Anorectal Manometry Test | Procedure and Cost
At PACE Hospitals, Hyderabad, the Anorectal Manometry Test, also known as anal manometry, is performed by experienced gastroenterologists and colorectal specialists to evaluate rectal and anal sphincter muscle function. This advanced Anorectal Manometry procedure helps diagnose conditions such as chronic constipation and fecal incontinence. Our specialists conduct the anorectal manometry test using advanced diagnostic technology to ensure accurate results and effective treatment planning.
Book Appointment for a Anorectal Manometry
Anorectal Manometry Test Appointment
Why Choose PACE Hospitals for Anal Manometry Test?
State-of-the-Art Anorectal Diagnostic Suites Equipped with High-Resolution Anorectal Manometry & Pelvic Floor Pressure Systems
Expert Gastroenterologists & Colorectal Surgeons Specializing in Accurate Anorectal Manometry Testing
Non-Invasive Anorectal Manometry Test with Precise Measurement of Rectal Pressure, Anal Sphincter Function & Pelvic Floor Coordination
Affordable Anorectal Manometry Testing with Insurance Support & Cashless Options
Recognized for excellence in healthcare delivery with
NABH, NABL, NBE/DNB, NABH Nursing Excellence, and ISCCM accreditations.
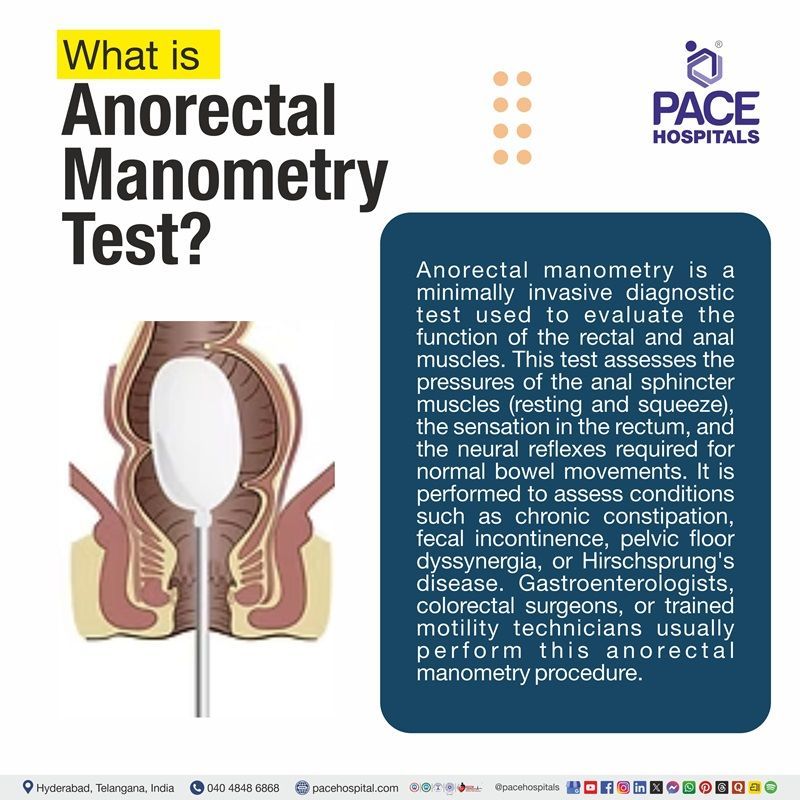
What is Anorectal Manometry Test?
Anorectal manometry is a minimally invasive diagnostic test used to evaluate the function of the rectal and anal muscles. This test assesses the pressures of the anal sphincter muscles (resting and squeeze), the sensation in the rectum, and the neural reflexes required for normal bowel movements.
It is performed to assess conditions such as chronic
constipation, fecal incontinence, pelvic floor dyssynergia, or Hirschsprung's disease.
Gastroenterologists,
colorectal surgeons, or trained motility technicians usually perform this anorectal manometry procedure. This low-risk, painless test helps guide treatments like surgery or biofeedback therapy.
Types of Anorectal Manometry
The classification of anorectal manometry tests is based on their technical resolution and measurement capabilities; improvements have improved the diagnostic precision and spatial detail. Below are the main types:
- Conventional (Non-High Resolution) Manometry
- High-Resolution Anorectal Manometry (HR-ARM)
- High-Definition/3D Anorectal Manometry (HD/3D-ARM)
Conventional (Non-High Resolution) Manometry
Fewer sensors are used to assess rectal sensation, rectoanal inhibitory reflex, and basic anal sphincter pressures. Although this approach has limits in topographic mapping, it is suitable for routine evaluations.
