Frozen Shoulder - Types, Symptoms, Causes, Diagnosis & Treatment
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. Raghuram - Orthopaedic Consultant, Trauma, Shoulder and Knee Arthroscopic Surgeon, Hip and Knee Joint Replacement Specialist
Frozen shoulder definition
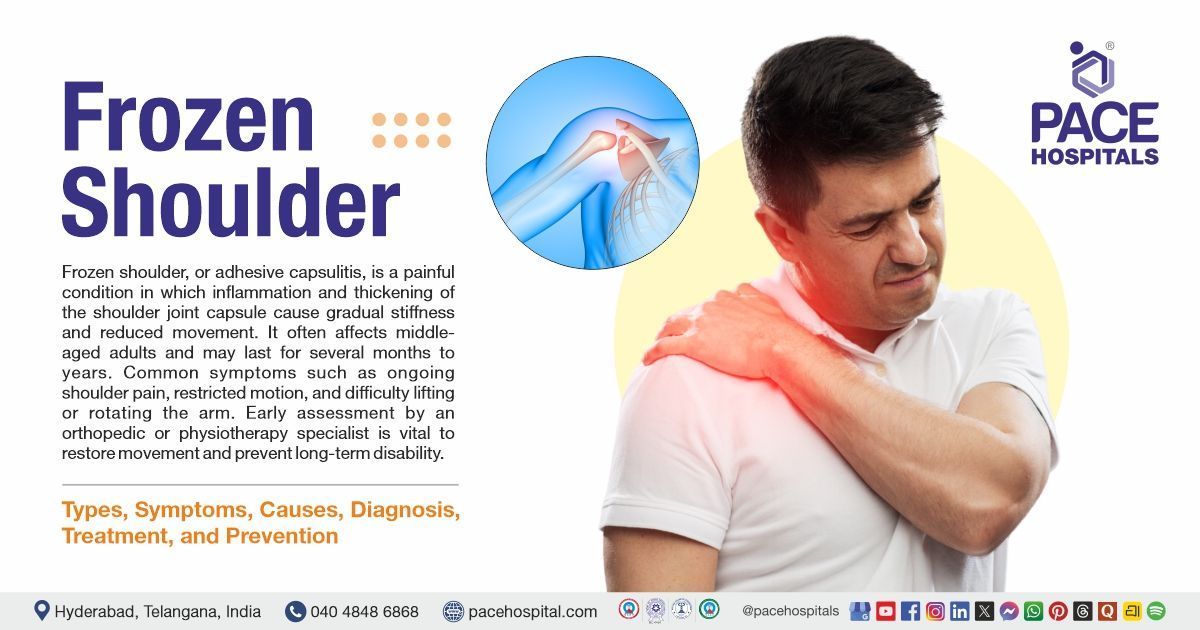
Frozen shoulder, or adhesive capsulitis, is a painful condition causing progressive stiffness and loss of motion in the shoulder joint due to inflammation and thickening of the joint capsule. It usually develops in middle-aged adults and can last for months to years. If not treated, it can limit daily activities and shoulder function.
Common signs of frozen shoulder include persistent shoulder pain, restricted range of motion, and difficulty lifting or rotating the arm. Early evaluation and management by an orthopedic or physiotherapy specialist are essential to restore mobility and prevent long-term disability.
Frozen shoulder meaning
Frozen shoulder, medically referred to as “adhesive capsulitis”. It describes a painful shoulder condition marked by inflammation and thickening of the joint capsule, resulting in stiffness and limited movement. The word “adhesive” refers to sticking or binding, while “capsulitis” combines the Latin word capsula (capsule) with the suffix -itis (inflammation). Thus, “adhesive capsulitis” literally means inflammation of the capsule with adhesion, describing the pathological process that leads to a frozen, immobile shoulder.
Frozen Shoulder Prevalence
Frozen shoulder prevalence worldwide
Adhesive capsulitis, or frozen shoulder, affects approximately 2% to 5% of the general population globally. It most commonly occurs between the ages of 40 and 60 and is more prevalent in women. Among people with diabetes, the prevalence is significantly higher, estimated between 10% and 30%, with some studies reporting rates up to 30%. This condition constitutes a significant cause of shoulder pain and limited motion worldwide.
