Colectomy Surgery, Procedure and Cost
PACE Hospitals offers advanced colectomy surgery in Hyderabad, India, providing effective treatment for conditions such as colon cancer, diverticular disease, and inflammatory bowel disorders. Our surgeons perform various types of colectomy, including total, subtotal, partial, sigmoid, right, and left colectomy, using both open and laparoscopic (minimally invasive) techniques for better precision and recovery.
With a focus on accurate diagnosis and personalized care, we ensure safe procedures, faster healing, and improved long-term outcomes for better digestive health and quality of life.
Book an Appointment for Colectomy Surgery
Colectomy Surgery Appointment
Why Choose PACE Hospitals for Colectomy?
Expert Colorectal Surgeons in Hyderabad Specializing in Comprehensive Colectomy Surgery for Cancer, IBD & Other Colorectal Disorders
Precision Colectomy Surgery with Laparoscopic & Open Techniques for Safe Removal & Restoration
Transparent Colectomy Surgery with Insurance & Cashless Options
Colectomy Meaning
A colectomy is a surgical procedure in which a part or the entire colon (large intestine) is removed. This procedure is done to treat various conditions such as
colon cancer, severe infections,
inflammatory bowel diseases, or intestinal blockage. The surgery can be partial (removing only the affected part) or total (removing the whole colon). After the surgery, the parts of the digestive system that were left are put back together so that the bowels can work normally. A stoma is a temporary or permanent opening that is made in some cases to allow waste to pass through. This procedure helps relieve symptoms and prevent further complications.
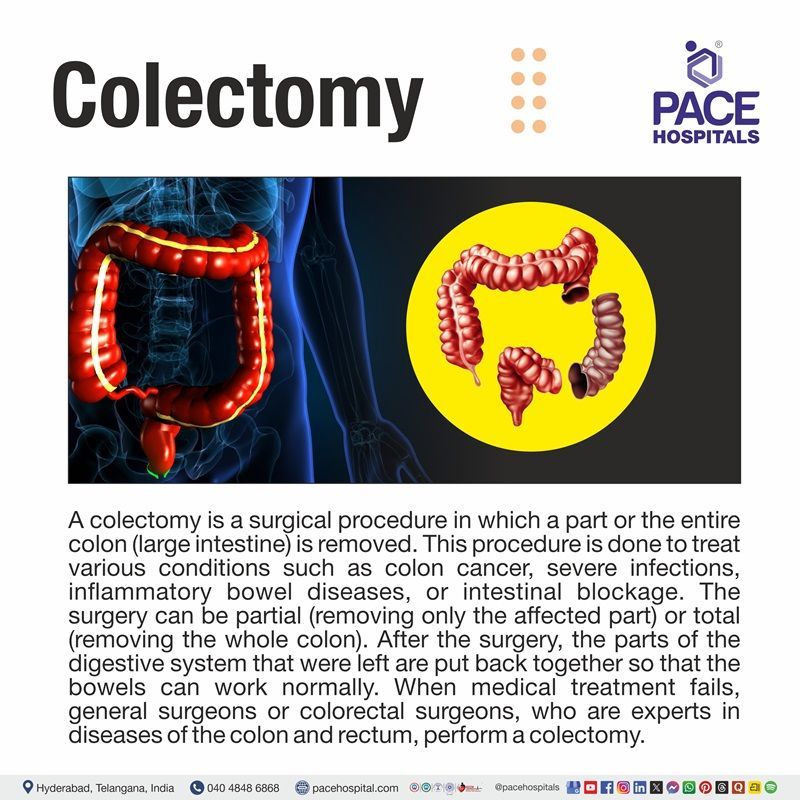
When medical treatment fails,
general surgeons or colorectal surgeons, who are experts in diseases of the colon and rectum, perform a colectomy. In some cases, the procedure may also be done by minimally invasive surgeons. It implies taking out the diseased part of the colon and connecting the bowel back together. It is done while the patient is under anesthesia and requires careful care after the surgery. This surgery helps relieve symptoms and prevent serious complications.
Types of Colectomy
The extent and anatomical segment of colon removed classify the different types of colectomy. Depending on the location and severity of the disease, different surgical approaches are chosen. Each type targets a particular segment of the colon to effectively treat the condition while preserving as much normal bowel function as possible. Common types of colectomy surgery include:
- Total colectomy
- Partial (subtotal) colectomy
- Segmental colectomy
- Hemicolectomy
- Sigmoid colectomy
- Proctocolectomy
Total colectomy
Total colectomy is a type of surgery in which the complete colon is removed. It is most commonly used for diseases that affect the entire colon, like cancer or severe inflammatory disease. After removal, the small intestine may be connected to the rectum, or a stoma may be created for waste elimination. The procedure helps eliminate diseased tissue and prevents complications.
