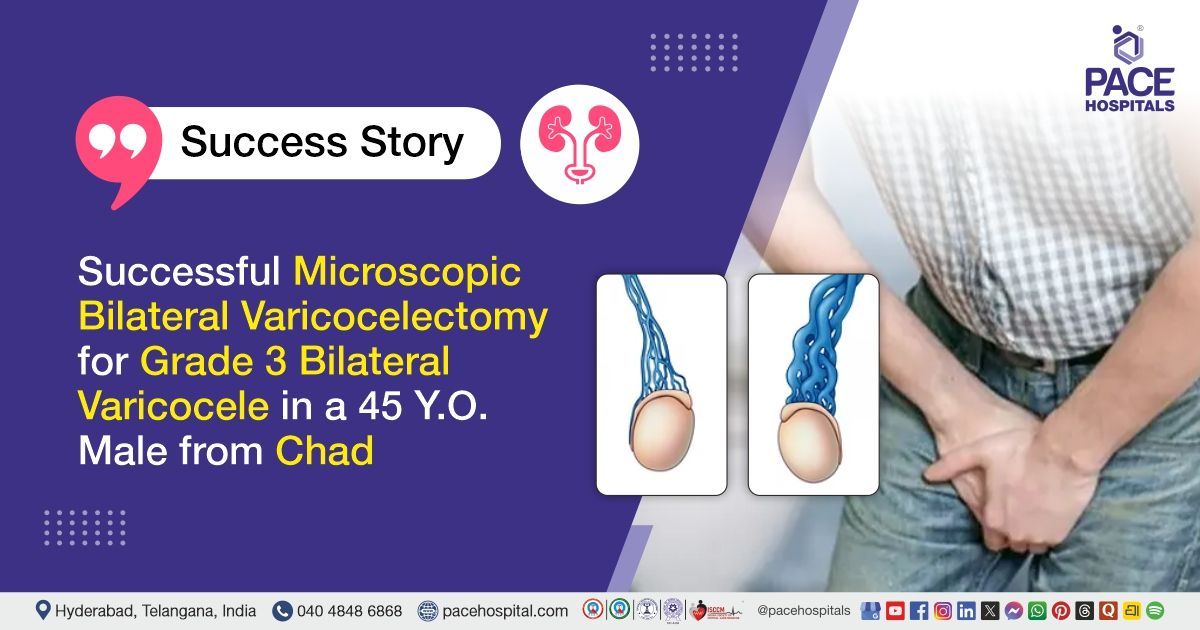
Successful Microscopic B/L Varicocelectomy for Grade 3 B/L Varicocele
PACE Hospitals
PACE Hospital’s expert Urology team successfully performed a Bilateral Varicocelectomy (subinguinal microscopic) on a 45-year-old male patient from Chad diagnosed with bilateral varicocele. The aim of the procedure was to treat the enlarged scrotal veins, relieve discomfort, improve testicular blood flow, and help preserve or enhance testicular function using a precise, minimally invasive microscopic technique.
Chief Complaints
A 45-year-old male patient with a body mass index (BMI) of 21 presented to the Urology Department at PACE Hospitals, Hitech City, Hyderabad, with complaints of bilateral scrotal pain.
Past Medical History
The patient had no significant past medical history and no known drug allergies. There were no chronic illnesses or previous surgeries reported, and overall health was good prior to admission.
On examination
On general examination, the patient was conscious, coherent, and oriented. He was found to have bilateral scrotal swelling with associated discomfort. Local examination revealed prominent dilated scrotal veins bilaterally without any signs of acute inflammation, and the rest of the systemic examination was normal.
Diagnosis
Upon admission to PACE Hospitals, the patient was thoroughly evaluated by the Urology team, including a detailed review of his medical history and a comprehensive clinical examination. He presented with bilateral scrotal pain, raising clinical suspicion of bilateral varicocele.
The patient underwent diagnostic investigations, including clinical evaluation and ultrasonographic assessment of the scrotum, which confirmed the presence of bilateral grade 3 varicocele with normal bilateral testes. Laboratory investigations, including complete blood picture, renal function tests, blood sugar, coagulation profile, serum electrolytes, and viral screening for HIV, Hepatitis B, and C, were all within normal limits. Cardiovascular, abdominal, and neurological examinations were normal, and the respiratory system examination was normal with no abnormalities.