Prevalence of frozen shoulder in India
Frozen shoulder primarily affects middle-aged adults and is more frequently seen in women, likely due to hormonal and metabolic factors. In India, its prevalence among individuals with diabetes ranges widely—from about 11% to 45%—depending on variations in study populations, diagnostic approaches, and regional health conditions. Frozen shoulder remains an important cause of shoulder pain and disability in India.

Types of frozen shoulder
Frozen shoulder, also known as adhesive capsulitis, can present in various forms depending on the underlying cause. Understanding the type of frozen shoulder is essential for selecting the most appropriate treatment and predicting recovery outcomes. The following are the different types of frozen shoulder:
- Primary frozen shoulder (Idiopathic)
- Secondary frozen shoulder
- Systemic secondary
- Extrinsic (extra-articular) secondary
- Intrinsic (intra-articular) secondary
Primary frozen shoulder (Idiopathic)
- Usually, the onset is idiopathic, which means that there is no known cause for it.
- It usually occurs gradually and is more common in people aged 40 to 60.
- Thyroid issues and diabetes mellitus are two illnesses that may make people more susceptible.
Secondary frozen shoulder
- Develops as a result of a known cause, predisposing factor, or surgical event.
- Common triggers include post-surgery, post-stroke, or post-injury.
- In post-injury cases, altered movement patterns to protect painful structures can affect shoulder motor control, reduce range of motion, and gradually lead to joint stiffness.
Subcategories of secondary frozen shoulder:
- Systemic secondary
- Systemic frozen shoulder is associated with metabolic or systemic conditions, such as diabetes mellitus and other metabolic disorders, which can increase the risk by affecting the health and healing of the shoulder joint tissues.
- Extrinsic (extra-articular) secondary
- Related to factors outside the shoulder that indirectly affect its mobility. Such as cardiopulmonary disease, cervical disc disorders, stroke (CVA), humerus fractures, and Parkinson’s disease.
- Intrinsic (intra-articular) secondary
- Intrinsic frozen shoulder is caused by structural or pathological changes within the shoulder itself, such as rotator cuff disorders, biceps tendinopathy, calcific tendinopathy, and acromioclavicular (AC) joint arthritis.
Frozen Shoulder Symptoms
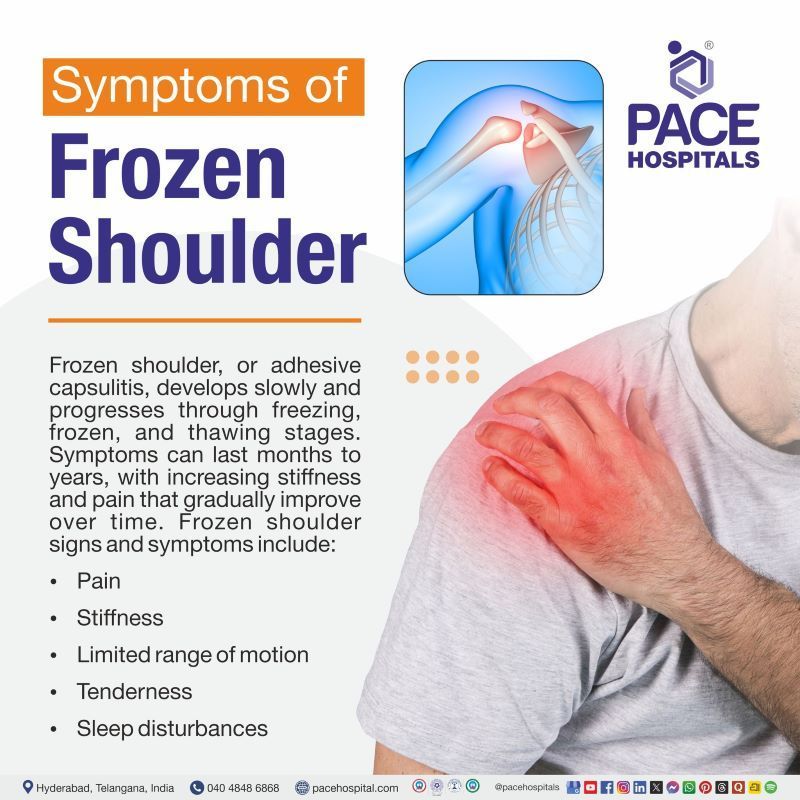
Frozen shoulder, or adhesive capsulitis, develops gradually and typically progresses through three stages — freezing, frozen, and thawing. These symptoms can last from several months to years, gradually improving as the condition moves through its stages. Frozen shoulder signs and symptoms include:
- Pain
- Stiffness
- Limited range of motion
- Tenderness
- Sleep disturbances
Pain: The shoulder often aches, particularly with movement or at night time, due to inflammation of the joint capsule. Pain becomes worsen as the condition advances through the freezing stage.
