Upper Abdominal Pain: Causes, Symptoms & Warning Signs
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. Govind Verma - Senior Consultant Gastroenterologist & Hepatologist
Upper abdominal pain is a common health issue that affects people of all ages. The upper abdomen is located between the lower ribs and the belly button. It contains many important organs, including the stomach, liver, gallbladder, pancreas, spleen, and parts of the small intestine. Any kind of pain in this area can present in various ways, ranging from mild, persistent discomfort to sudden, severe pain that may indicate a medical emergency and require immediate attention.
Understanding the location, characteristics, and accompanying symptoms of upper abdominal pain is crucial for identifying potential causes and determining appropriate treatment. This comprehensive guide examines the various causes of upper abdominal pain, diagnostic methods, treatment approaches, and preventive measures to help you make informed decisions about your health.
Understanding Upper Abdominal Pain
Upper abdominal pain refers to discomfort occurring in the area between the lower edge of the rib cage and the umbilicus (belly button). Healthcare providers generally divide this region into sections to better find out the sources of pain:
- Upper right quadrant: Has liver, gallbladder, right kidney, parts of the small and large intestines, and the right side of the pancreas
- Upper left quadrant: Houses the stomach, spleen, left kidney, pancreas (left portion), and parts of the colon
- Epigastric region (central upper abdomen): Includes the stomach, duodenum (first part of small intestine), pancreas, and the lower esophagus
The nature of upper abdominal pain can be acute (sudden onset, typically severe) or chronic (persistent or recurring over weeks or months). The pain may present as sharp, dull, cramping, burning, or aching sensations, each potentially indicating different underlying conditions.
Upper Right Abdominal Pain
Common Causes of Upper Right Abdomen Pain
Gallbladder Disease
Gallbladder problems are among the most frequent causes of upper right abdominal pain. The gallbladder is a small pear-shaped organ that stores bile produced by the liver.
Gallstones (Cholelithiasis)
Gallstones are crystallised deposits of digestive fluid that can form in the gallbladder. When these stones obstruct the bile ducts, they cause intense pain.
Symptoms include:
- Sudden, severe pain in the upper right abdomen that may radiate to the backside or right shoulder blade
- Pain that intensifies after eating fatty meals
- Pain lasting from 30 minutes to several hours
- Nausea and vomiting
- Sweating
- Restlessness
Cholecystitis (Gallbladder Inflammation)
Cholecystitis occurs when the gallbladder becomes inflamed, which inflammation usually due to gallstones blocking the cystic duct. This is a medical emergency that requires timely treatment.
Warning signs include:
- Severe and constant pain in the upper right abdomen
- Fever and chills
- Tenderness when touching the abdomen
- Nausea and vomiting
- Pain that worsens with deep breathing
- Jaundice (yellowing of skin and eyes) in severe cases
Liver Conditions
Hepatitis
Hepatitis refers to liver inflammation, which can be caused by viral infections (hepatitis A, B, C), alcohol abuse, medications, or autoimmune conditions.
Symptoms include:
- Dull, aching pain in the upper right-sided abdomen
- Fatigue and weakness
- Jaundice
- Dark urine
- Pale or clay-colored stools
- Loss of appetite
- Nausea
Liver Abscess
A liver abscess is a pus-filled mass in the liver caused by bacterial or parasitic infection. It causes severe upper right abdominal pain along with high fever, chills, and general malaise.
Fatty Liver Disease
Fatty liver disease is a buildup of excessive fat in the liver cells. There are two types of fatty liver diseases non-alcoholic fatty liver disease (NAFLD) or alcohol-related fatty liver, which can cause mild to moderate discomfort in the upper right abdomen, though many people remain asymptomatic until the disease progresses.
Kidney Problems
Kidney Stones
When kidney stones develop in the right kidney or become lodged in the ureter, they cause severe upper right abdominal and flank pain.
Characteristics include:
- Intense, wave-like pain (renal colic)
- Pain radiating from the back to the front and down toward the groin
- Blood in urine (hematuria)
- Frequent urination with small amounts
- Nausea and vomiting
- Fever if infection is present
Kidney Infection (Pyelonephritis)
A kidney infection affecting the right kidney causes upper right abdominal pain, back pain, fever, chills, and urinary symptoms.
Other Conditions Affecting the Upper Right Abdomen
- Pneumonia: Right lower lobe pneumonia can cause referred pain to the upper right abdomen
- Peptic ulcer: Particularly duodenal ulcers may cause right-sided pain
- Hepatic flexure syndrome: Gas trapped in the bend of the colon under the liver
- Pancreatitis: Though typically central, can sometimes present with right-sided pain
- Appendicitis: In rare cases, appendicitis can cause upper abdominal pain before localizing to the lower right abdomen
Upper Left Abdominal Pain
Common Causes of Pain in the Upper Left Abdomen
Gastric (Stomach) Issues
Gastritis
Gastritis is the inflammation of the stomach lining caused by bacterial infection (H. pylori), excessive alcohol consumption, prolonged use of NSAIDs, or stress.
