Spinal Fusion Surgery, Procedure & Cost
PACE Hospitals offers advanced spinal fusion surgery in Hyderabad, India, providing effective treatment for conditions such as spinal instability, degenerative disc disease, and spinal deformities. Our spine surgeons perform spinal fusion procedures using both minimally invasive and conventional techniques to stabilize the spine, reduce pain, and improve mobility.
As a trusted center for spine care, we ensure precise diagnosis and personalized treatment planning for each patient. With a focus on safety, faster recovery, and long-term outcomes, our approach helps restore spinal strength and enhance overall quality of life.
Book an Appointment for Spinal Fusion Surgery
Spinal Fusion Surgery Appointment
Why Choose PACE Hospitals for Spinal Fusion Surgery?
Experienced Spine Surgeons in Hyderabad for Advanced Spinal Fusion Procedures
Precision-Guided Spinal Fusion Using Advanced Implants, Pedicle Screws & Minimally Invasive Methods
Transparent Spinal Fusion Surgery with Insurance & Cashless Options
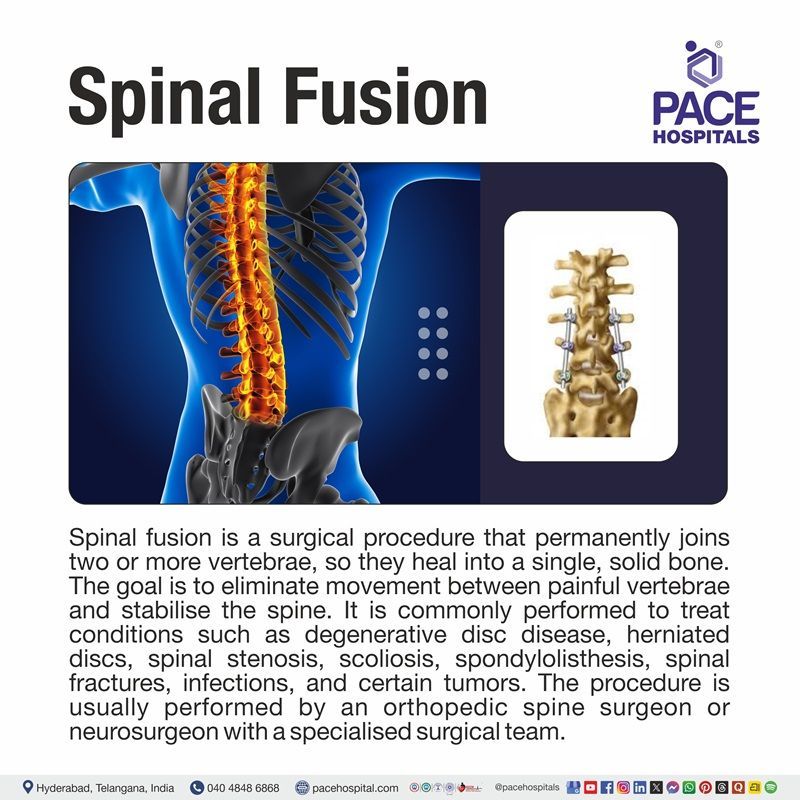
What is Spinal Fusion?
Spinal fusion is a surgical procedure that permanently joins two or more vertebrae in the spine, allowing them to heal into a single, solid bone. The goal of the surgery is to eliminate motion between painful vertebrae and provide stability to the spine.
Spinal fusion is commonly performed to treat several spinal conditions. These include degenerative disc disease, herniated discs, spinal stenosis, scoliosis, spondylolisthesis (when one vertebra slips over another), spinal fractures, infections, and certain spinal tumors. It is also used to correct spinal deformities and to stabilise the spine after removal of a damaged disc. The surgery is generally recommended when non-surgical treatments such as medication, physical therapy, or injections have not relieved symptoms.
This surgery is performed by a spine specialist, generally either an orthopedic spine surgeon or a neurosurgeon who specialises in spinal procedures. In many cases, a surgical team including anesthesiologists, nurses, and surgical assistants works together to ensure the procedure is performed safely and effectively.
Spinal fusion meaning
The term spinal fusion comes from two Latin-derived words:
- “Spina” – meaning “thorn” or “backbone.”
- “Fusio” – meaning “to pour” or “to melt.” It later came to mean “to join together” or “to merge into one.”
So, spinal fusion literally means “joining or melting together of the backbone.” In medical usage, it refers to surgically joining two or more vertebrae, so they heal into a single solid bone.
Types of Spinal Fusion
Spinal fusion procedures are classified based on the surgical approach (direction from which the spine is accessed) and the surgical technique used. The main types of spinal fusion surgery are categorised as follows:
Based on Surgical Approach
Anterior approach
- Anterior cervical discectomy and fusion (ACDF)
- Anterior lumbar interbody fusion (ALIF)
Lateral approach
- Lateral lumbar interbody fusion (LLIF)
- Direct lateral interbody fusion (DLIF)
- Oblique lateral interbody fusion (OLIF)
- Extreme Lateral Interbody Fusion (XLIF)
- Anterolateral Lumbar Interbody Fusion
Posterior approach
- Posterior lumbar interbody fusion (PLIF)
- Posterior cervical fusion
- Transforaminal lumbar interbody fusion (TLIF)
Type based on technique
- Minimally invasive spinal fusion
- Traditional open spinal fusion
Based on Surgical Approach
Anterior approach
The surgeon reaches the spine from the front of the body rather than the back. This approach includes:
- Anterior cervical discectomy and fusion (ACDF): This is performed in the neck (cervical spine). In this procedure, the damaged disc is removed through a small cut in the front of the neck. After removing the disc, a bone graft or cage is placed between the vertebrae, and sometimes a plate and screws are added for stability. It is used to treat herniated discs, nerve compression, and cervical degenerative disc disease.
