Sepsis: Symptoms, Causes, Treatment & Prevention
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. Manasa Gaddam - Consultant Critical Care Specialist
Sepsis definition
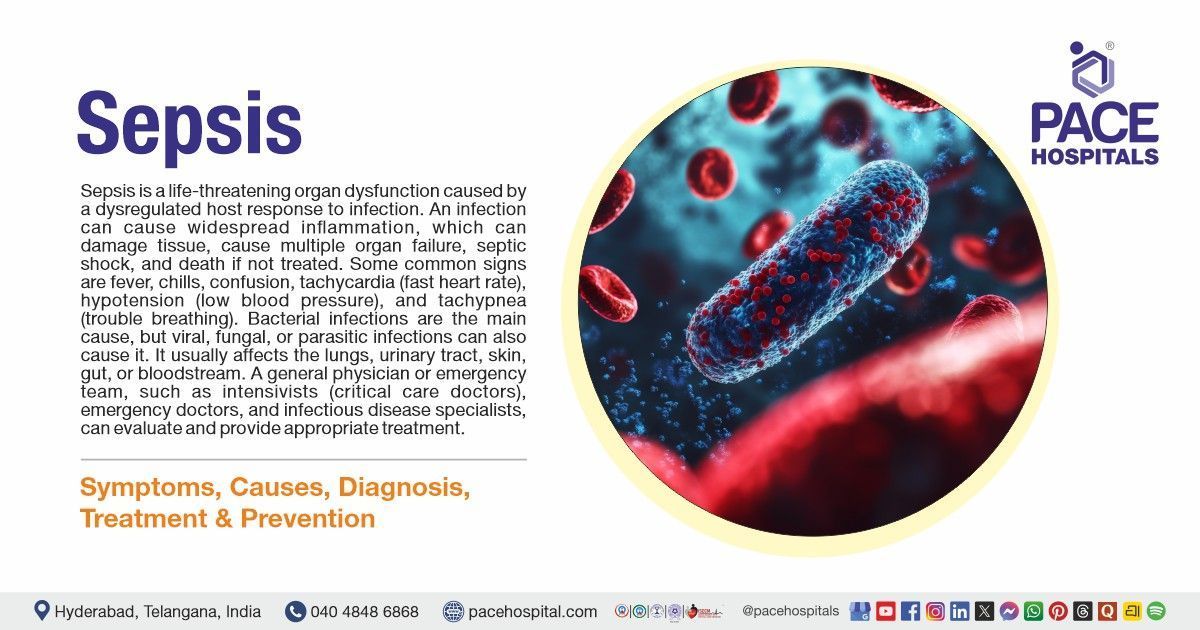
Sepsis is a life-threatening organ dysfunction caused by a dysregulated host response to infection. It happens when a preexisting infection triggers an inflammatory response throughout the body, resulting in complications like progressive tissue damage, multiple organ failure, septic shock (sepsis-induced organ dysfunction with persistent low blood pressure despite administration of fluids) and possibly death if not treated early. Healthcare teams diagnose sepsis based on physical signs and laboratory tests, such as fever with chills, confusion, breathing difficulty, low blood pressure, increased heart rate or weak pulse, and extreme pain, along with blood tests to detect infection or organ damage (e.g., blood cultures).
Bacterial infections mainly cause sepsis, but viral, fungal, or parasitic infections can also trigger it, and common affected organs include the lungs, skin, gastrointestinal tract, urinary tract, and bloodstream. Severe cases may result in long-term health problems due to organ dysfunction.
A
general physician or emergency team, such as intensivists (critical care doctors), emergency doctors, and infectious disease specialists, can evaluate and provide appropriate treatment.
Sepsis meaning
- Sepsis is derived from the ancient Greek word sepsis, meaning "rotting" or "decay," indicating that severe infections cause body tissues to rot.
- Ancient Greek physicians describe sepsis as putrefaction or decomposition in the body.
Sepsis means "putrefaction," which is a sign of the condition: the body's life-threatening reaction to an infection that causes organ dysfunction because of widespread inflammation, not the infection itself.
