Successful Open Bile Duct Excision with Roux-en-Y Hepaticojejunostomy for Choledochal Cyst
PACE Hospitals
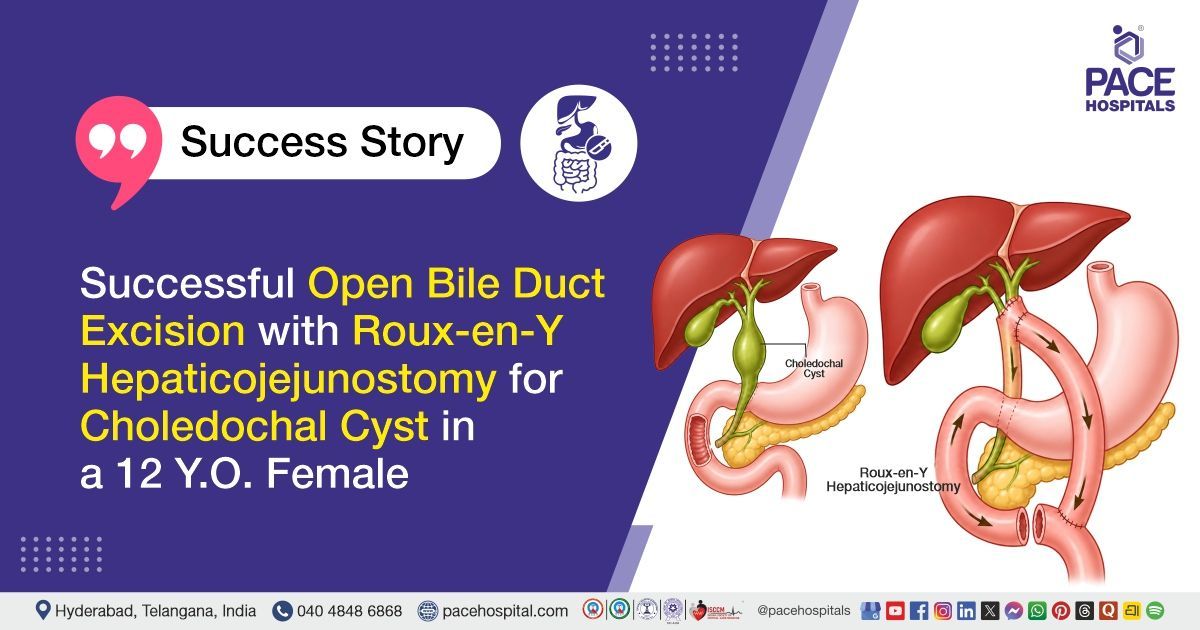
PACE Hospitals’ expert surgical gastroenterology team successfully performed an Open Extrahepatic Bile Duct Excision with Roux-en-Y Hepaticojejunostomy on a 12-year-old female patient diagnosed with Type 1 choledochal cyst, iron deficiency anemia, and primary hypothyroidism. The aim of the procedure was to remove the abnormal bile duct and prevent future complications such as infection or malignancy. It also aimed to restore effective bile drainage by creating a new connection between the liver and the small intestine.
Chief Complaints
A 12-year-old female patient with a body mass index (BMI) of 19 presented to the Surgical Gastroenterology Department at PACE Hospitals, Hitech City, Hyderabad, with complaints of intermittent abdominal pain in the right upper quadrant and epigastric region for the past four years. The last episode of pain occurred four days prior to admission. There was no history of fever, jaundice, right upper abdominal lump, altered bowel habits, or weight loss.
Past Medical History
The patient was a newly diagnosed case of primary hypothyroidism with no other known comorbidities and no history of prior abdominal surgery. There was a history of similar intermittent complaints over the past four years. The patient had a documented allergy to a cephalosporin-class antibiotic.
On Examination
On examination, the patient was conscious, alert, and well-oriented, with stable vital signs and no evidence of fever or respiratory distress. General physical examination revealed no pallor, icterus, lymphadenopathy, or edema. Per abdominal examination showed a soft, non-tender abdomen with no palpable masses or organomegaly, and no signs of guarding or rigidity; bowel sounds were normal. Other systemic examinations were unremarkable.