- Anterior lumbar interbody fusion (ALIF): This is performed in the lower back (lumbar spine). The surgeon makes an incision in the abdomen to access the spine from the front. The damag ed disc is removed and replaced with a bone graft or implant to help the vertebrae fuse together.
Lateral approach
It involves accessing the spine from the side of the body. This approach includes:
Lateral lumbar interbody fusion (LLIF): In LLIF, the surgeon removes the damaged disc and inserts a spacer or cage with bone graft between the vertebrae. This approach helps to restore disc height, relieve nerve compression, and stabilise the spine. It is often used for degenerative disc disease,
scoliosis, and spinal instability. This includes:
- Direct lateral interbody fusion (DLIF): This is performed by approaching the spine directly from the side through the psoas muscle. The disc is removed and replaced with an interbody cage to allow fusion between vertebrae.
- Oblique lateral interbody fusion (OLIF):This surgery differs slightly because the surgeon approaches the spine from a more front-side (oblique) angle, avoiding direct passage through the psoas muscle. This may reduce nerve irritation.
- Extreme lateral interbody fusion (XLIF): This is a specific minimally invasive type of lateral fusion where the surgeon reaches the spine through a small incision in the side of the abdomen.
- Anterolateral lumbar interbody fusion: This combines features of anterior and lateral approaches, accessing the spine from a front-side angle to insert the graft or cage and promote fusion.
Posterior approach
These posterior spinal fusion procedures involve the surgeon accessing the spine from the back side. Include:
- Posterior lumbar interbody fusion (PLIF): This is performed in the lower back through a posterior incision. The surgeon removes the damaged disc from between two lumbar vertebrae and inserts a bone graft or interbody cage into the disc space. Pedicle screws and rods are typically added to provide stability while fusion occurs.
- Posterior cervical fusion: This is done in the neck region from the back. It is commonly used to treat cervical instability, fractures, deformities, or nerve compression. A bone graft is placed along the back of the cervical vertebrae, and metal instrumentation (plates, rods, or screws) is used to maintain alignment during healing.
- Transforaminal lumbar interbody spinal fusion (TLIF): This is a variation of posterior fusion performed in the lumbar spine. The surgeon accesses the disc space from one side (through the foramen) to reduce nerve retraction compared to PLIF. A cage or bone graft is inserted between the vertebrae, and screws and rods are used to secure the spine.
Based on the Techniques
In addition to being classified by surgical approach, spinal fusion procedures can also be categorised based on the surgical technique used to access and operate on the spine. The techniques are:
- Minimally invasive spinal fusion: This technique uses small incisions and specialised instruments to access the spine. Muscles are gently separated rather than cut off and imaging guidance is used to correctly place screws and cages. It causes less muscle injury, lowers blood loss, and typically speeds up recovery.
- Traditional open spinal fusion: This involves making a bigger incision to fully expose the spine. It improves vision for difficult patients, but it may result in longer recovery times and more tissue disturbance.
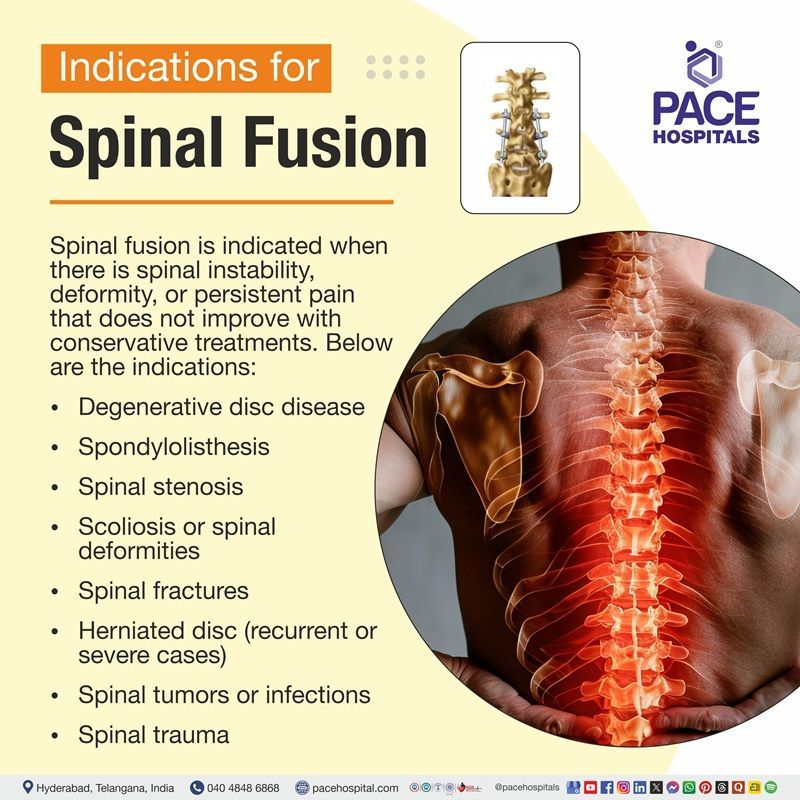
Spinal Fusion Indications
Spinal fusion is indicated when there is spinal instability, deformity, or persistent pain that does not respond to conservative treatment (e.g., medications, physiotherapy, injections). The goal is to stabilise the affected spinal segment, relieve nerve compression, and prevent abnormal motion. The common indications of spinal fusion are:
- Degenerative disc disease
- Spondylolisthesis
- Spinal stenosis
- Scoliosis or spinal deformities
- Spinal fractures
- Herniated disc (recurrent or severe cases)
- Spinal tumors or infections
- Spinal trauma
Degenerative disc disease
In degenerative disc disease, the intervertebral discs lose height, hydration, and elasticity. This can cause abnormal motion between vertebrae, leading to chronic back pain. Spinal fusion is indicated when conservative treatments fail, and pain is due to mechanical instability.