High-Resolution Anorectal Manometry (HR-ARM)
It improves the visualisation of coordination and dyssynergia patterns by using sensors that are ≤1 cm apart to provide detailed pressure profiles along the anorectum.
High-Definition/3D Anorectal Manometry (HD/3D-ARM)
It is suitable for complex motility disorder study, it has 12–16 radial sensors per recording site for 360° circumferential pressure mapping in three dimensions.

Anorectal Manometry Indications
To guide diagnosis and treatment, anorectal manometry assesses anorectal function in a variety of illnesses. Important clinical indications include:
- Fecal incontinence
- Functional Anorectal Pain
- Chronic Constipation and Defecatory Disorders
- Preoperative Assessment
- Hirschsprung's Disease
- Other Indications
Fecal incontinence
Involuntary stool leakage is known as faecal incontinence, and it is frequently caused by nerve injury or sphincter dysfunction. By detecting low resting or squeeze pressures, anorectal manometry can direct biofeedback or surgical procedures such as sacral nerve stimulation. It aids in separating irreversible damage from curable causes.
Functional Anorectal Pain
This comprises rectal hypersensitivity or raised sphincter tone associated with levator ani syndrome or proctalgia fugax. By measuring dyssynergia and hypercontractility, manometry enables focused biofeedback to ease tense muscles. It excludes fissures and other organic pathologies.
Chronic Constipation and Defecatory Disorders
Straining and persistent constipation are signs of dyssynergic defecation, a condition in which the pelvic floor muscles do not relax during evacuation. Over slow-transit problems, manometry confirms functional defecatory abnormalities by detecting paradoxical contraction or insufficient propulsion. Biofeedback therapy for coordination training is based on results.
Preoperative Assessment
It is performed to estimate the risk of postoperative incontinence prior to rectal prolapse repair, fistula surgery, lateral internal sphincterotomy (LIS), or low anterior resection (LAR).
Hirschsprung's Disease
Due to the lack of a rectoanal inhibitory reflex, a congenital aganglionosis is creating functional blockage. Particularly in newborns or older children, manometry helps confirm biopsy by confirming the absence of responsiveness despite feeling. Idiopathic constipation is not the same as this.
Other Indications
It is used to measure the level of damage following obstetric anal sphincter injury or to track biofeedback progress in cases of pelvic floor dyssynergia. Additionally, it assesses pruritus or rectal ulcer syndrome that is resistant to treatment. aids in difficult workups for motility disorders.

Anorectal Manometry Contraindications
Contraindications of anorectal manometry are fewer because of the test's low-risk profile, mainly focusing on anatomical risks or acute conditions. Below are some of the contraindications:
- Latex Allergy (for Balloon Use)
- Acute Anal/Rectal Pathology
- Recent Colorectal Surgery or Trauma
- Severe Rectal Prolapse or Stenosis
- Uncooperative Patients
Latex Allergy (for Balloon Use)
Allergy to latex balloons used for sensation testing: alternatives are available. Prior to the procedure, the patient's history must be reviewed.
Acute Anal/Rectal Pathology
The risk of pain, bleeding, or perforation is increased by active
fissures, abscesses, fistulas, or severe
haemorrhoids. Until the acute inflammation is treated medically or surgically, insertion is postponed. Accurate testing is ensured, and procedural complications are avoided with this precaution.
Recent Colorectal Surgery or Trauma
After an anal trauma, biopsy, or
polypectomy, testing should be avoided for four to six weeks. Healing time reduces the risk of infection, bleeding, or incorrect results from changed pressures. Recovery is confirmed by follow-up prior to elective manometry.
Severe Rectal Prolapse or Stenosis
Safe catheter advancement is limited by tight strictures or unreduced prolapse. The insertion attempts run the risk of causing mucosal damage or insufficient assessment. Management choices are guided by pre-procedure imaging.
Uncooperative Patients
Manoeuvres are invalidated by cognitive impairment, extreme anxiety, or small children who are unable to cooperate. Without the right squeeze or bearing-down efforts, results become unreliable. Case-by-case consideration may be given to sedation or streamlined processes.
