in older people with weak bones, even when they fall from lower heights.
Oblique fracture cause
When a force is applied at an angle to the long axis of a bone, it breaks obliquely, which includes the following causes of oblique fracture:
Angled force on bone: This angled force creates a slanted fracture line (>30° relative to the bone's long axis) because shear stress makes the bone bend and breaks diagonally. They usually occur when bending and axial loads act together, not from straight impacts.
A transverse fracture causes
Transverse fractures are breaks that go straight across the bone's long axis and include the following causes:
Direct perpendicular trauma: It refers to a force striking a bone at a precise 90-degree angle to its longitudinal axis, often producing a clean transverse fracture across the bone shaft.
Bending forces: When a bone is bent sharply (like against a hard surface), the tension on one side and the compression on the other cause it to break straight across.
An avulsion fracture causes
When a tendon or ligament pulls on a piece of bone, it can break off, which is known as an avulsion fracture, including the following causes:
Sudden muscle contraction: Sudden, strong muscle contractions can generate enough tensile force to pull a piece of bone from its attachment site, a condition called an avulsion fracture. Muscles pull on bony insertions through tendons. In some cases, the bone-tendon interface fails before the tendon does.
Sports injuries/rapid acceleration: In sports, quick starts, stops, or changes in direction can put a lot of stress on tendons all at once. If the attachment site is weaker than the pulling muscle, an avulsion fracture can occur.
Basilar skull fracture causes
High-speed blunt trauma, like car crashes, motorcycle crashes, or pedestrian impacts, is the most common cause of basilar skull fractures. This is because a lot of force passes through the skull base, which includes the following causes:
High-velocity blunt trauma: High-velocity blunt trauma occurs when a strong impact doesn't break through the skin (like in a high-speed car crash or a heavy object hitting you) and sends a lot of kinetic energy to the body. Even though the skin remains intact, this violent impact can break bones, injure internal organs, and damage soft tissues.
Penetrating trauma: Assault-related penetrating trauma occurs when any object penetrates through the skin and into the body's tissues, such as gunshot or stab wounds, and it accounts for under 10% of cases. This usually occurs with a weapon that moves quickly, like bullets.
Bimalleolar fracture causes
A bimalleolar fracture is a type of ankle fracture that happens when both the lateral and medial malleoli break. This usually occurs when a weight-bearing ankle joint is hit hard.
Twisting injury of the ankle: A common cause of bimalleolar fractures is when the foot is suddenly twisted or turned while it is planted, which puts stress on both the lateral and medial malleoli (bony prominences on either side of the ankle).
Eversion/external rotation trauma: When the ankle is forced to turn or rotate outward (eversion), the ligaments and bones fail under stress and break. This often leads to both malleoli breaking, according to clinical classification systems.
A fall or misstep causing sudden ankle stress: If individuals trip, slip, or fall, the ankle joint can quickly be subjected to twisting or bending forces, which can fracture the bones on both sides of the ankle.

Risk Factors for Fractures
Conditions or factors that weaken bones or increase the likelihood of injury are risk factors for fractures. These may be linked to age, lifestyle, underlying illnesses, or environmental factors that weaken or damage bones. The following are the risk factors for fractures:
- Increasing age
- Previous history of fracture
- Smoking
- Excess alcohol consumption
- Physical inactivity
- Poor nutrition
- Use of steroids or certain medications
- Chronic diseases
Increasing age: Increased age results in bones naturally losing density and strength, making them more fragile and likely to break from low-energy events such as simple falls. Older individuals are more prone to falls and have worse body balance, increasing their risk of fractures. Age is a significant factor in fragility fractures worldwide.
Previous history of fracture: A previous fracture, particularly from minimal trauma, substantially elevates the likelihood of subsequent fractures. This indicates inherent bone fragility and compromised bone healing ability. A prior fracture is a significant indicator of future fracture risk in clinical settings.
Smoking: Tobacco smoke contains chemicals that are harmful to bones, making them less dense. Major health organizations say that smoking is a risk factor that can be changed and raises the risk of fractures. It also affects balance and muscle strength, increasing the risk of falling.
Excess alcohol consumption: Long-term heavy drinking disrupts bone remodelling and reduces bone mineral density. It also makes coordination and balance harder, increasing the likelihood of falls that result in fractures. It also says that drinking alcohol is a lifestyle risk factor for fragile fractures.
Physical inactivity: Lack of physical activities that put stress on bones causes them to lose strength, as stress makes bones grow. Being inactive also weakens muscles and balance, increasing the risk of falling. It includes sedentary behaviour as a major risk factor for fractures that can be changed.
Poor nutrition: A diet that doesn't have enough nutrients, especially calcium and vitamin D, can lead to less bone mass and a higher risk of breaking bones. Not getting enough protein can result in bone and muscle injuries. It includes a diet low in nutrients as a risk factor for fractures that can be changed.
Use of steroids or certain medications: Long-term use of glucocorticoids and some other drugs, like anticonvulsants and some cancer treatments, speeds up bone loss. These drugs mess with the bones' functioning and make them less strong. It shows that these kinds of drugs raise the risk of osteoporosis and bone fractures.
