Successful Laparoscopic Ovarian Cystectomy for B/L Large Dermoid Cysts
PACE Hospitals
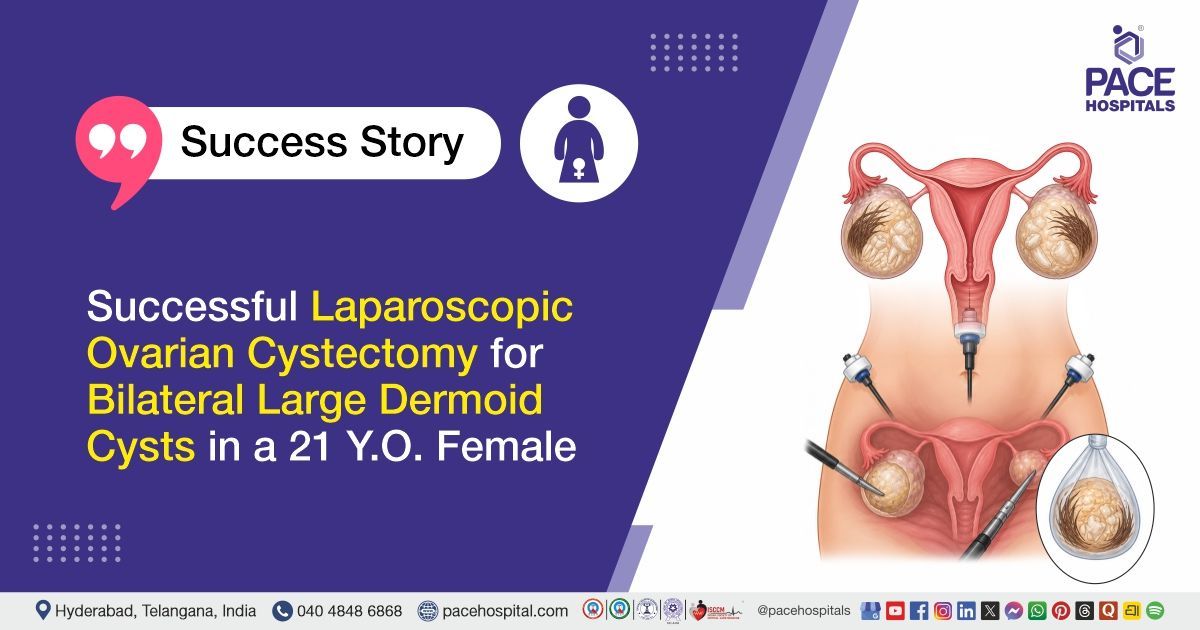
PACE Hospitals’ expert gynaecology team successfully performed a Laparoscopic Bilateral Ovarian Dermoid Cystectomy on a 21-year-old female patient diagnosed with bilateral large ovarian dermoid cysts with asymptomatic cholelithiasis. The aim of the procedure was to safely remove the cysts, relieve symptoms, prevent complications such as rupture or torsion, and preserve as much healthy ovarian tissue as possible to maintain future fertility.
Chief Complaints
A 21-year-old female patient with a body mass index (BMI) of 20 presented to the Gynaecology Department at PACE Hospitals, Hitech City, Hyderabad, with complaints of lower abdominal pain, abdominal bloating, and intermittent epigastric pain.
Past Medical History
The patient had no significant past medical or surgical history. She was previously on medication for anxiety, but was not taking any medications at the time of admission. There was no history of allergies or other chronic illnesses.
Menstrual and Obstetric History
The patient had regular menstrual cycles occurring every 28–30 days, with no history of dysmenorrhoea. She is nulligravida, with no history of prior pregnancies, abortions, or live births.
On Examination
On general examination, the patient was conscious, coherent, and oriented. She appeared hemodynamically stable. Systemic examination revealed equal air entry bilaterally in the respiratory system. Normal heart sounds were heard on cardiovascular examination. Abdominal examination showed a soft abdomen with a palpable pelvic mass corresponding to an enlarged uterus. Breast examination was normal with no lumps or abnormalities detected.
Diagnosis
Upon admission to PACE Hospitals, the patient was evaluated by the Gynaecology team with a detailed clinical history and examination. General examination revealed that the patient was conscious, coherent, and cooperative. Systemic examination showed equal bilateral air entry in the respiratory system, normal heart sounds on cardiovascular examination, and a soft abdomen with a palpable pelvic mass corresponding to an enlarged uterus size. Breast examination was normal with no lumps or abnormalities detected. Per abdominal findings suggested a large pelvic mass arising from the uterus region.
Ultrasound imaging and preoperative evaluation revealed bilateral large ovarian dermoid cysts, with the left ovarian cyst measuring approximately 8.5 × 6.25 cm and the right ovarian cyst measuring approximately 7 × 7 cm, both showing solid components. Imaging also incidentally suggested asymptomatic cholelithiasis (gallstones). There was no evidence of free fluid in the pelvis or other intra-abdominal abnormalities.
