Minimally Invasive Cardiac Surgery (MICS) | Procedure & Cost
PACE Hospitals is recognized as one of the best hospitals for minimally invasive cardiac surgery in Hyderabad, India, offering advanced MICS or keyhole heart surgery, through small chest incisions. These minimally invasive heart surgery techniques reduce pain, blood loss, and hospital stay compared to open-heart surgery.
As a leading center for minimally invasive cardiac surgery in Hyderabad, our expert cardiac surgeons perform complex procedures with precision and safety. We provide keyhole heart surgery for valve disorders, selected coronary artery disease, and structural heart conditions, supported by advanced technology and comprehensive cardiac care for faster recovery.
Book an Appointment for MICS Surgery
MICS Surgery Appointment
Why Choose PACE Hospitals for Minimally Invasive Heart Surgery?
Trusted Cardiac Surgeons with Expertise in Complex Minimally Invasive Heart Surgeries
Smaller Incisions, Reduced Blood Loss & Faster Post-Surgery Recovery with MICS
Cost-Effective Minimally Invasive Cardiac Surgery with Insurance & Cashless Support
Doctors for MICS Surgery
Dr. Seshi Vardhan Janjirala
Interventional Cardiologist, Specialist in Endovascular Procedures
14 years of expertise
Expertise
- Advanced coronary angiography and imaging for MICS suitability assessment
- Pre-procedural planning and risk stratification for minimally invasive cardiac surgery
- Hybrid cardiac procedures in collaboration with MICS cardiac surgeons
- Catheter-based evaluation and management before and after MICS procedures
Dr. Shriniwas Rajamouli Dussa
Cardiothoracic & Vascular Surgeon
24 years of expertise
Expertise
- Minimally Invasive Cardiac Surgery (MICS) for coronary and valvular heart diseases
- Small-incision and thoracoscopic cardiac procedures with faster recovery outcomes
- Advanced MICS techniques including valve repair and coronary bypass approaches
- Comprehensive perioperative management and post-MICS rehabilitation planning
Minimally Invasive Cardiac Surgery Definition
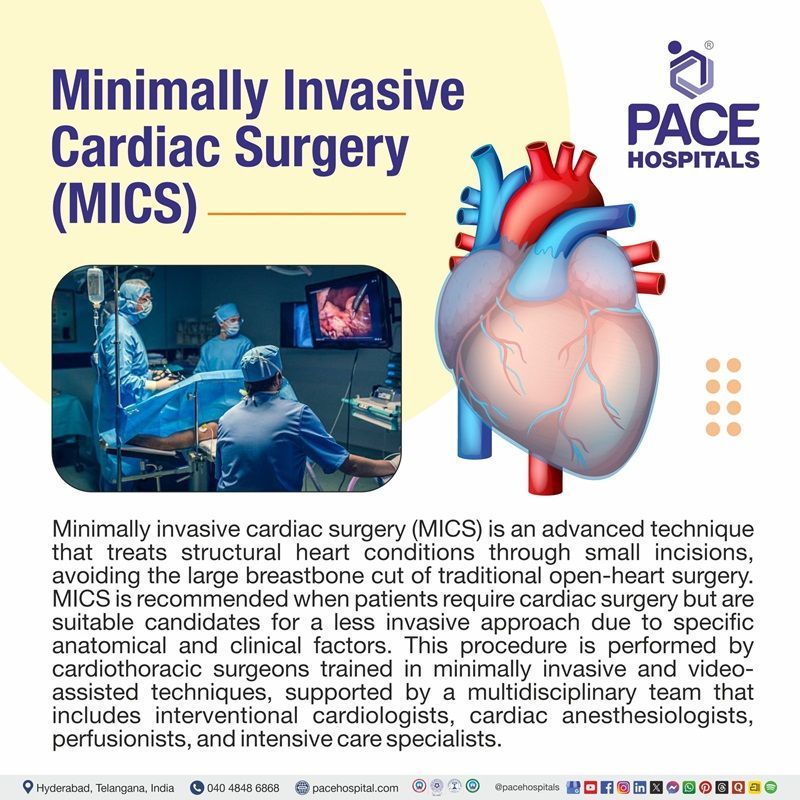
Minimally invasive cardiac surgery (MICS) is an advanced cardiac procedure performed through small incisions to treat structural heart problems without the need for a full breastbone cut, unlike traditional open-heart surgery. MICS aims to repair or replace diseased heart valves, correct congenital defects, or perform coronary bypass using less trauma, faster healing, and improved cosmetic outcomes.