Spondylolisthesis
It is the forward slippage of one vertebra over another. This condition creates abnormal movement and instability, which can also compress nearby nerves. Spinal fusion is indicated when there is symptomatic instability, progressive slippage, or any neurological deficits.
Spinal stenosis
Spinal stenosis involves narrowing of the spinal canal, which compresses the spinal cord or nerves. If decompression surgery (removal of bone or ligament) creates instability. Fusion helps maintain spinal alignment and prevents postoperative instability.
Scoliosis or spinal deformities
In cases of scoliosis and other spinal deformities, the spine abnormally curves. When the curvature is severe, progressive, or causes discomfort and functional limitations, spinal fusion may be performed to correct alignment and prevent further progression.
Spinal fractures
Spinal fusion surgery is recommended when the stability of the spine is compromised, or when there is a risk of further injury to the spinal cord or nerves. Fractures can cause misalignment of the vertebrae, leading to pain, neurological deficits, or deformity. Fusion surgery helps to stabilise the fractured segment, protect the spinal cord or nerves, and restore spinal alignment.
Herniated disc (recurrent or severe cases)
Most herniated discs are treated with discectomy alone. However, in recurrent disc herniations, severe disc degeneration, or when disc removal may leads to instability, spinal fusion may be indicated. This surgery prevents abnormal motion at the affected segment and reduces the risk of recurrent herniation.
Spinal tumors or infections
Spinal tumors and infections can destroy vertebral bone and surrounding structures, leading to spinal instability, deformity, and possible nerve or spinal cord compression. After removal of the tumor or infected tissue, spinal fusion is performed to restore stability, maintain alignment, relieve pain, and protect neurological structures.
Spinal trauma
Severe trauma from accidents or falls can cause vertebral displacement or instability. Spinal fusion is performed to realign and stabilise the spine, reducing the risk of further neurological damage.
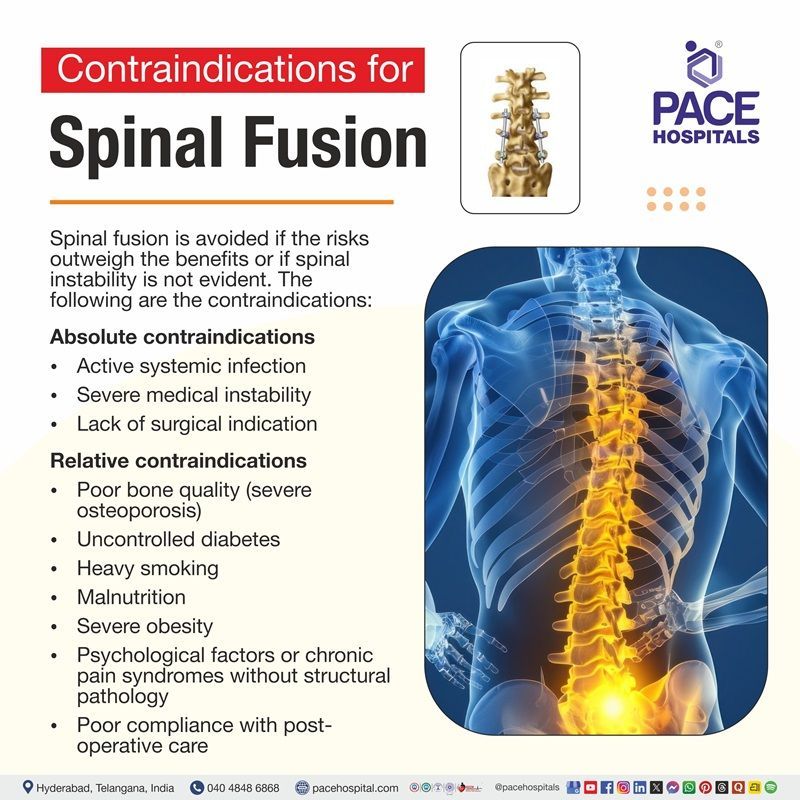
Spinal Fusion Contraindications
Spinal fusion procedure is avoided when the risks outweigh the benefits or when there is no clear indication of spinal instability. Contraindications may be absolute or relative.
Absolute contraindications
- Active systemic infection
- Severe medical instability
- Lack of surgical indication
Relative contraindications
- Poor bone quality (severe osteoporosis)
- Uncontrolled diabetes
- Heavy smoking
- Malnutrition
- Severe obesity
- Psychological factors or chronic pain syndromes without structural pathology
- Poor compliance with post-operative care
Absolute contraindications
- Active systemic infection: If a patient has an ongoing systemic infection (such as sepsis or untreated bacteremia), spinal fusion is contraindicated because introducing implants (screws, rods, cages) can allow bacteria to attach to the hardware. This greatly increases the risk of deep surgical site infection and implant failure. Surgery is delayed until the infection is fully treated.
