Successful Early Diagnosis & Treatment of CVST in a 23 Y.O. Female with PCOS and Severe Anemia
PACE Hospitals
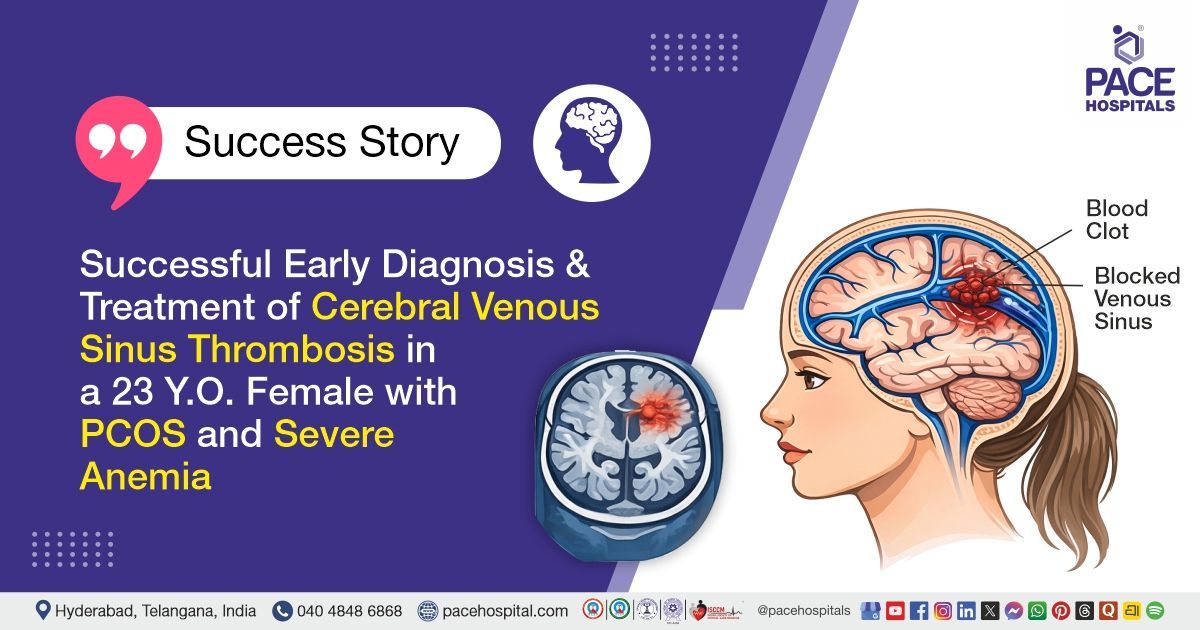
PACE Hospitals’ expert Neurology team successfully managed a 23-year-old female patient diagnosed with Cerebral Venous Sinus Thrombosis (CVST – involving the left transverse sinus, sigmoid sinus, and internal jugular vein), severe iron deficiency anemia, and polycystic ovary syndrome (PCOS). The management aimed to ensure timely recanalization and prevent thrombus progression to avoid neurological complications. It also focused on correcting iron deficiency anemia and addressing PCOS for improved overall recovery and long-term health.
Chief Complaints
A 23-year-old female patient with a body mass index (BMI) of 21 presented to the Neurology Department at PACE Hospitals, Hitech City, Hyderabad, with a 2-day history of headache accompanied by multiple episodes of vomiting and transient visual blurring.
Past Medical History
The patient had a known history of polycystic ovary syndrome (PCOS) and was on treatment prior to the current admission. She had no prior history of similar headache episodes, seizures, focal neurological deficits, or visual disturbances. There was no documented history of chronic medical illnesses such as hypertension, diabetes mellitus, or any previous thrombotic events.
On Examination
On examination, the patient was conscious, coherent, and oriented. She was afebrile with stable vital signs. Neurological examination revealed intact higher mental functions with normal memory, speech, and language. Cranial nerve examination showed normal extraocular movements with no evidence of nystagmus. Motor system examination was normal with preserved power in all four limbs, and sensory examination was intact. There were no cerebellar signs or focal neurological deficits noted.
Diagnosis
Upon admission, the patient underwent a comprehensive clinical evaluation, including a detailed medical history and neurological assessment by the Neurology team. She presented with complaints of severe holocranial headache (involving the whole head) associated with multiple episodes of vomiting and transient visual blurring. Clinical examination revealed no focal neurological deficits, and higher mental functions were intact.
Laboratory investigations were conducted as part of the assessment. Complete blood count (CBC) revealed anemia with microcytic hypochromic picture. Iron studies showed low serum iron and low transferrin saturation with elevated total iron-binding capacity, consistent with severe iron deficiency anemia. Vitamin B12 levels were low, while folate levels were within normal limits. Renal and liver function tests were within normal limits. Thyroid function tests (T3, T4, and TSH) were also within normal range. Coagulation profile showed mildly prolonged prothrombin time and INR.