Partial (subtotal) colectomy
Partial colectomy involves the removal of only the affected portion of the colon. It has different types:
- Segmental colectomy: A segmental colectomy involves the removal of a small diseased portion of the colon while preserving the remaining healthy tissue. It is usually done for localized conditions such as small tumours or limited inflammation. The cut ends of the colon are then reconnected to maintain normal bowel function.
- Hemicolectomy: Hemicolectomy is a surgical procedure in which one side of the colon, either right or left, is removed based on the location of the disease. The right hemicolectomy removes the ascending colon, while the left removes the descending colon. After removal, the remaining parts of the intestine are connected to re-establish normal bowel function.
- Sigmoid Colectomy: A sigmoid colectomy involves the removal of the sigmoid colon, the lower part of the large intestine. It is commonly performed for conditions like diverticulitis (disease of the large bowel) or cancer. After removal, the descending colon is connected to the rectum to maintain normal bowel function.
Proctocolectomy
Proctocolectomy is the surgical removal of the colon and the rectum. It is usually done for severe issues like
ulcerative colitis (inflammatory bowel disease) or colorectal cancer that affects the rectum. After surgery, waste is eliminated through an ileostomy (surgical opening) or a pouch may be created. This procedure removes all diseased large intestinal tissue and helps control symptoms.
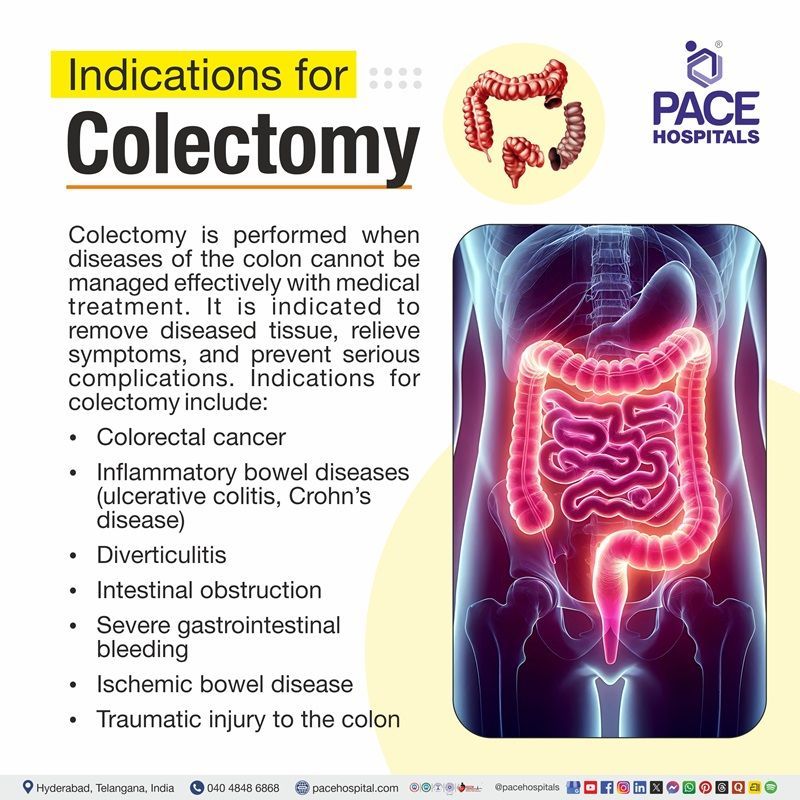
Colectomy indications
Colectomy is performed when diseases of the colon cannot be managed effectively with medical treatment. It is indicated to remove diseased tissue, relieve symptoms, and prevent serious complications. Indications for colectomy include:
- Colorectal cancer
- Inflammatory bowel diseases (ulcerative colitis, Crohn’s disease)
- Diverticulitis
- Intestinal obstruction
- Severe gastrointestinal bleeding
- Ischemic bowel disease
- Traumatic injury to the colon
Colorectal cancer
Colectomy is commonly done to remove cancerous growths in the colon. The affected segment, along with nearby lymph nodes, is removed to prevent spread. It is a primary treatment for localized colon cancer. Early surgery improves survival and reduces recurrence.
Inflammatory bowel diseases (ulcerative colitis, Crohn’s disease)
When the disease is severe and fails to get better with medicine, surgery is recommended. In some cases, like when there are problems like bleeding, perforation, or a risk of cancer, it may be necessary. Removal of the diseased colon helps control symptoms. It can significantly improve the quality of life.