Symptoms include:
- Burning or gnawing sensation in the upper left abdomen
- Pain that may improve or worsen with eating food
- Nausea and vomiting
- Feeling of fullness after eating small amounts
- Loss of appetite
- Bloating and belching
Peptic Ulcer Disease
Peptic ulcer diseases are open sores that develop on the inner lining of the stomach (called gastric ulcers) or the upper part of the small intestine (duodenal ulcers). Gastric ulcers typically cause central epigastric burning pain.
Characteristic features include:
- Burning stomach pain that may be worse between meals or at night
- Pain that temporarily improves with food or antacids
- Bloating and belching
- Heartburn
- Nausea
- Dark or bloody stools (indicating bleeding ulcer)
- Unexplained weight loss
Splenic Conditions
The spleen, present in the upper left side of the abdomen, can cause pain when enlarged or injured.
Splenomegaly (Enlarged Spleen)
An enlarged spleen can result from infections (mononucleosis), liver disease, blood cancers, or inflammatory conditions.
Symptoms include:
- Dull ache or fullness in the upper left abdomen
- Feeling full quickly when eating
- Fatigue
- Easy bleeding or bruising
- Frequent infections
Splenic Infarction
A splenic infarction occurs when blood supply to the spleen is blocked, causing tissue death (necrosis). This causes sudden, severe upper left abdominal pain, often with fever.
Splenic Rupture
It is a medical emergency that involve involves a tear or break in the surface of the spleen, which is a life-threatening emergency. It causes severe upper left abdominal pain, dizziness, rapid heartbeat, and signs of shock.
Kidney Problems (Left Side)
Left kidney stones or kidney infections cause upper left abdominal pain similar to right-sided kidney problems, with pain radiating to the back and flank.
Pancreatic Issues
While pancreatitis typically causes central upper abdominal pain, it can sometimes be more pronounced on the left side, especially if the tail of the pancreas is primarily affected.
Additional Causes of Upper Left Abdominal Pain
- Costochondritis: It is a common, benign condition characterised by inflammation of the cartilage that connects a ribs to the breastbone, causing chest and upper abdominal pain
- Broken or bruised ribs: Trauma causing pain that worsens with breathing or movement
- Diverticulitis: Though more common in the lower left abdomen, can sometimes affect the upper colon
- Pericarditis: Inflammation of the heart's outer lining can cause left-sided chest and upper abdominal pain
- Irritable bowel syndrome (IBS): Can cause cramping in the upper left abdomen
Central Upper Abdominal Pain (Epigastric Pain)
Conditions Affecting the Central Upper Abdomen
Gastroesophageal Reflux Disease (GERD)
A chronic condition occurs when stomach acid commonly flows back into the esophagus, causing irritation.
Symptoms include:
- Burning sensation in the upper centre abdomen and chest (heartburn)
- Acid reflux or regurgitation
- Difficulty swallowing
- Chronic cough
- Sore throat or hoarseness
- Sensation of a lump in the throat
Pancreatitis
The pancreas, located behind the stomach, produces digestive enzymes and insulin. When inflamed, it causes significant upper central abdominal pain.
Acute Pancreatitis
Acute pancreatitis is sudden inflammation often caused by gallstones or excessive alcohol consumption.
Symptoms include:
- Severe, constant pain in the upper central abdomen that radiates to the back
- Pain that worsens after eating
- Nausea and vomiting
- Fever
- Rapid pulse
- Tender, swollen abdomen
Chronic Pancreatitis
Chronic pancreatitis is a progressive condition involves long-term inflammation causing permanent damage.
Features include:
- Persistent or recurring upper abdominal pain
- Unintentional weight loss
- Oily, foul-smelling stools (steatorrhea)
- Diabetes (if insulin-producing cells are damaged)
Hiatal Hernia
A hiatal hernia occurs when the upper portion of the stomach protrudes through the hiatus into the chest cavity, causing upper central abdominal discomfort, heartburn, and regurgitation.
Functional Dyspepsia (Indigestion)
Functional dyspepsia is chronic or recurrent pain in the upper central abdomen without an identifiable cause.
Symptoms include:
- Feeling of fullness during or after meals
- Uncomfortable stomach fullness after eating usual amounts
- Burning or pain in the upper abdomen
- Bloating and nausea
Heart-Related Pain (Referred Pain)
In certain cases, cardiovascular conditions like angina or myocardial infarction (heart attack) can present as upper abdominal pain rather than usual chest pain, especially in women, elderly individuals, and people suffering with diabetes.