Anorectal Manometry Advantages
Anorectal manometry improves diagnosis and treatment choices by providing objective information on anorectal pressures, sensation, and coordination. Below are some of the advantages of anorectal manometry:
- Non-Invasive and Safe
- Monitors Treatment Response
- Predicts Surgical Outcomes
- Guides Targeted Therapy
- Accurate Diagnosis of Disorders
Non-Invasive and Safe
It is an outpatient test with low rates of complications, excellent patient tolerance, and little discomfort. It allows regular usage in management.
Monitors Treatment Response
It repeats to evaluate the recovery of sphincter function following surgery or biofeedback progress. It gives measurable metrics for improvement.
Predicts Surgical Outcomes
Baselines are used to predict the probability of postoperative incontinence prior to rectal procedures such as low anterior resection. Aids in efficiently counselling patients or procedures.
Guides Targeted Therapy
It uses muscular coordination deficiencies to guide biofeedback training for incontinence or dyssynergic defecation. It also increases pelvic floor rehabilitation success rates.
Accurate Diagnosis of Disorders
It measures sphincter pressures and reflexes to provide the clear cause of dyssynergia, constipation, or faecal incontinence. It avoids unwanted testing by distinguishing between structural and functional concerns.
Anorectal Manometry Test Steps
Anorectal manometry test involves the following steps:
Before the test
- Two hours before starting the test, patients need to take one or two Fleet® enemas. The Fleet enema is available at pharmacies and supermarkets.
- Two hours before the procedure, patients should avoid eating anything. Adjusting the diabetic medication may be necessary if they have diabetes.
- At least two hours before the test, patients are allowed to take their usual medications with small sips of water.
During the test
- As directed by the technician or nurse performing the test, patients must undress from the waist down or change into a hospital gown. A technician will answer questions, take a quick medical history, and explain the entire procedure.
- Patients need to lie on their left side and bring their knees up into a fetal position.
- A gloved finger may be inserted into the anus to feel for abnormalities as part of a digital rectal exam before the technician begins the anorectal manometry test.
- The rectum is filled with a tiny, flexible, lubricated tube that resembles a thermometer and has a deflated balloon at the end. A pressure-measuring device is attached to the tube.
- The balloon will be positioned inside the rectum at different depths, and the technician will collect multiple benchmark pressure readings.
- After the balloon has reached a specific size, the technician will ask patient to squeeze, relax, push, or cough for short periods of time. These exercises are repeated using various balloon sizes or rectum locations. Every time, the pressures of the anal sphincter muscles are measured.
- Squeezing involves tightening the sphincter muscles as though attempting to stop something from escaping. The anal sphincter is also contracted when the patient coughs.
- The patient needs to bear down as if they were trying to make a bowel movement in order to push or strain.
- Additionally, the technician may ask the patient if the size of the balloon affects how their rectum feels. When they feel the desire to have a bowel movement, they have to say it.
- The technician removes and deflates the balloon after the test is complete.
After the test
- Following the examination, the patient is allowed to drive themselves home and can resume their regular activities.
- Patients do not need to recover from sedation and can immediately resume eating, medicine, and activities.
- Initial results are generated instantly; at follow-up, a thorough analysis and therapy discussion will take place.
Anal Manometry Test Results
- Gastroenterologists and colorectal surgeons can determine the cause of constipation or incontinence and develop a treatment plan based on test results.
- For example, the test may identify inadequate rectal feeling or weak anal sphincter muscles, both of which can lead to faecal incontinence. These issues are treatable. Strengthening the muscles and enhancing sensation can be achieved by biofeedback procedures that use anal manometry and specific pelvic floor exercises.
- Test findings may indicate that when patients push to make a bowel movement, the anal sphincter muscles may not relax properly, which can lead to constipation. Biofeedback techniques can be used to retrain these muscles as well.
Anorectal Manometry Interpretation
Abnormal findings guide diagnosis per the London Classification (tone, contractility, coordination, sensation).
- Low Resting Pressure (<40 mmHg): Internal sphincter weakness (incontinence, scleroderma).
- Low Squeeze Pressure (<100 mmHg): External sphincter neuropathy or injury (obstetric trauma).
- Absent RAIR: Hirschsprung's disease or aganglionosis.