Diverticulitis
Diverticulitis is inflammation or infection of small pouches (diverticula) that form in the wall of the colon, and colectomy is done in recurrent or complicated cases. Indications include abscess, perforation, or fistula formation. The affected segment of the colon is removed to prevent further episodes. This helps reduce the risk of serious complications.
Intestinal obstruction
Surgery is required when blockage of the colon cannot be relieved by conservative methods. Causes include tumors, strictures, or volvulus. The obstructed portion is removed to restore bowel passage. This prevents bowel damage and perforation.
Severe gastrointestinal bleeding
Colectomy may be necessary when bleeding from the colon cannot be controlled. It is considered in life-threatening or recurrent bleeding cases. The source of bleeding is removed surgically. This helps stabilize the patient and prevent further blood loss.
Ischemic bowel disease
Surgery is indicated when there is a reduced blood supply, causing tissue death in the colon. If untreated, it can lead to perforation and infection. The affected non-viable segment is removed. This prevents the spread of infection and serious complications.
Traumatic injury to the colon
Colectomy is performed in cases of severe abdominal trauma involving the colon. Injuries may cause perforation or contamination of the abdomen. The damaged section is removed to prevent infection. Surgical repair helps restore bowel function.
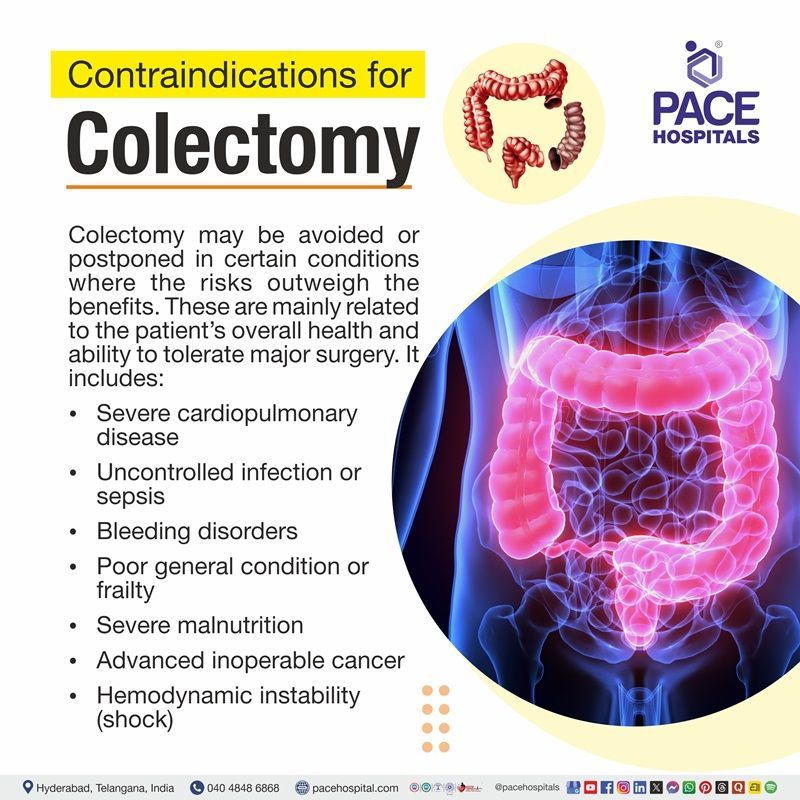
Colectomy Contraindications
Colectomy may be avoided or postponed in certain conditions where the risks outweigh the benefits. These are mainly related to the patient’s overall health and ability to tolerate major surgery. It includes:
- Severe cardiopulmonary disease
- Uncontrolled infection or sepsis
- Bleeding disorders
- Poor general condition or frailty
- Severe malnutrition
- Advanced inoperable cancer
- Hemodynamic instability (shock)
Severe cardiopulmonary disease
Patients with serious heart or lung conditions may not tolerate anesthesia or major surgery. There is a high risk of complications such as cardiac failure or respiratory distress. Surgery may worsen their condition and increase the risk of mortality. Hence, it is usually avoided unless absolutely necessary.
Uncontrolled infection or sepsis
Active infection or sepsis increases the risk of surgical complications and poor healing. It can lead to the spread of infection and organ failure during or after surgery. Stabilization with antibiotics and supportive care is required first. Surgery is postponed until the infection is controlled.
Bleeding disorders
Conditions affecting blood clotting can cause excessive bleeding during surgery. This increases the risk of hemorrhage and complications. Coagulation status must be corrected before any surgical procedure. Elective colectomy is delayed until safe levels are achieved.