Stiffness: Progressive tightening of the shoulder capsule reduces elasticity, leading to increasing difficulty with everyday movements. Stiffness is typically most pronounced during the frozen stage.
Limited range of motion: The joint’s range narrows across multiple directions, making overhead reaching, behind-the-back tasks, and rotation hard. This limitation persists even with minimal effort.
Tenderness: Tenderness is usually deep around the joint rather than superficial and may not be evident with external palpation. Symptoms often reflect intra-articular involvement rather than surface injury.
Sleep disturbances: Pain and stiffness can disturb sleep, especially when lying on the affected side. Sleep quality often improves as motion gradually gets back during the thawing phase.
Frozen Shoulder Causes
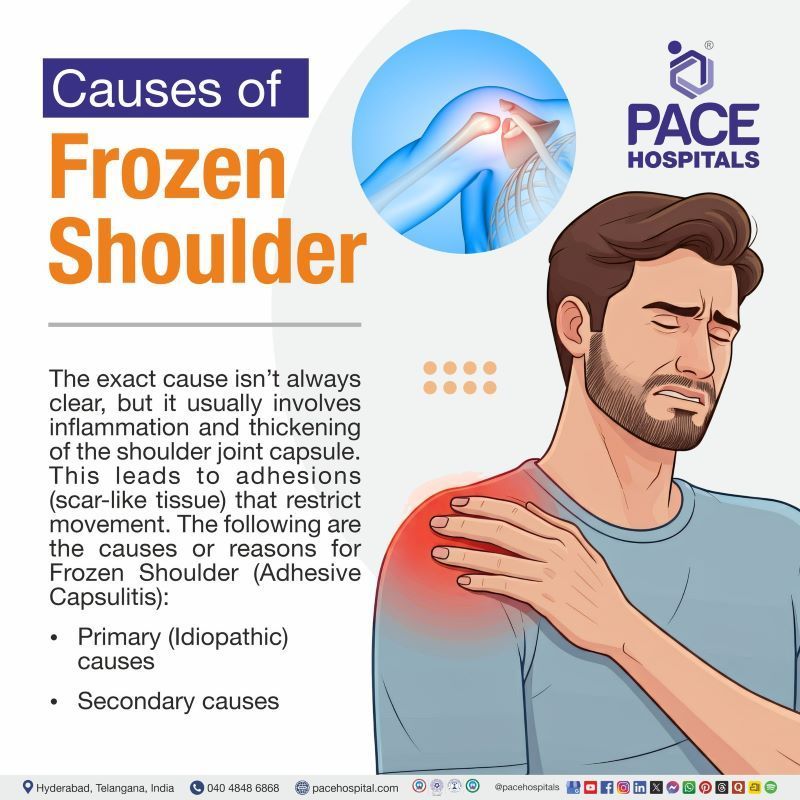
The exact cause isn’t always clear, but it usually involves inflammation and thickening of the shoulder joint capsule. This leads to adhesions (scar-like tissue) that restrict movement. The following are the causes or reasons for Frozen Shoulder (Adhesive Capsulitis):
- Primary (Idiopathic) causes
- Secondary causes
Primary (Idiopathic) causes:
- Unknown specific cause.