Critical warning signs include:
- Pressure, squeezing, or pain in the upper abdomen or chest
- Pain radiating to jaw, neck, arms, or back
- Shortness of breath
- Nausea, lightheadedness, or cold sweats
Important: Any suspicion of cardiac symptoms requires immediate emergency evaluation.
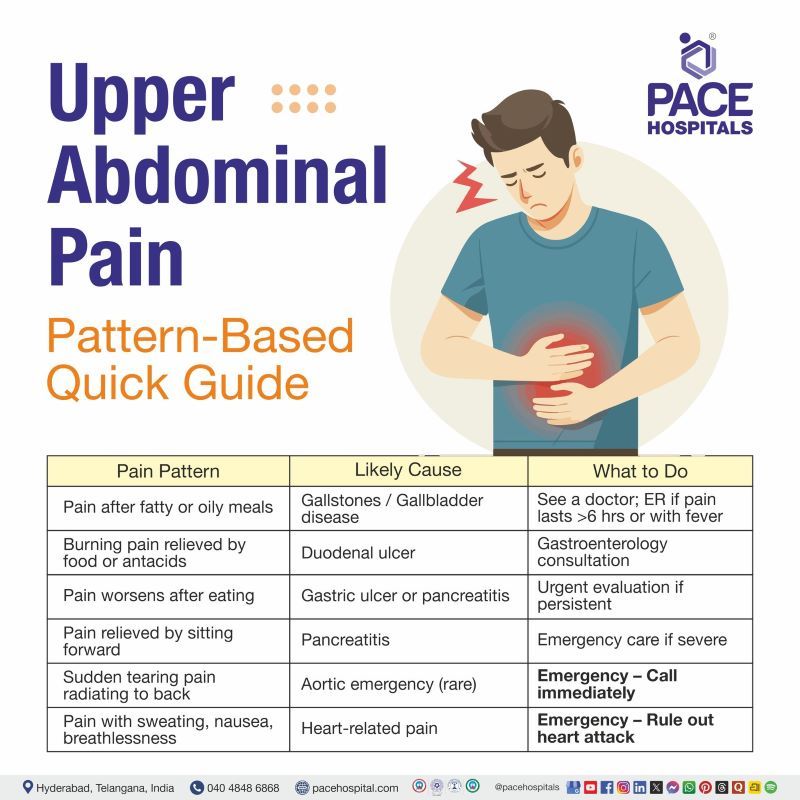
What the Pattern of Upper Abdominal Pain Can Indicate?
Upper Abdominal Pain – Pattern-Based Quick Guide
| Pain Pattern | Possible Cause | What to Do |
|---|---|---|
| Pain after fatty or oily meals | Gallstones / gallbladder disease | See a doctor; ER if pain lasts >6 hrs or with fever |
| Burning pain relieved by food or antacids | Duodenal ulcer | Gastroenterology consultation |
| Pain worsens after eating | Gastric ulcer or pancreatitis | Urgent evaluation if persistent |
| Pain relieved by sitting forward | Gastric ulcer or pancreatitis | Emergency care if severe |
| Sudden tearing pain radiating to back | Gastric ulcer or pancreatitis | Emergency – Call immediately |
| Pain with sweating, nausea, breathlessness | Heart-related pain | Emergency – Rule out heart attack |
PACE Hospitals offers 24/7 emergency care with advanced imaging, in-house specialists, and rapid diagnosis for abdominal and chest emergencies.
Note: This guide helps with early recognition, not diagnosis. Severe or unusual pain or discomfort always requires medical attention.
How Pain Patterns Can Help Identify Upper Abdominal Conditions?
Upper abdominal pain patterns can helps to point toward specific causes. Pain after fatty meals commonly suggests gallbladder disease. Burning pain that improves with food indicates a duodenal ulcer, whereas pain that gets worsens after eating gives hints for gastric ulcer or pancreatitis. Chronic pain that relieves by leaning forward is typical of pancreatitis. Sudden tearing pain radiating to the back is rare but may indicate a life-threatening aortic condition and requires immediate emergency care.
Upper Abdominal Pain by Age and Risk Factors
Upper abdominal pain can mean different things depending on your age and health background. While many causes are harmless, certain groups have a higher risk of serious conditions—so the same symptom deserves different urgency.
Children & Adolescents
In younger people, upper abdominal pain is often related to temporary digestive irritation or infections, but trauma should never be ignored.