Poor general condition or frailty
Frail (weak) patients with poor physical status may not recover well after surgery. They have higher risks of complications, infections, and delayed healing. Surgery can lead to prolonged hospitalization and poor outcomes. Careful assessment is needed before proceeding.
Severe malnutrition
Malnourished patients have reduced ability to heal wounds and fight infections. This increases the risk of postoperative complications. Nutritional support is often required before surgery. Colectomy may be delayed until nutritional status improves.
Advanced inoperable cancer
When cancer has spread to many parts of the body, removing the colon may not cure the disease. In such cases, surgery can be risky and may not improve survival. Doctors usually focus on relieving symptoms and improving comfort (palliative care). Colectomy is done only if needed to reduce problems like blockage, pain, or bleeding.
Hemodynamic instability (shock)
Patients in shock have unstable blood pressure and poor organ perfusion. They are at very high risk during anesthesia and surgery. Immediate stabilization with fluids and medications is required. Surgery is usually delayed until the patient becomes stable.
Colectomy Advantages
Colectomy offers significant benefits in conditions affecting the colon by removing the diseased segment and relieving symptoms. Following are the advantages of colectomy:
- Removal of Diseased Tissue
- Symptom Relief
- Prevention of Complications
- Improved Quality of Life
- Life-saving Intervention
- Restoration of Bowel Function
Removal of Diseased Tissue
Colectomy effectively removes cancerous or damaged parts of the colon. This helps eliminate the source of disease. It is especially important in conditions like colon cancer or severe inflammation. Removing it early can stop the disease from getting worse.
Symptom Relief
The procedure helps relieve symptoms such as abdominal pain, bleeding, and bowel obstruction. Patients often experience improvement in bowel function after recovery. It reduces discomfort caused by chronic conditions. This leads to better daily functioning.
Prevention of Complications
Colectomy helps prevent major complications like perforation, infection, or the spread of disease. Removing the part that is affected reduces the chances of potential issues. This is especially important for serious or recurring conditions.
Improved Quality of Life
Colectomy improves the patient's quality of life by treating the underlying condition. Symptoms are reduced, which makes it possible to perform normal activities. It helps with long-term illnesses that make daily life challenging. Patients often feel better after recovery.
Life-saving Intervention
In emergency cases such as severe bleeding or obstruction, colectomy is used. It helps quickly control serious situations. Timely surgery prevents further deterioration. It plays an important role in acute care.
Restoration of Bowel Function
After removal of the diseased portion, the remaining bowel is reconnected. This helps restore normal digestive function in many cases. Patients can return to regular bowel habits. It supports better overall digestion.
Book a Free Second Opinion for Colectomy Procedure with Experienced Specialists
At PACE Hospitals, we are committed to providing our patients with the best possible care, and that includes offering second medical opinions with super specialists for treatment or surgery. We recommend everyone to get an expert advance medical second opinion, before taking decision for your treatment or surgery.
Colectomy Procedure
A colectomy may be performed using two different approaches:
- Open colectomy
- Laparoscopic-assisted colectomy
Open colectomy
In this method, the surgeon creates a single long incision along the abdomen to access the colon directly.
Laparoscopic-assisted colectomy
This technique involves making several small openings in the abdominal skin. A miniature camera is inserted through one opening to provide internal visualization, while specialized slender instruments are introduced through the others to carry out the procedure. Because the incisions are smaller, patients typically experience less discomfort and a quicker recovery.
Colectomy procedure steps are as follows:
Before colectomy surgery
- Before the surgery, the surgeon and medical team perform a preoperative evaluation to ensure the patient is suitable for colectomy. This includes physical examination, medical history, and investigations such as blood tests, colonoscopy, CT or MRI scans to identify the affected area of the colon.
- Patients must inform the doctor about all allergies (medications, anaesthesia) and provide a complete list of medications, including prescribed drugs, over-the-counter medicines, vitamins, and herbal supplements. Specific medications like blood thinners may need to be stopped as advised.
- Before colectomy, bowel preparation is often required to clean the colon. Patients are also instructed to fast before surgery and maintain good control of existing conditions such as diabetes or hypertension.
- Lifestyle modifications like quitting smoking and reducing alcohol intake are advised to reduce surgical risks and promote better recovery.
- Before the procedure, informed consent is obtained after explaining the benefits, risks, alternatives, and expected outcomes. Patients are advised to arrange postoperative support.
During colectomy surgery
- Anaesthesia Administration: The procedure starts with general anaesthesia, which induces the patient's unconsciousness and keeps them from experiencing any pain. To ensure safety, vital signs are monitored throughout the surgery.