- Thought to arise from intrinsic inflammation in the shoulder capsule leading to fibrosis.
- Possibly related to an abnormal immune or inflammatory response.
- Often linked with systemic conditions such as diabetes and thyroid disorders.
Secondary causes:
- Trauma or injury to the shoulder.
- Surgical procedures involving the shoulder or chest wall.
- Prolonged immobilization of the shoulder after injury or surgery.
- Underlying systemic conditions like diabetes mellitus, thyroid dysfunction, Parkinson’s disease, and cardiac disease.
- Musculoskeletal problems around the shoulder, such as rotator cuff pathology or biceps tendonitis.

Frozen Shoulder Risk Factors
Certain medical conditions, injuries, lifestyle or systemic factors can increase a person’s likelihood of developing frozen shoulder by promoting joint stiffness, inflammation, or reduced mobility; the main risk factors of frozen shoulder include:
- Age
- Sex
- Diabetes mellitus
- Thyroid disorders
- Prolonged immobilization
- Shoulder injuries
- Stroke
- Parkinson’s disease
- Dupuytren’s disease
- Complex Regional Pain Syndrome (CRPS)
- Post-surgical causes
- Cardiovascular disease
Age: Frozen shoulder commonly affects middle-aged and older adults, usually between 40 and 60 years, as joint tissues tend to stiffen with age.
Sex: Women are more likely to develop frozen shoulder than men, possibly due to hormonal influences and differences in connective tissue.
Diabetes Mellitus: Diabetes is a strong risk factor, increasing the likelihood of frozen shoulder due to glycation-induced stiffness and long term inflammation in connective tissues.
Thyroid Disorders: Both hypo- and hyperthyroidism can contribute to frozen shoulder by altering metabolism and collagen turnover, leading to joint capsule thickening.
Prolonged Immobilization: Long periods of arm immobility from injury or surgery promote joint capsule contracture and adhesions, triggering frozen shoulder.
Shoulder Injuries: Trauma or repetitive strain may cause inflammation and scarring in the shoulder capsule, predisposing it to frozen shoulder.
Stroke: Post-stroke hemiplegia restricts shoulder movement, increasing the risk of frozen shoulder due to disuse and muscle imbalance.
Parkinson’s Disease: Parkinsonian rigidity and decreased range of motion cause shoulder stiffness and frozen shoulder development.
Dupuytren’s Disease: This fibrotic hand condition shares similar pathological collagen changes and is associated with a higher risk of frozen shoulder.
Complex Regional Pain Syndrome (CRPS): CRPS involving the shoulder can lead to severe pain and restricted movement, increasing the likelihood of secondary frozen shoulder.
Post-Surgical Causes: Surgery around the shoulder or chest can cause local inflammation and scarring, leading to frozen shoulder during recovery.
Cardiovascular Disease: Vascular insufficiency may impair tissue healing and contribute to chronic (long term) inflammation, indirectly increasing frozen shoulder risk.
Frozen Shoulder Complications
Frozen shoulder is a condition characterised by progressive pain and stiffness in the shoulder joint region, that can cause several significant complications. Below are some of the complications of frozen shoulder:
- Persistent pain and stiffness
- Chronic limitation of the range of motion
- Muscle weakness and atrophy
- Sleep disturbance
- Recurrence or bilateral involvement
- Risk of complications from interventions.
Persistent Pain and Stiffness: Some patients may continue to experience pain and limited shoulder movement after treatment. This can last for months or even years and make it hard to do everyday things like getting dressed, grooming, or reaching overhead.
Chronic limitation of the range of motion: The thickening and tightening of the shoulder capsule, along with adhesions, restrict both active and passive motion—primarily external rotation, abduction, and flexion—leading to long-term disability.
Muscle weakness and atrophy: Reduced shoulder use during the painful, stiff phases leads to muscle wasting around the joint, further impairing function.