Common causes
- Gastritis / indigestion (spicy food, irregular meals)
- Viral gastroenteritis or stomach infection
- Constipation or gas
- Injury/trauma from sports or falls (rib or abdominal injury)
When to worry
- Severe pain after a fall or hit to the abdomen
- Persistent vomiting, dehydration, or high fever
- Pain with severe weakness, fainting, or blood in vomit/stool
Adults (30–50 years)
This age group commonly experiences lifestyle- and diet-related upper abdominal pain, especially from acid reflux and gallbladder issues.
Common causes
- Gallstones / gallbladder attacks (often after fatty meals)
- GERD (acid reflux) and gastritis
- Fatty liver diseases (commonly linked with obesity, diabetes, high cholesterol)
- Peptic ulcers disease (including H. pylori or NSAID-related gastric inflammation)
When to worry
- Continuous right-sided pain in the upper abdomen part with vomit like feeling after meals (possible gallbladder disease)
- Unexplained weight loss, black stools, or persistent pain beyond a few days
- Jaundice (yellow eyes/skin) or dark urine
Elderly (>60 years)
In older adults, upper abdominal pain is more likely to be linked to serious conditions, and symptoms can be “atypical” (less obvious).
Common causes
- Heart-related pain presenting as upper abdominal discomfort (especially “burning” or pressure)
- Pancreatic and bile duct disorders
- Reduced blood supply to the gut (ischemia) in those with vascular disease
- Medication-related gastritis/ulcers (NSAIDs, blood thinners)
When to worry (urgent evaluation)?
- Upper abdominal pain with sweating, breathlessness, weakness, or dizziness
- New pain that is severe, persistent, or wakes you up from sleep
- Persistent vomiting, black stools, or sudden severe tenderness
Diabetics & Smokers (High-Risk Group)
Diabetes and smoking increase the risk of severe digestive and cardiac causes of pain—and symptoms may be less “typical,” delaying diagnosis.
Common causes
- Atypical heart attack/angina (may feel like indigestion or upper abdominal pressure)
- Pancreatitis (higher risk with alcohol use, high triglycerides, gallstones)
- GERD and gastroparesis (delayed stomach emptying) in long-term diabetes
- Peptic ulcers disease and its complications, more in smokers
When to worry (don’t self-treat)?
- “Indigestion-like” pain with sweating, nausea, fatigue, or breathlessness
- Pain radiating to the back with vomiting (possible pancreatitis)
- Persistent symptoms despite antacids or home care
Note: If you’re over 60, diabetic, or a smoker, and you develop new upper abdominal pain get evaluated early, even if symptoms seem mild.

When to Seek Medical Attention for Upper Abdominal Pain?
While some upper abdomen pain resolves with rest or over-the-counter medications. However, certain symptoms may indicate serious conditions, that requires urgent medical care.
Emergency Warning Signs
Call the PACE Hospitals emergency ambulance service, or go to the emergency room immediately, if you experience the following symptoms:
- Severe, sudden abdominal pain: Especially if it's unbearable or unlike anything you've experienced
- Chest pain or pressure: With or without abdominal pain, particularly if radiating to arm, jaw, or back
- Difficulty breathing or shortness of breath: Accompanying abdominal pain
- Vomiting blood: Or vomit that appears black or like coffee grounds
- Black, tarry, or bloody stools: This indicates gastrointestinal (GI) bleeding
- Rigid, board-like abdomen: Severe tenderness or inability to touch the abdomen
- High fever: Body temperature above 101°F (38.3°C) with abdominal pain
- Yellowing of skin or eyes (jaundice): Indicating liver or bile duct problems
- Severe pain after abdominal injury: Such as car accident or fall
- Signs of shock: Rapid pulse, sweating, confusion, pale skin, dizziness
- Pregnancy with abdominal pain: Any abdominal pain during pregnancy requires evaluation
- Continuous vomiting: Inability to keep food or liquids down for more than 12 ho
When to Schedule a Doctor’s Appointment for Upper Abdominal Pain?
Contact your healthcare provider within a day or two if you have:
- Upper abdominal pain lasting more than a few days
- Pain that progressively worsens
- Recurring pain that comes and goes
- Unexplained weight loss
- Loss of appetite persisting for several days
- Persistent nausea or changes in bowel habits
- Pain that awakens you from sleep
- Pain worsening after eating
- Dark urine or pale stools
- Persistent bloating or feeling of fullness
If you have recurring or chronic upper abdominal pain, consulting a gastroenterologist or physician early can help prevent complications. At PACE Hospitals, patients are looked after by a multidisciplinary team. Gastroenterologists focus on digestive problems, hepatologists manage liver and bile duct conditions, GI surgeons treat gallbladder disease and surgical problems, urologists evaluates kidney-related causes, and cardiologists are consulted when heart-related concerns need to be find out. Care is supported by advanced diagnostic facilities and 24/7 emergency services.
What Not to Ignore with Upper Abdominal Pain?