Sepsis Prevalence
Sepsis prevalence worldwide
Recent estimates show that sepsis is a major problem around the world. In 2020, there were about 489 lakh cases and 110 lakh deaths related to sepsis, which is almost 20% of all deaths in the world. These numbers, which come from World Health Organisation (WHO) data published in 2024, show that almost half of the cases happen in children under 5 years old. The highest rates of cases and deaths are in low- and middle-income countries.
Prevalence of sepsis in India
India has an estimated 82–113 lakh annual sepsis cases with 21–29 lakh deaths (~20–26% of global sepsis mortality), per Global Burden of Disease data up to 2021.ICU studies report 30–50% sepsis prevalence among admissions (25–45% mortality), driven by Gram-negative bacteria with high resistance.
Sepsis Pathophysiology
The following are the steps involved in the pathophysiology of sepsis, which include:
Dysregulated host immune response to infection
Sepsis begins when an infection triggers dysregulation of the immune response, rather than a controlled protective response, leading to damage to the host's tissues and organs.
Systemic inflammatory response (cytokine release)
Activated immune cells release excessive amounts of inflammatory mediators, such as cytokines and interleukins, leading to widespread systemic inflammation known as the systemic inflammatory response syndrome (SIRS).
Endothelial dysfunction and increased vascular permeability
Inflammatory mediators damage the vascular endothelium, causing vasodilation (dilation of blood vessels) and fluid leakage into the surrounding tissues, which results in hypotension (low blood pressure), oedema (swelling), and impaired blood and oxygen supply to the tissues (perfusion).
Activation of coagulation pathways(microthrombosis)
Systemic inflammation can further activate coagulation pathways and suppress fibrinolysis (breakdown of fibrin clots), resulting in the formation of blood clots (thrombi) in microvessels, known as microvascular thrombosis, which can impair blood supply to organs and cause organ dysfunction.
Circulatory and metabolic abnormalities
Sepsis can cause circulatory failure, leading to decreased cardiac output (reduced pumping of blood from the heart), vasodilation, and metabolic dysfunction (impaired body functions), resulting in tissue hypoxia and lactic acidosis (excessive lactic acid buildup).
Immunosuppression phase
After the initiation of systemic hyperinflammation, host counter-regulatory mechanisms may suppress immunity, increasing susceptibility to secondary infections.
Progression to organ dysfunction and multiorgan failure
Multiple organ dysfunction (lungs, kidneys, brain, heart and liver) can be due to persistent inflammation, microvascular thrombosis and hypoperfusion. If not treated immediately, it progresses to septic shock and death.
Sepsis Symptoms
Sepsis infection symptoms are clinical warning signs that appear when the body mounts an extreme, life-threatening immune response to an infection, indicating systemic inflammation and possible organ dysfunction that require immediate medical attention. The following are the signs and symptoms of sepsis:
Early sepsis symptoms
- Fever
- Tachycardia (rapid heart rate)
- Tachypnea (rapid, deep breathing)
Severe sepsis symptoms
- Altered mental status/confusion
- Oliguria (reduced urine output) or anuria (absence of urine output)
- Hypoxia (low blood oxygen)
- Cyanosis (bluish skin discoloration)
- Ileus
Common sepsis symptoms
- Clammy or sweaty skin
- Extreme pain or discomfort
- Hypotension
Fever: A fever is a temperature that is higher than 38 C, and hypothermia is a temperature that is lower than 36 C.
Tachycardia (rapid heart rate): Adult patients with tachycardia have a heart rate greater than 90 beats per minute, while pediatric patients have a heart rate above 2 standard deviations for their age.
Tachypnea (rapid deep breathing): Is when an adult's breathing rate exceeds 20 breaths per minute or is more than 2 standard deviations above their age-based reference.
Altered mental status/confusion: It means the brain isn't working properly due to cytokines, low oxygen levels, and metabolic problems, which worsen the prognosis. Altered mental status in severe sepsis is caused by systemic inflammation and low blood flow to the brain, which can lead to confusion, disorientation, or coma.