Based on the confirmed findings, the patient was advised to undergo Ovarian Dermoid Cysts Treatment in Hyderabad, India, along with asymptomatic cholelithiasis (gallstones) under the expert care of the gynaecology department.
Medical Decision Making (MDM)
After a detailed consultation with Dr. Mugdha Bandawar, a Gynaecologist, and cross consultation with Dr. Suresh Kumar S, Surgical Gastroenterologist, a comprehensive evaluation of the patient was undertaken. Considering her complaints of lower abdominal pain, bloating, and intermittent epigastric pain, clinical examination revealed a palpable pelvic mass. Ultrasound imaging and preoperative evaluation confirmed bilateral huge ovarian dermoid cysts, with the left ovarian cyst measuring 8.5 × 6.25 cm and the right ovarian cyst measuring approximately 7 × 7 cm, both with solid components suggestive of dermoid cysts. Incidental imaging findings also revealed asymptomatic cholelithiasis, with no other significant abdominal or pelvic abnormalities.
Further evaluation, including clinical assessment and radiological findings, confirmed the diagnosis of bilateral huge ovarian dermoid cysts with asymptomatic cholelithiasis. Based on these findings, it was determined that laparoscopic bilateral ovarian dermoid cystectomy was the most appropriate surgical management to remove the cysts, preserve ovarian tissue, alleviate symptoms, and prevent potential complications such as torsion, rupture, or infection.
The patient and her family members were counselled in detail regarding the diagnosis, planned procedure, potential risks and benefits, and postoperative recovery expectations. Following counselling, informed consent was obtained for surgical intervention.
Surgical Procedure
Following the decision, the patient was scheduled to undergo a Laparoscopic Bilateral Ovarian Dermoid Cystectomy Surgery in Hyderabad at PACE Hospitals under the supervision of the expert Gynaecology Department.
The following steps were carried out during the procedure:
- Laparoscopic Access and Entry: The patient was administered general anaesthesia and positioned appropriately. Pneumoperitoneum was created and laparoscopic ports were inserted under direct vision to access the abdominal cavity safely.
- Intraoperative Assessment: A detailed laparoscopic survey revealed a large right ovarian dermoid cyst (~7 × 7 cm) and a large left ovarian dermoid cyst (~8 × 7 cm). The uterus and bilateral fallopian tubes were inspected and found to be normal.
- Bilateral Ovarian Cystectomy: Cystectomy was performed on both ovaries. The right ovarian cyst was removed with preservation of the ovary. On the left side, cystectomy was performed with partial ovarian preservation while completely excising the cyst wall.
- Intraoperative Complication and Procedure Modification: During surgery, rupture of the dermoid cyst occurred, leading to spillage of contents and an increased risk of infection. In view of this, the planned cholecystectomy was aborted, and this decision was communicated to the patient’s relatives intraoperatively.
- Peritoneal Toilet, Hemostasis, and Closure: Thorough peritoneal lavage was performed to clear the cyst contents. Hemostasis was achieved and confirmed. Instrument count was verified as correct, and laparoscopic ports were closed after ensuring
Postoperative Care
Postoperatively, the patient was monitored in the Surgical Intensive Care Unit (SICU) for observation and later shifted to the ward once she was hemodynamically stable. She received treatment for infection prevention, gastric protection, control of nausea and vomiting, pain relief, bowel regulation, and maintenance of hydration and electrolyte balance. An injection was also administered on the first postoperative day to suppress ovarian activity and reduce the risk of recurrence of dermoid cysts. The histopathology report showed a benign ovarian tumor (mature cystic teratoma/dermoid cyst) containing tissues like hair, fat, and bone, with no signs of cancer. The patient showed good recovery and was discharged in a hemodynamically stable condition.
Discharge Medications
Upon discharge, the patient was prescribed medications for the prevention of postoperative infection, control of pain and inflammation, reduction of postoperative swelling, gastric protection, bowel regulation, and overall supportive care. She was also advised to use a topical application for local wound care to promote healing and prevent infection. In addition, a nutritional supplement was prescribed for continued recovery and general health support over the following months.
Advice on Discharge
The patient was instructed to follow a high-protein diet and avoid junk food and outside food to support healing and recovery. She was also advised to avoid heavy lifting and strenuous physical activities during the postoperative period to prevent strain and promote proper recovery.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms like abdominal pain, heavy menstrual bleeding, or fever.
Review and Follow-up Notes
The patient was advised to return for a follow-up appointment with the Gynaecologist in Hyderabad at PACE Hospitals after 1 week.
Conclusion
This case highlights bilateral huge ovarian dermoid cysts with asymptomatic cholelithiasis managed by laparoscopic bilateral ovarian cystectomy. The procedure was successfully completed with preservation of ovarian tissue, despite intraoperative cyst rupture and deferment of cholecystectomy. The postoperative course was uneventful, and discharge was given in a hemodynamically stable condition with appropriate follow-up advice.