MICS is recommended when patients require cardiac surgery but are suitable candidates for a less invasive approach due to specific anatomical and clinical factors. This surgery is suggested when patients want reduced blood loss, a shorter hospital stay, fewer complications, and a quicker return to daily activities.
This surgery is performed by a multidisciplinary team of cardiac surgeons specialising in minimally invasive and robotic-assisted techniques. This procedure is performed by cardiothoracic surgeons trained in minimally invasive and video-assisted techniques, and supported by interventional cardiologists, cardiac anaesthesiologists, perfusionists, and intensive care specialists.
Types of Minimally Invasive Cardiac Surgeries
MICS comprises a broad range of surgical techniques designed to reduce tissue trauma while achieving the same therapeutic goals as conventional open-heart surgery. These techniques involve keyhole (smaller incisions), specialised equipment, and video- or robotic-assisted technologies, and these surgeries are selected depending on the patient's pathology, anatomy, and overall risk profile. The major types of MICS include:
Core Categories by Indication
- Minimally invasive coronary artery bypass surgery
- Minimally invasive valve surgery
- Minimally invasive atrial septal defect (ASD) repair
- Minimally invasive arrhythmia Surgery
Enabling Technologies and Advanced Applications
- Robotic-assisted cardiac surgery
- Minimally Invasive Heart Failure Interventions
Minimally invasive coronary artery bypass surgery
This technique repairs blocked coronary arteries through small chest incisions (partial sternotomy or mini-thoracotomy) without fully opening the chest. Hybrid coronary revascularisation combines minimally invasive bypass surgery with coronary stenting to treat blockages. Surgeons perform a small-incision bypass to the most critical artery (usually the LAD), and interventional cardiologists place stents in the other blocked arteries.
Minimally invasive valve surgery
This surgery repairs or replaces diseased mitral or aortic valves through mini-thoracotomy or partial sternotomy, using small incisions and specialised tools. The heart is accessed through narrow spaces, allowing the valve to be corrected without a whole chest opening. Tricuspid valve repair/replacement (TVR) surgery is performed through a right mini-thoracotomy or keyhole incisions instead of opening the whole chest. Surgeons repair or replace the tricuspid valve using long, slender instruments and endoscopic vision. This approach is increasingly preferred for tricuspid regurgitation and combined valve disease.
Minimally invasive atrial septal defect (ASD) repair
This surgery uses small thoracic incisions with endoscopic or robotic assistance to close the defect in the atrial septum. This approach avoids the larger sternotomy and offers faster recovery with similar safety and efficacy.
Minimally invasive Arrhythmia Surgery
The minimally invasive Maze procedure treats atrial fibrillation by creating precise lines of scar tissue in the atria using radiofrequency or cryotherapy delivered through small incisions. These lines block abnormal electrical signals that cause irregular heart rhythm.
Robotic-Assisted Cardiac Surgery
This surgery uses a robotic system to perform heart procedures through very small keyhole incisions. This technique is commonly used for mitral valve repair, tricuspid valve surgery, coronary artery bypass (in selected cases), and atrial septal defect repair.
Minimally Invasive Heart Failure Interventions
A minimally invasive VAD implantation involves placing a mechanical pump that helps a weak heart pump blood, but through small thoracic incisions instead of a full sternotomy. Surgeons insert the device using limited-access approaches on the left side of the chest.

Minimally Invasive Cardiac Surgery Indications
Minimally invasive cardiac surgery is recommended for patients who require cardiac procedures but are suitable for smaller incisions instead of a full sternotomy. Common indications include:
- Coronary artery disease (CAD)
- Valvular heart disease
- Rhythm surgery
- Atrial septal defects (ASD)
- Anatomical factors favouring MICS
- Additional procedures
Coronary artery disease (CAD)
It is indicated for patients with coronary artery disease when bypass grafting can be safely performed through small chest incisions. It is beneficial for blockages in the left anterior descending (LAD) artery or other vessels accessible through a mini-thoracotomy.
