Arthroscopy Assisted Fixations for Bone Fractures and Fractures Around Joints
PACE Hospitals
Understanding Fractures around Joints
Fractures around joints, also known as peri-articular fractures, involve the bone surfaces that contribute to joint movement. These fractures are more complex than mid-shaft fractures because they affect not only the bone but also cartilage, ligaments, and surrounding soft tissues. Commonly affected joints include the knee, ankle, shoulder, elbow, and wrist.
In such injuries, restoring the joint surface accurately is critical. Even a small step or gap in the joint surface can alter load distribution, increasing the risk of pain, reduced range of motion, and post-traumatic arthritis. Traditional open surgical methods, while effective, may involve extensive soft-tissue dissection, which can delay recovery and increase stiffness.
With changing protocols and trends in medicine we at pace hospitals want to give our best possible treatment protocols. There are many modalities of fixing bone fractures. Especially periarticular fractures (fractures around joints) should be fixed with utmost care. With state-of-the-art equipment and well trained Orthopaedic team we aim at perfect fixation of periarticular fractures. At pace hospitals we are now focusing at arthroscopic assisted fixation of all periarticular fractures at affordable prices.
We present to you a few scenarios:
- Young male of age 34 years going to work on his scooter meets with an accident and fells over his right knee. This has caused a valgus knee injury thus causing proximal tibia fracture. he was evaluated in detail and we have managed him with dual plating for proximal tibia with arthroscopy assisted reduction of tibiofemoral joint.
- Young male software employee falls over stairs and supports his weight by his arm. he sustained and distal radius comminuted intra articular fracture. We did three column fixations of distal radius with arthroscopic assisted reduction of radiocarpal joint.
- Earlier surgeons depend on only intraoperative radiographs for viewing joint congruency but with
arthroscopy now surgeons have an option of viewing real time image of articular surface directly and correct articular malreduction.
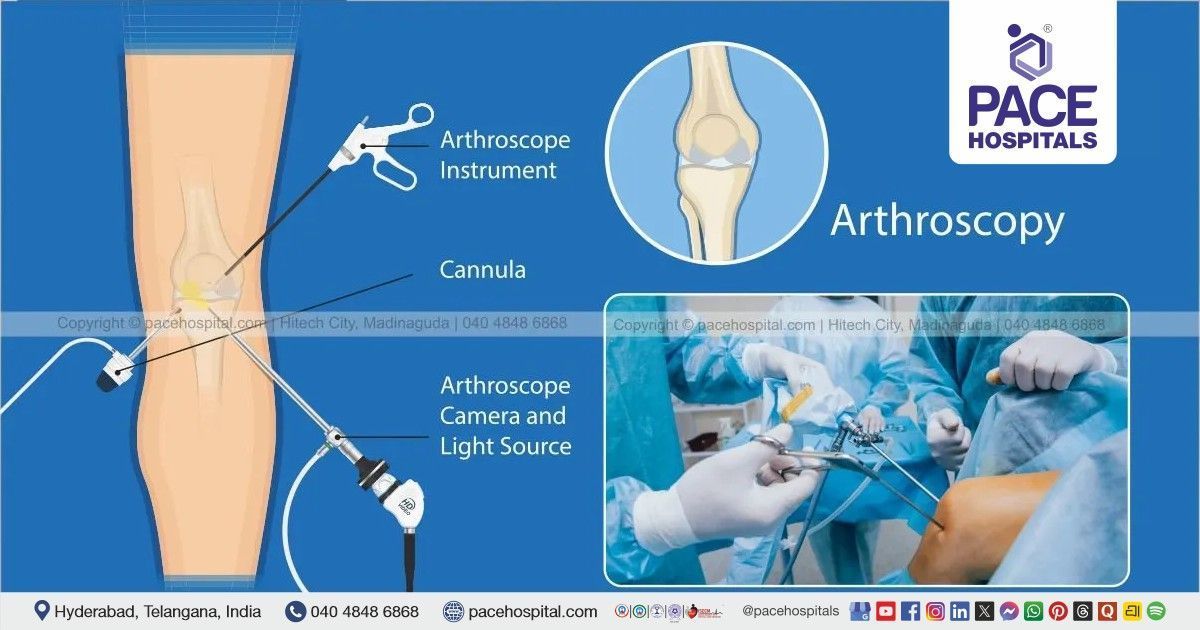
What Is Arthroscopy-Assisted Fixation?