Chronic diseases: Some long-term illnesses, such as rheumatoid arthritis (it is a long-term disease when the body's immune system (which normally fights infections) mistakenly attacks its own joints), endocrine disorders, and gastrointestinal diseases, disrupt the normal processes of bone metabolism and nutrient absorption. These conditions make bones thinner and cause inflammation throughout the body, which raises the risk of fractures.
Risk Factor of Femur Fractures
High-impact trauma or weak bones are the most common causes of femur fractures. The risk of bone fracture increases with age, osteoporosis, and accidents. The following are the femur fracture risk factors:
- Female gender
- Previous falls or gait abnormalities
- Neurological or cognitive disorders
- Psychoactive/antiepileptic drugs
- Muscle weakness and poor balance
- Low body mass index (BMI)
Female gender: Women, especially older women, are much more likely than men to break their hips (proximal femur). This is because bone loss after menopause (linked to a drop in hormone) makes bones weaker. About 70% of these fractures that are treated in hospitals occur in women. The risk increases with increased age and the development of osteoporosis.
Previous falls or gait abnormalities: If individuals have a preexisting fall history, they are much more likely to fall again and break their femur. If they have trouble walking or balancing, they are more likely to fall. These mobility problems are strong indicators that older people are at risk of hip fractures. Most hip fractures in older people are caused by falls.
Neurological or cognitive disorders: Some of the neurological disorders, such as dementia (loss of memory), cognitive impairment, and neurological disorders (such as Parkinson's), can affect balance, coordination, and judgment, which makes falls more likely and more dangerous. This higher risk of falling directly raises the risk of fractures in the femur region.
Psychoactive/antiepileptic drugs: Some medicines, like tranquilizers, sedatives, antidepressants, and antiepileptic drugs, can make individuals dizzy, sleepy, or slow down their reflexes, which can make them less stable. These side effects make older people more likely to fall, increasing their risk of fractures.
Muscle weakness and poor balance: In individuals with weak lower-body strength and poor balance, it's harder to recover from slips or trips. This makes falls resulting in femur fractures much more likely. Maintaining muscle strength and balance is an important goal for older people to help prevent complications from fractures.
Low body mass index (BMI): A low BMI often indicates lower muscle and bone mass, making bones weaker and less stable. People with a lower BMI are more likely to break bones because their bones are less dense and they are more likely to fall.
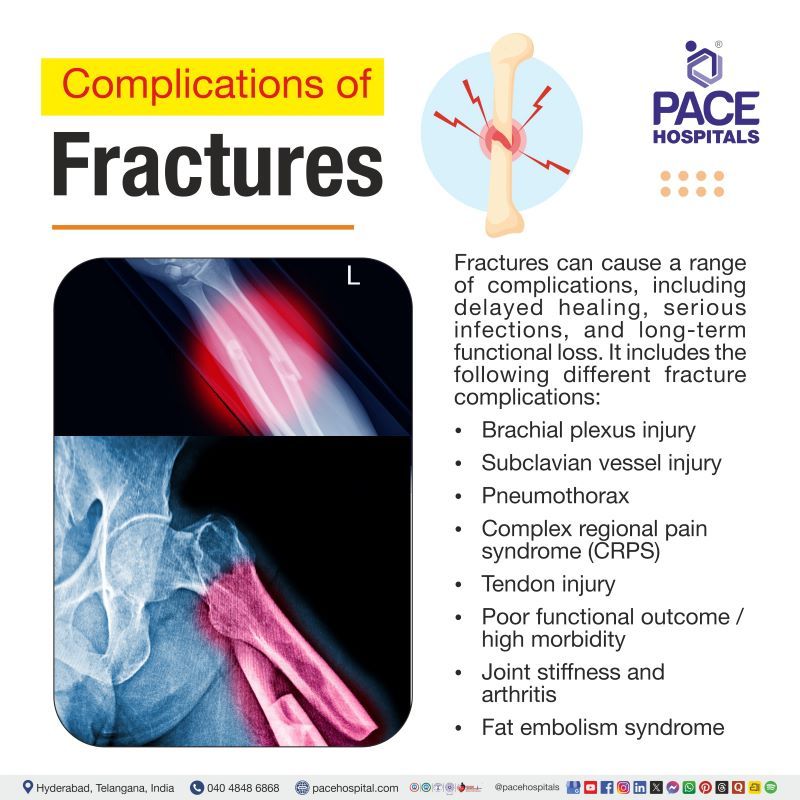
Complications of Fracture
Fractures can cause a range of complications, including delayed healing, serious infections, and long-term functional loss. It includes the following different fracture complications:
Clavicle/collarbone fracture complications
- Brachial plexus injury
- Subclavian vessel injury
- Pneumothorax
- Malunion
- Nonunion
- Post-traumatic arthritis
Distal radius/Colles fracture complications
- Complex regional pain syndrome (CRPS)
- Tendon injury
- Infection
Distal femur complications
- Poor functional outcome/high morbidity
- Joint stiffness and arthritis
General long bone fracture complications (applies to femur and tibia fracture complications)
- Fat embolism syndrome
- Compartment syndrome
- Deep vein thrombosis (DVT)
Rib fracture complications
- Pulmonary contusion
- Respiratory failure/pneumonia
Open fracture complications
Hip fracture complications
- Avascular necrosis (AVN)
- Pressure sores
Pelvic fracture complications
- Severe hemorrhage
- Bladder/urethral injury
- Nerve injury
Ankle and bimalleolar fracture complications
- Joint instability
Basilar skull fracture complications
- CSF leak
- Meningitis
- Cranial nerve injury
Compression fracture (spine)
- Chronic pain
- Kyphosis (spinal deformity)
- Reduced lung capacity
Closed fracture complications
- Neurovascular injury
Complications of avulsion fracture
- Loss of function due to tendon imbalance
Femur fracture (shaft) complications
- Hemorrhagic shock
Clavicle/collarbone fracture complications
If not properly treated, clavicle fractures and their complications can have a greater impact on shoulder function, mobility, and overall quality of life. Some of the following complications are mentioned below:
Brachial plexus injury: It occurs when the network of nerves that control movement and sensation in the shoulder, arm, and hand is injured or compressed, either when the bone breaks or during healing. This can make the affected limb feel numb or weak, or affect mobility. It is rare but clinically significant to detect early.