- Severe medical instability: Patients with unstable cardiac, respiratory, or other life-threatening medical conditions may not tolerate anesthesia or the physiological stress of major spine surgery. In such cases, spinal fusion is contraindicated until the patient’s condition is stabilized.
- Lack of surgical indication: If there is no proven spinal instability, deformity, or structural cause for symptoms, spinal fusion should not be performed. Surgery without a clear indication exposes the patient to unnecessary risks without expected benefit.
Relative contraindications
- Poor bone quality (severe osteoporosis): Fusion relies on strong bone for screw fixation and bone healing. In severe osteoporosis, bones are fragile, increasing the risk of screw loosening, implant failure, or non-union (failed fusion).
- Uncontrolled diabetes: Poorly controlled diabetes impairs wound healing and increases the risk of infection. It also affects bone healing, which may reduce the success rate of fusion.
- Heavy smoking: Tobacco alkaloid can reduce blood flow to bone and inhibit bone-forming cells, which can directly impairs fusion rates. Smoking is associated with delayed healing, pseudoarthrosis, and high complication rate. Many surgeons suggest smoking cessation before elective fusion surgery.
- Malnutrition: Adequate protein, vitamins, and minerals are important for wound healing and bone formation. Malnourished patients have higher risks of infection, poor wound healing, and failed fusion.
- Severe obesity: Obesity increases surgical difficulty, anesthesia risks, wound complications, and mechanical stress on spinal implants. It may also prolong recovery.
- Psychological factors or chronic pain syndromes without structural pathology: If pain is primarily due to psychological causes or chronic pain disorders without clear structural spinal disease, fusion may not relieve symptoms. This can lead to poor patient satisfaction and persistent pain after surgery.
- Poor compliance with post-operative care: Successful spinal fusion requires adherence to activity restrictions, bracing (if prescribed), physiotherapy, and follow-up visits. Patients unlikely to comply with these instructions have a higher risk of complications and failed fusion.
Spinal Fusion Surgery Benefits
Spinal fusion is performed to stabilise the spine, relieve pain, and restore proper alignment. It not only addresses the underlying cause of spinal instability but also improves overall function and quality of life. The procedure offers many advantages, ranging from pain reduction to protection of neurological structures. The following are the advantages of spinal fusion surgery:
- Relieves pain
- Improves spinal stability
- Protection of nerves and spinal cord
- Corrects spinal deformities
- Prevention of further damage
- Improved function and quality of life
- Long-term results
Relieves pain
Spinal fusion reduces pain by eliminating abnormal or excessive movement between unstable vertebrae. When motion at a painful segment is stopped, mechanical back or neck pain decreases significantly, especially in conditions like degenerative disc disease or spondylolisthesis.
Improves spinal stability
Fusion permanently joins two or more vertebrae, which prevents slippage, shifting, or aberrant motion. This surgery is useful in cases of spinal instability caused by trauma, degeneration, or past surgery.
Protection of nerves and spinal cord
After decompressing nerves or the spinal cord, fusion aids in maintaining appropriate alignment and preventing recurring compression. Stabilising the spine lowers the chance of additional nerve irritation or neurological impairment.
Corrects spinal deformities
In conditions such as scoliosis or kyphosis, spinal fusion helps straighten and stabilise the spine. Once corrected, the fused bones maintain alignment and prevent progression of the deformity.
Prevention of further damage
By stabilising weakened or damaged spinal segments, fusion prevents worsening slippage, collapse, or repeated disc problems. This helps stop the progression of certain spinal disorders.
Improved function and quality of life
When pain is reduced and stability restored, patients often regain mobility and are able to perform daily activities more comfortably. This leads to improved independence and overall well-being.
Long-term results
Because the vertebrae are permanently fused into a single solid bone, spinal fusion can provide lasting stability and durable symptom relief, particularly when the surgery is performed for the correct indication.
Get a Free Second Opinion for Spinal Fusion Surgery
At PACE Hospitals, we are committed to providing our patients with the best possible care, and that includes offering second medical opinions with super specialists for treatment or surgery. We recommend everyone to get an expert advance medical second opinion, before taking decision for your treatment or surgery.
Spinal Fusion Procedure Steps
Procedure steps for spinal fusion surgery include the following:
Before Spinal Fusion Surgery
- Preoperative investigations: The surgeon orders tests to ensure the patient is fit for surgery. Blood tests are done to check haemoglobin level, blood sugar, kidney function, and clotting ability. Imaging studies like X-ray, MRI, or CT scan of the spine are reviewed to confirm the exact location and severity of the spinal problem. In some patients, additional tests like an electrocardiogram (ECG) or chest X-ray may be required to assess heart and lung fitness for anaesthesia.
- Medication review: Patients must inform the doctor about all prescription medicines, over-the-counter drugs, vitamins, and herbal supplements they are taking. Blood thinners and certain anti-inflammatory medicines may need to be stopped several days before surgery under medical guidance to reduce the risk of bleeding.
- Informed consent: The surgeon explains the procedure, expected benefits, possible risks and complications, hospital stay, recovery period, and postoperative restrictions. After understanding the details and having their questions answered, the patient signs a written informed consent form agreeing to undergo the surgery.