Valvular heart disease
Conditions such as severe mitral regurgitation, aortic stenosis, or significant tricuspid regurgitation are commonly treated using this approach. Minimally invasive valve surgery is chosen when it can provide the same surgical benefit as conventional surgery with less trauma and a faster recovery.
Rhythm surgery
Patients with atrial fibrillation (AF) may qualify for MICS if their irregular heart rhythm does not improve with medications or catheter ablation. Using these small thoracoscopic openings, surgeons can create accurate scar patterns that prevent incorrect electrical signals. This method is recommended because it effectively restores rhythm without requiring a full sternotomy.
Atrial septal defects (ASD)
Patients with an ASD that requires surgical closure are strong candidates for minimally invasive repair. The procedure can be performed through small right-sided chest incisions using long instruments and endoscopic visualisation. It is most suitable for simple secundum ASDs and patients with favorable chest anatomy.
Anatomical factors favouring MICS
MICS is indicated when the patient’s physical anatomy supports a safe small-incision approach. Ideal anatomical factors include a normal chest structure, minimal scar tissue from past surgeries, and good peripheral vessels for cannulation. Patients at high risk for sternum healing problems (such as those who are obese, diabetic, or elderly) also benefit.
Additional procedures
Many other heart procedures can be done effectively with minimal incisions, making them indications for MICS. These include left atrial appendage closure, removal of small tumours, pericardial procedures, and selected congenital repairs.

Minimally Invasive Cardiac Surgery Contraindications
MICS is usually safe and effective for many patients; certain medical conditions, anatomical, or technical factors may make the approach unsuitable. In such situations, a standard open heart surgery may offer better exposure, safer cannulation, and more reliable operative control to the surgeon. The major contraindications to minimally invasive cardiac surgery include the following:
- Emergency or unstable situations
- Complex anatomical issues
- Severe lung disease
- Higher age
- Severe pectus excavatum
- Previous cardiac surgeries
- Patient preference
Emergency or unstable situations
Hemodynamic instability or emergency surgery that requires immediate intervention makes minimally invasive cardiac surgery contraindicated. This is because there is limited access for quick resuscitation, longer setup times, and a greater chance of having to switch to sternotomy. These factors can lead to worse outcomes than those seen with direct open access.
Complex anatomical issues
Patients with complex heart or chest anatomy often cannot undergo minimally invasive cardiac surgery. Severe aortic calcification, unusual heart position, enlarged chambers, or complex valve anatomy can limit visibility and instrument movement through small incisions.
Severe lung disease
Severe lung diseases such as advanced chronic obstructive pulmonary disease (COPD) or restrictive lung conditions make minimally invasive surgery risky because the procedure usually requires one-lung ventilation. Patients with poor lung function cannot tolerate collapsing one lung, which may cause dangerously low oxygen levels or respiratory failure.
Higher age
Old age by itself is not a strict barrier. However, it combines with frailty, a high EuroSCORE, or other health issues to discourage minimally invasive cardiac surgery (MICS). This combination raises the risks during and after surgery, as the benefits of less access may not make up for longer procedure times in at-risk patients.
Severe pectus excavatum
Severe pectus excavatum alters the shape and position of the chest cavity, making it difficult to access the heart through small side incisions. This causes limited working space and poor visibility during minimally invasive surgeries.
Previous cardiac surgeries
Patients who have undergone previous heart surgeries often develop scar tissue inside the chest. These adhesions increase the risk of injury to the heart, grafts, or lungs when entering through small incisions. Minimally invasive access becomes unsafe because the surgeon cannot predict the exact location of the scarred structures.
Patient preference
If a patient refuses or prefers minimally invasive heart surgery, it is a clear reason not to proceed. Surgery cannot happen without informed consent, and ethical guidelines require full patient agreement. Patients may refuse for various reasons, such as fear, misunderstanding, cultural beliefs, or a preference for a different method.