Subclavian vessel injury: Sharp bone pieces can damage the subclavian artery or vein in high-energy or severely displaced clavicle fractures. This injury to the blood vessels could cause excessive bleeding, hematoma (bruise), or blood flow problems in the arm. Even though it doesn't occur very often, it can be life-threatening and needs to be evaluated and treated promptly.
Pneumothorax: When air builds up in space around the lung, it can partially or completely collapse the lung. This can occur when a broken clavicle or adjacent rib fragment injures the lung apex or pleura, allowing air into the pleural space. This is a rare but serious problem that needs chest imaging and often an urgent chest drain.
Malunion: It occurs when a broken clavicle heals in the wrong position, resulting in bending, shortening, or a misshapen appearance. Even though the bone does heal, this can cause shoulder problems, changes in shoulder function, pain, and changes in appearance. If the outcome results in serious symptoms, corrective surgery may be needed.
Nonunion: It occurs when the broken ends of the clavicle don't heal together within the expected time frame (usually 4–6 months). It can cause long-term pain, weakness, and strange shoulder movement, which may require surgery by an orthopaedic surgeon. Risk factors include major fracture displacement and poor immobilization.
Post-traumatic arthritis: It can arise in the joints adjacent to a clavicle fracture, especially when the injury affects or modifies the joint surfaces, resulting in persistent pain and rigidity. The acromioclavicular (AC) or sternoclavicular joint gets worse over time, which limits its function. It's a late, rare complication of clavicle injuries.
Distal radius/Colles fracture complications
Colles fractures of the distal radius can cause several complications that make it harder for nerves, soft tissue, and the whole body to heal. Some common complications of Colles ' fractures are:
Complex regional pain syndrome (CRPS): CRPS is a long-term pain condition that occurs after a fracture or surgery. It is characterized by pain, swelling, and autonomic nervous system changes that are disproportionate to the injury. It can occur after both surgical and non-surgical treatment of distal radius fractures.
Tendon injury: Sharp bone fragments and hardware used to fix a fracture can both irritate or tear tendons, especially the extensor pollicis longus (long muscle in the forearm) and other wrist tendons. These tendon issues can occur weeks or months after the fracture, and if they cause significant problems, surgery is usually needed to fix them.
Infection: Infection is an uncommon but significant complication, especially following surgical fixation, and may affect pin sites, surgical wounds, or deeper bone infections.
Distal femur complications
Fractures of the distal femur are serious injuries that occur near the knee joint at the lower end of the thighbone. They are often very complicated and involve the joint surface, so even after treatment, they can cause serious long-term problems.
Poor functional outcome/high morbidity: Modern surgical techniques help the body heal better, but distal femoral fractures can make it hard for the knee to work properly, especially in older people or when there is a lot of comminution or involvement of the joint. Functional impairment may endure due to difficulties in reinstating complete joint mechanics, resulting in reduced mobility and strength despite fixation.
Joint stiffness and arthritis: Knee stiffness after an injury or surgery is common because of prolonged immobilization, scar tissue formation, and damage to the cartilage around the fracture site. Intra-articular damage also makes people more likely to get early post-traumatic
osteoarthritis, which causes pain, limited movement, and a decline in function over time.
General long bone fracture complications (applies to femur and tibia fracture complications)
Long bone fractures, including those of the femur and tibia, can result in significant systemic and localized complications during the initial post-injury phase, potentially endangering life or limb if not promptly identified or addressed.
Fat embolism syndrome: It is a rare but serious complication that happens when fat droplets from bone marrow get into the bloodstream after a long-bone fracture. This can cause small blood vessels to become blocked, leading to respiratory distress, neurological symptoms, and skin changes within 24 to 72 hours of the injury.
Compartment syndrome: It is a medical emergency that happens after a long bone fracture. It occurs when the pressure in a muscle compartment rises, preventing blood and oxygen from reaching tissues. If left untreated, it can cause permanent nerve and muscle damage.
Deep vein thrombosis (DVT): Deep vein thrombosis occurs when a blood clot forms in the deep veins of the leg after a fracture and immobilization. This can occur often after lower extremity fractures and can cause pulmonary embolism if the clot breaks loose.
Rib fracture complications
Rib fracture complications arise due to impaired chest wall movement and associated lung injury following trauma.