Neuroimaging investigations, including Magnetic Resonance Imaging (MRI) of the brain with contrast, revealed filling defects in the left transverse sinus, left sigmoid sinus, and left internal jugular vein, suggestive of acute Cerebral Venous Sinus Thrombosis (CVST). Additional findings included features of raised intracranial pressure such as tortuosity of bilateral optic nerves, increased optic nerve sheath fluid, mild flattening of optic discs, and partial empty sella.
Based on the clinical presentation and radiological findings, the patient was advised to undergo Cerebral Venous Sinus Thrombosis (CVST) Treatment in Hyderabad, India, along with severe iron deficiency anemia and underlying polycystic ovary syndrome (PCOS), under the expert care of the Neurology Department with anticoagulation therapy, correction of anemia, and multidisciplinary support.
Medical Decision-Making (MDM)
After a detailed consultation by Dr. S Pramod Kumar, Consultant Neurophysician, along with cross-consultants Dr. Mounika Jetti and Dr. Mugdha Bandawar, the patient was diagnosed with cerebral venous sinus thrombosis (CVST) involving the left transverse sinus, sigmoid sinus, and internal jugular vein, associated with severe iron deficiency anemia and underlying PCOS. As the patient presented with an acute onset of severe headache and vomiting with radiological evidence of venous thrombosis and raised intracranial pressure, prompt anticoagulation and supportive management were considered essential.
It was determined that anticoagulation therapy to prevent thrombus propagation and facilitate recanalization, along with management of raised intracranial pressure and correction of underlying anemia with parenteral iron therapy, constituted the most appropriate treatment plan. Multidisciplinary care including gynecological evaluation for PCOS and menorrhagia was also incorporated to address contributing factors and optimize overall clinical outcomes.
The patient and her family members were counselled in detail regarding the condition, treatment plan, importance of medication adherence, recognition of warning symptoms such as worsening headache, vomiting, or neurological deficits, and the need for regular follow-up in the Neurology outpatient department to monitor recovery and prevent complications.
Treatment
Following the decision, the patient underwent treatment for Cerebral Venous Sinus Thrombosis (CVST) along with severe iron deficiency anemia and underlying polycystic ovary syndrome (PCOS) in Hyderabad at PACE Hospitals, under the expert supervision of the Neurology team.
During the hospital stay, the patient was initiated on appropriate therapy aimed at preventing further progression of intracranial venous thrombosis and promoting recanalization of the affected sinuses. Measures were taken to reduce raised intracranial pressure and alleviate symptoms such as headache and vomiting. Supportive care including hydration and symptomatic management was provided throughout the course of treatment.
In view of severe iron deficiency anemia, she received treatment for correction of anemia to improve hematological status and overall recovery. A multidisciplinary approach was adopted, and gynecological evaluation was obtained to address underlying PCOS and associated menstrual concerns. The patient showed clinical improvement with resolution of symptoms and remained neurologically stable at the time of discharge.
Discharge Medications
At the time of discharge, the patient was advised to continue medications aimed at preventing further clot formation and promoting resolution of the existing thrombosis. She was also prescribed treatment to support hematological recovery and improve overall wellbeing. The importance of strict compliance with medications, monitoring for any warning symptoms, and regular follow-up was emphasized to ensure optimal recovery and prevent recurrence.
Advice on Discharge
The patient was advised to continue all prescribed medications as directed.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms such as severe headache, vomiting, giddiness, seizures, or any new neurological deficits.
Review and Follow-Up Notes
The patient was advised to return for a follow-up with the Neurophysician in Hyderabad at PACE Hospitals after 1 week.
Conclusion
This case highlights cerebral venous sinus thrombosis with raised intracranial pressure and severe iron deficiency anemia, along with underlying PCOS. Targeted management for thrombosis, correction of anemia, and supportive care led to the resolution of symptoms. The patient was discharged hemodynamically stable, advised to continue medications, follow up in neurology OPD, and seek immediate care if any acute neurological symptoms develop.
Multidisciplinary Approach in CVST with Hematological and Endocrine Comorbidities
Cerebral Venous Sinus Thrombosis (CVST) often presents headaches, vomiting, and signs of raised intracranial pressure. Early imaging and prompt management under a Neurophysician/Neurology doctor are crucial for accurate diagnosis and effective treatment. Timely anticoagulation remains the cornerstone of therapy, while correction of underlying hematological issues, such as iron deficiency anemia, supports recovery and reduces complications.
Endocrine or gynecological disorders, like PCOS, may contribute to risk and should be addressed in a multidisciplinary manner. Coordinated care between neurology, hematology, and gynecology improves outcomes. Close monitoring, supportive therapy, and structured follow-up are essential to prevent recurrence and maintain long-term health. Patient education regarding warning signs and adherence to therapy is vital for early detection of complications. Individualized treatment plans help optimize recovery and minimize long-term neurological deficits.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868