Based on these confirmed findings, the patient was advised to undergo
Bilateral grade 3
Varicocele Treatment in Hyderabad, India, under the expert care of the Urology Department.
Medical Decision Making (MDM)
After a detailed consultation with Dr. Abhik Debnath, Consultant Laparoscopic Urologist, a comprehensive evaluation was conducted focusing on the patient’s presentation of bilateral scrotal pain and scrotal swelling. Clinical examination and diagnostic assessment confirmed the presence of bilateral grade 3 varicocele with no evidence of acute infection or other significant scrotal pathology.
It was determined that bilateral subinguinal microscopic varicocelectomy was the most appropriate intervention to relieve pain, improve venous drainage, prevent progression of symptoms, and preserve testicular function.
The patient and his family members were informed about the diagnosis of bilateral varicocele, the planned surgical management, the associated risks, and the expected benefits aimed at relieving symptoms and preventing future complications.
Surgical Procedure
Following the decision, the patient was scheduled to undergo a Bilateral varicocelectomy Surgery in Hyderabad at PACE Hospitals, under the expert care of the urology department.
The procedure involved the following steps:
- Patient Preparation and Anaesthesia: The patient was taken to the operating room and placed in a supine position. Under strict aseptic precautions, general anaesthesia was administered. The genital and groin regions were shaved, cleaned, and draped in a sterile fashion.
- Surgical Exposure (Subinguinal Approach): A small subinguinal incision was made on each side just below the inguinal canal. The spermatic cord was carefully isolated and delivered into the operative field without opening the inguinal canal.
- Microscopic Identification of Structures: Under operating microscope magnification, the components of the spermatic cord were dissected carefully. The testicular artery, lymphatic channels, and vas deferens were identified and preserved. Dilated and tortuous veins were clearly visualized bilaterally.
- Ligation of Dilated Veins: All enlarged internal and external spermatic veins were meticulously ligated and divided using fine sutures, ensuring complete interruption of abnormal venous reflux while preserving arterial and lymphatic supply.
- Closure and Completion: Hemostasis was achieved, and the spermatic cord was repositioned. The incision was closed in layers with absorbable sutures, and sterile dressing was applied. The procedure was completed without complications.
Postoperative Care
Post-operatively, the patient was monitored for pain control, wound status, and scrotal swelling. Scrotal support was advised to reduce discomfort and minimize postoperative edema. Regular wound care and dressing changes were performed to ensure proper healing and prevent infection. The patient remained hemodynamically stable with an uneventful recovery and was discharged in stable condition.
Discharge Medications
Upon discharge, the patient was prescribed medications for prevention of post-operative infection, control of pain, reduction of inflammation and scrotal swelling, gastric protection, and nutritional support to promote healing and recovery following surgery. These were advised for short-term use with continuation based on symptom improvement and follow-up assessment.
Advice on Discharge
The patient was advised to continue a normal diet as tolerated and to use scrotal support to reduce discomfort and aid in recovery following surgery.
Emergency Care
The patient was instructed to contact the emergency ward at PACE Hospitals in the event of an emergency or development of symptoms such as fever, increasing scrotal pain, swelling, or wound discharge.
Review and Follow-up Notes
The patient was advised to return for a follow-up visit with the Urologist in Hyderabad at PACE Hospitals after 3 days for dressing.
Conclusion
This case highlights a patient with bilateral scrotal pain diagnosed as bilateral grade 3 varicocele. He underwent successful bilateral subinguinal microscopic varicocelectomy under general anaesthesia without complications. The postoperative course was uneventful, and the patient was discharged in stable condition.
Clinical Overview and Management Principles in Varicocele
Varicocele is a common condition resulting from dilatation of the pampiniform venous plexus due to venous reflux, often presenting with scrotal discomfort or heaviness. A urologist/urology doctor evaluates the condition based on symptom severity, clinical grading, and associated complications to guide management decisions. Microsurgical subinguinal varicocelectomy is the preferred surgical approach as it allows precise ligation of affected veins while preserving the testicular artery and lymphatic channels. This reduces the risk of recurrence and postoperative complications such as hydrocele formation. Bilateral involvement may suggest a more generalized venous insufficiency requiring careful evaluation. Timely intervention in symptomatic cases ensures effective symptom relief and prevents progression. Overall, microsurgical repair remains the gold standard for optimal surgical outcomes.