Pulmonary contusion: A pulmonary contusion is a traumatic injury to the lung parenchyma caused by blunt chest trauma. It makes it harder for the lungs to exchange gases and can lead to respiratory failure.
Respiratory failure/pneumonia: Pulmonary contusions resulting from rib fractures can impair normal lung function and potentially result in severe complications, including pneumonia and respiratory failure.
Open fracture complications
Open fracture complications happen when the broken bone is exposed to the external environment, which raises the risk of serious infection and delayed healing.
Sepsis: In open fractures, the wound exposes bone and soft tissues to outside germs, greatly increasing the risk of bacterial infection that can spread beyond the injury site. If bacteria get into the blood and overwhelm the body's defences, this can lead to sepsis, which needs immediate medical attention to stop organ failure and death.
Hip fracture complications
Hip fractures can cause serious complications like immobility, infection, and increased mortality, especially in older people.
Avascular necrosis (AVN): It occurs when blood flow to bone tissue stops, which can happen after a hip fracture when blood flow to the femoral head is impaired.
Pressure sores: Pressure sores (pressure ulcers) are localized injuries to the skin and underlying tissues over bony areas that occur when someone is under prolonged pressure and can't move. They are a common problem for older adults who have broken their hips while in the hospital.
Pelvic fracture complications
Pelvic fractures can cause serious complications, such as internal bleeding, damage to organs, infection, and long-term problems with movement.
Severe hemorrhage: Pelvic fractures can cause excessive bleeding because they damage pelvic blood vessels and the venous plexus. This often leads to the formation of hematomas and hemorrhagic shock, which indicates that bleeding is a major cause of illness and death.
Bladder/urethral injury: Pelvic fractures can be linked to trauma to the bladder or urethra, and bone fragments or strong impacts can cause physical injury in a significant number of cases.
Nerve injury: The lumbosacral plexus is the most common nerve injury that happens after a pelvic fracture. This is because it is close to the fractured sites and is caused by traction or compression from bleeding or a displaced bone.
Ankle and bimalleolar fracture complications
Ankle and bimalleolar fractures can lead to complications both early on (like swelling, infection, and nerve and blood vessel damage) and later on (like malunion, joint stiffness, and post-traumatic osteoarthritis).
Joint instability: A normal ankle joint is stable when it can move within its normal range of motion. This is because of the way the bones are shaped, the ligaments, and the muscles that surround them. In an unstable injury (such as a bimalleolar fracture), these stabilizing structures are damaged, exceeding the joint's normal limits and making it unstable.
Basilar skull fracture complications
Basilar skull fractures can be difficult to spot, but if they aren't evaluated and treated promptly, they can cause serious and possibly life-threatening complications.
CSF leak: A tear in the dura mater at the base of the skull can let cerebrospinal fluid leak out of the body. This creates a direct link between the central nervous system and the external environment, which raises the risk of infection.
Meningitis: A CSF leak from a basilar skull fracture can allow germs into the subarachnoid space, leading to meningeal inflammation, which is often mistaken for bacterial meningitis.
Cranial nerve injury: Basilar skull fractures can damage or compress cranial nerves as they leave the base of the skull, which can cause nerve palsies or problems with movement or sensation.
Compression fracture (spine)
A spinal compression fracture is a painful condition that occurs when a vertebra collapses. This can occur due to osteoporosis, an injury, or trauma.
Chronic pain: Compression fractures in the spine can cause long-term back pain that lasts long after the injury. This can make it difficult for people to perform everyday activities, affecting their quality of life.
Kyphosis (spinal deformity): When individuals have multiple spinal compression fractures, their spine may curve too far forward (kyphosis), which can make their posture rounded or hunched.
Reduced lung capacity: Compression fractures can cause severe kyphosis, which can make it harder for the lungs to expand because it limits the space available.
Closed fracture complications
A closed fracture may appear less serious externally, but if not treated properly, it can still cause serious complications like swelling, internal bleeding, nerve damage, or delayed healing.
Neurovascular injury: If a closed fracture isn't evaluated and treated immediately, it can damage nearby arteries and nerves, leading to impaired blood flow and sensory and motor function below the injury.
Complications of avulsion fracture
It can include chronic pain, joint instability, delayed healing, nonunion of the bone fragment, and reduced range of motion if left untreated.
Loss of function due to tendon imbalance: An avulsion fracture occurs when a tendon tears off a piece of bone. This can change the muscle–tendon unit's normal pull, weakening the joint or reducing its range of motion.
Femur fracture (shaft) complications
A femoral shaft fracture can cause serious complications, so it's important to obtain a prompt diagnosis, provide the right treatment, and monitor the patient to ensure they recover fully.
Hemorrhagic shock: A fracture of the femoral shaft can lead to significant blood loss, worsening circulation and hemorrhagic shock.
Fracture Diagnosis
It is very important to diagnose fractures early and appropriately to avoid complications and achieve optimal healing. A comprehensive clinical assessment, supported by suitable imaging modalities, facilitates accurate diagnosis and efficient treatment of bone injuries.
The following are the steps commonly included in the fracture diagnostic evaluation:
- Medical history and evaluation
- Physical examination
- Imaging studies (radiography)
- Bone x-ray
- Comparison views
- Advanced imaging (if necessary)
- Computed Tomography (CT scan)
- Magnetic Resonance Imaging (MRI)
- Bone scan
Ankle fracture diagnosis
A break in one or more of the bones that make up the ankle joint is called an ankle fracture. It usually occurs when someone falls, twists, or sustains an injury.