Key Considerations in the Management of Bilateral Ovarian Dermoid Cysts with Intraoperative Challenges
Effective management of bilateral ovarian dermoid cysts requires accurate diagnosis through clinical evaluation and imaging, followed by planned minimally invasive surgical intervention guided by a gynaecologist/gynaecology doctor with a focus on fertility preservation. In large or complex cysts, careful laparoscopic technique is essential to ensure complete cyst removal while minimizing ovarian damage. Intraoperative complications such as cyst rupture must be promptly managed with thorough peritoneal lavage to reduce the risk of infection and chemical peritonitis. Surgical decisions may need real-time modification, including deferring additional procedures when safety concerns arise. Postoperative care is crucial for monitoring stability, preventing infection, and supporting recovery with appropriate medical therapy. A multidisciplinary approach and individualized patient-centered planning further enhance surgical safety and long-term outcomes.
Frequently Asked Questions (FAQs)
Why was laparoscopic ovarian dermoid cystectomy preferred in this case?
Laparoscopic surgery is a keyhole surgical technique used to remove dermoid cysts through small cuts in the abdomen, allowing the surgeon better visibility inside. It helps in carefully removing the cyst while preserving healthy ovarian tissue, which is especially important in young patients. Compared to open surgery, recovery is usually quicker, with less pain and a shorter hospital stay. It also generally results in less blood loss and a lower risk of infection. Because of these advantages, laparoscopic surgery is commonly used for large but non-cancerous (benign) ovarian cysts.
Why was the ovary preserved even after removing large dermoid cysts?
Ovarian preservation is important because it helps maintain hormone production and future fertility. Even when cysts are large, surgeons try to remove only the cyst (cyst wall) while saving as much healthy ovarian tissue as possible. In some cases, part of the ovary is preserved, which still supports normal reproductive function. This approach helps reduce the risk of early hormonal imbalance or changes in the body. It is especially important in young patients, as it supports future fertility and overall reproductive health.
What is the significance of finding hair and sebaceous material inside the cyst?
Dermoid cysts, also known as mature teratomas, often contain tissues like hair, fat, and calcifications. These findings confirm the benign nature of the cyst in most cases. Such contents develop from germ cells that can form different tissue types. Although unusual in appearance, they are common in dermoid cysts. Histopathology is done to rule out a rare malignancy.
Why was cholecystectomy planned but later not performed?
Gallstones were detected, but were asymptomatic, so surgery was planned as a combined procedure. During ovarian cyst removal, rupture of the dermoid cyst increased the risk of infection. Performing gallbladder surgery in the same sitting could have increased complications. Hence, the decision was made to defer cholecystectomy for patient safety. Such intraoperative decisions are based on risk assessment.
What complications can occur if a dermoid cyst ruptures during surgery?
Rupture can lead to the spillage of cyst contents into the abdominal cavity. This may cause chemical peritonitis or inflammation if not managed properly. Thorough washing of the abdomen is done to minimize this risk. Infection risk increases slightly in such cases. Close post-operative monitoring is therefore required.
Why was ICU observation needed after the surgery?
ICU or SICU monitoring ensures early detection of complications after major procedures. It helps in monitoring vital signs, fluid balance, and pain control. In cases with intraoperative challenges like cyst rupture, closer observation is preferred. Once stable, patients are shifted to the regular ward. This step improves overall safety and recovery outcomes.
Why was only cyst removal done instead of removing the entire ovary?
In young patients, saving the ovary is important to maintain normal hormone levels and future fertility. During surgery, doctors try to remove only the cyst (cystectomy) and keep as much healthy ovarian tissue as possible. Even if the cyst is large, careful separation techniques are used to protect the normal ovary. This helps reduce the chance of early hormonal imbalance in the body. It is a commonly followed approach in benign (non-cancerous) ovarian conditions whenever it can be safely done.
Why is histopathological examination (HPE) important after cyst removal?
HPE (Histopathological Examination) is done to confirm the exact type of cyst and to rule out cancer (malignancy). Although dermoid cysts are usually benign, in rare cases, they can show cancerous changes. Under the microscope, the tissue is studied in detail to give a final and definite diagnosis. The report also helps doctors decide if any further treatment is needed in case any abnormal findings are seen. Checking and reviewing the biopsy (HPE) report is an important part of follow-up care.
What lifestyle precautions are necessary after this type of surgery?
Avoiding heavy lifting and strenuous activities helps reduce pressure on the healing surgical area. A high-protein diet provides faster wound healing and overall recovery of the body. Maintaining good hygiene helps lower the risk of infection at the surgical site. Adequate rest is important, and normal daily activities should be restarted slowly as advised by the doctor. Regular follow-up visits are necessary to ensure proper healing and to detect any complications at an early stage.
When should immediate medical attention be sought after discharge?
Persistent abdominal pain, fever, or unusual swelling may be a sign of infection or other complications. Heavy menstrual bleeding can indicate hormonal imbalance or effects related to surgery. Signs of wound infection, such as redness, pain, swelling, or discharge, should be checked by a doctor without delay. Any sudden worsening of symptoms should not be ignored. Early medical review helps in identifying problems quickly and preventing serious complications.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868