- Lifestyle optimisation: Patients are advised to stop smoking or using stimulant drug products at least 3 to 4 weeks before surgery, as they delay bone healing and increase the risk of fusion failure. Alcohol consumption needs to be avoided for several weeks before the procedure. Maintaining a healthy weight (ideally BMI below 35), controlling diabetes, and managing blood pressure are important to improve surgical outcomes.
- Fasting instructions: Patients must strictly follow fasting guidelines before surgery. Usually, no solid food is allowed for at least 6 to 8 hours before the procedure, and clear liquids may be stopped a few hours prior, as instructed by the doctor. This helps ensure safe administration of anaesthesia.
During Spinal Fusion Surgery
- Anaesthesia administration: The patient is taken to the operating room and positioned carefully on the operating table. General anaesthesia is given so the patient remains completely asleep and pain-free throughout the procedure. A breathing tube is inserted to help breathing during surgery, and vital signs are monitored continuously.
- Positioning and surgical site preparation: The patient is positioned depending on the location of the spinal problem. The surgical area is cleaned with an antiseptic solution to reduce the risk of infection. Sterile drapes are placed around the area to maintain a sterile environment.
- Surgical incision: The surgeon makes an incision over the affected part of the spine. The muscles and soft tissues are carefully moved aside to expose the spine. In some operations, minimally invasive techniques may be used with smaller incisions and special instruments.
- Removal of the problem area (if required): If spinal fusion is being done to treat a herniated disc, spinal stenosis, or instability, the surgeon may first remove the damaged disc, bone spurs, or part of the vertebra that is pressing on nerves. This step helps relieve nerve compression and pain.
- Placement of bone graft: A bone graft is placed between the affected vertebrae to help them grow together (fuse) into one solid bone. The bone graft may be taken from the patient’s own body (commonly from the pelvis), from a donor (allograft), or may be a synthetic bone substitute.
- Insertion of metal implants: To keep the spine stable while the bones fuse, spinal fusion hardware such as metal screws, rods, or plates is inserted into the vertebrae. These implants hold the bones in the correct position and provide support during the healing process.
- Checking alignment and stability: The surgeon checks the spinal alignment and may use intraoperative X-ray (fluoroscopy) to confirm the correct placement of screws and hardware.
- Closure of incision: Once the fusion materials and implants are secured, the muscles and soft tissues are carefully placed back into position. The incision is closed with sutures or staples. A sterile dressing is applied to protect the wound.
After Spinal Fusion Surgery
- Recovery room monitoring: After the completion of the surgery, the patient is shifted to the recovery room. Vital signs such as blood pressure, heart rate, oxygen level, and breathing are closely monitored as the patient wakes up from anaesthesia. Pain levels are assessed and managed with medications.
- Pain management: Pain control is an important part of recovery. Pain medications may be given through an IV line, orally, or through a patient-controlled analgesia (PCA) pump. As recovery progresses, medications are gradually shifted to oral pain relievers.
- Hospital stay and early mobilisation: Most patients stay in the hospital for a few days, depending on the extent of surgery. Early mobilisation is encouraged to prevent complications such as blood clots and lung infections. With the help of a physiotherapist, the patient is usually assisted to sit, stand, and walk within 24–48 hours after surgery.
- Wound care: The surgical incision is covered with a sterile dressing. The healthcare team monitors the wound for signs of infection like redness, swelling, discharge, or fever. Stitches or staples are usually removed after 10–14 days, unless absorbable sutures are used.
- Use of brace (if advised): In some cases, a spinal brace may be prescribed to support the spine and restrict movement during the healing period.
- Activity restrictions: Patients are advised to avoid bending, lifting heavy objects, or twisting movements for several weeks to months. Gradual return to normal activities is guided by the surgeon and physiotherapist. Driving and returning to work depend on the type of job and recovery progress.
- Physiotherapy and rehabilitation: A structured physiotherapy program is started to improve strength, flexibility, and posture. Rehabilitation helps to restore function and promotes healthy healing of the fused spine.
- Follow-up visits: Regular follow-up appointments are scheduled to monitor healing. X-rays may be taken to check the progress of bone fusion and the position of implants.
Spinal Fusion Complications
Although spinal fusion can reduce pain and improve function in appropriately selected patients. Since it is a major operative intervention involving bone grafting, instrumentation, and alteration of normal spinal biomechanics. Due to its invasive nature and the complexity of spinal anatomy, including proximity to the spinal cord, nerve roots, and major blood vessels, there is an inherent risk of complications. Spinal fusion surgery complications include:
- Infection
- Bleeding & blood clots
- Nerve damage
- Failed fusion (pseudarthrosis)
- Hardware problems
- Adjacent segment disease
- Chronic pain
- Anesthesia risks
Infection
After spinal fusion surgery, there is a risk of infection at the cut (incision) or deeper around the bones and metal implants. Signs may include redness, swelling, fever, or drainage from the wound. Some infections can be treated with antibiotics, but serious ones may need another surgery.
Bleeding and blood clots
During spinal fusion, muscles and tissues are moved to reach the spine, which can cause bleeding. After surgery, patients may not move much for some time. Lack of movement can cause blood clots to form in the legs. In rare cases, these clots can travel to the lungs and become serious.