The following are the steps commonly included in the diagnosis of an ankle fracture:
- Medical history
- Physical examination
- Ottawa Ankle Rules
- Imaging Tests (Radiology)
- X-ray
- Stress test/stress X-ray
- CT scan
- MRI
- Neurovascular assessment
Clavicle fracture diagnosis
A broken clavicle is a common orthopaedic injury that is usually diagnosed on physical examination and confirmed with imaging tests such as X-rays.
The following are the steps commonly included in the diagnosis of a clavicle fracture:
- Medical history
- Physical examination
- Imaging studies
- X-rays
- CT scan
- Classification (identifying the location)
Diagnosis of femur fracture
To prevent complications and ensure the best recovery, it is important to evaluate a femur fracture early and appropriately.
The following are the steps commonly included in the femur fracture diagnosis:
- Medical history
- Physical examination
- Imaging studies (diagnostic tests)
- X-ray
- Adjacent joint imaging
- CT scan
- CT angiography
- MRI
- Classification and diagnosis confirmation
- Location
- Pattern
- Alignment
- Common associated injuries to rule out
- Ipsilateral femoral neck fracture
- Pelvic fractures
- Knee ligamentous injuries
Fracture Treatment
Effective management of fracture treatment is essential for facilitating adequate healing and preventing long-term complications. Patients can have much better recovery outcomes if they understand the steps involved in treating a fracture.
The following are the steps involved in the medical management of fractures:
- Immediate first aid management of fracture/stabilization
- Reduction (realigning the bone)
- Closed reduction
- Open reduction
- Immobilization (holding the bone)
- Casts and splints
- Traction
- External fixation
- Rehabilitation
Rib fracture treatment
Rib fractures can be very painful and uncomfortable, and they need to be taken care of to heal. Timely and appropriate rib fracture management is very important for full recovery and to prevent complications.
The following are the steps involved in rib fracture management:
- Pain management (analgesia)
- Respiratory care
- Supportive care and activity management
- Physiotherapy
- Surgical management of fracture (severe cases)
Clavicle fracture treatment
A clavicle fracture, also known as a collarbone fracture, is a common injury that can significantly impact mobility and daily activities. The severity of the fracture usually determines the treatment, which can range from conservative care to surgery for more complicated cases.
The following are the steps involved in clavicle fracture management:
- Sling or shoulder immobilizer
- Pain management and care
- Initial rehabilitation (0-3 weeks)
- Rehabilitation (3-6 weeks)
- Rehabilitation (6-12 weeks)
- Surgical intervention (when required)
Femoral neck fracture treatment
A femoral neck fracture is a serious injury that occurs frequently in older people. It usually occurs when they fall or are hit hard, and they need prompt medical attention.
The following are the steps involved in neck of femur fracture management:
- Initial assessment and stabilization
- Surgical management of fracture
- Open reduction internal fixation (ORIF)
- Partial hip replacement (hemiarthroplasty)
- Total hip replacement (arthroplasty)
- Postoperative management
- Rehabilitation (physical therapy)
- Early phase
- Progressive phase
- Long-term recovery
Colles fracture treatment
The goal of Colles' fracture treatment is to realign the bone, control pain, and speed up healing through a combination of immobilization, physical therapy, and, in some cases, surgery.
The following are the steps involved in Colles fracture management:
- Immediate assessment and diagnosis
- Closed reduction (non-surgical realignment)
- Immobilization (casting/splinting)
- Surgical intervention (ORIF- open reduction internal fixation)
- Follow-up care and X-rays
- Rehabilitation and physiotherapy
Stress fracture treatment
To heal stress fractures, effective treatment focuses on rest, proper nutrition, and targeted rehabilitation to prevent further injuries and restore mobility.
The following are the steps involved in stress fracture management:
- Rest and activity modification
- Immobilization and protective support
- Pain and inflammation control
- Physical therapy and rehabilitation
- Nutrition support
- Gradual return to activity
- Surgical management (rarely indicated)
Femur fracture treatment
Effective treatment for a femur fracture is essential to facilitate proper healing, prevent complications, and restore mobility.
The following are the steps involved in femur fracture management:
- Initial stabilization
- Surgical planning
- Anesthesia
- Reduction (realignment)
- Closed reduction
- Open reduction
- Fixation
- Intramedullary nailing
- ORIF (open reduction internal fixation)
- Dynamic hip screw
- Wound closure
- Postoperative care and rehabilitation
- Pain management
- Early motion
- Weight-bearing
Pelvic fracture treatment
To avoid complications and speed up recovery, effective treatment for pelvic fractures is very important. It should focus on stabilizing the fracture, managing pain, and rehabilitation.
The following are the steps involved in pelvic fracture management:
- Emergency stabilization (immediate care)
- Assessment and diagnostic imaging
- Non-surgical management (conservative care)
- Bed rest
- Pain management
- Mobilization
- Assistive devices
- Surgical management of pelvic fracture (operative care)
- External fixation
- Internal fixation (ORIF)
- Angiographic embolization
- Skeletal traction
- Rehabilitation and recovery
Tibia fracture treatment
To ensure that a tibia fracture heals properly, restores mobility, and doesn't cause long-term complications, it needs to be treated properly.