Do not ignore upper abdominal pain associated with fever, jaundice, chest discomfort, back radiation, or persistent vomiting—these may indicate serious or life-threatening conditions.
Upper Abdominal Pain – What Should You Do Now?
Home care if:
- Mild pain
- Improves with antacids
- No fever, vomiting, or jaundice
See a doctor within 24–48 hrs if:
- Pain persists or recurs
- Pain after meals
- Unexplained weight loss
Go to the Emergency Room immediately if:
- Severe or sudden pain
- Chest pain, breathlessness
- Vomiting blood, black stools
- Jaundice with pain
Diagnosis of Upper Abdominal Pain?
Accurate diagnosis of upper abdominal pain involves a comprehensive approach combining clinical evaluation, laboratory tests, and imaging studies.
Medical History and Physical Examination
Your doctor will gather detailed informations, which include:
Pain Characteristics
- Exact location and radiation pattern
- Onset (sudden vs. gradual)
- Duration and frequency
- Quality (burning, sharp, dull, cramping)
- Severity on a scale of 1-10
- Factors that worsen or relieve pain (eating, position, medications)
Associated Symptoms
- Nausea, vomiting, or changes in appetite
- Fever or chills
- Changes in bowel habits or urine
- Weight changes
- Jaundice or dark urine
Medical and Lifestyle History
- Previous abdominal surgeries or medical conditions
- Medications and supplements
- Alcohol consumption and smoking habits
- Recent travel or dietary changes
- Family history of digestive diseases
Physical Examination
- Your doctor will:
- Palpate (press on) various areas of the abdomen to identify tenderness, masses, or organ enlargement
- Listen to bowel sounds with a stethoscope
- Check for jaundice, pallor, or other visible signs
- Assess for signs of peritonitis (inflammation of abdominal lining)
- Perform specialized tests like Murphy's sign (for gallbladder disease)
Laboratory Tests
Blood Tests
- Complete blood count (CBC): Helps to detect infection, anemia, or blood disorders
- Liver function tests: To evaluate liver health condition and bile duct function
- Pancreatic enzymes (like amylase, lipase): Diagnose pancreatitis
- Kidney function tests: To assess kidney health condition
- Cardiac enzymes (troponin): Used to confirm or rule out a heart attack when symptoms suggest
- C-reactive protein (CRP): Indicates the presence and level of inflammation in the body
Urine Tests
- Urinalysis: Detects urinary tract infections or kidney stones
- Urine culture: Identifies specific bacteria causing infection
Stool Tests
- Fecal occult blood test: Checks for hidden blood
- Stool culture: Identifies infections
- H. pylori testing: Detects bacteria causing ulcers
Imaging Studies
- First-line imaging performed to detect gallbladder disease, liver conditions, and kidney problems
- Non-invasive and radiation-free
- Excellent for detecting gallstones, bile duct obstruction, and organ enlargement
- Provides detailed cross-sectional images of abdominal organs
- Excellent for diagnosing pancreatitis, kidney stones, abscesses, and tumors
- Can identify complications like perforation or bleeding
MRI Scan (Magnetic Resonance Imaging)
- Provide superior soft tissue detail
- MRCP (magnetic resonance cholangiopancreatography) specifically visualizes bile and pancreatic ducts
- Used when detailed imaging of liver, pancreas, or bile ducts is needed
X-rays
- Can detect intestinal obstruction, perforation, or kidney stones
- Less detailed than CT or MRI but easily available and fast
HIDA Scan (Hepatobiliary Iminodiacetic Acid Scan)
- Nuclear medicine test specifically for gallbladder function
- Evaluates bile flow and gallbladder emptying
Specialized Procedures
- Upper Endoscopy (EGD - Esophagogastroduodenoscopy)
- Direct visualization of esophagus, stomach, and duodenum using a flexible camera
- Allows biopsy of suspicious areas
- Can diagnose ulcers, gastritis, esophagitis, and tumors
- Can provide therapeutic intervention (stop bleeding, remove polyps)
ERCP (Endoscopic Retrograde Cholangiopancreatography)
- Combines endoscopy and X-ray to examine bile ducts and pancreatic ducts
- Can remove gallstones from bile ducts
- Can place stents to relieve obstruction
Laparoscopy
- Minimally invasive surgery to directly visualize abdominal organs
- Used when diagnosis remains unclear after other tests
- Can be both diagnostic and therapeutic
Treatment Options for Upper Abdominal Pain
Treatment for upper abdominal pain depends entirely on the underlying cause, intensity of symptoms, and individual patient factors.