Oliguria (reduced urine output) or anuria (absence of urine output): Oliguria (less than 0.5 mL/kg/h of urine) or anuria in severe sepsis indicates that the kidneys have been injured rapidly due to low blood flow and inflammation. It shows that the kidneys aren't working right, which is usually a sign that creatinine levels are rising. This means a higher risk of death.
Hypoxia (low blood oxygen): In severe sepsis, hypoxia occurs due to inflammation that causes acute lung injury, acute respiratory distress syndrome (ARDS), or a mismatch between ventilation and perfusion. It shows up as low oxygen saturation, which can lead to multiple organ failure and problems with thinking.
Cyanosis (bluish skin discoloration): Cyanosis occurs in severe sepsis due to significant hypoxemia and inadequate tissue perfusion, resulting in bluish discolouration of the skin. Peripheral or central cyanosis indicates circulatory failure, frequently accompanied by the advancement of septic shock.
Ileus: When someone has severe sepsis, ileus occurs when inflammation, ischemia, and autonomic dysfunction stop peristalsis, making the gut not work properly. It makes the stomach swell, makes you feel sick, and speeds up the movement of bacteria, worsening the infection.
Clammy or sweaty skin: Excessive sweating and cold, clammy skin (cold sweating) occur due to activation of the sympathetic nervous system, indicating poor perfusion of blood to tissues and circulatory shock, which is common in severe sepsis.
Extreme pain or discomfort: Patients experience the worst pain ever, which is indicated as systemic organ stress due to widespread systemic inflammation that causes tissue injury and cytokine release, which is an inflammatory mediator released in response to infection.
Hypotension (low blood pressure): Hypotension in sepsis occurs because of the activation and dysregulation of the body’s systemic inflammatory response to an infection, leading to multiple hemodynamic disturbances and low blood pressure.

Sepsis Causes
Sepsis can occur because of preexisting infection, which triggers an abnormal immune response in the body, leading to widespread systemic inflammation and organ damage. The most commonly targeted organs are the lungs, skin, urinary tract, and abdomen, and the condition rapidly progresses if untreated. The following are the causes of sepsis infection, which include:
- Bacterial infections
- Viral infections
- Fungal infections
- Infections in specific body sites
- Bloodstream infections (bacteremia or fungemia)
- Hospital-acquired infections
Bacterial infections: These are the most common causes of sepsis: bacteria such as Escherichia coli and Staphylococcus aureus enter the body through various infections, which can stimulate a severe systemic inflammatory response leading to sepsis.
Viral infections: Viruses such as influenza or dengue virus can increase the risk of secondary bacterial sepsis when the body’s immune response becomes uncontrolled. This dysregulation results in the release of inflammatory cytokines, causing vascular leakage (widespread), organ dysfunction and septic shock.
Fungal infections: Immunocompromised or weakened immunity patients are prone to the development of sepsis when various fungi, such as Candida, Mucorales, or Aspergillus, invade the bloodstream and spread widely systemically, leading to fungemia and multiorgan dysfunction.
Infections in specific body sites: Various bacterial infections can trigger sepsis in major organs, including the lungs (pneumonia), the urinary tract, the gastrointestinal tract, and the skin and wounds. They can also affect tissues that spread to the bloodstream, leading to a dysregulated immune response and potential multiorgan dysfunction.
Bloodstream infections (bacteremia or fungemia): When bacteria or fungi enter the bloodstream, they activate the body's immune system, leading to systemic inflammation and organ dysfunction, which can result in sepsis.
Hospital-acquired infections: Patients who are in the hospital for a long time may get sepsis from surgical site infections, catheter-related infections, or ventilator-associated infections. These are some of the most common healthcare-associated infections (HAIs) in intensive care settings.

Risk Factors for Sepsis
Sepsis can affect any age, but certain groups are at higher risk due to age, underlying chronic illnesses, weakened immunity or recent exposure to medical care in a hospital. The following are the sepsis risk factors, which include:
- Extremes of age (Neonatal sepsis)
- Chronic medical conditions
- Weakened immune system
- Recent severe illness, surgery or hospitalization
- Pregnancy and postpartum (puerperal sepsis)
- Previous episode of sepsis
- Hospitalized or ICU patients
Extremes of age (Neonatal sepsis): Neonatal sepsis is a risk for babies, especially those who are less than 28 days old. It can happen "early-onset" (from the mother during birth) or "late-onset" (in the hospital or community). Because a newborn's immune system isn't fully developed, the infection may rapidly spread to the brain and blood (meningitis).
