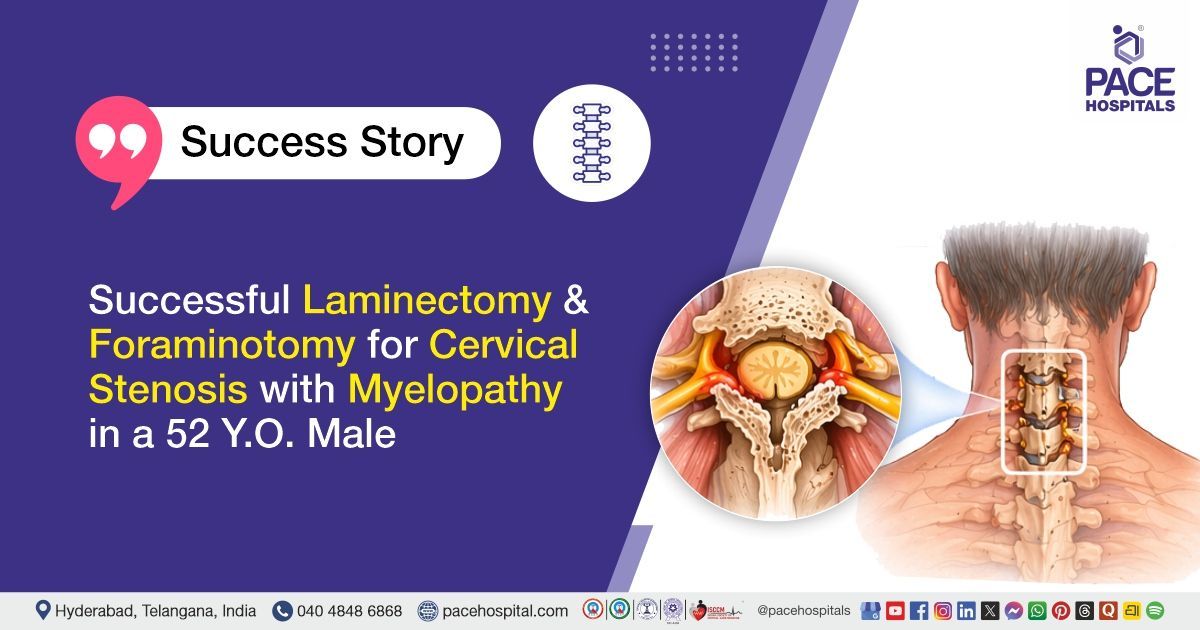
Successful Laminectomy and Foraminotomy for Cervical Stenosis with Myelopathy in a 52 Y.O. Male
PACE Hospitals
PACE Hospitals’ expert Neurosurgery team successfully performed a C4–C6 Cervical Spine Posterior Stabilization along with C5–C6 Laminectomy and Foraminotomy on a 52-year-old male patient diagnosed with cervical canal stenosis with compressive myelopathy at the C5–C6 level, with the aim of decompressing the spinal cord and nerve roots, relieving pressure caused by canal narrowing, restoring spinal stability, improving neurological function, and preventing further progression of the condition.
Chief Complaints
A 52-year-old male patient with a body mass index (BMI) of 21 presented to the Neurosurgery Department at PACE Hospitals, Hitech City, Hyderabad, with complaints of bilateral lower limb and left upper limb weakness for the past two years, along with neck pain and paresthesias (tingling) in the left upper limb for six months.
The symptoms were insidious (gradual) in onset and gradually progressive. The patient had a history of lifting heavy weights on the head and neck for 15–20 years. He also reported neurogenic claudication (nerve-related walking pain) and a swelling over the nape of the neck present for the past 10–15 years. There were no associated urinary complaints.
Past Medical History
The patient was a known case of hypertension and type 2 diabetes mellitus and had been on regular medications for the same. There was no documented history of prior neurological disorders, spinal surgeries, or any other significant chronic illnesses.
On Examination
On general examination, the patient was conscious, coherent, and oriented, and was moderately built and nourished with stable vital signs. Cardiovascular and respiratory system examinations were normal, with normal heart sounds and bilateral air entry present. Per abdominal examination was soft and non-tender. Local examination revealed a soft, non-tender, mobile swelling over the nape of the neck with slipping of skin present.
Neurological examination showed reduced motor power in all four limbs with increased tone. Deep tendon reflexes were exaggerated, and plantar reflexes were extensor bilaterally, suggestive of upper motor neuron involvement. Cranial nerve examination was normal, with no cerebellar signs or meningeal irritation.
Diagnosis
Upon admission to PACE hospitals, the patient underwent a comprehensive clinical evaluation, along with a detailed medical history and diagnostic assessment by the Neurosurgery team.
Laboratory investigations were conducted as part of the preoperative workup. Complete blood count (CBC) revealed normal hemoglobin, RBC, and platelet counts with evidence of mild leukocytosis. Renal function tests, including blood urea and serum creatinine, were within normal limits. Serum electrolytes showed mild hyponatremia, while potassium and chloride levels were within normal range. Autoimmune screening with an ANA profile was negative. Cardiac evaluation with NT-proBNP was within normal limits.