Benefits of Minimally Invasive Cardiac Surgery
Minimal invasive cardiac surgery offers several advantages compared with traditional open-heart surgery. Instead of using the traditional surgical method, surgeons operate through small keyhole-sized openings, which reduces physical stress on the body. The benefits listed below highlight why this method is increasingly preferred for eligible patients:
- No opening of the chest or cutting of bones
- Faster recovery
- Minimal pain
- Decreased blood loss and no need for blood transfusion
- Minimal scarring
- Shorter hospital stay
- Lower risk of complications
No opening of the chest
In MICS, the surgeon uses small keyhole cuts instead of splitting the breastbone (sternotomy). Because the chest is not fully opened, the body experiences less trauma. This makes the surgery gentler compared to traditional open-heart surgery.
Faster recovery
In MICS, the bones are not cut, and there is less tissue damage, allowing the body to heal more quickly. Patients can return to normal activities weeks earlier than with traditional open-heart surgery.
Minimal pain
Less disruption of muscles, bones, and soft tissue leads to significantly reduced postoperative pain. Many patients require fewer pain medications and report greater comfort during recovery.
Decreased blood loss and no need for blood transfusion
Because the incisions are smaller and no major bones are cut, surgical bleeding is minimised. This also makes surgery safer for patients who have bleeding risks. Reduced blood loss often eliminates the need for transfusions, lowering the risk of transfusion-related reactions and infections. It is helpful for patients who prefer to avoid transfusions.
Minimal scarring
Small incisions (often only a few centimetres long) result in tiny, less noticeable scars compared to the long midline scar from a traditional sternotomy.
Shorter hospital stay
Faster healing, fewer complications, and reduced pain allow patients to leave the hospital sooner—sometimes within a few days—compared to a week or more with open-heart surgery.
Lower risk of complications
Preserving the sternum lowers the risk of mediastinitis, dehiscence, and deep sternal wound infection. This is especially advantageous for high-risk individuals like those with diabetes, obesity, osteoporosis, or chronic lung disease.
Get a Free Second Opinion for Minimally Invasive Cardiac Surgery
At PACE Hospitals, we are committed to providing our patients with the best possible care, and that includes offering second medical opinions with super specialists for treatment or surgery. We recommend everyone to get an expert advance medical second opinion, before taking decision for your treatment or surgery.
Minimally Invasive Cardiac Surgery Steps
It includes the following steps:
Before minimally invasive cardiac surgery
- Before MICS, patients undergo a comprehensive pre-operative evaluation to ensure the heart, lungs, and overall body condition are safe for surgery. Surgeons evaluate patients' medical history, existing heart conditions, previous surgeries, and risk factors.
- The surgical team suggest a set of diagnostic tests be performed, which includes blood tests, electrocardiogram (ECG), chest X-ray, echocardiography, and, sometimes, computed tomography (CT) angiography, to determine chest anatomy. These tests help detect any structural challenges that could affect port placement or surgical access.
- Medication management is also optimised. Blood thinners, diabetes medications, and certain heart medications may need adjustment to reduce bleeding risk and maintain stable heart function. Smoking cessation is strongly advised several weeks before surgery to minimise respiratory problems.
- Patients are counselled on the procedure, risks, benefits, and expectations for recovery. They are instructed to maintain good nutrition, prevent infections, and follow fasting restrictions the night before the surgery. This careful pre-operative preparation increases surgical safety, minimises complications, and enhances postoperative recovery.
During Minimally Invasive Cardiac Surgery (MICS)
Anaesthesia and monitoring
This procedure is performed under general anaesthesia, with endotracheal intubation and controlled mechanical ventilation. A transesophageal echocardiogram (TEE) is inserted to guide the surgery and monitor heart function throughout the procedure.
Patient positioning and incision
The patient is placed in a supine position, sometimes with the right chest slightly elevated. A mini-thoracotomy (4–6 cm) or small keyhole ports are created, depending on the procedure. CO₂ is insufflated to reduce the risk of air embolism.
Cannulation and cardiopulmonary bypass (CPB)
In this surgery, circulation is often supported through peripheral cannulation, most commonly involving the femoral artery and vein. Once the extracorporeal circuit is functioning, the surgeon uses cardioplegia to arrest cardiac activity, which creates a motionless, blood-depleted environment that facilitates targeted intracardiac repair.