Chronic medical conditions: Underlying disease conditions like diabetes associated with excessive blood sugar-induced infections, kidney disease (dialysis patients are more prone to sepsis because of vascular access infections, liver disease (cirrhosis) associated with bacterial peritonitis due to ascites (fluid buildup), lung disease (pneumonia) and other chronic illnesses increase infection risk leading to sepsis.
Weakened immune system: Several conditions, like cancer, human immunodeficiency virus disease (HIV) and patients indicated for immunosuppressive therapy, like chemotherapy in various cancer conditions, are more prone to the development of infections because of compromised immune activity (the body's ability to fight against infections), leading to sepsis risk.
Recent severe illness, surgery or hospitalization: Recent hospitalization or invasive procedures (catheters, ventilators) increase the risk of infections, and about 10-15% of adult cases of sepsis usually start primarily in the hospital itself. Identification of early sepsis symptoms, such as fever and difficulty breathing, is essential in these patients to prevent progression to septic shock.
Pregnancy and postpartum (puerperal sepsis): Women who are pregnant or have just given birth are at risk of puerperal sepsis (also called postpartum sepsis). It is a dangerous infection of the genital tract that can happen anytime between the start of labor or the rupture of membranes and the 42nd day after giving birth. It is still one of the "big five" things that kill pregnant women around the world.
Previous episode of sepsis: Individuals who previously been affected by sepsis infection and recovered are referred to as sepsis survivors; they are highly prone to the development of sepsis again in the future because of their previous sepsis history.
Hospitalized or ICU patients:
Patients who are admitted to hospitals, especially in intensive care units or receiving any interventional procedures due to the use of invasive devices like central lines and ventilators, are at higher risk of healthcare -associated infections leading to sepsis. While central venous catheterization and mechanical ventilation (artificial breathing support for patients who do not breathe on their own adequately) further lead to secondary infections in those already septic.
Complications of Sepsis
Sepsis can cause serious and life-threatening complications if not treated immediately, because it can damage tissues and organs due to the body's immune response to infections. Severe sepsis cases may progress to shock, multiple organ failure or even death. The following are the sepsis complications, which include:
- Septic shock
- Multiple organ failure
- Tissue damage and blood clotting disorders
- Death
- Increased risk of future infections
- Post-sepsis syndrome (long-term physical and psychological effects)
Septic shock: Sepsis, if not treated immediately, can progress to septic shock. It is a severe condition associated with dangerously low blood pressure, even on administration of fluids and decreased perfusion (blood flow, oxygen supply) to the vital organs like the brain, kidney, lungs, liver and heart, resulting in increased risk of death. Septic shock can occur when the body's immune response to infection causes circulatory (low cardiac output) and metabolic abnormalities.
Multiple Organ Failure: Organ dysfunction, also called organ failure, is generally caused by sepsis and leads to multiple organ failure involving the liver, kidneys, heart, lungs, and brain. This occurs due to impaired hypoperfusion and oxygen supply, tissue damage, and systemic inflammation resulting from immune system activation in response to infections.
Tissue damage and blood clotting disorders: Sepsis may cause abnormal blood clotting and reduced blood supply to vital organs, leading to tissue damage and organ dysfunction. The development of small blood clots in blood vessels or bleeding will harm tissues and organs.
Death: Both sepsis and septic shock can result in death if not identified early and treated immediately. Mortality rate is the rate of death, which increases significantly with multiple organ failure and septic shock.
Increased risk of future infections: Sepsis survivors are highly prone to the development of infections in later life because of differences in the immune system. Sepsis can weaken immune defenses against severe infections over time, thereby increasing the risk of future infections.