- Incision and Access: The surgeon makes an incision in the abdomen (open surgery) or several small incisions (laparoscopic surgery). Surgical instruments and a camera may be inserted to visualize the colon.
- Identification of Diseased Segment: The affected portion of the colon is carefully located. Blood supply to that segment is controlled before removal.
- Resection of the Colon: The part of the colon that is diseased is removed. In some cases, nearby lymph nodes are also removed, especially if cancer is in the area.
- Anastomosis (Reconnection): To restore bowel continuity, the healthy ends of the colon are reconnected. This lets stool pass through normally.
- Stoma Formation (if required): If reconnection isn't possible or needs time to heal, a stoma (colostomy or ileostomy) is made to move waste outside the body.
- Closure of Incision: The area where the surgery was done is checked for bleeding, and the incisions are closed with sutures or staples. After that, the patient is moved to the recovery room for monitoring.
After colectomy surgery
- After the procedure, the patient is taken to a recovery area where vital signs are closely monitored. A hospital stay of several days is usually required, depending on the type of surgery and recovery.
- Pain is managed with medications, and the patient may have tubes such as an IV line for fluids, a urinary catheter, or a nasogastric tube to keep the stomach empty.
- At first, the patient is not allowed to eat or drink. Fluids are gradually introduced, followed by soft and then regular foods as bowel function returns. Passing gas indicates that the intestines are working again.
- The patient is encouraged to move early to prevent blood clots and improve recovery. Breathing exercises may also be recommended to avoid lung complications.
- Before discharge, the patient is advised about wound care, activity level, diet, and follow-up. They are advised to contact the doctor if they develop fever, increasing pain, or signs of infection.
Complications of colectomy surgery
Colectomy is a major abdominal surgery associated with potential postoperative complications. The following are the colectomy complications:
- Anastomotic leak
- Hemorrhage
- Surgical site infection (SSI)
- Postoperative ileus
- Bowel obstruction
- Intra-abdominal abscess
- Wound dehiscence
- Incisional hernia
- Sepsis
- Deep vein thrombosis (DVT) / Pulmonary embolism (PE)
- Pneumonia
- Urinary tract infection
- Ischemic colitis
Anastomotic leak
Anastomotic leak happens when the surgical join between two parts of the bowel breaks down, allowing intestinal contents to leak into the abdomen. It is one of the most serious problems that can happen after a colectomy and can cause peritonitis and sepsis. Patients usually show up with a fever, abdominal pain, tachycardia, and an ileus. Management involves antibiotics, drainage, and frequently urgent reoperation.
Hemorrhage
After a colectomy, bleeding may occur from the surgical site or from inside the abdomen. Tachycardia, hypotension, and a decrease in hemoglobin levels are some of the signs of this condition. Bleeding that happens right after surgery is usually caused by the surgery itself, while bleeding that happens later may be caused by an infection or the erosion of a blood vessel. Treatment includes fluid resuscitation, blood transfusions, and surgery if necessary.
Surgical site infection (SSI)
Surgical site infection occurs when the incision or deeper tissues get infected after surgery. Redness, swelling, pain, pus discharge, and fever are common signs of this condition. Colorectal surgeries have a higher risk because bacteria from the bowel can get into the body. Antibiotics, draining pus, and taking care of the wound properly are a part of management.
Postoperative ileus
After surgery, postoperative ileus is a short-term blockage in bowel movement. It causes abdominal distension, vomiting, and the inability to pass stool. It is often caused by handling the bowels, anesthesia, and an imbalance of electrolytes. Management usually involves fluids, bowel rest, and early mobilization.
Bowel obstruction
Bowel obstruction after colectomy is usually due to adhesions, strictures, or hernias. Patients present with irritable abdominal pain, vomiting, distension, and constipation. It can occur in the early or late postoperative period. Management depends on severity and ranges from conservative treatment to surgery.
Intra-abdominal abscess
An intra-abdominal abscess is a localized collection of pus within the abdomen. It usually results from infection or anastomotic leakage. Patients with symptoms like fever, abdominal pain, and leukocytosis. Management includes antibiotics and drainage.
Wound dehiscence
Wound dehiscence is when the layers of the surgical incision come apart. It occurs due to poor healing, infection, or increased abdominal pressure. Patients may notice discharge or wound opening. It requires urgent surgical management.
Incisional hernia
An incisional hernia is a protrusion of abdominal contents through a weakened surgical scar. It happens months after surgery because the wound doesn't heal properly. Patients present with a bulge at the incision site. Treatment is usually surgical repair.