Nerve damage
The surgery is done close to the spinal nerves. In rare cases, a nerve can be irritated or injured. This may cause numbness, weakness, tingling, or pain in the back, arms, or legs. Sometimes these symptoms improve, but occasionally they can be long-lasting.
Failed fusion (pseudarthrosis)
The goal of spinal fusion is to join two or more bones together so they heal as one solid bone. Sometimes the bones do not heal properly and fail to fuse. When this happens, the spine may remain unstable and pain can continue.
Hardware problems
Metal screws and rods are used to hold the spine steady while it heals. In some cases, the hardware can loosen or break. This may cause pain or discomfort and could require further treatment.
Adjacent segment disease
After fusion, the fused part of the spine no longer moves. Because of this, extra pressure is placed on the nearby spinal segments above and below the fusion. Over time, this added stress can cause those areas to wear out faster and lead to new back problems.
Chronic pain
Some patients may continue to have pain even after surgery. This may be due to nerve irritation, scar tissue, or other spine problems. Additional treatment may be needed to manage ongoing pain.
Anesthesia risks
Spinal fusion is done under general anesthesia. Although usually safe, anesthesia can sometimes cause breathing problems, allergic reactions, or heart issues, especially in older adults or people with other health conditions.
Spinal Fusion Recovery Timeline
Recovery after spinal fusion surgery happens in stages and can take several months to a year for full healing. Stages include:
Immediate recovery
After spinal fusion surgery, patients are usually encouraged to sit up and walk within 24 hours to improve circulation and prevent complications. The hospital stay is about 2–5 days. During the first 2–6 weeks, the surgical wound heals and pain and stiffness gradually improve. Walking is the main recommended activity, while bending, twisting, and heavy lifting are restricted. Fatigue is common, and activity levels are increased slowly under medical guidance.
Functional recovery
Between 6–12 weeks, strength and mobility continue to improve. Many patients with desk jobs can return to work around 8–12 weeks after surgery, whereas those with physically demanding jobs may need more time. Physical therapy may be started or intensified during this stage to improve flexibility and muscle strength. Although patients feel significantly better, care must still be taken to protect the healing spine.
Bone fusion and long-term healing
The actual bone fusion process can take several months. Fusion often occurs over 6-12 months and, in some cases, continues to strengthen for 1-2 years. Even if the discomfort improves earlier, complete internal recuperation takes time. Long-term rehabilitation and final outcomes are determined by factors like age, overall health, smoking status, and if several spinal levels were fused.
What questions can patients ask the healthcare team about spinal fusion?
- Why do I need spinal fusion?
- What happens if I delay or avoid surgery?
- How will the surgery be performed? (open or minimally invasive?)
- How long will the surgery take?
- What type of anesthesia will I receive?
- What is the risk that the bones will not fuse properly?
- What signs of complications should I watch for after surgery?
- How much pain should I expect after surgery?
- When can I walk, drive, or return to work?
- Will I need physical therapy?
- Will I have permanent movement restrictions?
- How will this surgery affect my quality-of-life long term?
Difference between spinal fusion and laminectomy
Spinal Fusion vs Laminectomy
Spinal fusion and laminectomy are two common spine surgeries, but they are performed for different reasons and have different goals. The table below shows the key differences between these procedures.
| Parameters | Spinal fusion | Laminectomy |
|---|---|---|
| Definition | A surgical procedure that permanently joins two or more vertebrae so they heal as one solid bone. | A surgical procedure in which part of the lamina (back portion of the vertebra) is removed to relieve pressure on the spinal cord or nerves. |
| Main goal | To stabilise the spine and prevent abnormal movement between vertebrae. | To decompress (relieve pressure on) the spinal cord or nerve roots. |
| Reason for surgery | Done when there is spinal instability, severe degeneration, fractures, deformity (like scoliosis), or after removal of a damaged disc. | Done mainly for spinal stenosis or nerve compression causing leg or arm pain, numbness, or weakness. |
| Surgical technique | Uses bone grafts and often metal screws, rods, or plates to hold the bones together until they fuse. | Removes bone and sometimes thickened ligaments to create more space; usually does not involve fusion unless instability is present. |
| Recovery time | Longer recovery; bone fusion may take 6–12 months or more. | Usually shorter recovery; many patients improve within weeks to a few months. |
| Outcome focus | Long-term stability and pain reduction from instability. | Relief of nerve-related symptoms such as radiating pain or numbness. |
Spinal Fusion Surgery Cost in Hyderabad, India
The cost of Spinal Fusion Surgery in Hyderabad generally ranges from ₹2,00,000 to ₹7,50,000 and above (approx. US $2,410 – US $9,040).
The exact cost of spinal fusion surgery varies depending on the underlying spinal condition (degenerative disc disease, spinal stenosis, spondylolisthesis, spinal deformity, or trauma), number of spinal levels involved, type of fusion (lumbar, cervical, or thoracic), surgical approach (open or minimally invasive), and implants used (screws, rods, cages). Additional factors such as preoperative imaging (MRI, CT), navigation technology, anesthesia, duration of hospital stay, and postoperative rehabilitation also influence the overall cost. Availability of cashless treatment options, TPA corporate tie-ups, and insurance assistance may further affect expenses.