Diagnosis
Upon admission to PACE Hospitals, following the clinical assessment, the Surgical Gastroenterology team conducted a comprehensive evaluation based on the patient’s complaints of recurrent right upper quadrant and epigastric abdominal pain with a history of similar episodes over four years. A detailed medical history, physical examination, and preoperative assessment were performed to evaluate overall fitness for surgery and to identify associated comorbid conditions, including primary hypothyroidism and iron deficiency anemia.
Baseline investigations, including complete blood picture, renal function tests, liver function tests, serum electrolytes, coagulation profile, inflammatory markers, thyroid profile, iron studies, vitamin levels, viral screening, blood and urine cultures, chest X-ray, electrocardiography, ultrasonography of the abdomen and pelvis, computed tomography (CT) abdomen, magnetic resonance cholangiopancreatography (MRCP), and other relevant biochemical and imaging studies were carried out. Imaging revealed a Type I choledochal cyst with dilatation of the extrahepatic biliary tree, while other investigations were largely within acceptable limits for surgical intervention.
Based on the confirmed diagnosis, the patient was advised to undergo
Type 1 Choledochal Cyst Treatment in Hyderabad, India, under the expert care of the Surgical Gastroenterology Department.
Medical Decision Making (MDM)
After a detailed consultation with the surgical gastroenterologist Dr. CH. Madhusudhan, along with the Gastroenterology consultants Dr. Govind Verma, Dr. M Sudhir, and Dr. Padma Priya, and the Endocrinologist Dr. Tripti Sharma, a comprehensive clinical, biochemical, endocrinological, and radiological evaluation was carried out to determine the most appropriate management plan for the patient. Based on the patient’s history of chronic intermittent right upper quadrant and epigastric abdominal pain and imaging findings from USG abdomen, CECT abdomen, and MRCP showing dilatation of the extrahepatic biliary tree with smooth distal tapering, a diagnosis of Type I choledochal cyst was established. Associated iron deficiency anemia and primary hypothyroidism were also identified and medically optimized prior to surgery.
A detailed review of investigations, including complete blood picture, liver function tests, renal function tests, serum electrolytes, coagulation profile, iron studies, vitamin levels, thyroid profile, inflammatory markers, infection screening tests, cultures, and radiological imaging, was performed by the multidisciplinary team to assess surgical fitness and define disease extent. Based on the collective evaluation and multidisciplinary consensus, and considering the risk of recurrent biliary infection, pancreatitis, cholangitis, and long-term malignant transformation associated with choledochal cysts, surgical management was planned.
It was determined that open extrahepatic bile duct excision with Roux-en-Y hepaticojejunostomy was the most appropriate definitive treatment to remove the diseased biliary segment and restore normal biliary drainage. The patient was optimized preoperatively with correction of anemia, and supportive care.
The patient and her family members were counselled in detail regarding the diagnosis, surgical procedure, expected outcomes, and possible complications, including bile leak, anastomotic stricture, infection, and need for long-term follow-up, along with postoperative care instructions.
Surgical Procedure
Following the decision, the patient was scheduled to undergo Open Extrahepatic Bile duct excision with Roux-en-Y Hepaticojejunostomy in Hyderabad at PACE Hospitals under the expert care of the Surgical Gastroenterology Department.
The procedure involved the following steps:
- Surgical Access and Exposure: Right-sided subcostal (Kocher’s) incision was given. Abdomen was opened in layers and adequate exposure of the hepatobiliary region was achieved. Intraoperatively, dilated common bile duct (CBD), common hepatic duct (CHD), and cystic duct were identified.
- Bile Duct Dissection and Hilar Anatomy Identification: Circumferential dissection of the CBD was performed carefully. Hepatic arterial anatomy was delineated, including common hepatic artery (CHA), right hepatic artery (RHA), and left hepatic artery (LHA). It was noted that the RHA had an early origin from CHA and was coursing posterior to the CBD.