The following are the steps involved in tibia fracture management:
- Initial assessment and stabilization
- Closed reduction (nonsurgical)
- Surgical management
- Intramedullary nailing
- ORIF
- External fixation
- Rehabilitation and recovery
- Physical therapy
- Weight-bearing restrictions
Distal radius fracture treatment
Distal radius fractures, also known as wrist fractures, need to be treated promptly and properly to heal and fully restore hand and wrist function.
The following are the steps involved in distal radius fracture management:
- Initial immobilization (conservative/non-operative)
- Closed reduction
- Surgical treatment (operative-ORIF)
- External fixation
- Rehabilitation (physical therapy)
Fibula fracture treatment
Depending on the severity of the injury, the best treatment for a fibula fracture is usually a combination of rest, immobilization, and, in some cases, surgery.
The following are the steps involved in fibula fracture management:
- Initial diagnosis and management
- Immobilization
- Closed reduction
- ORIF
- Weight-bearing management
- Physical therapy and rehabilitation
- Follow-up care
Hip fracture treatment
To ensure hip fractures heal properly, patients need effective treatment that restores their mobility and improves their quality of life.
The following are the steps involved in hip fracture management:
- Preoperative optimization
- Surgical intervention
- Internal repair (osteosynthesis/fixation)
- Partial hip replacement (hemiarthroplasty)
- Total hip replacement (arthroplasty)
- Postoperative care
- Pain management
- Blood clot prevention
- Early mobilization
- Rehabilitation (physical therapy)
- Secondary prevention
Ankle fracture treatment
For an ankle fracture to heal properly, reduce pain, and restore mobility, it is important to get the appropriate treatment. This will allow individuals to get back on their feet quickly and safely.
The following are the steps involved in ankle fracture management:
- Initial assessment and stabilization
- Pain management and care
- Reduction (realigning bones)
- Closed reduction
- Open reduction internal fixation
- Immobilization
- Rehabilitation (rehab/physical therapy)
Patellar (Knee) fracture treatment
Proper treatment of knee fractures is important to ensure they heal properly, restore mobility, and avoid long-term problems.
The following are the steps involved in patellar fracture management:
- Initial assessment and immediate care
- Non-surgical treatment (stable fractures)
- Immobilization
- Weight-bearing restrictions
- Follow-up imaging
- Surgical treatment (displaced/complex fractures)
- ORIF
- Tension band wiring
- Fragment removal
- Partial/total patellectomy
- Rehabilitation and early recovery
- Early motion
- Physical therapy
- Gradual weight-bearing
- Long-term recovery
- Pain management
- Medication
- Icing
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support

Prevention of Fracture
Daily habits like eating a balanced diet, exercising regularly, and being aware greatly lower the risk of breaking a bone. Prioritizing bone health not only prevents injuries but also helps long-term mobility and independence.
The following are the fracture preventions, which include:
- Improve diet and nutrition
- Regular physical activity and exercise
- Prevention of falls
- Smoking cessation
- Limit alcohol consumption
- Vitamin D and calcium supplementation
- Early assessment and treatment of osteoporosis
- Health system-level coordination and policy integration
Improve diet and nutrition: A healthy, balanced diet that includes essential nutrients like calcium and vitamin D helps keep bones strong, reducing the risk of fractures.
Regular physical activity and exercise: Regularly performing weight-bearing and muscle-strengthening activities like walking or strength training makes bones denser, improves balance, and strengthens muscles, which lowers the risk of fractures.
Prevention of falls: Taking preventive measures such as home safety checks, balance exercises, and vision and medication reviews can all help lower the risk of falls, especially in older adults.
Smoking cessation: Quitting smoking is good for bones because smoking can lower bone mass and make it more likely to break bones over time.
Limit alcohol consumption: It is best to limit alcohol consumption because excessive drinking can make bones weaker and make individuals more likely to fall, which increases their chances of breaking a bone.
Vitamin D and calcium supplementation: It is advised to get enough vitamin D and calcium from food and supplements to help maintain bone density and lower the risk of fractures.
Early assessment and treatment of osteoporosis: Identifying people at high risk by assessing bone density and providing them with early support can help prevent fractures.
Health system-level coordination and policy integration: Public health strategies that include awareness of fracture risk, prevention programs, and policy support make it easier to implement large-scale fracture prevention.
Difference between Colles and Smith Fracture
Colles Fracture vs Smith Fracture
A Colles fracture occurs when the wrist bone breaks and moves up, usually because someone falls on an outstretched hand. A Smith fracture, on the other hand, is a break in the same bone that occurs when the wrist bends inward, usually because of a fall on a bent wrist. Below are the key differences between a Colles fracture and a Smith fracture:
| Characteristics | Colles fracture | Smith fracture |
|---|---|---|
| Displacement direction | Dorsal position (backward/posterior). | Volar position (forward /anterior). |
| Common cause | FOOSH: Fall on Outstretched Hand with Wrist in Extension. | Fall on a bent wrist (or hit the back of the hand directly). |
| Deformity name | “Dinner Fork’’ deformity. | “Garden spade’’ deformity. |
| Frequency | Most common. | Less common, approximately 5% of radial fractures. |
| Stability | Usually, it is more stable than a Smith fracture. | Often unstable and require careful management. |
Difference between Sprain and Fracture
Sprain vs Fracture
Both sprains and fractures damage the body, but in different ways. A sprain occurs when ligaments are stretched too far or torn, and a fracture occurs when a bone breaks or cracks.