Arthroscopy-assisted fixation combines minimally invasive joint visualization and internal fracture fixation. Arthroscopy uses a small camera inserted through tiny incisions to provide a clear, magnified view of the joint interior. This allows the surgeon to directly visualize cartilage surfaces, fracture lines, and associated soft-tissue injuries during the procedure.
By combining arthroscopy with fracture repair procedures such as screws or plates, surgeons can accurately reduce joint fragments while conserving surrounding tissues. This technique bridges the gap between traditional open surgery and minimally invasive treatment.
Why Arthroscopy Plays a Crucial Role in Fracture Management
One of the major advantages of arthroscopy is direct visualization. Conventional imaging methods, such as X-rays and CT scans, provide valuable preoperative information, but they cannot replace real-time visualization of the joint during surgery. Arthroscopy allows orthopedic surgeons to confirm that the joint surface is properly aligned before final fixation.
In addition, arthroscopy enables identification of associated injuries that may otherwise go unnoticed. Cartilage damage, meniscal tears, or ligament injuries frequently accompany joint fractures. Addressing these injuries in the same surgical session enhances total joint stability and long-term results.
Common Fractures Treated Using Arthroscopy Assistance
Arthroscopy-assisted fixation is particularly useful in selected fracture patterns where joint involvement is significant. Common examples include:
- Ankle fractures involving the articular surface, especially those affecting stability
- Tibial plateau fractures, where joint surface restoration is essential for knee function
- Distal femur fractures extending into the knee joint
- Shoulder fractures involving the glenoid or humeral head
- Elbow and wrist fractures where cartilage integrity and alignment are critical
Not all fractures require arthroscopy assistance. However, Patient factors, fracture complexity, and surgeon expertise guide the decision-making process.
Preoperative Evaluation and Surgical Planning
Successful arthroscopy-assisted fixation begins with careful evaluation. Detailed history, physical examination, and imaging studies are essential. CT scans are often used to understand fracture geometry and joint involvement in greater detail for individual patients.
At PACE Hospitals, surgical planning emphasizes choosing the least invasive approach that still allows accurate reduction and stable fixation. Arthroscopy is considered when joint visualization is likely to improve precision or when associated soft-tissue injuries are suspected.
How the Procedure Is Performed?
The procedure usually begins with an arthroscopic inspection of the joint through tiny portals. This allows the surgeon to assess fracture displacement, cartilage condition, and any associated injuries. Fracture pieces are then minimized by direct visualization.
Once alignment is adequate, internal fixation is carried out using the proper hardware. Arthroscopy is used again to confirm joint congruity before completing the procedure. This step-by-step procedure ensures proper healing while reducing needless tissue irritation and significant harm to joint structure.
Advantages of Arthroscopic Assisted Fixations
- Supervised reduction and fixation of intraarticular fractures
- Simultaneous repair of ligament injuries
- Decreased chances of arthritis
- Long term good functional outcome and full range of movements
Benefits of Arthroscopy-Assisted Fixation
Arthroscopy-assisted fixation offers several advantages over conventional open methods. Smaller incisions reduce soft-tissue trauma, postoperative pain, and scarring. Improved visualization allows precise joint surface restoration, which is critical for long-term function.
Patients frequently have less postoperative stiffness and can begin rehabilitation sooner. Preserving the surrounding tissues also promotes faster recovery and better mobility, particularly in active people.
Comparison with Traditional Open Fixation
Traditional open fixation remains a significant treatment option for many fractures, particularly when considerable exposure is necessary. However, open procedures may result in larger incisions and greater muscle and soft tissue disruption.