Surgical technique
The choice of technique depends on the cardiac condition. For cardiac surgeries, such as mitral valve repair or replacement, atrial septal defect closure, minimally invasive coronary bypass, or tricuspid valve surgery, surgeons use small thoracic access points, long-shafted instruments, and endoscopic visualization. Through these small incisions, the surgeon repairs or replaces the mitral valve, and atrial septal defects can be closed with suturing or patching techniques. Coronary grafting can be done using the left internal mammary artery (LIMA) to revascularize the LAD on a beating heart, and tricuspid valve pathology can be addressed through focused right-sided access.
Intraoperative care and haemostasis
This step focuses on careful haemostasis and precise repair using absorbable materials. It requires constant attention to avoid kind of injury to nearby nerves and vessels. The team reassesses transesophageal echocardiography (TEE) to confirm proper valve function, check patch integrity, and ensure there are no remaining defects.
Weaning from cardiopulmonary bypass and closure
After the repair is completed, the heart gradually returns to normal function. The patient is smoothly taken off cardiopulmonary bypass, with TEE used to confirm that the cardiac function is satisfactory, the valves are moving properly, and there is no residual air. The small incisions are then closed, chest drains are placed, and the patient is transferred to the cardiac intensive care unit (ICU) for further monitoring.
After minimally invasive cardiac surgery
Recovery room monitoring
Patients are observed for vital signs stability, bleeding, and pain control in the post-anaesthesia care unit. The breathing tube remains in place initially and is removed once the patient is stable and breathing adequately on their own.
Pain management and respiratory care
Pain is usually less than that of open-heart surgery, and can be managed with IV or oral medicines. Breathing exercises, incentive spirometry, and early chest physiotherapy all help to prevent lung infections and improve expansion.
Chest tube and wound care
Chest drains remove excess fluid or air from the heart and lungs and are normally removed within 24 to 48 hours. Surgical sites are examined daily for bleeding, redness, and infection. The dressings are kept clean and dry.
Early mobilisation
Patients are encouraged to sit, stand, and walk within 24 hours. Early movement reduces the risk of blood clot formation, improves lung functioning, and speeds recovery.
Medication management
The doctor prescribes postoperative drugs that may include anticoagulants, antiplatelets, beta-blockers, diuretics, and pain relievers. Medication adjustments are done based on heart rhythm, blood pressure, fluid balance, and valve type (if valve surgery was done).
Hospital stay duration
Most patients stay 3–5 days, shorter than traditional open-heart surgery, because there is no sternotomy to heal.
Follow-ups
Patients were advised that follow-up is usually scheduled within 1–2 weeks after discharge to assess wound healing, heart rhythm, medications, and rehabilitation progress. Sutures or staples may be removed during this visit.
Complications of Minimally Invasive Cardiac Surgery
Minimally invasive cardiac surgery generally has a lower rate of complications than traditional open-heart surgery. However, it still carries inherent risks common to all surgeries and some specific to the technique. Below are the common MICS complications:
- Bleeding and need for re-exploration
- Conversion to full sternotomy
- Wound complications and infection
- Stroke
- Renal (kidney) dysfunction
- Respiratory complications
- Valve-related complications
Bleeding and need for re-exploration
Bleeding can still occur in MICS because even though the cuts are small, the surgery is performed on major blood vessels and the heart. Small thoracotomy wounds may hide internal bleeding, and sometimes a blood vessel or stitch may leak. If bleeding does not stop on its own or causes a drop in blood pressure, the surgeon may need to return to the operating room to control it.
Conversion to full sternotomy
During MICS, the chest is not fully opened, which limits visibility and access. If the surgeon experiences uncontrolled bleeding, unexpected anatomy, or technical difficulty, they may switch to an open sternotomy to protect the patient and finish the surgery safely.
Wound complications and infection
Wound infections can occur even in less invasive incisions, generally in patients with risk factors such as obesity.
Stroke
It can occur due to embolism or hypoperfusion during surgery and is a serious postoperative risk with potential for long-term disability.
Renal (kidney) dysfunction
The patient may develop kidney problems after MICS due to temporary low blood pressure, inflammation from the heart–lung bypass machine, or reduced blood flow during surgery. Patients with diabetes, older age, or pre-existing kidney disease are more at risk.