Cost Breakdown According to Type of Spinal Fusion Surgery
- Single-Level Lumbar Spinal Fusion – ₹2,00,000 – ₹4,00,000 (US $2,410 – US $4,820)
- Multi-Level Lumbar Fusion Surgery – ₹3,50,000 – ₹6,50,000 (US $4,210 – US $7,830)
- Cervical Spine Fusion Surgery – ₹2,50,000 – ₹5,50,000 (US $3,010 – US $6,630)
- Minimally Invasive Spinal Fusion – ₹3,00,000 – ₹7,50,000 (US $3,615 – US $9,040)
- Revision / Complex Spinal Fusion Surgery – ₹4,50,000 – ₹8,00,000+ (US $5,420 – US $9,640+)
Frequently Asked Questions (FAQs) on Spinal Fusion Surgery
What are the permanent restrictions after spinal fusion?
After successful fusion surgery, most individuals can resume normal daily activities. However, some long-term considerations also exist. The fused spinal segment no longer moves, which permanently reduces motion at that level. This may slightly limit flexibility, particularly bending and twisting, if multiple levels are fused. Doctor suggests that heavy repetitive lifting, high-impact activities (such as competitive contact sports), and extreme spinal twisting may be discouraged, especially after multi-level fusion.
These precautions are intended to reduce stress on adjacent spinal segments, as adjacent segment degeneration can occur over time due to increased mechanical load above and below the fused level.
Which Is the Best Hospital for Spinal Fusion Surgery in Hyderabad, India?
PACE Hospitals, Hyderabad, is a trusted centre for advanced spine surgery and comprehensive spinal care, offering specialised treatment for patients with chronic back pain, nerve compression, and spinal instability.
We have highly experienced spine surgeons, neurosurgeons, orthopedic specialists, anesthesiologists, and rehabilitation teams who follow evidence-based surgical protocols to stabilise the spine, relieve nerve compression, and restore mobility.
We manage complex cases and are equipped with state-of-the-art modular operation theatres, spine navigation systems, intraoperative imaging, advanced implants, and structured physiotherapy programs ensuring safe, precise, and patient-centred spinal fusion surgery at PACE Hospitals
How long to recover from spinal fusion surgery?
Recovery from spinal fusion occurs in stages. Hospital stay typically lasts a few days, while return to light daily activities may occur within 4–6 weeks. However, full bone healing may take 6–12 months. Improvement in pain and function often continues gradually during this period. Recovery time varies depending on age, overall health, smoking status, and the number of spinal levels fused.
What is the success rate of spinal fusion?
Spinal fusion surgery success rate varies depending on the condition being treated and patient health. Studies shows that 70–90% of the patients experience significant pain relief and improved function, when surgery is performed for clear spinal instability or nerve compression. Success is usually measured by reduced discomfort and improved daily activity, not complete pain elimination. However, certain risk factors like smoking, excessive body mass, and poor bone quality are associated with lower fusion rates and outcomes.
What Is the Cost of Spinal Fusion Surgery at PACE Hospitals, Hyderabad?
At PACE Hospitals, Hyderabad, the cost of spinal fusion surgery typically ranges from
₹1,90,000 to ₹6,80,000 and above (approx. US $2,290 – US $8,190), making it a competitive option for advanced spine surgery in Hyderabad. However, the final cost depends on:
- Type and severity of spinal condition
- Number of spinal levels involved
- Type of implants used (screws, rods, cages)
- Surgical approach (open vs minimally invasive)
- Duration of hospital stay and ICU requirement
- Diagnostic imaging (MRI, CT scan)
- Postoperative physiotherapy and rehabilitation
For single-level fusion procedures, costs remain toward the lower end, while multi-level or complex spinal fusion surgeries fall toward the higher range.
After a detailed spine evaluation, imaging review, and neurological assessment, our specialists provide a transparent cost estimate tailored to the patient’s condition and surgical plan.
Are there alternatives to spinal fusion?
Alternatives to spinal fusion depend on the diagnosis and severity of symptoms. Non-surgical treatments such as physiotherapy, structured exercise, analgesic medications, and spinal injections are first-line treatment options for many patients. In certain conditions, other approache such as artificial disc replacement or decompression surgery without fusion may be considered. These options aim to relieve nerve pressure or prevent movements. A careful diagnostic evaluation is necessary to determine the most appropriate treatment.
What is the role of physical therapy after spinal fusion?
Physical therapy is essential for healing following spinal fusion surgery. Guided rehabilitation enhances strength, balance, and daily functionality. Physical therapy typically begins with gentle walking before progressing to activities that strengthen and support the core muscles and spine. Education on posture and safe movement is also provided. Structured rehabilitation has been associated with better functional outcomes, reduced disability, and improved confidence in returning to normal activities.
Looking for the Best Spinal Fusion Surgery Hospital Near Me?
If you’re searching for the top spine surgery hospital near me in areas like HITEC City, Madhapur, Kondapur, Gachibowli, Kukatpally, or KPHB, it is important to choose a hospital with experienced spine surgeons and advanced surgical technology.
Effective spinal fusion surgery requires:
- Accurate diagnosis with advanced imaging
- Precision surgical planning
- High-quality implants and fixation systems
- Postoperative rehabilitation and physiotherapy
At PACE Hospitals, Hyderabad, patients receive comprehensive spine care with a multidisciplinary approach aimed at long-term pain relief and improved mobility.
What is spinal fusion surgery?