Frequently Asked Questions (FAQs)
What is the recovery time after a bilateral varicocelectomy?
The typical recovery time after a bilateral varicocelectomy is around 2-4 weeks. Patients should avoid strenuous activities during this period to allow the body to heal. Wearing scrotal support helps minimize swelling and provides comfort. Follow-up appointments ensure the wound is healing properly and that there are no complications. The treating physician will provide guidance on when to resume normal activities.
What should be done if there is swelling or pain after surgery?
Mild swelling and pain after surgery are common and usually improve gradually over time, but if the swelling or pain gets worse or does not start reducing after a few days, you should contact your healthcare provider; severe or ongoing discomfort may be a sign of a complication that needs medical attention, pain can be controlled with prescribed medications, but it is important to seek medical advice if symptoms continue, and a follow-up visit will help the doctor check the healing process and ensure proper recovery.
How long should scrotal support be worn after surgery?
Scrotal support should be worn for a few weeks after surgery to help reduce swelling and discomfort; it also gives proper support during the recovery period and limits movement of the scrotal area, which helps healing, and the exact time for using it depends on the surgeon’s advice, usually about 2–4 weeks, so it should be worn during physical activities as well as while resting, and regular follow-up visits will help the doctor confirm that it is being used correctly for proper healing.
When should I follow up after surgery?
A follow-up appointment is usually needed within 3–5 days after surgery for dressing changes and to check wound healing; during this visit the doctor will assess recovery progress and look for any signs of infection or other complications, and based on how the patient is healing, further follow-up visits may be scheduled as needed according to the surgeon’s recommendations, so it is important to attend all follow-up appointments to ensure proper healing and safe recovery.
Can physical activity be resumed after surgery?
Patients should avoid heavy physical activity and strenuous exercise for about 2-4 weeks after surgery. This period allows the surgical site to heal without putting additional stress on the body. Lighter activities, such as walking, can be resumed as per the doctor’s advice. Once the initial recovery phase is complete, and the follow-up visit confirms proper healing, normal activities can be gradually resumed. Always consult the doctor before returning to intense physical exertion.
Are there any dietary restrictions post-surgery?
No specific dietary restrictions are required after a bilateral varicocelectomy. However, maintaining a healthy, balanced diet is crucial for overall recovery. Foods rich in vitamins, minerals, and antioxidants can help promote healing and support the immune system. Staying hydrated is also essential for recovery. The patient is encouraged to follow a regular diet to maintain energy levels and support the body’s healing process.
Is it normal to experience mild bruising or redness after surgery?
Mild bruising and redness around the surgical site are common after surgery and usually settle on their own within a few weeks; this is a normal part of the healing process and is generally not a cause for concern, but if the bruising or redness increases, becomes painful, or looks unusual, you should seek medical advice to rule out any complications, as temporary discoloration and swelling can happen due to the body’s natural healing response and typically improve over time, and a follow-up visit will help the doctor confirm that healing is progressing properly.
What are the signs that indicate a complication after the surgery?
Signs of possible complications after surgery include severe pain, fever, excessive swelling, or increasing redness at the surgical site; any unusual symptoms or changes in the operated area should be reported to the healthcare provider without delay, and if there is bleeding or signs of infection like pus or abnormal drainage, immediate medical attention is required, so it is important to stay alert to any changes in symptoms and seek help when needed, while regular follow-up visits help in early detection and management of complications.
Can the surgery improve male fertility?
Bilateral varicocelectomy is a surgery done to improve sperm quality, which can help in improving male fertility; after the procedure, many patients may see better sperm count, motility (movement), and overall reproductive health, but the level of improvement can vary from person to person, so regular follow-up visits are important to monitor fertility progress, and the doctor may also suggest further fertility evaluations if needed to understand the long-term effects on fertility.
When is it safe to resume normal activities after surgery?
It is generally advised to wait about 4–6 weeks before returning to normal activities following bilateral varicocelectomy, as this gives enough time for proper healing of the surgical site and helps reduce the risk of complications; starting physical activities too early may cause discomfort or affect the healing process, so the doctor will check recovery during follow-up visits and guide you on when it is safe to resume normal routine, and it is important to always follow the surgeon’s instructions for post-surgery care.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868