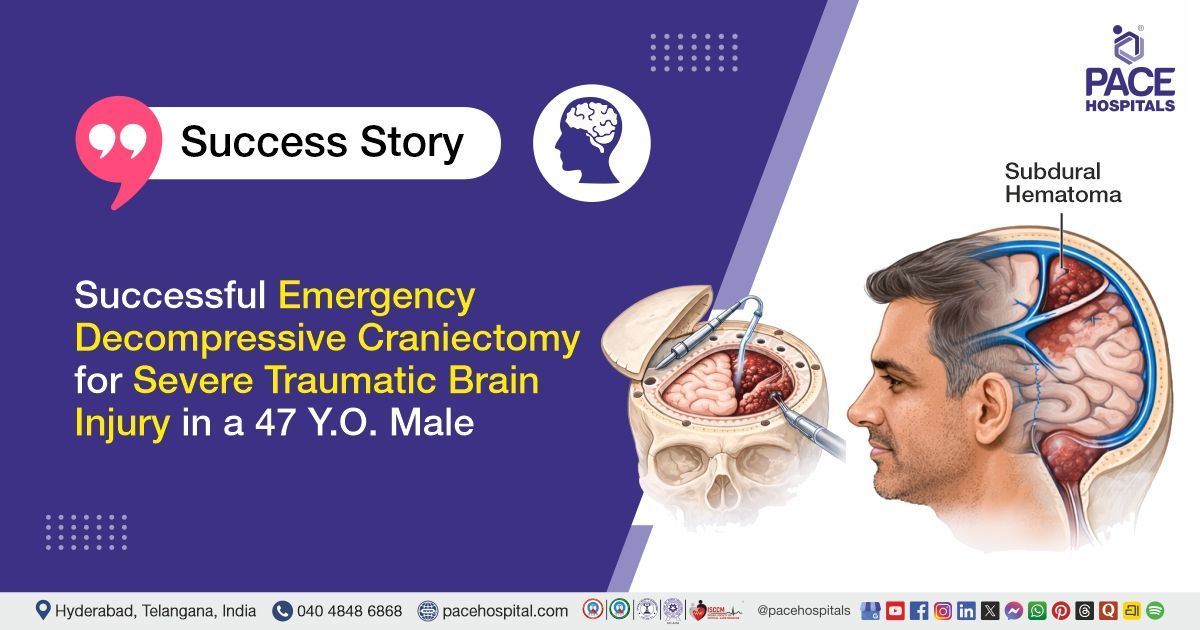
Successful Emergency Decompressive Craniectomy for Severe Traumatic Brain Injury in a 47 Y.O. Male
PACE Hospitals
PACE Hospitals’ expert Neurosurgery team successfully performed a Right Decompressive Craniectomy with Lax Duraplasty and Abdominal Bone Flap Placement on a 47-year-old male patient diagnosed with traumatic right frontoparietotemporal subdural hematoma (SDH), right temporal contusion, and left parietal contusion, with the aim of relieving raised intracranial pressure, preventing further brain injury, and improving cerebral blood flow to support optimal neurological recovery.
Chief Complaints
A 47-year-old male patient with a body mass index (BMI) of 20 presented to the Neurosurgery Department at PACE Hospitals, Hitech City, Hyderabad, with a history of road traffic accident–related head injury, associated with decreased consciousness and multiple episodes of vomiting. The injury was sustained following a fall from a bike. There was no history of loss of consciousness or seizures. On examination, he had bleeding from the left ear and nose.
Past Medical History
The patient had no known prior history of chronic medical illnesses such as hypertension, diabetes mellitus, or seizure disorder before the current episode. There was no documented history of previous head injury or neurosurgical intervention. No other significant past medical or surgical history was noted.
On Examination
On general examination, the patient was found to be moderately built and nourished, with an abnormal general condition and guarded clinical status. Neurological examination was abnormal, with depressed consciousness, impaired Glasgow Coma Scale, and unequal pupils initially, indicating significant neurological involvement. Multiple abrasions were present over the face, and bleeding from the left ear and nose was noted, which was abnormal and suggestive of associated traumatic injury. Respiratory status was abnormal at presentation, with reduced oxygenation and signs concerning for aspiration. Overall, the systemic examination was abnormal, consistent with severe traumatic brain injury with associated neurological and respiratory compromise.