- Excision of Diseased Bile Duct: Distal CBD was dissected up to the pancreatic head, then divided, and the distal stump was securely sutured. The CBD was further dissected off the portal vein (PV) and RHA and divided near the hepatic hilum, completing extrahepatic bile duct excision.
- Reconstruction – Roux-en-Y Hepaticojejunostomy Formation: A Roux limb was created and brought in a retrocolic fashion through the transverse mesocolon. End-to-side hepaticojejunostomy was performed with posterior layer continuous suturing using PDS 5-0, and anterior layer interrupted suturing using PDS 5-0. Jejunojejunostomy was completed in two layers using outer 4-0 silk and inner 4-0 Vicryl.
- Completion, Hemostasis, and Closure: Mesenteric rent was closed, and meticulous hemostasis was achieved. The hepaticojejunostomy site was checked for leak using gauze. A Jackson-Pratt drain was placed, and the incision was closed in layers after confirming stability of the operative field.
Postoperative Care
During the postoperative period, the patient had an uneventful recovery after surgery. She was managed with intravenous fluids to maintain hydration, treatment to prevent postoperative infection, and acid suppression therapy to protect the stomach lining and support gastrointestinal healing. Supportive care included close monitoring of vital signs, adequate pain control, and maintenance of overall clinical stability.
The patient was closely observed for possible complications such as bile leakage, intra-abdominal fluid collection, and wound infection, with regular clinical assessment and imaging when required. A screening ultrasound confirmed satisfactory postoperative recovery, following which the drain was safely removed. Oral feeding was introduced gradually and advanced stepwise as tolerated until a normal diet was achieved. At discharge, she was stable, ambulatory, and advised regular follow-up along with proper wound care.
Discharge Medications
Upon discharge, the patient was advised a short course of treatment to prevent and manage postoperative infection and support recovery after surgery. Medications were given for the protection of the stomach and upper gastrointestinal tract, along with relief of post-surgical pain and discomfort. Ongoing therapy was continued to manage hypothyroidism and maintain hormonal balance. Additional supportive treatment was prescribed to promote bile flow and aid liver recovery following biliary reconstruction. Nutritional supplementation was also recommended to support wound healing and overall recovery, with clear instructions on regular intake and adherence.
Advice on Discharge
The patient was advised to follow an iron-rich diet to support correction of anemia and promote postoperative recovery. Discharge advice included proper wound care with maintenance of cleanliness and dryness of the surgical site, along with alternate-day dressing changes under aseptic precautions to ensure optimal healing and prevent infection.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms such as abdominal pain, fever, or vomiting.
Review and Follow-up Notes
The patient was advised to follow up with the Surgical Gastroenterologist in Hyderabad at PACE Hospitals, after 1 week, and to also review with the Gastroenterologist after 1 week for further evaluation and management.
Conclusion
This case highlights a Type I choledochal cyst in a pediatric patient presenting with chronic right upper abdominal pain, confirmed on imaging and managed surgically. The patient underwent successful open extrahepatic bile duct excision with Roux-en-Y hepaticojejunostomy without complications. Postoperative recovery was uneventful with clinical improvement, drain removal, and stable condition at discharge.
Surgical Management of Pediatric Biliary Tract Disorders
Pediatric biliary tract disorders are usually diagnosed using imaging tests like ultrasound and MRCP, which help identify bile duct abnormalities and obstruction. Treatment generally involves surgical removal of the affected bile duct followed by reconstruction to restore normal bile flow into the intestine. This reconstruction is commonly done using procedures such as Roux-en-Y hepaticojejunostomy under the care of a surgical gastroenterologist / surgical gastroenterology doctor.
The main goal of surgery is to eliminate the diseased segment and establish a safe, long-term pathway for bile drainage. After surgery, patients are closely monitored for complications such as infection, bile leakage, or fluid collection, along with careful assessment of recovery progress. Most patients show steady improvement with gradual return to normal diet and daily activities as tolerated. Proper postoperative care plays a key role in ensuring smooth healing and reducing risks. Long-term follow-up is essential to evaluate liver function, biliary drainage, and overall growth and health outcomes.