Post-sepsis syndrome (long-term physical and psychological effects): After recovery from sepsis, patients may experience various symptoms such as weakness, fatigue (low energy), anxiety, depression or mood changes, basically ranging for months or years, and these long-term complications are known as post-sepsis syndrome.
Sepsis Diagnosis
Evaluation of sepsis includes early clinical suspicion, scoring systems, laboratory tests, biomarkers, and microbial investigations to detect infection and organ dysfunction. Accurate detection of sepsis is essential for early treatment support and improved survival outcomes.
The following are the steps commonly included in the sepsis diagnostic criteria:
- Medical history
- Physical examination
- Early screening tools
- Systemic Inflammatory Response Syndrome (SIRS) criteria
- National Early Warning Score (NEWS)/Modified Early Warning Score (MEWS) for initial suspicion
- Initial Laboratory investigations
- Complete blood count (CBC)
- Blood cultures
- Urinalysis and source cultures
- Serum lactate
- Chemistry panel
- Inflammatory markers
- Coagulation profile
- Liver function tests
- Arterial blood gas
- Serum glucose monitoring
- Blood urea nitrogen (BUN)
- Serum electrolytes
- Imaging and Targeted Test
- Chest X-ray
- Extremity X-rays
- Ultrasound/CT scan
- Lumbar puncture
- Scoring systems
- Sequential organ failure assessment qSOFA score
- Full SOFA score
Sepsis Treatment
Sepsis treatment guidelines emphasize early identification and prompt management to prevent organ failure and reduce mortality. Early interventions, such as supportive care, antibiotics, and fluid administration, are essential in sepsis treatment to stabilize the patient and control infection. The following steps are involved in sepsis management:
- General supportive ICU measures
- Early recognition and diagnosis
- Immediate Antimicrobial therapy (within 1 hour)
- Intravenous fluid resuscitation
- Vasopressors (if hypotension persists)
- Source control of infection
- Oxygen and respiratory support
- Hemodynamic monitoring and organ support
- Intensive care unit (ICU) management
- Adjunctive therapies (if needed)
- Corticosteroids
- Blood transfusion
- Prevention and follow-up care
Non-pharmacological therapy
- Supportive care
- Nutritional support
- Temperature management
- Non-conventional immunomodulatory approaches
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support

Sepsis Prevention
Sepsis prevention protocols mainly focus on early infection prevention, early identification, and immediate treatment to prevent progression to sepsis. The following are the steps involved in the prevention of sepsis:
- Maintaining good hygiene to prevent infections
- Early treatment of infections
- Vaccination according to national immunization schedules
- Infection prevention and control (IPC) in healthcare facilities
- Management of chronic conditions
- Maintain good nutrition and breastfeeding in infants
- Improve sanitation and access to clean water
- Recognise early signs and seek urgent medical attention
- Health education and awareness programs
Maintaining good hygiene to prevent infections: Maintaining good personal hygiene by washing hands regularly with alcohol based handwash, practising safe food preparation and avoiding unsanitary conditions like dirty, unclean or unhygienic conditions. These are the key prevention management steps that reduce exposure to bacteria, fungi and viral pathogens that can cause infections leading to sepsis.
Early treatment of infections: Sepsis can be prevented by early diagnosis and immediate, accurate treatment with selective, appropriate therapy, such as antibiotics to kill bacterial pathogens, antifungals to treat fungal infections, and antivirals to treat viral infections, to prevent progression to systemic infection and organ dysfunction. The therapy is selected based on susceptible pathogens.
Vaccination according to national immunization schedules: Administration of timely vaccinations scheduled according to the national immunisation protocol for various serious infections, such as pneumonia (fluid buildup in the lungs caused by pneumococcal bacteria), meningitis (inflammation of the brain meninges due to meningococcal bacterial infection), and influenza virus, which are common triggers of sepsis. So, vaccination helps in reducing the severity or occurrence of infections that may lead to sepsis.
Infection prevention and control (IPC) in healthcare facilities: Practising IPC programs in hospitals is essential to maintain and follow strict hygiene protocols, such as sterilising all equipment, including ventilators and catheters, especially in ICU settings; handwashing; and cleaning protocols, which are essential to prevent hospital-acquired infections that may lead to sepsis.