Neuroimaging investigations, including Magnetic Resonance Imaging (MRI) of the cervical spine, demonstrated multilevel spondylotic changes with disc osteophyte complexes, most pronounced at the C5–C6 level, causing severe spinal canal stenosis with compressive myelopathy. Additional findings included neural foraminal narrowing and lateral recess stenosis at multiple levels.
Based on the confirmed diagnosis, the patient was advised to undergo Compressive Myelopathy with Cervical Canal Stenosis Treatment in Hyderabad, India, under the expert care of the Neurosurgery Department.
Medical Decision-Making (MDM)
After a detailed evaluation by Dr. U.L. Sandeep Varma, Consultant Neurosurgeon, along with cross consultations from Dr. Govind Verma, Gastroenterologist, for preoperative medical and gastrointestinal evaluation and Dr. Seshi Vardhan Janjirala, Cardiologist, for preoperative cardiac risk assessment and optimization. The patient was diagnosed with cervical canal stenosis with compressive myelopathy at the C5–C6 level.
The patient presented with progressive neurological deficits, including quadriparesis with upper motor neuron signs, and MRI findings confirmed severe spinal canal stenosis with cord compression at C5–C6, along with multilevel cervical spondylotic changes. Considering the severity of cord compression, progressive symptomatology, and risk of further neurological deterioration, surgical intervention was deemed necessary as conservative management would not be sufficient.
It was determined that C4–C6 posterior cervical spine stabilization along with C5–C6 laminectomy and foraminotomy was identified as the most appropriate surgical intervention to achieve adequate spinal cord decompression, nerve root decompression, and stabilization of the cervical spine, thereby preventing further neurological decline.
The patient and his family members were counselled in detail regarding the diagnosis, multidisciplinary evaluation, need for surgical management, severity of the condition, potential risks and benefits, expected postoperative recovery, rehabilitation plan, medication adherence, and the importance of regular follow-up for optimal functional outcome.
Surgical Procedure
Following the decision, the patient was scheduled to undergo a C4–C6 Posterior Cervical Spine Stabilization with C5–C6 Laminectomy surgery in Hyderabad at PACE Hospitals, along with Foraminotomy under the expert supervision of the Neurosurgery team.
The procedure involved the following steps:
- Patient Positioning and Exposure: Under strict aseptic precautions and general anaesthesia, the patient was placed in the prone position. The operative field was painted and draped in a sterile manner. A vertical midline incision was given over the posterior cervical spine, and dissection was carried down through the subcutaneous tissue to expose the posterior elements.
- Muscle Dissection and Level Exposure: Paraspinal muscles were carefully separated and retracted to expose the C4 to C6 vertebral lamina and lateral masses. Adequate exposure of the surgical field was achieved for decompression and stabilization.
- Decompression Procedure (Laminectomy and Foraminotomy): A C5 and C6 laminectomy was performed to decompress the spinal canal and relieve spinal cord compression. Left-sided foraminotomy was also done to decompress the exiting nerve root and relieve foraminal stenosis.
- Instrumentation and Stabilization: C4 to C6 lateral mass fixation was performed using appropriate screws and rods. Stabilization of the cervical spine was achieved using posterior instrumentation (Jayon lateral mass screws 3.5 × 16 mm, rods, and connectors).
- Bone Grafting and Wound Closure: Posterolateral fusion was performed using autologous bone graft to promote spinal fusion. Hemostasis was secured, and a drain was placed. The wound was closed in layers in a standard fashion. The dura was noted to be pulsatile at the end of the procedure, indicating adequate decompression.
Postoperative Care
Postoperatively, the patient was shifted to the Intensive Care Unit (ICU) for overnight monitoring to ensure hemodynamic stability and early detection of neurological or surgical complications following cervical spine decompression and stabilization. During the hospital stay, appropriate medications were administered for postoperative pain control, infection prevention, gastric protection, neuropathic symptom control, and management of comorbid conditions as required.
Neurological status, vital parameters, and wound condition were closely observed, and the patient remained stable. The surgical drain and urinary catheter were removed on postoperative day 2 after satisfactory recovery, and the patient was gradually mobilized with assistance. He was subsequently planned for discharge after achieving stable recovery and adequate functional improvement.
Discharge Medications
Upon discharge, the patient was prescribed medications for prevention of postoperative wound infection, control of neuropathic pain, relief of musculoskeletal pain and inflammation, gastric acid suppression for gastrointestinal protection, nutritional and neuroregenerative support, and management of pre-existing hypertension and diabetes mellitus. He was advised to continue long-term therapy for blood pressure control and glycemic control as per ongoing requirements, along with short-term medications aimed at improving postoperative recovery and functional outcomes following cervical spine decompression and stabilization surgery.
Advice on Discharge
The patient was allowed to take a bath and was advised that he could ambulate independently and climb stairs as tolerated. He was instructed to avoid strenuous physical activities and heavy exertion to prevent strain on the cervical spine and surgical site. He was advised to continue physiotherapy as prescribed for postoperative rehabilitation and functional recovery and to adhere to the treatment regimen regularly.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms, such as fever, wound discharge, increasing neck pain, or any new or worsening weakness or numbness in the upper or lower limbs.