Arthroscopy-assisted fixation complements open techniques by reducing surgical trauma in selected cases. The choice between methods depends on fracture pattern, joint involvement, and patient-specific factors. At PACE Hospitals, the goal is always to choose the approach that best supports recovery and long-term joint health.
Detecting and Treating Associated Joint Injuries
Joint fractures rarely occur in isolation. Ligament injuries, cartilage damage, and meniscal tears are common. Arthroscopy provides an opportunity to identify and address these injuries during the same procedure.
Treating associated injuries early improves joint stability and reduces the risk of persistent pain or functional limitation. This integrated approach is a key advantage of arthroscopy-assisted techniques.
Postoperative Recovery and Rehabilitation
Recovery following arthroscopy-assisted fixation depends on the joint involved and fracture severity. In most cases it takes around 1 week to several months for complete recovery. Early controlled movement is often encouraged to prevent stiffness, while weight-bearing is guided based on fracture stability.
Physiotherapy plays a central role in rehabilitation. Gradual strengthening, range-of-motion exercises, and functional training help restore normal movement patterns. Rehabilitation programs at PACE Hospitals are tailored to each patient's specific needs and continuously monitored.
Risks Associated with Periarticular Fractures (Fracture around Joints)
- Stiffness.
- Articular steps leading to arthritis.
- May be associated with ligament injuries.
As with any surgical procedure, arthroscopy-assisted fixation carries some risks, including infection, stiffness, or incomplete fracture healing. Technical challenges may arise in cases related with complex fractures, emphasizing the importance of orthopedic surgeon expertise.
Not all fractures are suitable for arthroscopy assistance. In certain cases, traditional open fixation provides better access and stability. Proper patient selection is therefore essential.
Long-Term Outcomes and Joint Health
When done correctly, arthroscopy-assisted fixation provides excellent functional results. Accurate joint surface healing lowers the likelihood of post-traumatic arthritis and persistent pain.
Regular follow-up ensures optimal healing and the early detection of any problems. Long-term success is based on both surgical precision and patient adherence to rehabilitation regimens recommended by healthcare experts.
Orthopaedic Expertise at PACE Hospitals
PACE Hospitals offers advanced orthopaedic care supported by experienced sports medicine specialists and advanced surgical facilities all performed under guidance of highly experienced orthopedic surgeons. Arthroscopy-assisted fracture fixation is part of a broader commitment to minimally invasive, patient-focused care.
The orthopaedic team works closely with skilled physiotherapists and rehabilitation specialists to ensure quick and seamless recovery. The emphasis is on maintaining joint function, limiting problems, and guiding patients through each stage of treatment.
When to Seek Orthopaedic Consultation?
Prompt orthopaedic evaluation is recommended after joint injuries accompanied by swelling, pain, instability, or reduced movement. Early diagnosis and appropriate, timely management are important in orthopedics, particularly for joint-related fractures, as they significantly improve patient outcomes, reduce complications, and significantly improve outcomes, particularly in joint-related fractures.
Delaying treatment may give rise to stiffness, misalignment, or long-term joint damage. Early consultation helps determine whether arthroscopy-assisted fixation or another approach is most suitable.
Frequently Asked Questions on Arthroscopy-Assisted Fixation for Bone Fractures
What is arthroscopy-assisted fixation in fracture management?
Arthroscopy-assisted fixation is a surgical technique where a small camera (arthroscope) is used to visualize the joint while fixing fractures that involve or lie close to joint surfaces. This method enables surgeons to examine the fracture directly within the joint and restore alignment with better precision.
How does arthroscopy improve fracture fixation compared to open surgery?
Arthroscopy provides a magnified, real-time view of the joint interior. This helps orthopedic surgeons assess fracture reduction precisely, identify hidden cartilage or ligament injuries, and avoid extensive soft-tissue dissection required in open procedures.
Which types of fractures are commonly treated with arthroscopy assistance?