Medical Treatments
Medications
For Acid-Related Conditions (GERD, Ulcers, Gastritis)
- Proton pump inhibitors (PPIs): Indicated for the treatment and management of acid-related gastrointestinal disorders
- H2 blockers: Indicated for the short-term relief and prevention of heartburn and the treatment of mild to moderate acid-related conditions
- Antacids: For quick relief of heartburn
- Antibiotics: For H. pylori eradication (typically triple or quadruple therapy)
- Protective agents: Gastrointestinal agent forms a protective barrier over the gastric lining to promote healing and reduce irritation
For Gallbladder Disease
- Pain medications: NSAIDs or opioids for gallstone attacks
- Antibiotics: For cholecystitis or infection
- Hepatoprotective agent: May dissolve certain types of gallstones (limited use)
For Pancreatitis
- Pain management: Ranges from NSAIDs to opioid analgesic, depending on severity
- Pancreatic enzyme supplements: For chronic pancreatitis
- Insulin: If diabetes develops
For Liver Conditions
- Antiviral medications: For hepatitis B or C
- Corticosteroids or immunosuppressants: For autoimmune hepatitis
- Specific treatments for fatty liver: Weight loss, diabetes management
For Kidney Stones
- Pain relievers: NSAIDs
- Alpha-blockers: Help stones pass more easily
- Medications to prevent future stones: Depending on stone type
Surgical Interventions
- Cholecystectomy (Gallbladder Removal)
- Laparoscopic surgery is the standard approach for gallstone disease
- Usually, outpatient or overnight hospital stay
- High success rate with low complication rates
Procedures for Kidney Stones
- Extracorporeal shock wave lithotripsy (ESWL): Uses sound waves to break up stones
- Ureteroscopy: Removes or breaks up stones using a scope
- Percutaneous nephrolithotomy: For large kidney stones
Surgery for Peptic Ulcer Complications
- Required for perforation, obstruction, or uncontrolled bleeding
- May involve patching perforation or removing part of stomach
Pancreatic Surgery
- Necrosectomy: Surgical removal of necrotic pancreatic tissue
- Drainage procedures: For pancreatic pseudocysts
- Whipple procedures (pancreaticoduodenectomy): This is indicated for pancreatic cancer
Splenectomy
- Removal of spleen for rupture, severe enlargement, or certain blood disorders
Home Remedies and Self-Care
For mild, non-emergency upper abdominal pain:
Dietary Modifications
- Eat smaller and more frequent meals rather than eating large portion
- Avoid trigger foods (spicy, fatty, acidic foods)
- Limit caffeine, alcohol, and carbonated beverages
- Don't eat within 2-3 hours of bedtime (for GERD)
- Stay hydrated with water
- Follow a bland diet if experiencing gastritis or ulcer symptoms
Lifestyle Adjustments
- Maintain a healthy body mass index (BMI)
- Elevate the head of the bed by 6–8 inches to reduce nighttime reflux symptoms in GERD.
- Don't lie down immediately after eating
- Wear loose-fitting clothing around the abdomen
- Quit smoking
- Limit alcohol consumption
Over-the-Counter Remedies
- Antacids: Calcium carbonate, magnesium hydroxide for heartburn
- Anti-gas medications: Simethicone for bloating and gas
- H2 blockers: Available over-the-counter for acid reduction
Heat and Rest
- Apply heating pad to the painful area (not for acute, severe pain)
- Rest and avoid strenuous activity
- Practice stress-reduction techniques
When to Avoid Self-Treatment?
- Never self-treat severe or persistent pain
- Don't mask symptoms of serious conditions
- Consult a doctor if symptoms does not improve within a few days
Prevention Strategies for Upper Abdominal Pain
Although not all causes of upper abdomen pain are preventable, many can be reduced through healthy lifestyle changes and preventive steps.
For Digestive Health
Dietary Recommendations
- Follow a balanced diet, like fruits, vegetables, and whole grains
- Limit fatty, fried, and processed foods
- Reduce portion sizes to avoid overeating
- Identify and avoid personal trigger foods
- Limit spicy foods if they cause discomfort
- Reduce caffeine and alcohol intake
- Stay hydrated throughout the day
Eating Behaviors
- Eat slowly and chew food thoroughly
- Avoid eating large meals before bedtime
- Maintain regular mealtimes
- Don't skip meals, especially breakfast
For Gallbladder Health
- Maintain a healthy body weight through gradual weight loss (if needed)
- Avoid rapid weight loss or crash dieting
- Maintaining regular meals with moderate fat content
- Include healthy fats from fish, nuts, and olive oil
- Stay physically active
For Liver Health
- Limit alcohol consumption (not more than moderate levels)
- Maintain a healthy weight
- Exercise regularly
- Get vaccinated for hepatitis A and B
- Use medications as prescribed and avoid excessive analgesic and antipyretic drugs
- Avoid sharing infected needles or personal items that may have blood on them
- Practice safe sexual activities to prevent hepatitis transmission
For Kidney Health
- Drink plenty of water (8-10 glasses daily)
- Limit sodium intake
- Reduce animal protein consumption
- Limit foods high in oxalates (spinach, nuts, chocolate) if prone to calcium oxalate stones
- Maintain a healthy weight
- Manage blood pressure and blood sugar
For Acid-Related Conditions
- Avoid lying down for at least 2–3 hours after meals to reduce reflux and improve digestion.