Management of chronic conditions: Individuals suffer from various chronic and long-term conditions like diabetes, cancer, kidney disease and autoimmune conditions like rheumatoid arthritis, systemic lupus erythematosus, where immunity is compromised, and they are highly prone to the development of infections because the body's ability to fight against infections is reduced. So proper disease control reduces sepsis risk.
Maintain good nutrition and breastfeeding in infants: Consuming healthy fruits and vegetables by adults helps boost immunity, and breastfeeding provides newborns with protection against infections through breast milk, which contains immunoglobulins, helping neonates build strong immunity and reduce sepsis risk.
Improve sanitation and access to clean water: Maintaining good hygiene, including clean water and sanitation, helps prevent the transmission of diseases by safely managing garbage and human waste. It helps prevent illnesses like diarrhoea and cholera (bacterial infections transmitted through contaminated water), which can be transmitted via the faecal-oral route. So, improving water quality and sanitation in the community helps prevent sepsis.
Recognise early signs and seek urgent medical attention: Identification of early signs and symptoms of infection helps prevent the progression of a simple infection to sepsis or severe sepsis, which can lead to septic shock. Seeking medical care immediately is essential to reduce the risk of sepsis.
Health education and awareness programs: Conducting health awareness programs on sanitation practices and healthy habits is important for preventing various infections in the community. Educating people by healthcare workers helps in early detection, prevention behaviour, and adherence to protocols. All these practices help in preventing sepsis.
Difference between Septicemia and Sepsis
Septicemia vs Sepsis
Septicemia and sepsis are related but not similar clinically. Septicemia refers to the infection in the bloodstream, and sepsis is a life-threatening emergency condition, involving immune system activation and response to infection that can cause organ failure and possibly death. Below are the key differences between septicemia and sepsis.
| Characteristics | Septicemia | Sepsis |
|---|---|---|
| Definition | It is defined as an infection in the bloodstream caused by bacteria, rarely viruses or fungi. Septicemia is also called blood infection. | It is a life-threatening systemic immune response of the body to an infection, causing organ failure and possibly death if not treated promptly. |
| Pathophysiology | Bacteria or other infecting pathogens enter the lungs or the urinary tract, then enter the blood and multiply there. | Activation of the immune system and dysregulation (cytokine release), endothelial damage, and lack of blood supply to tissue (hypoperfusion) can lead to organ dysfunction. |
| Primary cause | Direct invasion of a microorganism into the bloodstream indicates local infection. | It is stimulated by infections (pneumonia, UTI), leading to widespread immune reactions, including systemic inflammation, which can cause tissue damage and organ failure. |
| Clinical scope | It is mainly targeting to treat bloodstream infection and requires blood cultures for diagnosis. | Targeting the entire body because of widespread infection, causing systemic inflammation, tissue damage and organ failure |
| Severity | Septicemia can be mild to severe and may progress to sepsis. | Sepsis is a serious emergency condition that always requires immediate medical attention. |
| Complications | It can progress to sepsis and septic shock if not treated immediately. | It can cause septic shock, acute respiratory distress syndrome (ARDS), multiple organ failure and death. |
| Terminology usage | It is an older term that is sometimes used as a synonym, but technically it refers to bloodstream infections. | It is a current standard term used in modern clinical practice and guidelines. |
| Clinical outcome | Septicemia may be resolved with early treatment (antibiotics) or progress to sepsis otherwise. | Early treatment with antibiotics, fluid and ICU care improves the survival rate; otherwise, sepsis can lead to death if not treated immediately. |
Difference between Bacteremia and Sepsis
Bacteremia vs Sepsis
Both bacteremia and sepsis are related, but clinically, they differ in the infectious diseases they cause. Understanding the differences between them is essential for accurate diagnosis and treatment. Below are the key differences between bacteremia and sepsis.