Diagnosis
Following the clinical evaluation, the Neurosurgery team at PACE Hospitals conducted a detailed assessment focusing on the patient’s complaints following a road traffic accident due to a fall from a bike, which resulted in severe head injury, decreased consciousness, repeated vomiting, and bleeding from the left ear and nose.
A comprehensive clinical and systemic examination was performed to assess the severity of the trauma. On admission, the patient was in a guarded condition with a reduced Glasgow Coma Scale score, abnormal pupillary response, low oxygen saturation on room air, and multiple facial abrasions, indicating significant traumatic brain injury. The patient was intubated in view of a low GCS score and signs of aspiration. Radiological evaluation with CT brain confirmed a traumatic right fronto-parieto-temporal acute subdural hematoma with midline shift, right temporal hemorrhagic contusion, left-sided cerebral contusion, and associated skull fractures involving the left parieto-temporal and mastoid temporal regions. HRCT chest findings were suggestive of aspiration pneumonia, and subsequent imaging indicated features of pleural effusion.
Laboratory investigations further supported the diagnosis and guided treatment planning. Initial blood tests showed abnormal white blood cell count suggestive of infection, followed by persistent anaemia on subsequent evaluations. Blood sugar levels and HbA1c were in the diabetic range, indicating de novo diabetes. Viral screening was positive for hepatitis B infection. Renal function was largely within normal limits, with occasional mild abnormalities in urea levels. Procalcitonin levels were elevated, supporting the presence of bacterial infection. Sputum cultures initially showed bacterial growth and later revealed multidrug-resistant organisms, leading to escalation of antibiotics as per sensitivity. Blood and urine cultures remained within normal limits with no bacterial growth detected. These findings indicated severe traumatic brain injury complicated by respiratory infection and associated systemic comorbidities.
Based on these findings, the patient was advised to undergo Traumatic brain injury Treatment in Hyderabad, India, under the expert care of the Neurosurgery Department to evacuate the hematoma, relieve raised intracranial pressure, prevent further neurological deterioration, and facilitate recovery and rehabilitation.
Medical Decision Making (MDM)
After a detailed consultation with Dr. U.L. Sandeep Varma, Consultant Neurosurgeon, and cross consultations with Dr. Pradeep Kiran Panchadi, Consultant pulmonologist, and Dr. Tripti Sharma, Endocrinologist, a comprehensive evaluation was performed to determine the most appropriate diagnostic and therapeutic approach. Considering the patient’s history of road traffic accident due to a fall from a bike, associated head injury, decreased consciousness, repeated vomiting, and bleeding from the left ear and nose, along with clinical findings of a guarded general condition, low Glasgow Coma Scale score, abnormal pupillary response, low oxygen saturation, and multiple facial abrasions, a focused neurological examination, systemic assessment, and radiological evaluation were undertaken to formulate an optimal treatment strategy.
Based on the clinical findings, imaging, and laboratory investigations, which confirmed traumatic right fronto-parieto-temporal subdural hematoma, right temporal contusion, left parietal contusion, midline shift, and associated skull fractures, it was determined that Right Decompressive Craniectomy with Lax Duraplasty and Abdominal Bone Flap Placement was identified as the most suitable approach to evacuate the hematoma, relieve raised intracranial pressure, reduce brain compression, prevent further neurological deterioration, and support neurological recovery. Supporting investigations also showed abnormal infection-related findings, aspiration-related lung involvement on chest imaging, sputum culture positivity, anaemia, abnormal diabetic profile, and hepatitis B positivity, all of which were taken into consideration during perioperative and postoperative management.
The patient and his family members were thoroughly counselled regarding the diagnosis, the need for emergency surgery, the procedure details, possible ventilatory support, postoperative ICU care, potential risks and benefits, the expected recovery course, and the importance of continued rehabilitation and follow-up care.
Surgical Procedure
Following the diagnosis, the patient was scheduled to undergo Right Decompressive Craniectomy with Lax Duraplasty and Abdominal Bone Flap Placement Surgery in Hyderabad at PACE Hospitals, under the supervision of the expert Neurosurgery Department.