Below are the key differences between a sprain and a fracture:
| Characteristics | Sprain | Fracture (broken bone) |
|---|---|---|
| Affected tissue | It mainly affects the ligaments (which connect bone to bone). | It affects bones (hard tissue) |
| Primary cause | Twisting or stretching a joint too far | Trauma that has a high impact, such as falls or direct blows (physical hits or strikes). |
| Pain type | Initially, pain was intense but may be partially manageable. | Pain is sharp, strong, and persistent (that lasts for a long time). |
| Pain location | Pain appears around the joints. | Pain appears directly over the bone. |
| Mobility | Can usually limp or walk, but movement is limited. | Often, there is an inability to move the limb or bear weight, or marked pain with minimal movement. |
| Deformity | No visible deformity. | Deformity or misalignment is seen potentially. |
| Sound | Possibly a popping sensation | Possibly snapping (sharp, quick noise) or grinding sound. |
| Healing time | It takes days to weeks for recovery. | Fracture recovery takes weeks to months. |
| Common treatment | R.I.C.E (rest, ice, compression and elevation). | Treatment includes immobilization (cast/splint) or surgery. |
Frequently Asked Questions (FAQs) on Fractures
What is a fracture?
A fracture is a break, crack, or tear in a bone or other hard material that is either complete or partial. It can happen because of too much stress, too much force, or medical conditions like osteoporosis. As a verb, it means to break or crack, and it is the same as a broken bone. There are many kinds of fractures, such as open, closed, displaced, and nondisplaced.
What are the different types of fractures?
Fractures are divided into types according to the pattern of the fracture, severity, and whether they pierce the skin. There are many types of bone fractures, ranging from minor stable fractures to severe shattering fractures. The main types are transverse (straight across), oblique (at an angle), spiral (twisted), greenstick (partial, common in children), comminuted (shattered), and open (piercing the skin). Standard classifications also include additional common types such as avulsion, compression, displaced/non-displaced, and stress fractures.
What is a hairline fracture?
A hairline fracture, also known as a stress fracture, is a small, thin crack or bruise in a bone. It usually occurs when the bone is used repetitively, due to excessive strain, or when the activity level suddenly increases. These painful injuries often occur in the lower leg and foot. They don't go all the way through the bone, but they need rest, immobilization, and proper medical care to prevent them from worsening.
Does a hairline fracture need a plaster cast?
Most of the time, hairline fractures don't require a full plaster cast, but they do need to be immobilized to heal properly. To prevent a crack from turning into a full break, treatment usually includes protective measures such as a removable brace, splint, or special walking boot, along with rest.
Why is a hip fracture so dangerous?
A hip fracture is dangerous because it can lead to a series of serious health problems. For example, elderly patients have a 20–30% chance of death within a year because of immobility-related issues, which can lead to pneumonia, blood clots, and infections. It makes people lose their independence suddenly and severely, and it often requires high-risk surgery.
How long does a fracture take to heal?
Adults usually take 6 to 12 weeks to heal a broken bone (fracture), but this can vary widely depending on the bone, its severity, the person's age, and overall health. It takes 3 to 6 weeks for the first repair (soft callus formation) to occur, but it can take months or even a year for the bone to remodel and regain its full strength.
Can fractures lead to permanent disability?
Yes, this is true since fractures can cause disabilities, especially if the fractures are severe, occur around the joints, or do not heal properly. Although most fractures heal without any complications, the problems that might occur, such as chronic pain and reduced mobility, might cause disabilities.
Can individuals walk on a fractured fibula?
People with a broken fibula usually can't walk on their own initially because they need to be immobilized and do not put any weight on it to heal properly. Under medical supervision, only stable, isolated fractures may allow limited weight-bearing with a boot or crutches. Unstable or displaced fractures do not allow this. Always get imaging and orthopaedic advice before trying to walk.
How long does a hairline fracture take to heal?
A hairline fracture (stress fracture) usually heals in 6 to 8 weeks, but some may take 10 to 12 weeks, depending on the location, such as the foot or hip. To heal properly, individuals need to rest, keep the affected area immobilized (with a cast or boot), and avoid activities that place excessive stress on the fracture.
What is a greenstick fracture?
A greenstick fracture is a partial break in which the bone bends and cracks on one side but does not break all the way through. It looks like a broken young "green" tree branch. These fractures often occur in children under 10 years because their bones are still growing and more flexible. They usually occur in long bones such as the radius, ulna, or tibia after a fall.
What is a transverse fracture?
A transverse fracture is a type of broken bone where the bone breaks at a straight-across angle to its long axis. High-force direct impacts, such as falls or car accidents, often cause these injuries. They most often occur in long bones such as the femur, tibia, and humerus, or in the vertebrae.
What is a comminuted fracture?
A comminuted fracture is a serious injury in which a bone breaks into three or more pieces. These fractures are often caused by high-impact trauma, like car accidents or falls, resulting in intense pain, swelling, and sometimes bone fragments that push through the skin (open fracture). In most cases, surgery is needed to hold the broken pieces together.
