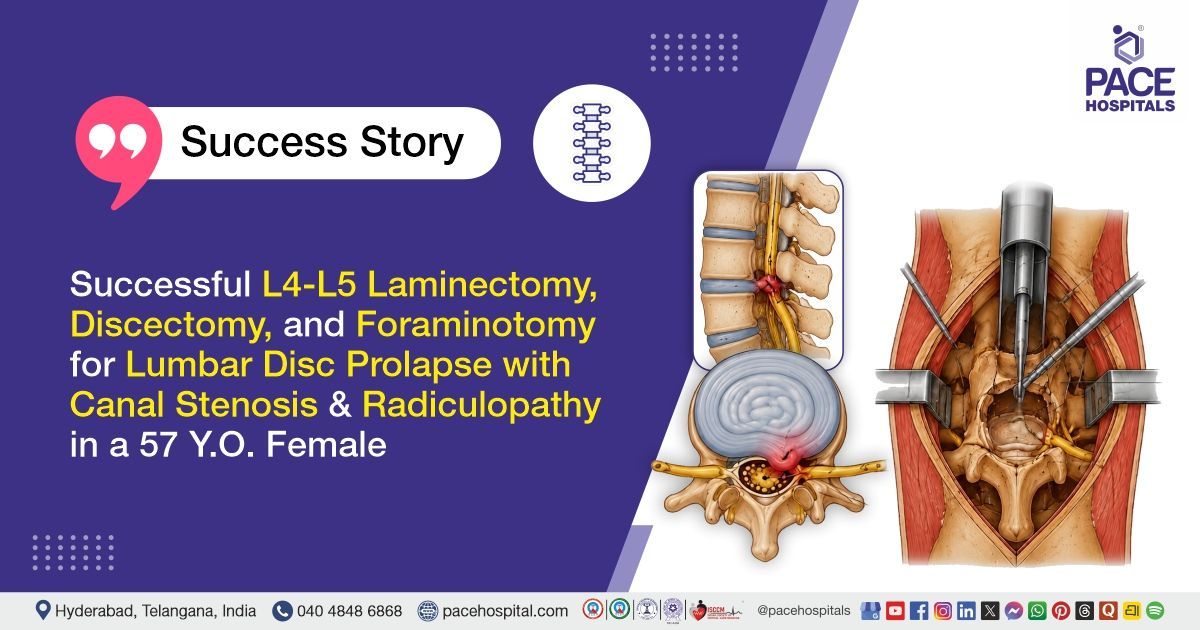
Successful L4-L5 Laminectomy, Discectomy & Foraminotomy for Lumbar Disc Prolapse
PACE Hospitals
PACE Hospitals’ expert Neurosurgery team successfully performed an L4–L5 Minimally Invasive Laminectomy, Discectomy, and Foraminotomy on a 57-year-old female patient diagnosed with L4–L5 intervertebral disc prolapse with canal stenosis and left lower limb radiculopathy, with the aim of relieving pressure on the compressed spinal nerves, alleviating radiating pain and numbness in the left lower limb, improving mobility, and enhancing the patient’s overall quality of life through a minimally invasive surgical approach.
Chief Complaints
A 57-year-old female patient with a body mass index (BMI) of 21 presented to the Neurosurgery Department at PACE Hospitals, Hitech City, Hyderabad, with complaints of persistent low back pain associated with left lower limb radiculopathy for the past six months. She had a history of similar episodes of back pain, which were previously managed conservatively. The pain was present even at rest, aggravated by physical activity, and did not improve with medications. There was no associated history of motor weakness, bowel disturbances, or bladder dysfunction.
Past Medical History
The patient had no significant past medical history of diabetes mellitus, hypertension, cardiac illness, renal disease, thyroid disorders, tuberculosis, or any major previous surgical interventions. There was no history of bowel or bladder dysfunction or other significant comorbid illnesses.
On Examination
On examination, the patient was moderately built and nourished, conscious, coherent, alert and hemodynamically stable. Neurological examination revealed a positive straight leg raising test on the left side, suggestive of nerve root irritation. Motor power was preserved in both lower limbs, and plantar reflexes were bilaterally flexor. Cardiovascular examination revealed normal heart sounds, while respiratory system examination showed bilateral air entry with no added sounds. There were no focal neurological deficits, bowel or bladder involvement, or signs of systemic illness noted during evaluation.
Diagnosis
Upon admission to PACE hospitals, the patient underwent a comprehensive clinical evaluation, along with the patient’s medical history and diagnostic investigations conducted by the Neurosurgery team.
Laboratory and special investigations were conducted as part of the preoperative assessment. Complete blood counts (CBC) revealed microcytic hypochromic anemia with leukocytosis, while renal function tests, liver function tests, serum electrolytes, coagulation profile, and blood sugar levels were within normal limits. Viral screening for HIV, Hepatitis B, and Hepatitis C was negative. Urine analysis was normal. Chest X-ray demonstrated normal heart size with clear bilateral lung fields. Two-dimensional echocardiography showed normal cardiac chambers with good left ventricular and right ventricular function and Grade I left ventricular diastolic dysfunction, without any significant structural abnormalities.