- Dyssynergia (Types I-IV): Paradoxical contraction during evacuation; biofeedback indicated.
- Rectal Hyposensitivity (>50 mL first sensation): It contributes to constipation.
- Hypercontractility (>200 mmHg squeeze): Anismus or proctalgia fugax
Anorectal Manometry Normal Values
Normal ranges differ by system (HR-ARM preferred), age, and sex; pressures are higher in men.
- Resting Anal Pressure: It reflects internal sphincter tone and typically ranges from 40 to 80 mmHg, with a mean of roughly 65 mmHg.
- Maximal Squeeze Pressure: It usually indicates the strength of the external sphincter and ranges from 100 to 200 mmHg (mean 168 mmHg).
- Rectoanal Inhibitory Reflex (RAIR): Transient anal relaxation is caused by the rectoanal inhibitory reflex (RAIR), which is present at balloon volumes of 10–30 mL.
- First Sensation Volume: For initial rectal awareness, the first sensation volume is 10–40 mL, and the desire to defecate happens at 30-90 mL.
- Maximum Tolerated Volume: In order to evaluate rectal compliance, the maximum tolerated volume is 150–300 mL prior to pain.
Anorectal Manometry Complications
As anorectal manometry is a minimally invasive procedure, complications are uncommon, occurring in less than 1% of patients. Below are some of the complications of anorectal manometry:
- Pain or Minor Discomfort
- Vaginal or Uterine Perforation (Rare)
- Rectal Perforation (Very Rare)
- Bleeding
- Vasovagal Syncope
Pain or Minor Discomfort
When inserting a catheter or inflating a balloon, patients may experience brief anal pain or cramping. Without medical intervention, this discomfort usually goes away on its own.
Vaginal or Uterine Perforation (Rare)
Rarely, females may experience a perforation during the surgery due to catheter misplacement. In most situations, prompt detection enables conservative management.
Rectal Perforation (Very Rare)
This rare but serious consequence, which manifests as bleeding or pain, affects high-risk patients who have had past surgery or strictures. Antibiotics and bowel rest are frequently effective in stable patients.
Bleeding
Mucosal irritation, especially in people using blood thinners, causes little bleeding. In most cases, it resolves on its own after taking anticoagulants.
Vasovagal Syncope
During the test, discomfort or strain may cause brief lightheadedness or fainting. Rest and support help symptoms to go away rapidly.
Anorectal Manometry Recovery Time
Anorectal manometry is a 15–45-minute outpatient procedure that requires no anaesthesia or sedation, so patients recover right away and can return to their regular activities, diet, and medications.
Minor spotting from mucosal irritation, pressure sensation, or mild anal discomfort may last for a few hours or longer but usually goes away on its own without help; severe symptoms call for immediate medical attention.
In most situations, rare problems such as vasovagal syncope from straining or perforation (<1%) resolve on their own, and complete recovery is expected within hours.
What questions can patients ask the healthcare team about anorectal manometry?
- When will I get the results of my anorectal manometry test?
- What do the results of my anorectal manometry mean?
- When can I go back to my normal activities after anorectal manometry?
- How soon should I contact the healthcare team if I notice any unusual symptoms after the procedure?
- What signs of complications should I watch out for after anorectal manometry?
- Are there any specific activities I should avoid during recovery from anorectal manometry?
- Do I need any follow-up tests or appointments based on my anorectal manometry results?
Difference between defecography and anorectal manometry
Defecography vs anorectal manometry
Defecography images anatomic defects like rectocele/prolapse during simulated defecation via X-ray/MRI. Anorectal manometry measures functional sphincter pressures, sensation, and coordination via a catheter. Below are some of the parameters that help in differentiating defecography and anorectal manometry:
| Parameters | Defecography | Anorectal manometry |
|---|---|---|
| Purpose | It indicates anatomical abnormalities such as rectocele and prolapse, as well as dynamic defecation. | It measures the rectoanal inhibitory reflex, sensation, and sphincter pressures. |
| Method | Fluoroscopic/MR imaging with barium paste evacuation | Catheter sensors/balloon for maneuvers |
| Invasiveness | Higher cost, Radiation/contrast | Minimally invasive, no radiation |
| Primary Use | Structural disorders | Incontinence, Functional dyssynergia |
| Duration | 20-30 min | 15-45 min |
| Sedation | Usually none | None required |
Anorectal Manometry Test Cost in Hyderabad, India
The cost of an Anorectal Manometry Test in Hyderabad generally ranges from ₹4,000 to ₹12,000 (approximately US $50 – US $145).