| Characteristics | Bacteremia | Sepsis |
|---|---|---|
| Definition | It is defined as the presence of bacteria in the bloodstream, detected by blood culture. | It is a body’s extreme and dysregulated immune response to an infection, causing systemic illness leading to life-threatening organ dysfunction. |
| Cause | Bacterial pathogens enter the bloodstream via local infection sites, wounds, catheters or during procedures. | Various infections, such as bacteria, viruses, fungi, and parasites, can trigger a systemic inflammatory response. |
| Nature | Laboratory condition (microbiological finding). | Clinical syndrome and medical emergency. |
| Systemic response | May occur without systemic inflammatory response. | An always systemic, inflammatory, and dysregulatory host response is present. |
| Symptoms | Mostly asymptomatic (symptoms absent), mild (fever, chills). | Severe symptoms such as low blood pressure (hypotension), confusion and difficulty breathing. |
| Severity | Usually mild and may resolve by using antibiotics. | Severe cases can cause death if untreated immediately. |
| Progression | Can progress to sepsis if untreated. | Sepsis can progress to septic shock and multiple organ dysfunctions if not treated promptly. |
| Clinical status | It is not always life-threatening. | It is a medical emergency with high mortality risk. |
Frequently Asked Questions (FAQs) on Sepsis
How long does it take to die from sepsis?
Sepsis can be fatal (death risk), especially when it progresses to the severe stage of sepsis known as septic shock, as little as about 12 hours after the beginning of symptoms if treatment is delayed. The exact time for fatal risk varies based on the severity of the disease, patient health and treatment response. Still, if sepsis remains untreated, it can be fatal within hours to days; for this reason, it is considered a medical emergency requiring immediate medical attention. The risk of mortality increases every hour by approximately 7.6% to 9% if not treated immediately.
What is the most common cause of sepsis?
The most common cause of sepsis is bacterial infection, which usually initiates in the lungs (pneumonia caused by Streptococcus pneumoniae bacteria), skin (Staphylococcus aureus), digestive tract (Escherichia coli), and urinary tract infections (Escherichia coli), which stimulate the immune response to infection, spreading widely and dysregulated throughout the body.
What bacteria cause sepsis?
Various bacteria, both gram-positive and gram-negative, can cause sepsis, including Staphylococcus aureus, Escherichia coli, Klebsiella species, and Pseudomonas aeruginosa. These organisms usually affect organs such as the lungs, skin, urinary tract, or gastrointestinal tract by initiating a host immune response to infections that is widespread and dysregulated.
What are the early warning signs of sepsis?
The early signs of sepsis include a combination of symptoms such as fever, chills or feeling very cold, confusion or altered mental status, difficulty breathing, low blood pressure (hypotension), rapid heartbeat or weak pulse, sweaty or clammy (cold-sweat) skin, and extreme pain or discomfort. All these warning signs indicate that sepsis is a medical emergency requiring immediate medical attention; otherwise, it can lead to progressive organ failure and death if not treated immediately.
Can sepsis cause kidney failure?
Yes, sepsis can cause acute kidney injury and if severe or untreated can cause permanent severe renal failure as it is a life-threatening medical emergency in which the body’s response to extreme infection, causing widespread systemic inflammation, can rapidly damage tissue, organ failure and death if not treated immediately. As kidneys are among the vital organs that can fail during this process because of impaired blood flow and systemic inflammation if untreated.
How to avoid sepsis?
To avoid sepsis, it is recommended to get vaccinations on time to prevent infections (for the flu, COVID-19, and pneumonia). Taking care of wounds, managing chronic health conditions, and seeking medical help immediately if signs of infection are noticed. Cleaning and covering cuts, eating well, and avoiding sick people are all important steps. It is important to take care of chronic illnesses like diabetes and cancer, and get medical help right away if you notice signs of an infection, like a fever or confusion.
What is sepsis?
Sepsis is a life-threatening medical emergency characterised by the host's extreme immune activation and dysregulated response to an infection, rather than a controlled protective response, leading to tissue damage, organ dysfunction and possibly death if not treated. It occurs through the release of inflammatory mediators, such as cytokines and leukotrienes, into the bloodstream, causing widespread systemic inflammation. Treating immediately with antibiotics and fluid is essential.
Is sepsis contagious?