Arthroscopy is often useful in fractures involving the knee, ankle, shoulder, elbow, and wrist—especially when the fracture extends into the joint. It is commonly used in tibial plateau fractures, ankle joint fractures, and selected shoulder or elbow injuries.
What are the advantages of arthroscopy-assisted fixation?
This approach often results in smaller incisions, reduced soft-tissue damage, better joint alignment, and lower risk of postoperative stiffness. Patients may benefit from quicker rehabilitation and improved joint movement when compared to traditional open techniques.
Does arthroscopy reduce the risk of post-traumatic arthritis?
Accurate joint surface restoration is key to reducing long-term arthritis risk. Arthroscopy helps ensure that joint congruity is achieved, which may lower the chances of uneven wear and degeneration over time.
Is arthroscopy-assisted fixation suitable for all fractures?
No. The technique is best suited for selected fractures involving joints. Fracture pattern, bone quality, soft-tissue condition, and patient factors all influence suitability. An orthopaedic specialist determines the best approach after evaluation.
Are there risks associated with arthroscopy-assisted fixation?
As with any surgery, risks such as infection, bleeding, or stiffness exist. However, when performed by experienced surgeons, arthroscopy-assisted fixation is generally safe and well-tolerated.
When should a patient seek orthopaedic evaluation after joint injury?
Persistent pain, swelling, reduced movement, joint instability, or inability to bear weight after injury should prompt early orthopaedic consultation. Timely evaluation improves treatment options and outcomes.
Why are fractures around joints considered more complex?
Fractures near joints affect not only the bone but also cartilage, ligaments, and joint alignment. Even modest anomalies can eventually result in stiffness, discomfort, or arthritis. Accurate restoration of the joint surface is therefore essential for long-term function.
Can associated joint injuries be treated during the same procedure?
Yes. Arthroscopy allows surgeons to identify and manage associated injuries such as cartilage damage, meniscal tears, or ligament injuries during the same surgery. Early treatment of these issues can help with joint stability and rehabilitation.
What role does imaging play before surgery?
X-rays and CT scans aid to determine fracture anatomy and joint involvement. These imaging investigations help surgeons plan their procedures and assess whether arthroscopy is necessary.
How long does recovery take after arthroscopy-assisted fixation?
Recovery times vary based on the fracture type and joint involved. Early mobility is frequently promoted with coaching, followed by formal physiotherapy. Full recovery may take weeks to months, depending on healing and rehabilitation progress.
Is physiotherapy important after the procedure?
Yes. Physiotherapy plays a critical role in restoring joint movement, strength, and stability. Early guided rehabilitation helps prevent stiffness and supports functional recovery.
How does PACE Hospitals approach arthroscopy-assisted fracture care?
At PACE Hospitals, arthroscopy-assisted fixation is integrated into a comprehensive orthopaedic care pathway that includes precise diagnosis, based upon minimally invasive procedures, and structured rehabilitation planning with proper treatment plan.
What facilities support arthroscopy-assisted fracture treatment at PACE Hospitals?
PACE Hospitals offers advanced arthroscopy equipment, high-resolution imaging, and multidisciplinary orthopaedic expertise to manage complex joint fractures effectively with better outcomes.
How is patient recovery monitored after surgery at PACE Hospitals?
Recovery is monitored with scheduled check-ups, imaging as appropriate, and coordinated physiotherapy. The primary target is to improve joint function while avoiding long-term complications.
Why is early intervention important in joint-related fractures?
Early and accurate treatment helps preserve joint surfaces, prevent stiffness, and lower the risk of chronic pain or arthritis in individuals. Arthroscopy-assisted procedures help achieve this goal by increasing surgical precision.
What is the overall goal of arthroscopy-assisted fracture fixation?
The ultimate goal of arthroscopy-assisted fracture fixation is to accomplish precise anatomic reduction and stable internal fixation of intra-articular fractures while reducing soft tissue trauma, allowing for early mobilization and lowering the risk of long-term joint deterioration.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868