The exact cost may vary based on several factors, such as the hospital infrastructure, technology used (high-resolution manometry systems), consultant expertise, need for additional tests (balloon expulsion test or EMG), and whether the procedure is done as part of a comprehensive gastrointestinal motility evaluation package.
Cost breakdown according to the type of anorectal manometry evaluation:
- Standard Anorectal Manometry – ₹4,000 – ₹7,000 (US $50 – US $85)
- High-Resolution Anorectal Manometry (HRAM) – ₹6,000 – ₹10,000 (US $75 – US $120)
- Anorectal Manometry with Balloon Expulsion Test – ₹7,000 – ₹11,000 (US $85 – US $135)
- Comprehensive Pelvic Floor Evaluation (Manometry + EMG + Expulsion Test) – ₹8,000 – ₹12,000 (US $100 – US $145)
Frequently Asked Questions (FAQs) on Anorectal Manometry
What is the recovery time for anorectal manometry?
As there is no anaesthesia involved, anorectal manometry patients recover immediately and can quickly get back to their regular activities, food, and medication regimen following the 30-minute procedure. A brief episode of mild anal discomfort or spotting is possible, but it usually goes away on its own in the span of minutes to hours.
Who needs anorectal manometry?
Patients with persistent constipation with suspected defecatory problems, functional anorectal pain, and faecal incontinence unresponsive to conservative therapy should undergo anorectal manometry. It is also advantageous for evaluating Hirschsprung's disease or post-obstetric sphincter injury and for preoperative evaluation prior to rectal procedures.
Which is the best hospital for Anorectal Manometry Test in Hyderabad, India?
PACE Hospitals, Hyderabad, is regarded as one of the trusted centres for advanced gastrointestinal motility testing and pelvic floor diagnostics. Our Department of Gastroenterology specialises in diagnosing complex bowel disorders using advanced high-resolution anorectal manometry systems.
Our team of expert gastroenterologists focuses on correct diagnosis and targeted treatment planning for conditions such as:
- Chronic constipation
- Fecal incontinence
- Hirschsprung’s disease
- Pelvic floor dysfunction
- Post-surgical bowel dysfunction
Using advanced diagnostic technology, evidence-based protocols, and patient-centred care, PACE Hospitals ensures precise evaluation, early intervention, and improved quality of life — supported by cashless facility options, TPA corporate tie-ups, and assistance with medical insurance processing for eligible patients.
What is the difference between anorectal manometry and endoscopy?
Anorectal manometry is used to diagnose functional abnormalities such as dyssynergia or incontinence by measuring anorectal pressures, sensation, and coordination. Although endoscopy cannot evaluate sphincter function, it can visually scan the mucosa for structural problems such as inflammation or tumours.
Endoscopy requires sedation, whereas manometry does not; they are complementary for a thorough anorectal examination.
What is the cost of Anorectal Manometry Test at PACE Hospitals, Hyderabad?
At PACE Hospitals, Hyderabad, the cost of anorectal manometry typically ranges from ₹5,000 to ₹10,000 and above (approximately US $60 – US $120), depending on:
- Whether high-resolution manometry technology is used
- The need for additional pelvic floor assessment
- Underlying condition (chronic constipation, fecal incontinence, Hirschsprung’s disease, pelvic floor dyssynergia)
- Consultant gastroenterologist evaluation charges
For routine anorectal manometry, the cost is on the lower end, while advanced pelvic floor function studies fall toward the higher range.
After a detailed gastroenterology consultation and clinical evaluation, our team provides a personalised diagnostic plan and precise cost estimate tailored to your symptoms and clinical needs.
How long does a manometry take?
Anorectal manometry usually takes 15 to 45 minutes to finish; the entire process, including catheter insertion and manoeuvres, takes about 30 minutes on average. With preparation and post-test instructions, the entire clinic session could last up to 60 minutes.
What are the risks of anorectal manometry?
Minor discomfort, mild bleeding from mucosal irritation, or infrequent rectal or vaginal perforation in high-risk patients are among the few (<1%) risks. Straining may cause a brief episode of vasovagal syncope, but people who have had previous surgery or are taking anticoagulants are more likely to experience major problems, including perforation.