- Elevate the head of your bed
- Maintain a healthy weight
- Quit smoking
- Identify and avoid trigger foods
- Manage stress effectively
- Limit use of NSAIDs
General Health Measures
Exercise regularly (at least for 150 minutes of moderate activity weekly)
Don't smoke or use tobacco products
Managing stress through relaxation techniques
Get adequate sleep (7-9 hours nightly)
Attend regular health check-ups
Take medications as prescribed
Practice good hygiene to prevent infections
Frequently Asked Questions (FAQs) on Upper Abdominal Pain
What are the most common causes of upper abdominal pain?
The most common causes of upper abdominal pain include acid reflux (GERD), gastritis, peptic ulcers, gallstones, indigestion, and muscle strain. Other frequent causes include pancreatitis, hepatitis, kidney stones, and irritable bowel syndrome. The specific location of pain helps narrow down the cause—upper right pain often indicates gallbladder or liver issues, upper left pain suggests stomach or spleen problems, and central upper pain typically points to stomach, pancreas, or esophageal conditions.
When should I go to the emergency room (ER) for upper abdominal pain?
You should seek immediate medical attention if upper abdominal pain is sudden, severe, or worsening, or if it occurs along with any of the following symptoms: chest pain or pressure that spreads to the arm, neck, or jaw; shortness of breath; vomiting blood or material that looks like coffee grounds; black or bloody stools; a hard or rigid abdomen; a high fever (above 101°F); yellowing of the skin or eyes (jaundice); severe pain following an injury; signs of shock such as a rapid heartbeat, confusion, or pale, clammy skin; or abdominal pain during pregnancy. These warning signs may point to serious or life-threatening conditions that require urgent diagnosis and treatment.
What does upper right abdominal pain indicate?
Pain in the upper right abdominal area is most often related to gallbladder problems (gallstones or cholecystitis), liver conditions (hepatitis, fatty liver, liver abscess), or right kidney issues (stones or infection). The pain characteristics help distinguish causes—sharp, severe pain after fatty meals suggests gallstones, while dull, constant pain with jaundice may indicate hepatitis. Less common causes include pneumonia, peptic ulcers, or pancreatitis. Sudden, severe upper right pain, especially with fever, requires prompt medical evaluation.
Can stress cause upper abdominal pain?
Yes. Stress is a significant contributor to upper abdominal pain. Stress can cause or worsen gastritis, peptic ulcers, functional dyspepsia, and irritable bowel syndrome through the gut-brain connection. Stress increases stomach acid production disrupts normal digestive processes and can cause muscle tension in the abdominal wall. Chronic stress also weakens the immune system and may lead to unhealthy coping behaviours like excessive alcohol use or poor dietary choices, further contributing to digestive problems.
What causes upper left abdominal pain after eating?
Upper left abdominal pain after eating results from gastritis, peptic ulcers (gastric ulcers specifically), or functional dyspepsia. The stomach is in the upper left quadrant, and inflammation or ulcers can cause pain when acidic gastric contents come into contact with the damaged lining during digestion. Other causes may such as pancreatitis (pain worsens after eating), splenic flexure syndrome (gas trapped in the colon), food intolerances, or overeating. If pain consistently occurs after meals, keep a food diary and consult a experienced gastroenterologist.
What helps relieve upper abdominal pain at home?
Mild upper abdominal pain, try these remedies: take over-the-counter antacid medications for acid-related pain, apply an heating pad (non-acute pain), eat small portion (usually bland meals), avoid trigger foods (too much oily, spicy, acidic, processed items), stay upright after eating, drink herbal tea, practice relaxation techniques, and rest. However, severe, sudden, or persistent pain should not be self-treated. If pain doesn't improve within 24-48 hours, worsens, or is accompanied by fever, vomiting, or other concerning symptoms, consult a healthcare provider.
Is upper abdominal pain a symptom of pancreatic cancer?
Upper abdominal pain can be a symptom of pancreatic cancer, though it's not specific to cancer and more commonly indicates other conditions. Pancreatic cancer pain is typically located in the upper central abdomen and often radiates to the back. Other concerning symptoms include unexplained weight loss, new-onset diabetes, jaundice, loss of appetite, and pale stools. However, pancreatic cancer often has no symptoms in early stages. Risk increases with age (over 65), smoking, obesity, chronic pancreatitis, and family history. Persistent upper abdominal pain with these features warrants medical evaluation.