Respiratory complications
This surgery requires working through the side of the chest, sometimes using one-lung ventilation. This can temporarily reduce lung capacity and lead to problems such as prolonged mechanical ventilation, re-expansion pulmonary edema (a rare complication of MICS), atelectasis (lung collapse), pneumonia, or breathing difficulty, especially in older adults or smokers.
Valve-related complications
In valve surgeries done minimally invasively, complications can include arrhythmias, heart block, and valve malfunction, which sometimes necessitate further interventions.
Minimally Invasive Cardiac Surgery Recovery Time
Minimally invasive cardiac surgery generally offers a much shorter recovery time than open-heart surgery. Individuals often recover in 2 to 4 weeks after MICS, compared to 6 to 12 weeks after open-heart surgery. Hospital stays are shorter, lasting 2 to 5 days for MICS. Patients usually start cardiac rehabilitation within 1 to 2 weeks after surgery to safely regain heart fitness and overall strength. Most people can return to routine activities, including work and exercise, within 2-4 weeks, although heavy lifting is avoided for several weeks longer. Recovery speed varies based on individual factors such as age, pre-operative health, and adherence to rehabilitation plans.
What questions can patients ask the healthcare team about minimally invasive cardiac surgery?
- What type of minimally invasive approach will be used (mini-thoracotomy, mini-sternotomy, robotic)?
- Am I a suitable candidate for minimally invasive cardiac surgery?
- What are the benefits of this approach compared with open-heart surgery?
- What is the success rate of this procedure?
- How long is the hospital stay after MICS?
- Will I need cardiac rehabilitation?
- How much postoperative pain should I expect?
- What precautions should I follow after surgery?
- Will I need to continue the same heart medications after surgery?
- What signs or symptoms after discharge should make me seek urgent care?
Difference between minimally invasive cardiac surgery and open-heart surgery
Minimally invasive cardiac surgery vs Open-heart surgery
| Parameters | Minimally invasive cardiac surgery (MICS) | Open-heart surgery |
|---|---|---|
| Definition | Surgery is performed via small chest incisions using specialised tools to reduce trauma and speed recovery. | Surgery is performed via a large incision down the chest, cutting through the sternum to expose the heart entirely. |
| Incision size | Small incisions (usually <4 inches), often between ribs | Large incision through the sternum (breastbone) |
| Surgical access | Limited, using specialised or robotic instruments | Full direct access through sternotomy |
| Use of the heart-lung machine | Usually required (peripheral cannulation via the femoral vessels); off-pump CABG is possible in select cases. The heart often stopped with cardioplegia. | Usually required (central cannulation); the heart stopped for most procedures. |
| Recovery time | Faster recovery, shorter hospital stay | Longer recovery, longer hospital stay |
| Risk of Infection | Lower risk due to smaller wounds | Higher risk due to a larger wound |
Minimally Invasive Cardiac Surgery (MICS) Cost in Hyderabad, India
The
cost of Minimally Invasive Cardiac Surgery (MICS) in Hyderabad generally ranges from ₹2,50,000 to ₹5,20,000 (approx. US $3,010 – US $6,265).
The exact cost of Minimally Invasive Cardiac Surgery (MICS) varies depending on factors such as the type of heart condition treated (valve repair or replacement, ASD closure, or CABG), the minimally invasive or thoracoscopic surgery approach used (mini-thoracotomy, mini-sternotomy, thoracoscopic, or keyhole techniques), the use of advanced surgical instruments, the patient’s risk profile, surgeon expertise, ICU and postoperative care requirements, and the hospital facilities chosen including cashless treatment options, TPA corporate tie-ups, and assistance with medical insurance wherever applicable.