Neuroimaging investigations, including X-ray and Magnetic Resonance Imaging (MRI) of the lumbar spine, demonstrated multilevel degenerative changes. MRI findings revealed Grade I retrolisthesis of L4 over L5 with diffuse disc bulge, peripheral annular tear, ligamentum flavum hypertrophy, and moderate to severe spinal canal stenosis at the L4–L5 level, along with bilateral neural foraminal narrowing and severe lateral recess stenosis causing impingement of bilateral traversing nerve roots. Associated spondylotic and facetal arthropathy changes were also noted at multiple lumbar levels.
Based on the confirmed diagnosis, the patient was advised to undergo L4-L5 Intervertebral Disc Prolapse Treatment in Hyderabad, India, with canal stenosis and left lower limb radiculopathy under the expert care of the Neurosurgery Department.
Medical Decision-Making (MDM)
After a detailed consultation with Dr. U. L. Sandeep Varma, Consultant Neurosurgeon, a comprehensive neurological assessment and radiological evaluation were performed to determine the most appropriate management and therapeutic approach. The patient presented with low back ache associated with left lower limb radiculopathy since 6 months, which was progressive in nature and not relieved with conservative medical management. MRI of the lumbosacral spine revealed L4–L5 intervertebral disc prolapse with diffuse disc bulge, ligamentum flavum hypertrophy, and moderate to severe spinal canal stenosis with severe bilateral lateral recess stenosis and bilateral nerve root impingement, along with moderate bilateral neural foraminal compromise, consistent with L4–L5 disc pathology causing left lower limb radiculopathy.
The clinical and radiological evaluation revealed features of significant lumbar canal stenosis with nerve root compression at the L4–L5 level correlating with the patient’s symptoms. It was determined that L4–L5 minimal invasive laminectomy and discectomy with foraminotomy under general anaesthesia was the most appropriate surgical intervention. This procedure was aimed at adequate decompression of neural elements, relief of radicular pain, improvement in functional status, and prevention of further neurological deterioration.
The patient and her family members were counselled in detail regarding the diagnosis, surgical procedure, postoperative care, physiotherapy, medication adherence, activity modification, and the need for regular follow-up to ensure optimal recovery and long-term functional outcome.
Surgical Procedure
Following the decision, the patient was scheduled to undergo an L4-L5 Minimal Invasive Laminectomy and, Discectomy Surgery in Hyderabad at PACE Hospitals along with Foraminotomy under the expert supervision of the Neurosurgery Department.
The procedure involved the following steps:
- Patient Positioning and Anaesthesia: The patient is placed in a prone position on the operating table after administration of general anaesthesia. Proper padding and positioning are ensured to avoid pressure injury. The surgical field is prepared and draped under strict aseptic precautions.
- Level Identification and Exposure: The L4–L5 level is identified using fluoroscopic guidance. A small midline or paramedian incision is made, and the paraspinal muscles are gently separated to expose the interlaminar space with minimal tissue disruption.
- Laminectomy and Decompression: A partial removal of the lamina at L4 is performed to access the spinal canal. The ligamentum flavum is excised to decompress the underlying neural elements and improve visibility of the dura and nerve root.
- Discectomy and Nerve Root Decompression: The affected L4–L5 disc is identified and prolapsed disc material is removed carefully in a piecemeal manner. Adequate decompression of the traversing nerve root is achieved, ensuring free and pulsatile neural structures.
- Foraminotomy and Closure: The neural foramen is widened to relieve any residual nerve compression. Hemostasis is secured, and the wound is closed in layers after confirming adequate decompression and stability of neural structures.
Postoperative Care
Postoperatively, the patient was monitored in the Intensive Care Unit (ICU) for hemodynamic stability, neurological status, and immediate surgical recovery. After stabilization, she was shifted to the ward for continued observation and care. Early mobilization was initiated under supervision, and she tolerated ambulation well with improving symptoms and stable neurological findings. The surgical wound was regularly assessed and remained clean, dry, and intact without evidence of infection or discharge. She was continued on medications for pain control, neuropathic symptom relief, infection prophylaxis, gastric protection, and bowel regulation, along with initiation of physiotherapy during the hospital stay.
Discharge Medications
Upon discharge, the patient was prescribed medications for postoperative nerve healing and nutritional recovery support. Local application was advised for wound care to promote healing and prevent infection. Medications were given for relief of pain and reduction of muscle spasm. Gastric protection was advised to prevent acidity and gastric discomfort during recovery. Treatment was provided for neuropathic pain and associated nerve-related symptoms. Antibiotic coverage was prescribed for prevention of postoperative infection, and bowel regulation support was advised to prevent constipation during the recovery period.
Advice on Discharge
The patient was advised to avoid prolonged sitting for more than 1 hour to reduce strain on the spine. She was instructed to strictly adhere to the prescribed medications as directed. Strenuous physical activities and heavy exertion were to be avoided during the recovery period. The patient was permitted to walk and climb stairs as tolerated. She was also advised that bathing is allowed while maintaining proper wound care precautions.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms such as fever, increasing back pain, weakness in the lower limbs, discharge from the surgical wound, severe or worsening pain, or any new neurological symptoms.