No, sepsis itself is not contagious because it is not a communicable disease (it does not spread from one individual to another), as it is an extreme immune response to infection rather than an infectious disease itself. However, the underlying conditions, such as causative bacteria like Staphylococcus aureus or Escherichia coli that trigger sepsis, can be contagious, but sepsis itself is not contagious.
Can sepsis cause seizures?
Yes, sepsis can cause seizures. This is usually a sign of sepsis-associated encephalopathy (SAE), which is associated with severe systemic inflammation, cytokine release (an inflammatory mediator), and metabolic problems that make the brain work less well. These seizures can be either convulsive (rapid jerky shaking of the body) or nonconvulsive (non-jerky moments usually characterised by confusion, behavioural changes, and unresponsiveness), and they raise the risk of having more seizures in the future.
What is the difference between sepsis and septic shock?
Sepsis is a life-threatening medical emergency that triggers an immune response to infection, causing damage to tissues and organs. The body's response to infection hurts its own tissues. Septic shock is the most severe stage, with dangerously low blood pressure and cellular problems that don't go away even after fluids are given. This stage often ends in death if not treated promptly.
Why does sepsis cause hypotension (low blood pressure)?
Sepsis causes low blood pressure (hypotension) mainly by triggering a strong systemic inflammatory response to infection, which dilates blood vessels (vasodilation) and makes capillaries more permeable. These dilated blood vessels and fluid leakage into nearby tissues reduce blood volume and blood pressure significantly (hypotension). So, in this way, sepsis lowers blood pressure.
How does pneumonia cause sepsis?
Pneumonia can cause sepsis by activating the immune system and spreading widely throughout the body rather than remaining locally. The body's immunity in this condition dysregulates leading to systemic widespread infection, thrombosis (formation of blood clots) which progresses to organ failure including acute respiratory distress syndrome (it is a severe life-threatening respiratory failure characterized by lung inflammation and fluid buildup in alveoli leading to low blood oxygen levels), which is a complication from lung micro vessel injury and fluid leakage in to surrounding tissues, that exacerbates respiratory failure and multiorgan dysfunction.
What are the symptoms of septic shock?
Septic shock includes symptoms such as severe low blood pressure (hypotension) that doesn't go away even after giving fluids, confusion or altered mental status, fever/chills or low body temperature, rapid heart rate, difficulty breathing, pale skin, reduced urine output, weakness or lethargy. It is the dangerous step of sepsis that requires immediate medical attention; otherwise, it leads to organ failure and death if not treated promptly.
Is sepsis the same as septicemia?
Sepsis and septicemia are not the same thing, even though they are very similar and are often used to mean the same thing. Septicemia is a type of bloodstream infection (blood poisoning) that can lead to sepsis. Sepsis is the body's extreme, life-threatening immune response to an infection. Septicemia frequently progresses and induces sepsis.
Does septicemia always cause sepsis?
Septicemia does not always cause sepsis. Septicemia occurs when bacteria or toxins enter the bloodstream (blood poisoning), which can lead to sepsis. Sepsis is a more serious condition that can occur when the body's immune system doesn't work properly against infections, not just those in the bloodstream. This includes infections limited to one area, such as pneumonia, urinary tract infections, skin infections, and viral and fungal infections.
When to consult a doctor for sepsis?
Consult a doctor for sepsis if you experience fever, chills, rapid heart rate, or rapid breathing following an infection. Signs that indicate a need for medical assistance are:
- Confusion, disorientation, or altered mental state
- Extreme pain or discomfort
- Shortness of breath or difficulty breathing
- Clammy, sweaty, pale, or blotchy skin
- Low urine output or no urination for more than 12 hours
If these symptoms continue, it is best to see an infectious disease (sepsis specialist) or an emergency physician for an accurate diagnosis and treatment. It is recommended to seek emergency medical attention if individuals experience severe confusion, a non-blanching rash (red, purple, or brown spots), blue lips, or breathing failure, as these may signal septic shock. A general physician or emergency team can provide appropriate sepsis treatment with antibiotics and supportive care to manage symptoms and reduce mortality.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868