Sepsis
Sepsis is a severe systemic response to infection, often from intra-abdominal sources. It presents with fever, tachycardia, hypotension, and organ dysfunction. It is life-threatening if not treated early. Management includes antibiotics, fluids, and intensive care.
Deep vein thrombosis (DVT) / Pulmonary embolism (PE)
DVT is the clot formation in deep veins due to immobility after surgery. PE occurs when the clot travels to the lungs, causing chest pain and breathlessness. These are major postoperative complications. Prevention and treatment involve anticoagulation and mobilization.
Pneumonia
Pneumonia is a postoperative lung infection that occurs because of reduced mobility and shallow breathing. It presents with cough, fever, and breathlessness. It happens often in older people or after surgeries that last a long time. Management includes antibiotics and respiratory support.
Urinary tract infection
UTI occurs commonly due to catheterization during surgery. It causes fever, painful urination, and cloudy urine. It is a common infection that people get in the hospital. Antibiotics and early catheter removal are part of the treatment.
Ischemic colitis
Ischemic colitis is caused by reduced blood supply to the colon. It leads to inflammation, abdominal pain, and bloody
diarrhea. It may occur due to vascular compromise during surgery. Treatment is mainly supportive, with surgery in severe cases.
Colectomy surgery recovery time
Colectomy recovery mainly depends on the surgical approach used. With laparoscopic colectomy, recovery is usually quicker due to smaller incisions. Hospital stay is shorter (approx. three to five days), and most patients are able to return to routine daily activities within 4–6 weeks.
Recovery after open colectomy generally takes longer because of the larger incision. Hospital stay is extended (approx. five to seven days), and full recovery may take 6–8 weeks or longer.
In both approaches, bowel movements may be irregular during the early recovery period, and a gradual increase in activity helps support healing.
What questions can patients ask the healthcare team about colectomy?
- When can discharge from the hospital be expected?
- When should the next follow-up visit be scheduled?
- What type of pain or discomfort is normal after surgery, and how will it be managed?
- When can normal daily activities such as walking, driving, or climbing stairs be resumed?
- What is the typical recovery time after colectomy?
- What precautions should be followed during the recovery period?
- What complications or warning signs should be watched for after surgery?
- Will bowel habits change after colectomy, and how long do they take to stabilize?
- Are there any long-term effects after the removal of part or all of the colon?
- What diet should be followed during early recovery and later stages?
- If a stoma is created, how should it be cared for, and is it temporary or permanent?
- Is any additional treatment or monitoring required after surgery?
Difference between colectomy and colostomy
Colectomy vs colostomy
Colectomy and colostomy are different surgical procedures used in the treatment of colon and bowel conditions. A colectomy involves the removal of a part or the entire colon, while a colostomy creates an opening in the abdomen to divert stool. Below are key parameters that differentiate colectomy and colostomy.
| Parameters | Colectomy | Colostomy |
|---|---|---|
| Definition | Colectomy is a surgical procedure in which a part or the whole of the colon is removed to treat disease or injury. | Colostomy is a procedure in which an opening (stoma) is created in the abdominal wall to divert stool into an external bag. |
| Purpose | Performed to remove diseased sections of the colon, such as cancer, inflammation, obstruction, or severe infection. | Performed to allow stool to pass safely when the colon or rectum cannot be used temporarily or permanently. |
| Recurrence / Reversal | Disease recurrence depends on the underlying condition, but bowel continuity is often restored during surgery. | Colostomy can often be reversed if bowel healing allows; some cases require permanent diversion. |
| Recovery time | Recovery usually takes several weeks, depending on the extent of colon removal. | Recovery focuses on stoma healing and adaptation; patients learn stoma care during recovery. |
| Use in the treatment pathway | It can be performed with or without creating a stoma. | It may be performed along with colectomy or as a standalone diversion procedure. |
Colectomy Surgery Cost in Hyderabad, India
The cost of Colectomy Surgery (removal of part or all of the colon) in Hyderabad generally ranges from ₹1,50,000 to ₹5,00,000 and above (approx. US $1,805 – US $6,020).
The exact cost of colectomy surgery varies depending on the type of colectomy (total, partial, laparoscopic, or open surgery), the reason for the surgery (e.g., colorectal cancer, diverticulitis, inflammatory bowel disease), the complexity of the condition, and the surgical approach (laparoscopic vs. open surgery). Additional factors such as preoperative imaging (CT scan, colonoscopy), hospital stay duration, postoperative care, and rehabilitation can further influence the total cost. Availability of cashless treatment options, TPA corporate tie-ups, and insurance assistance may also impact overall expenses.