How do I know if my upper abdominal pain is serious?
Upper abdomen discomfort can be severe if it is recurring and sudden, develops gradually, lasts for several days, or is accompanied by warning indications such as fever, vomiting blood, blood in stools, yellowing of skin and eyes, chest pain, breathlessness, or shock-like symptoms. Pain that interferes with daily activities, causes you to sleep, or feels different from past bouts demands evaluation. Trust your instincts—if pain feels unusually severe or you're concerned, seek medical attention. It's better to be evaluated and reassured than to delay treatment for a serious condition.
What is the difference between heartburn and a heart attack?
Heartburn causes burning-like pain in the upper central part of the abdomen and chest due to acid reflux, which worsens after eating or lying down and improves with antacids. Heart attack pain is usually described as pressure, squeezing, or heaviness in the chest that may radiate to the arms, jaw, neck, or back, associated with shortness of breath, sweating, nausea, or light-headedness. However, symptoms can overlap, especially in women, elderly, or diabetics. ANY suspicion of cardiac symptoms requires immediate emergency evaluation—don't assume it's just heartburn.
Can gallbladder pain go away on its own?
Gallbladder pain from a gallstone attack can subside on its own if the stone moves away from the duct opening, typically within a few hours. However, this does not mean that the problem has been cured; stones remain, and attacks often recur, potentially resulting in complications such as pancreatitis, cholecystitis, or bile duct obstruction. If you've experienced gallbladder pain, consult a doctor even if it has resolved. Cholecystectomy (gallbladder removal) is usually suggested to prevent any kind of future attacks and complications. Persistent pain beyond 5-6 hours requires emergency evaluation.
What does pancreatitis pain feel like?
Pancreatitis can cause intense, continuous pain in the upper central abdomen that radiates to the back, which is sometimes referred to as "band-like" pain. The pain usually starts suddenly, intensifies quickly, and lasts for hours or days. It characteristically worsens after eating, especially fatty foods, and may be slightly relieved by sitting up and leaning forward. Accompanying symptoms include nausea, vomiting, fever, rapid pulse, and abdominal tenderness. Acute pancreatitis is a medical emergency requiring hospitalization for pain management and supportive care.
Can kidney (renal) stones cause upper abdominal pain?
Yes, kidney stones can cause upper abdominal pain, particularly in the upper back and flank regions that may radiate to the upper abdomen. The pain location depends on where the stone is located. Stones in the kidney or upper ureter cause upper abdominal and flank pain, while stones moving down the ureter cause pain that radiates downward. The pain is typically severe and wave-like (renal colic), associated with nausea, vomiting, blood in urine, and urinary urgency.
Why does pain in the upper abdomen sometimes spread to the back?
Upper abdominal pain that radiates to the backside is commonly associated with pancreatic disorders. This pattern happens because the pancreas lies deep within the abdomen and near the back, which allows inflammation or disease to cause referred pain in that area. Other causes of radiating pain include gallbladder disease (pain to right shoulder blade and back), kidney problems (flank and back pain), peptic ulcers (occasionally back pain), and aortic aneurysm. Back-radiating abdominal pain, especially if severe or persistent, requires medical evaluation.
Can upper abdominal pain be caused by anxiety?
Yes. Anxiety can lead to or even worsen upper abdominal pain through various ways. Anxiety triggers stress response, which increases stomach acid production, disrupting normal digestive processes, and causing muscle tension in the abdominal wall. It can trigger or exacerbate functional dyspepsia, irritable bowel syndrome, and gastritis. Anxiety may also increase awareness and sensitivity to normal digestive sensations. However, never attribute all abdominal pain to anxiety without medical evaluation—physical causes must be ruled out first, especially for new or severe symptoms.
How long should upper abdominal pain last before be seeing a doctor?
See a doctor or physician if upper abdominal pain lasts more than 2-3 days without improvement, even if mild. Seek same-day or next-day evaluation if pain is moderate to severe, progressively worsening, or interfering with normal activities. Emergency evaluation is needed for severe, sudden pain; pain with fever, vomiting blood, or bloody stools; chest pain or breathing difficulty; or jaundice. For chronic, recurring pain (even if mild), schedule an appointment to identify and address the underlying cause. Don't delay evaluation, hoping pain will resolve—early diagnosis often leads to simpler, more effective treatment.
Medical Disclaimer: This article is for information only and does not provide medical advice. Always consult with a qualified physician or doctor for appropriate diagnostic evaluation and treatment for any medical issue. If you have severe or ongoing abdominal pain, get medical help right away.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868