Review and Follow-Up Notes
The patient was advised to return for a follow-up with the Neurosurgeon in Hyderabad at PACE Hospitals after 2 weeks for postoperative evaluation and wound assessment. He was also advised to undergo staple removal after 10 days at the hospital or a nearby healthcare facility.
Conclusion
This case highlights cervical canal stenosis with compressive myelopathy at the C5–C6 level associated with multilevel cervical spondylotic changes and severe spinal canal narrowing. Imaging confirmed significant cord compression at C5–C6 with associated neural foraminal stenosis. Surgical management was performed with posterior cervical decompression and stabilization, including laminectomy and foraminotomy. The postoperative course was stable with appropriate neurological recovery and an uneventful hospital stay.
Multilevel Cervical Spine Degenerative Disease Requiring Surgical Management
Degenerative cervical spine disease can lead to progressive narrowing of the spinal canal and compression of neural structures, resulting in myelopathic features and neurological impairment. Radiological evaluation typically demonstrates multilevel disc degeneration, osteophyte formation, and foraminal stenosis contributing to neural compression. In cases of progressive neurological deterioration or inadequate response to conservative management, surgical decompression with or without stabilization is considered. Decompression procedures with or without instrumentation may be performed to relieve neural pressure and maintain spinal stability based on clinical requirements.
Evaluation by a neurosurgeon/neurosurgery doctor is essential to assess neurological status and determine the need for surgical intervention along with optimization of perioperative care. Postoperative care includes neurological monitoring, early mobilization, and rehabilitation to support recovery. Timely intervention is essential to prevent permanent neurological deficits and improve functional outcomes.
Frequently Asked Questions (FAQs)
What is cervical spine stabilization, and why is it necessary after surgery?
Cervical spine stabilization is a procedure where the spine is supported and secured to allow healing after surgery. It’s necessary to prevent further injury, keep the spine in the correct position, and ensure that the healing process is as smooth as possible. This helps in avoiding complications such as spinal instability or nerve damage.
How long does recovery typically take after cervical spine laminectomy and foraminotomy?
Recovery from cervical spine laminectomy and foraminotomy typically takes several weeks to months. Initial healing may take about 4 to 6 weeks, while full recovery can take 3 to 6 months. During this time, physical therapy and rest are crucial for a smooth recovery.
When can physical activities be resumed after cervical spine surgery?
Strenuous physical activity should be avoided for the first 4 to 6 weeks after surgery to allow the spine to heal. Light activities can be gradually resumed after this period, as advised by the doctor. High-impact sports or exercises should be avoided for at least 3 months, or until the doctor gives clearance.
What is the role of physiotherapy in post-surgery recovery after cervical spine surgery?
Physiotherapy is essential for regaining strength, mobility, and flexibility after surgery. It helps reduce stiffness, improve posture, and alleviate pain. A physical therapist will guide through exercises that are safe and effective for recovery, helping return to normal activities without compromising healing.
When can work be resumed after undergoing cervical spine surgery?
The time to return to work depends on the nature of the job. For desk jobs that require sitting, work may be resumed in 4 to 6 weeks. However, for jobs involving heavy lifting or physical strain, it may be necessary to wait until full healing, which could take 2 to 3 months. It is important to consult the doctor before resuming work.
How does cervical spine surgery affect long-term mobility and daily activities?
After cervical spine surgery, many patients experience improved mobility, reduced pain, and better quality of life. While some limitations may remain depending on the extent of the surgery, there is often better movement and less discomfort during daily tasks, such as bending or turning the head, as long as the recovery plan is followed.
Are there any dietary recommendations after cervical spine surgery?
A balanced diet is important to support healing after surgery. Foods rich in protein, vitamins, and minerals, such as lean meats, vegetables, fruits, and whole grains, help with tissue repair and reduce inflammation. Calcium and vitamin D are crucial for bone health, and staying hydrated supports overall recovery.
How often are follow-up appointments required after cervical spine surgery?
Follow-up appointments are generally scheduled 2 to 3 weeks after surgery to assess healing progress and remove any stitches if necessary. Further visits may be required at 6 weeks and 3 to 6 months to track recovery, modify treatment plans, and evaluate the success of the surgery over time.
What lifestyle restrictions are recommended after cervical spine surgery?
After surgery, heavy lifting, twisting motions, and activities that strain the neck should be avoided for the first few months. Activities that risk falling or injury, such as high-impact sports, should also be avoided until the doctor confirms it is safe. Gentle stretching and walking are encouraged, but guidance from the doctor should be followed.
When should one worry after discharge?
Worry should arise after discharge if severe pain, difficulty moving, numbness or tingling in the arms or legs, fever, or swelling at the surgery site occur. These symptoms may indicate complications such as infection or nerve damage. In such cases, it is important to contact the healthcare provider promptly for evaluation and guidance.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868