What are the symptoms of fractures?
Common symptoms of a fracture are severe pain immediately, swelling, bruising, and a visible change in shape or alignment of the limb. Other important signs include tenderness or pain on pressure/palpation, inability to move or put weight on the area, and possibly numbness or tingling. In very severe cases, bones may protrude through the skin.
What are the complications of fractures?
The complications from fractures include those that are early (immediate), like compartment syndrome (increased dangerous pressures in a muscle compartment during long bone fracture, if untreated, can cause permanent nerve and muscle damage), infections (which are common in open fractures), and nerve and vessel damage. Long-term complications include malunion, nonunion, and joint stiffness. In some cases, they can even lead to death.
Can fractures be prevented?
Yes, fractures can be prevented by strengthening bones and minimizing the risk of falls. The most important ways include consuming adequate amounts of calcium and vitamin D (rich in diet/supplements), engaging in weight-bearing exercise, quitting smoking, avoiding excessive drinking, and conducting a home safety assessment to prevent falls.
What are the most common causes of fractures?
Trauma, underlying conditions such as osteoporosis that affect the strength of the bone, and overuse or repetitive stress are the most common causes of fractures. These causes usually exceed the bone's breaking point.
How does age affect fracture healing?
Age has a significant effect on fracture healing, prolonging recovery and increasing the risk of nonunion (failing to heal) fractures in older people. Ageing leads to a reduction in the number of stem cells, vascularization (blood supply), and metabolic rate, in addition to the high prevalence of co-existing diseases such as osteoporosis.
Are fractures common in children?
Yes, fractures are very common among children. One-third of all children have experienced at least one fracture before the age of 17. Fractures are a major cause of emergencies and pediatric injuries. Children tend to heal rapidly because their bones are more pliable (flexible or bendable).
How do fractures heal in children compared to adults?
Children have bones that have a thicker periosteum (outer bone layer) and better blood supply, and their growth plates allow for correction of mild deformities. However, children can have severe and unstable fractures, which may require surgical repair, and adults can have good healing without surgery with the use of casts and splints for various fractures.
What is a pathological fracture?
A pathological fracture is a broken bone that occurs because of a disease that makes the bone weaker, not because of an injury or trauma. When the bone isn't strong enough, normal activities like walking or bending can break it. Some of the most common causes are osteoporosis, cancer (metastasis), infections, and metabolic disorders.
What is a tibia fracture?
The fractured tibia is the larger of the two bones in the lower leg. A broken shinbone can occur when someone falls, has an accident, or plays sports. Severe pain, swelling, bruising, and sometimes a change in shape (deformity) can be seen, which are some of the symptoms. It often requires immediate medical attention, and in severe cases, treatment may involve surgery or casting.
What is penile fracture?
Penile fracture is a condition that is relatively rare but occurs due to the tearing of the tunica albuginea covering the erectile tissues, usually while an individual is having sexual intercourse. It comes with a cracking sound, severe pain, an inability to sustain an erection, and swelling, requires urgent medical care.
What is a colles fracture?
The Colles fracture is one of the most prevalent fractures of the radius bone, which usually occurs about the wrist joint. The hallmark of this injury is the dorsally (towards the back) displaced radius bone. It usually occurs from a fall onto an extended arm (FOOSH) and manifests as a "dinner fork" deformity.
What is the difference between a fracture and a dislocation?
A fracture is when a bone breaks or cracks. When bones are pushed out of their normal place at a joint, this is called a bone dislocation. Both can damage surrounding ligaments (connect bones to other bones), tendons (connect muscles to bones), and tissues that surround a joint, resulting in pain, swelling and deformity.
What is the difference between a Monteggia fracture and a Galeazzi fracture?
The main difference between Monteggia and Galeazzi fractures is where the fracture and dislocation occur in the forearm. Monteggia is a fracture of the proximal ulnar bone with a dislocated elbow (radial head). Galeazzi is a fracture of the distal radius with a dislocated wrist (DRUJ). People often use the mnemonics "MU" (Monteggia-Ulna) and "GR" (Galeazzi-Radius).
What is the difference between a fracture and a sprain/strain?
A broken bone characterizes a fracture, whereas a sprain refers to torn or stretched ligaments, which connect the bones, while a strain affects the muscle and/or tendon. Fractures cause intense pain, deformity, and inability to use the injured area, whereas sprains/strains result in swelling, soft-tissue pain, and restricted joint movement.
When to consult a doctor for fractures?
Consult a doctor for fractures if there is immediate pain, swelling, or deformity after an injury. Signs that indicate a need for medical assistance are:
- Inability to move or put weight on the affected area
- Bone protrusion or an unnatural angle in the limb
- Loss of pulse, numbness, or tingling distal to the injury
- Excessive bleeding or an open wound over the fractured site
- Pain that worsens during movement and persists even at rest
If individuals have any of these symptoms, they should see an orthopaedic or fracture specialist for an accurate diagnosis through X-ray and the appropriate fracture treatment. If a fracture is suspected in the spine, pelvis, or hip, or if you have changed consciousness, chest pain, or trouble breathing, you should get emergency medical help right away. These could be signs of life-threatening problems.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868