Frequently Asked Questions (FAQs)
Why was surgery required in Type 1 Choledochal Cyst treated with Roux-en-Y Hepaticojejunostomy?
In Type 1 choledochal cyst, the bile duct becomes abnormally dilated and cannot return to normal with medicines. This structural problem requires surgical correction. If left untreated, it may lead to repeated abdominal pain, infections, or blockage of bile flow. Over time, it can also affect liver function. Surgical removal of the cyst is considered the most effective and permanent treatment.
Why was bile duct removal necessary in this Type 1 Choledochal Cyst case?
The bile duct was removed as it had become abnormal and was not functioning properly. If such a diseased duct is left in place, it can continue to cause pain, infection, and other complications. Removing it helps eliminate the root cause of the problem completely. After removal, a new connection is made so that bile can flow from the liver into the intestine. This restores proper bile drainage, supports normal digestion, and helps prevent long-term harm to the liver.
Why was Roux-en-Y Hepaticojejunostomy performed after bile duct excision?
After removing the diseased bile duct, a new pathway is required for bile to reach the intestine. In Roux-en-Y hepaticojejunostomy, the bile ducts from the liver are directly joined to a part of the small intestine. This allows bile to flow normally again and helps in the proper digestion of food, especially fats. It also helps prevent future problems like blockage or backflow of bile. This is a well-established surgical method used to achieve safe and long-lasting results.
Why was open surgery preferred in this Type 1 Choledochal Cyst treatment?
Open surgery gives the surgeon a clear and direct view of important structures like the bile ducts and nearby blood vessels. In this case, careful and precise dissection was needed because of the complex anatomy. It allows the surgeon better control while performing the procedure step by step. This helps in protecting nearby organs from accidental injury. Because of this, open surgery is often chosen when accuracy and patient safety are the top priorities.
What complications were prevented by timely surgery in this case?
Timely surgical treatment helps prevent repeated infections and persistent abdominal pain. It reduces the risk of bile flow obstruction within the ducts. This helps protect the liver from long-term damage. It also lowers the chances of complications like pancreatitis. In some cases, it may reduce the long-term risk of bile duct cancer.
Why were multiple imaging tests used in diagnosing this case?
Different imaging tests give useful and complementary information about the condition. Ultrasound is usually the first test and helps identify any early changes or widening in the bile duct. A CT scan gives a more detailed view of the abdomen and helps assess nearby organs and any associated findings. MRCP (Magnetic Resonance Cholangiopancreatography) provides a clear and detailed image of the bile duct system and is very important for confirming the diagnosis. When all these tests are used together, they help doctors understand the problem accurately and plan the most appropriate surgical treatment.
How was recovery monitored after this surgery?
Recovery was assessed through regular monitoring of the patient’s condition and vital signs. Blood tests were performed to evaluate liver function and overall health. Imaging was used to rule out fluid collection or bile leakage. A surgical drain was placed and removed after confirming healing. Gradual return to a normal diet indicated good recovery.
Why was a drain placed after surgery in this case?
A surgical drain is placed after the operation to collect any fluid or bile that may build up in the surgical area. It also helps doctors quickly identify problems like a bile leak or fluid collection. This makes it possible to treat any complication early if needed. In this case, the drain was removed only after confirming that there was no leakage or abnormal fluid collection. It is a routine and important safety measure in such surgeries to ensure proper healing.
Why was hypothyroidism managed along with this surgical condition?
During evaluation, hypothyroidism was newly diagnosed in this patient. Thyroid hormones play an important role in metabolism and healing. If left untreated, it can delay recovery after surgery. Starting appropriate medication helps maintain normal body function. Managing both conditions supports better overall recovery.
What follow-up care is required after this surgery?
Regular follow-up is important to check bile drainage and liver function after surgery. Keeping the surgical wound clean and doing regular dressing changes helps reduce the risk of infection. If symptoms like fever, abdominal pain, vomiting, or yellowing of the eyes occur, they should be reported to the doctor immediately. A nutritious diet with iron-rich foods supports recovery and helps improve blood levels. Consistent follow-up visits ensure proper healing and long-term surgical success.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868