The surgical procedure involved the following steps:
- Patient Preparation and Surgical Exposure: The procedure was performed under strict aseptic precautions with the patient under general anaesthesia. The surgical site was cleaned, painted, and draped. A right fronto-parieto-temporal (FPT) scalp incision was made, and the skin flap was carefully elevated to expose the underlying skull.
- Craniotomy and Bone Flap Elevation: Multiple burr holes were created in the skull, and these were connected to raise a bone flap, providing access to the intracranial compartment. The bone flap was removed and preserved for later use, ensuring adequate exposure of the dura and underlying hematoma.
- Dural Opening and Hematoma Evacuation: The dura mater was incised, and the subdural hematoma (SDH) was identified. The accumulated blood clot was carefully evacuated to relieve pressure on the brain. Hemostasis was meticulously secured to prevent further bleeding.
- Lax Duraplasty and Decompression: A lax duraplasty was performed using pericranial graft to expand the dural space, allowing for brain swelling and reducing intracranial pressure. This step ensured adequate decompression and prevention of secondary brain injury.
- Closure and Bone Flap Preservation: After achieving complete hemostasis, the surgical wound was closed in layers over a drain. The removed bone flap was preserved by placing it in the left anterior abdominal wall for future cranioplasty, ensuring protection and viability for later reconstruction.
Postoperative Care
Postoperatively, the patient was managed in the intensive care unit (ICU) with ventilatory support and close neurological monitoring. Due to poor GCS, a tracheostomy was performed, and treatment was adjusted based on clinical condition and culture results to manage infection. Oxygen support was gradually reduced, and chest as well as limb physiotherapy was initiated to improve respiratory function and mobility. Serial imaging after surgery showed reduction in the hematoma and improvement in midline shift, although residual hemorrhage and cerebral edema persisted.
Once stable, the patient was shifted to the room and later discharged with advice for medications, wound and tracheostomy care, and rehabilitation for neurological recovery.
Discharge Medications
At the time of discharge, the patient was advised medications aimed at managing infection, relieving pain and fever, preventing seizures, and protecting gastric mucosa. Additional medications were prescribed to support neurological recovery, improve alertness and cognitive function, and enhance nerve health. Anticoagulation therapy was initiated to prevent blood clot formation, while respiratory medications including nebulisation were advised to improve airway clearance and lung function. Supportive therapy for bowel regulation was also given to prevent constipation. In view of elevated blood sugar levels, insulin therapy was prescribed for glycaemia control using both long-acting and short-acting regimens. Overall, the medication plan was tailored to support neurological recovery, prevent complications, manage infection, and stabilise associated comorbid conditions.
Advice on Discharge
At the time of discharge, the patient was advised to maintain proper wound care to ensure healing and prevent infection, along with regular tracheostomy care to maintain airway hygiene and patency. Suture removal was scheduled. The patient was also instructed to continue physiotherapy to improve mobility and support neurological recovery. In addition, strict measures for bed sore prevention were recommended, including regular repositioning and skin care.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms such as fever, breathlessness, seizures, or decreased consciousness.
Review and Follow-up Notes
The patient was advised to return for a follow-up with the Neurosurgeon in Hyderabad at PACE Hospitals after 10 days, and a follow-up with a Medical Gastroenterologist was also recommended.
Conclusion
This case highlights the timely emergency management of severe traumatic brain injury following a road traffic accident. The patient underwent right decompressive craniectomy with lax duraplasty and required intensive postoperative care, including ventilatory support, tracheostomy, infection control, and physiotherapy. With multidisciplinary care and close monitoring, the patient was stabilised and discharged with advice for rehabilitation and follow-up.
Multidisciplinary Approach in Severe Brain Injury Care
Severe traumatic brain injuries require rapid assessment and timely intervention by an experienced neurosurgeon to prevent irreversible neurological damage. Early decompressive procedures play a crucial role in reducing intracranial pressure and improving survival outcomes. However, recovery depends on comprehensive postoperative critical care, including ventilatory support, infection control, and continuous neurological monitoring.
Many patients may require prolonged respiratory support and structured rehabilitation due to delayed neurological recovery. Associated systemic conditions can further complicate management and require coordinated care. A multidisciplinary approach involving a Neurosurgeon/Neurosurgery doctor, intensive care team, and rehabilitation specialists is essential. Overall, long-term outcomes rely not only on surgery but also on sustained critical care and rehabilitation.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868