Looking for the Best Anorectal Manometry Test Hospital Near Me?
If you’re searching for the top anorectal manometry test hospital near me in areas like HITEC City, Madhapur, Kondapur, Gachibowli, Kukatpally, or KPHB, it is important to choose a facility with experienced gastroenterologists and advanced diagnostic motility testing.
Accurate testing requires:
- Comprehensive evaluation of bowel and pelvic floor function
- Specialised anorectal manometry procedure
- Immediate interpretation and follow up planning
- Access to further functional tests if needed
At PACE Hospitals, Hyderabad, patients receive expert consultation and cutting edge diagnostics for effective evaluation of anorectal disorders with personalised treatment guidance.
What is anorectal manometry test?
Anorectal manometry is a minimally invasive test which uses a catheter with sensors and a balloon to assess rectal sensation, rectoanal inhibitory reflex, and anal sphincter pressures (squeeze and rest). To guide biofeedback or surgical therapy, it assesses anorectal function to determine Hirschsprung's illness, dyssynergic defecation, persistent constipation, or fecal incontinence.
How do you prepare for anorectal manometry?
To ensure proper catheter placement, patients self-administer one or two Fleet saline enemas two to four hours prior to the test. They take their necessary medications with little sips of water, but they avoid solid food and most liquids for two hours before. Patients with diabetes can change their insulin dosage.
What is RAIR in anorectal manometry?
RAIR stands for Rectoanal Inhibitory Reflex. During anorectal manometry, the RAIR reflex causes the internal anal sphincter to temporarily relax in response to rectal balloon distension. It typically happens at a volume of 10–30 mL, enabling a stool sample; Hirschsprung's illness is indicated by the absence of RAIR.
How painful is anorectal manometry?
During balloon inflation and catheter placement, anorectal manometry produces a slight pressure sensation or discomfort rather than severe pain. Most patients easily tolerate the 20–30 minute outpatient procedure without sedation; some mild anal pain may continue for a short while thereafter.
Are patients awake during anorectal manometry?
Yes, as this outpatient procedure doesn't require anaesthesia, patients stay completely awake during normal anorectal manometry. To properly evaluate sphincter function, they must actively undertake squeeze, bear-down, and cough manoeuvres. Although it can change pressure measurements, general anaesthesia may occasionally be used in children who are uncooperative.
Is it normal to bleed after anorectal manometry?
No, bleeding following anorectal manometry is not common; nevertheless, in as many as 5% of instances, little spotting may result from mucosal irritation. Significant bleeding should be evaluated right away since it may indicate a rare perforation, especially in high-risk patients who have had past surgery or anticoagulation.
What type of doctor performs anorectal manometry?
Anorectal manometry is usually performed by gastroenterologists or colorectal surgeons with training in GI motility. In specialised motility labs, trained personnel frequently perform the test under the guidance of a physician.
Does anorectal manometry require sedation?
No, anorectal manometry usually doesn't require sedation because patients stay awake to precisely perform the necessary squeeze and bearing-down manoeuvres. Rarely used, sedation may change pressure readings in people who are very unwilling to cooperate or in small children.
What does anorectal manometry feel like?
Similar to the need for a bowel movement, patients usually experience minor pressure or discomfort during catheter placement and balloon inflation. Although cramping may occur during squeeze and bearing-down manoeuvres, severe pain is rare and normally goes away right away as the catheter is removed.
Is Anorectal Manometry Test Covered by Insurance at PACE Hospitals?
Yes, Anorectal Manometry Tests are generally covered under most health insurance policies at PACE Hospitals, subject to policy terms and approval. Since this test is a medically necessary diagnostic procedure for conditions like chronic constipation or incontinence, it is typically included under diagnostic and outpatient care coverage in private and corporate health plans.
At PACE Hospitals, patients can benefit from:
- Cashless hospitalization facilities with empanelled insurance providers
- Assistance from a dedicated insurance and TPA coordination team
- Pre authorization support and documentation guidance
- Transparent cost estimates before admission
- Support for government health schemes where applicable
Coverage depends on outpatient diagnostic testing clauses, sum insured limits, and policy inclusions. Patients are encouraged to share their insurance details in advance so the hospital’s insurance desk can verify eligibility and streamline approvals.