Cost Breakdown According to Type of Colectomy Surgery
- Partial Colectomy (Removal of part of the colon) – ₹1,50,000 – ₹3,00,000 (US $1,805 – US $3,615)
- Total Colectomy (Removal of the entire colon) – ₹2,00,000 – ₹4,00,000 (US $2,410 – US $4,820)
- Laparoscopic Colectomy – ₹2,50,000 – ₹4,50,000 (US $3,010 – US $5,420)
- Open Colectomy Surgery – ₹2,50,000 – ₹5,00,000 (US $3,010 – US $6,020)
- Colectomy with Colorectal Cancer Treatment (including chemotherapy, if required) – ₹3,00,000 – ₹6,50,000+ (US $3,615 – US $7,830+)
Frequently Asked Questions (FAQs) on Colectomy
Does colectomy cure ulcerative colitis?
Yes, colectomy cures ulcerative colitis because the disease only affects the colon and rectum. Removing the colon ceases the inflammation and prevents recurrence in the bowel. However, extraintestinal symptoms may still be present after surgery, so it is not a permanent cure for intestinal disease, but not for all systemic symptoms.
Looking for the Best Colectomy Surgery Hospital Near Me?
If you’re searching for the top colorectal surgery hospital near me in areas like HITEC City, Madhapur, Kondapur, Gachibowli, Kukatpally, or KPHB, it is essential to choose a hospital with experienced colorectal surgeons and advanced surgical technology.
Effective colectomy treatment requires:
- Accurate diagnosis with imaging (CT, colonoscopy, MRI)
- Laparoscopic or open surgery with precise technique
- Postoperative care, including nutrition and rehabilitation
- Support for cancer treatment if required (chemotherapy, radiation)
At PACE Hospitals, Hyderabad, patients receive comprehensive care with a multidisciplinary approach for the treatment of colorectal conditions requiring surgery.
Is a colectomy a major surgery?
Yes, colectomy is considered a major abdominal surgery because it involves the removal of bowel segments and the manipulation of abdominal organs. It requires general anesthesia and hospital recovery. Advances in minimally invasive techniques have improved safety and recovery outcomes.
Which Is the Best Hospital for Colectomy Surgery in Hyderabad, India?
PACE Hospitals, Hyderabad, is a trusted centre for advanced colorectal surgery and comprehensive gastrointestinal care, offering specialised treatment for patients with conditions like colorectal cancer, diverticulitis, Crohn’s disease, and ulcerative colitis that may require colectomy surgery.
We have highly experienced colorectal surgeons, oncologists, anesthesiologists, critical care teams, and nutritionists who follow evidence-based protocols to manage complex gastrointestinal conditions requiring surgery. Whether the surgery is laparoscopic or open, our surgeons use advanced techniques for minimal invasiveness, reduced recovery times, and improved patient outcomes.
We manage complicated cases and have facilities that include state-of-the-art operation theatres, laparoscopic equipment, imaging systems, and dedicated postoperative care, PACE Hospitals ensures a high standard of care for colectomy surgery patients.
What is the survival rate of a colectomy?
The survival rate after a colectomy is usually high, especially for elective surgeries. In otherwise healthy patients, the death rate is usually less than 1–5%. The patient's age, other health problems, and the reason for the surgery all play a role in the outcomes. Emergency colectomies have a higher risk, with death rates as high as 10% to 20%. Overall, most patients recover well with appropriate perioperative care.
What Is the Cost of Colectomy Surgery at PACE Hospitals, Hyderabad?
At PACE Hospitals, Hyderabad, the cost of colectomy surgery typically ranges from ₹1,40,000 to ₹4,50,000 and above (approx. US $1,685 – US $5,420), making it a cost-effective and high-quality option for colorectal surgery in Hyderabad. However, the final cost depends on:
- Type of colectomy (partial vs total, laparoscopic vs open)
- Complexity of the underlying condition (e.g., cancer, inflammatory bowel disease)
- Need for chemotherapy or additional treatments
- Hospital stay duration and ICU care if required
- Diagnostic tests (colonoscopy, CT scan)
- Postoperative rehabilitation and follow-up care
For partial colectomy or laparoscopic procedures, costs remain toward the lower end, while total colectomy with cancer treatment or open surgery may fall toward the higher range.
After a detailed gastrointestinal evaluation, imaging studies, and consultation with our specialists, we provide a transparent cost estimate tailored to the treatment plan.
What are the most common complications of a colectomy?
The most common complications of a colectomy include anastomotic leak, surgical site infection, and postoperative ileus. Other frequently seen complications are bowel obstruction, intra-abdominal abscess, and hemorrhage. Patients may also develop systemic complications such as sepsis, deep vein thrombosis, or pulmonary embolism. Early recognition and management are crucial to reducing morbidity and improving outcomes.