Cost Breakdown According to Type of Minimally Invasive Cardiac Surgery
- Minimally Invasive Mitral Valve Repair / Replacement – ₹2,80,000 – ₹4,80,000 (US $3,375 – US $5,780)
- Transcatheter Aortic Valve Replacement (TAVR) – ₹3,00,000 – ₹5,20,000 (US $3,615 – US $6,265)
- Minimally Invasive Direct Coronary Artery Bypass (MIDCAB / Keyhole Bypass) – ₹2,70,000 – ₹4,60,000 (US $3,255 – US $5,540)
- Minimally Invasive ASD / VSD Closure – ₹2,50,000 – ₹3,90,000 (US $3,010 – US $4,700)
- Redo Cardiac Surgery Using Minimally Invasive Approach –
₹3,40,000 – ₹5,20,000 (US $4,090 – US $6,265)
Frequently Asked Questions (FAQs) on Minimally Invasive Cardiac Surgery (MICS)
Is MICS surgery safe?
MICS is generally safe when performed by experienced surgeons, with low rates of complications such as excessive bleeding or stroke. Its advantages include reduced trauma and faster recovery compared to traditional heart surgery. Studies report good short- and long-term outcomes, including low mortality and complication rates, which make MICS a safe surgery.
What is the difference between MICS and CABG?
The difference between MICS and coronary artery bypass grafting (CABG) lies mainly in the surgical approach. MICS uses small incisions without splitting the breastbone, whereas CABG involves a large chest incision to access the heart.
Which Is the best hospital for Minimally Invasive Cardiac Surgery (MICS) in Hyderabad, India?
PACE Hospitals, Hyderabad, is a trusted centre for advanced minimally invasive heart surgeries, offering patient-focused cardiac care with reduced surgical trauma and faster recovery.
We have highly talented and experienced cardiac surgeons, cardiologists, anesthesiologists, and perfusion teams specialise in performing complex heart procedures through small incisions using precision-guided techniques, ensuring minimal blood loss, lower infection risk, reduced post-operative pain, and shorter hospital stays.
We deal complicated cases and have successful outcomes with state-of-the-art cardiac operation theatres, advanced imaging guidance, modern heart-lung machines, dedicated cardiac ICUs, in-house diagnostics, and structured cardiac rehabilitation programs, PACE Hospitals delivers safe, effective, and high-quality MICS procedures — supported by cashless insurance facilities, TPA corporate tie-ups, and seamless documentation support.
What is the success rate of MICS?
Studies show that minimally invasive cardiac surgery has a high success rate, above 90–95% for common procedures such as valve repair, valve replacement, and selected bypass surgeries. Studies indicate low complication rates, excellent long-term outcomes, and faster recovery time when compared to traditional open-heart surgery. Success depends on the patient’s health, the type of surgery required, and the experience of the surgical team, but overall outcomes are consistently strong.
What are the alternatives to CABG surgery?
Alternatives to CABG include medications to manage symptoms and prevent progression, angioplasty and stenting (a less invasive surgery to open blocked arteries using a balloon and metal scaffolding), and lifestyle changes to control risk factors. The choice depends on the extent of artery blockage, patient health, and specific heart conditions.
What Is the cost of Minimally Invasive Cardiac Surgery (MICS) at PACE Hospitals, Hyderabad?
At PACE Hospitals, Hyderabad, the cost of Minimally Invasive Cardiac Surgery (MICS) typically ranges from
₹2,40,000 to ₹4,90,000 and above (approx. US $2,890 – US $5,900), making it a cost-effective option for advanced cardiac care compared to many premium cardiac centres in Hyderabad. However, the final cost depends on:
- Type of cardiac condition and procedure performed
- Surgical approach and complexity
- Valve type or grafting requirement (if applicable)
- Patient’s overall health and associated medical conditions
- Surgeon expertise and technology used
- Duration of ICU and hospital stay
- Anesthesia, perfusion, and monitoring needs
- Diagnostic tests (echocardiography, CT scan, angiography)
- Medications, consumables, and rehabilitation support
For standard minimally invasive valve or bypass procedures, costs remain toward the lower end of the range, while complex redo or multi-procedure surgeries fall toward the higher side.
After a thorough cardiac evaluation, imaging review, and surgical planning, our specialists provide a personalised treatment plan and transparent cost estimate, tailored to your heart condition, recovery expectations, and financial
Which surgery is better, MICS or open-heart surgery?