Review and Follow-Up Notes
The patient was advised to return for a follow-up with the Neurosurgeon in Hyderabad at PACE Hospitals after 1 month for follow-up assessment and clinical evaluation.
Conclusion
This case highlights L4–L5 intervertebral disc prolapse with canal stenosis and associated radiculopathy presenting with chronic low back pain and failure of conservative management. Surgical management with L4–L5 minimally invasive laminectomy, discectomy, and foraminotomy under general anaesthesia was performed. Postoperatively, there was significant symptomatic improvement with stable neurological status and good recovery at discharge.
Lumbar Disc Prolapse with Canal Stenosis – Surgical Outcomes
Lumbar disc prolapse with canal stenosis is a common cause of chronic low back pain and radiculopathy due to nerve root compression. When conservative management fails, a neurosurgeon/neurosurgery doctor may recommend surgical decompression procedures such as laminectomy, discectomy, and foraminotomy to relieve pressure on neural structures. Proper patient selection and timely intervention play a key role in preventing long-term neurological deficits.
Postoperative outcomes are generally favorable with significant pain relief and improvement in neurological function. Early mobilization and physiotherapy are essential components of recovery and help restore functional independence. Most patients achieve good clinical recovery when adequate decompression is achieved without complications. Long-term prognosis depends on the severity of preoperative compression and adherence to rehabilitation protocols.
Frequently Asked Questions (FAQs)
What is the recovery time after a minimal invasive lumbar laminectomy and discectomy?
Recovery time varies among individuals, though many patients start feeling better within a few weeks. Pain usually reduces during the first month after treatment. Following the doctor’s instructions is important for proper healing. Complete recovery may take a few months, depending on the patient’s condition. Returning to normal activities should be done gradually as strength improves.
Can this procedure help alleviate long-term back pain caused by disc prolapse?
Yes, this procedure removes the disc bulge or stenosis that compresses the nerves, which often helps in relieving chronic back pain. It usually provides good symptom relief, although the outcome can vary depending on individual conditions. Postoperative care, including physiotherapy, is important for maintaining long-term improvement. Mild discomfort may still be present during the recovery period as healing progresses.
How soon can I resume normal activities after the surgery?
Walking and climbing stairs can usually be started within a few weeks after the procedure. Heavy activities should be avoided for at least one month to allow proper healing of the spine. Lifting heavy objects and sitting for long durations should be restricted during the early recovery period. Light exercises and physiotherapy help improve mobility and support recovery. Activity levels should be increased gradually as advised by the doctor.
What are the key post-operative care instructions after lumbar spine surgery?
Take medications as prescribed to manage pain and inflammation. Avoid sitting for long periods and follow the exercise routine to strengthen your back. Be sure to attend follow-up appointments to track your recovery. Physiotherapy is essential for regaining movement and strength. Watch for signs of infection or complications, such as increased pain or wound issues, and report them promptly.
What are the signs of complications that I should watch for after the surgery?
Seek immediate medical attention if you experience a fever, severe pain, or discharge from the wound. Any sudden weakness or numbness in your limbs should be reported. Unexplained bowel or bladder issues are also warning signs. These could indicate infection or nerve complications. Prompt treatment helps prevent serious problems and improves recovery.
How does physiotherapy help after this spinal surgery?
Physiotherapy helps strengthen the muscles supporting the spine and improves posture. It reduces stiffness and enhances flexibility. Regular sessions promote safe movement and build back strength. Following the advised exercises is important for proper recovery. It also helps in reducing pain and discomfort during the healing phase.
Will this surgery completely eliminate the risk of future back problems?
The surgery treats the existing disc prolapse but does not completely prevent future back problems. Maintaining proper posture, a healthy body weight, and regular physical activity is important for spine health. Activities that place excessive strain on the back, such as heavy lifting, should be avoided. Regular follow-up and a healthy lifestyle help reduce the risk of recurrence or further issues.
What is the difference between minimally invasive laminectomy and traditional open surgery for lumbar disc problems?
Minimally invasive laminectomy involves smaller incisions, which means less tissue damage and a faster recovery. Traditional open surgery requires larger cuts and a longer healing time. The minimally invasive approach causes less pain and has a lower risk of infection. It’s suitable for patients with certain types of disc problems. Overall, the recovery process is quicker with minimally invasive surgery.
Is it necessary to avoid all physical activity after lumbar spine surgery?
Strenuous activities and heavy lifting should be avoided, but mild physical activity like walking is encouraged. Short, frequent walks help prevent stiffness and support circulation. Climbing stairs is generally safe after a few weeks, but sitting for long periods should be avoided. Gradually increasing your activity level with the help of physiotherapy is recommended. Your doctor will guide you on which activities are safe as you recover.
What follow-up care is required after this procedure?
Follow-up appointments are important to ensure the surgery is healing properly. The first review is typically one month after surgery. During this visit, your doctor will assess your progress, address any concerns, and suggest further treatments if needed. Physiotherapy progress will also be monitored. Regular check-ups ensure that recovery is on track and any issues are dealt with early.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868