What is a sigmoid colectomy?
A sigmoid colectomy is a type of surgery that removes the sigmoid colon, the S-shaped part of the large intestine just above the rectum. It is performed to treat diverticular disease, tumours, strictures, or recurrent inflammation affecting this segment. After removal, the remaining colon is generally reattached to the rectum to restore bowel continuity.
What is a subtotal colectomy?
A subtotal colectomy involves the removal of most of the colon while preserving the rectum. This procedure is used when a disease affects multiple colon segments, such as extensive colitis, ischemia, or hereditary polyposis. Retaining the rectum allows the possibility of future bowel reconnection.
What is a partial colectomy?
A partial colectomy is a surgery that removes only the diseased part of the colon while preserving the healthy parts alone. It is commonly used for localized cancer, diverticulitis, or benign strictures. The remaining bowel ends are usually reconnected to maintain normal stool passage.
What is a total colectomy?
A total colectomy is a type of surgery that removes the entire colon but leaves the rectum intact. It is performed for conditions such as severe colitis, colonic inertia, or genetic cancer syndromes. Stool passage is maintained by connecting the small intestine to the rectum.
How long does a colectomy surgery take?
The duration of colectomy varies depending on the extent of resection and surgical approach. Most procedures take 2 to 4 hours, though complex cases may take longer. Laparoscopic colectomy surgeries often have slightly shorter operative times compared to open procedures.
Is colectomy safe in kids?
Colectomy is performed in children when medically necessary, such as for severe colitis, Hirschsprung disease (bowel blockage), or congenital conditions. Pediatric outcomes are generally favourable when surgery is done in specialized centres with appropriate follow-up care.
What is a total colectomy and ileostomy?
This procedure removes the entire colon and creates an ileostomy, where the small intestine is brought to the abdominal wall to pass stool into a bag. It is used when bowel reconnection is unsafe or not possible, either temporarily or permanently.
What to expect after a colectomy?
After colectomy, bowel movements may be irregular initially and improve over time. Hospital stay usually lasts several days, followed by a gradual return to normal activity. Diet progression, wound care, and follow-up visits are important parts of recovery.
Why is prophylactic colectomy not recommended in HNPCC?
In hereditary nonpolyposis colorectal cancer (HNPCC), routine prophylactic colectomy is not recommended because regular colonoscopic surveillance is effective in detecting early cancers. Surgery is reserved for confirmed cancer or high-risk findings rather than being performed prophylactically.
Is it normal for piles to occur after a colectomy?
Yes, after a colectomy, it is possible but not normal for piles (haemorrhoids) to happen. Increased pressure in the rectal veins can cause haemorrhoids. Haemorrhoids are caused by increased pressure in rectal veins, which may result from postoperative constipation, straining, or altered bowel habits. Changes in bowel movement patterns after surgery can contribute to their development. However, colectomy itself does not directly cause haemorrhoids, and they are managed with standard treatments.
Is Colectomy Surgery Covered by Insurance at PACE Hospitals?
Yes, colectomy surgery is generally covered under most health insurance policies at PACE Hospitals, subject to policy terms and approval. Since colectomy is often required for conditions like colorectal cancer or other serious gastrointestinal disorders, it is typically included under private insurance and corporate health plans.
At PACE Hospitals, patients can benefit from:
- Cashless hospitalization facilities with empaneled insurance providers
- Assistance from a dedicated insurance and TPA coordination team
- Pre-authorization support and documentation guidance
- Transparent cost estimates before admission
- Support for government health schemes where applicable
Coverage depends on waiting periods, sum insured limits, critical illness clauses, and policy inclusions. Patients are encouraged to share their insurance details at the time of admission so the hospital’s insurance desk can verify eligibility and streamline approvals.
Why choose PACE Hospitals?
- A Multi-Super Speciality Hospital.
- NABH, NABL, NBE & NABH - Nursing Excellence accreditation.
- State-of-the-art Liver and Kidney transplant centre.
- Empanelled with all TPAs for smooth cashless benefits.
- Centralized HIMS (Hospital Information System).
- Computerized health records available via website.
- Minimum waiting time for Inpatient and Outpatient.
- Round-the-clock guidance from highly qualified super specialist doctors, surgeons and physicians.
- Standardization of ethical medical care.
- 24X7 Outpatient & Inpatient Pharmacy Services.
- State-of-the-art operation theaters.
- Intensive Care Units (Surgical and Medical) with ISO-9001 accreditation.