No surgery is universally better; the choice depends on the patient's heart condition, overall health, and the surgeon's skill. MICS can lead to faster recovery, less pain, and shorter hospital stays due to smaller cuts, making it suitable for simpler cases. Open-heart surgery, provides better access for complex conditions, ensuring comprehensive therapy but causing more tissue damage and taking longer to heal.
What are the risks of MICS?
Risks of minimally invasive heart surgery are similar to open-heart surgery and include bleeding, infection at cut sites, irregular heartbeats, heart attack, stroke, or, rarely, death. Small incisions can lead to blood clots or lung fluid buildup on one side. In some cases, about 1-5% may convert to open surgery if issues arise during the operation.
What is a minimally invasive heart surgery?
MICS is a type of heart surgery performed via small incisions rather than the large cut used in traditional open-heart surgery. This approach includes procedures such as coronary artery bypass, valve repair or replacement, and congenital defect correction. Benefits generally include reduced blood loss, less pain, a quick recovery, and a lower risk of infection.
What conditions does MICS treat?
MICS is used to treat many heart problems that traditionally required open-heart surgery. It is effective in managing valve diseases (mitral, aortic, and tricuspid), coronary artery disease in selected patients, atrial septal defects, certain arrhythmias, and tumors inside the heart. It is also used for repairing or replacing damaged heart structures.
What are the disadvantages of minimally invasive heart surgery?
MICS procedures may take longer due to small cuts, which limit visibility and tool access, increasing the risk of needing to switch to open surgery. It requires highly trained surgeons and specialised instruments, which may not be available everywhere and may raise treatment costs. Not all patients qualify, particularly those with abnormal heart shapes, weak heart muscle, or prior chest infections.
Does MICS use a heart-lung machine?
Most MICS do use a heart-lung machine, especially for valve repair, valve replacement, and certain congenital heart procedures. Many studies show that using the machine allows the surgeon to work on a still, blood-free heart through small incisions, which improves precision and safety. However, some minimally invasive cardiac bypass surgeries can be performed without the machine. The decision depends on the patient’s heart condition and the type of surgery planned.
What is the size of the incision in MICS?
The incision size in MICS is generally small, about 3-4 inches (approximately 7-10 cm) for partial sternotomy or mini-thoracotomy. For mitral valve surgery, about 7 cm long incision is done on the right side of the chest is used. These incisions avoid cutting through the breastbone and result in less trauma and quicker healing compared to traditional open surgery.
Can elderly patients undergo minimally invasive cardiac surgery?
Yes, elderly individuals can undergo this surgery; but, the eligibility is determined by the patient's overall health, disease severity, and surgical risk evaluation.MICS may benefit elderly patients by reducing trauma and speeding recovery, but careful evaluation is important to ensure safety.
How long is the hospital stay after minimally invasive cardiac surgery (MICS)?
Most patients need to stay in the hospital for 3-5 days after minimally invasive cardiac surgery. The stay is often shorter than traditional open-heart surgery because smaller incisions lead to quicker mobility, better breathing comfort, and fewer complications.
Can a mitral valve be replaced without open-heart surgery?
Yes, mitral valve replacement or repair can be performed using minimally invasive procedures rather than complete open-heart surgery. Surgeons use advanced instruments and cardiopulmonary bypass support to access the valve through small incisions (such as a mini-thoracotomy), avoiding large chest cuts.
What is life expectancy after MICS?
Life expectancy after the surgery is generally comparable to that of open-heart surgery, according to many studies. Long-term survival mainly depends on the previous heart disease, overall health, age, and how well the heart responds after treatment, not on the incision size.
Why choose PACE Hospitals?
- A Multi-Super Speciality Hospital.
- NABH, NABL, NBE & NABH - Nursing Excellence accreditation.
- State-of-the-art Liver and Kidney transplant centre.
- Empanelled with all TPAs for smooth cashless benefits.
- Centralized HIMS (Hospital Information System).
- Computerized health records available via website.
- Minimum waiting time for Inpatient and Outpatient.
- Round-the-clock guidance from highly qualified super specialist doctors, surgeons and physicians.
- Standardization of ethical medical care.
- 24X7 Outpatient & Inpatient Pharmacy Services.
- State-of-the-art operation theaters.
- Intensive Care Units (Surgical and Medical) with ISO-9001 accreditation.