Spinal fusion is a surgical procedure that permanently joins two or more bones in the spine so they heal into one solid bone. It is commonly performed to treat instability, severe arthritis, fractures, deformity, or nerve compression that has not improved with non-surgical treatment. This procedure uses bone graft material, usually supported by screws and rods, to promote bone growth between vertebrae. Surgery goals are to reduce pain caused by abnormal motion and improve spinal stability and function.
How is lumbar spinal fusion performed?
Lumbar spinal fusion is performed under general anesthesia to join two or more bones in the lower back permanently. The damaged disc is usually removed, and a bone graft is placed between the vertebrae to help them grow together. Metal screws and rods are inserted to stabilise the bones while they heal. Over several months, the bones fuse into one solid segment, reducing movement and pain.
How long does spinal fusion surgery take?
Spinal fusion generally takes between 2 and 6 hours. The duration depends on several factors, including the number of vertebral levels being fused, the surgical approach used, the complexity of the condition, and whether it is a first-time or revision surgery. Single-level fusions using minimally invasive techniques may take closer to 2–3 hours, whereas multi-level or complex reconstructive procedures may take longer. Operative time also includes preparation, positioning, and anesthesia administration.
What to expect 6 months after spinal fusion?
At six months after surgery, substantial healing has usually occurred. Radiographic imaging often shows progressive bone fusion, although complete fusion can take 6–12 months or longer. Most individuals report a significant reduction in preoperative leg pain and improvement in stability-related
back pain.
By this time, many patients have returned to regular daily activities and, in many cases, work. Physical therapy typically focuses on strengthening core muscles and improving endurance. Mild stiffness and occasional discomfort can still occur, particularly after prolonged sitting or activity. Ongoing improvement may continue for up to one year following surgery.
How long screws are used in spinal fusion?
The screws used in lumbar spinal fusion, known as pedicle screws, typically range from about 30 to 50 millimeters (approximately 1.2 to 2 inches) in length, depending on the patient’s anatomy and the size of the vertebrae. Their diameter usually ranges from 5 to 7.5 millimeters. These screws are made of strong materials such as titanium or stainless steel and are designed to remain in the body permanently.
How soon can a patient walk after spinal fusion?
Most patients can walk normally after recovery from spinal fusion. Walking is generally encouraged soon after surgery to reduce complications and promote healing. Once the bones have fused and rehabilitation is complete, many individuals regain stable, independent walking ability. Some stiffness in the lower back may remain because the fused segment no longer moves, but overall mobility for daily walking activities is usually preserved.
What are the consequences of accidental bending after spinal fusion surgery?
Accidental bending after surgery is common during early recovery and usually does not cause damage if it happens once and without force. Fusion hardware, such as rods and screws, stabilises the bone while it heals. However, repetitive or strenuous bending, twisting, or lifting in the first few months may exacerbate discomfort, strain healing tissues, or delay bone fusion. Patients are advised to follow movement precautions carefully until solid bone healing is confirmed.
How painful is spinal fusion surgery?
Spinal fusion is a major surgery and can cause moderate to severe pain immediately afterwards. Post-operative pain is commonly strong for the first few days and improves steadily over several weeks. Modern pain management methods, such as medications and early movement, may help to control discomfort. Many patients experience a reduction in their original pain once healing occurs, although short-term surgical pain is expected.
How is a bone graft obtained for spinal fusion?
Bone graft material used in spinal fusion can be obtained in several ways. Autograft bone is taken from the patient’s own pelvis during surgery, which has strong healing potential but may cause additional soreness at the donor site. Allograft bone comes from screened human donors through tissue banks. Synthetic bone substitutes and growth-stimulating proteins are also commonly used. The choice depends on patient factors, surgeon preference, and surgical goals.
Can spinal fusion be repeated?
Spinal fusion can be repeated if symptoms return or if new spinal problems develop. Revision surgery can be done as a treatment for incomplete bone healing, hardware complications, or stress at nearby spinal levels. However, repeat surgery is generally more complex than the first procedure and may carry higher risks. Careful imaging and clinical evaluation are required before considering revision fusion.
Is Spinal Fusion Surgery Covered by Insurance at PACE Hospitals?
Yes, spinal fusion surgery is generally covered under most health insurance policies at PACE Hospitals, subject to policy terms and approval. Since it is a medically necessary procedure for spinal instability, nerve compression, or deformity, it is typically included under private insurance and corporate health plans.
At PACE Hospitals, patients can benefit from:
- Cashless hospitalization facilities with empaneled insurance providers
- Assistance from a dedicated insurance and TPA coordination team
- Pre-authorization support and documentation guidance
- Transparent cost estimates before admission
- Support for government health schemes where applicable
Coverage depends on waiting periods, sum insured limits, implant coverage, and policy inclusions. Patients are encouraged to share insurance details in advance so the hospital’s insurance desk can verify eligibility and streamline approvals.
Why choose PACE Hospitals?
- A Multi-Super Speciality Hospital.
- NABH, NABL, NBE & NABH - Nursing Excellence accreditation.
- State-of-the-art Liver and Kidney transplant centre.
- Empanelled with all TPAs for smooth cashless benefits.
- Centralized HIMS (Hospital Information System).
- Computerized health records available via website.
- Minimum waiting time for Inpatient and Outpatient.
- Round-the-clock guidance from highly qualified super specialist doctors, surgeons and physicians.
- Standardization of ethical medical care.
- 24X7 Outpatient & Inpatient Pharmacy Services.
- State-of-the-art operation theaters.
- Intensive Care Units (Surgical and Medical) with ISO-9001 accreditation.