Sleep disturbance: Pain often worsens at night, causing interrupted sleep, which can exacerbate pain perception and impact mental health due to fatigue and depression.
Recurrence or bilateral involvement: Although uncommon, frozen shoulder can recur in the same shoulder or develop in the opposite shoulder within 5 years, especially in patients with risk factors such as diabetes.
Risk of complications from interventions: Aggressive treatments such as manipulation under anaesthesia or surgery carry risks of complications like fractures, ligament injuries, nerve damage or tendon tears.
Frozen Shoulder Diagnosis
The diagnosis of frozen shoulder involves evaluating the patient’s medical history, conducting a physical examination, and using imaging studies to both confirm the condition and exclude other possible causes of shoulder pain and stiffness. The following diagnostic tests are commonly employed for frozen shoulder:
- Medical history
- Physical examination
- Laboratory tests
- Blood Glucose Tests
- Thyroid Function Tests
- Inflammatory Markers (ESR, CRP)
- Imaging tests
- X-ray (Radiography)
- Magnetic Resonance Imaging (MRI)
- Ultrasound (USG)
- Arthrography (Shoulder Arthrogram)
Frozen Shoulder Treatment
Treatment of frozen shoulder aims to relieve pain, reduce stiffness, and restore normal shoulder movement. Management depends on the stage of the condition, freezing, frozen, and thawing and may take several months for full recovery. The following treatment options include:
- Pharmacological treatment
- Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
- Analgesics
- Corticosteroids
- Physical Therapy
- Initial Phase (Freezing Stage)
- Intermediate Phase (Frozen Stage)
- Final Phase (Thawing/Recovery Stage)
- Surgical Management
- Manipulation Under Anesthesia (MUA)
- Arthroscopic Capsular Release
- Other Non-Surgical Interventions
- Hydrodilatation (Distension Arthrography)
- Physiotherapy Modalities
- Acupuncture
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support

Frozen Shoulder Prevention
Frozen shoulder can be prevented by keeping the shoulder mobility through regular exercises and early movement after injury or surgery. Controlling medical conditions and avoiding prolonged immobilization also reduce the risk of stiffness. Below are the preventive measures for frozen shoulder:
- Regular Shoulder Exercises and Stretches
- Early Mobilisation After Injury or Surgery
- Control Underlying Medical Conditions
- Avoid Prolonged Immobilisation
- Good Posture and Ergonomics
Regular Shoulder Exercises and Stretches: Performing gentle stretching and range-of-motion exercises keeps the shoulder flexible and prevents stiffness. Consistency helps maintain normal joint function over time.
Early Mobilisation After Injury or Surgery: Moving the shoulder soon after injury or surgical procedures prevents adhesions and loss of motion. Gradual exercises help restore function without causing pain.
Control Underlying Medical Conditions: Managing conditions such as diabetes and thyroid disorders can lower the risk of developing frozen shoulder. In order to avoid joint stiffness and inflammation, prompt and adequate medical attention is essential.
Avoid Prolonged Immobilization: Keeping the shoulder or arm in a sling for long periods can result in stiffness and restricted movement. Limiting immobilization helps preserve normal shoulder mobility.
Good Posture and Ergonomics: Maintaining proper posture and ergonomic habits decreases strain on the shoulder joint. This helps prevent overuse injuries that can trigger stiffness and pain.
Difference between Frozen Shoulder and Rotator Cuff Injury
Frozen shoulder vs rotator cuff
Frozen shoulder causes stiffness and restricted movement in all directions, developing gradually over months. Rotator cuff injury causes pain and weakness with specific movements due to tendon damage. Below are some of the parameters that help in differentiating Frozen Shoulder and Rotator Cuff Injury:
| Feature | Frozen Shoulder | Rotator Cuff Injury |
|---|---|---|
| Cause | Caused by the tightening and thickening of the shoulder capsule, leading to progressive stiffness. | Caused by inflammation, strain, or tearing of the rotator cuff tendons due to injury, overuse, or aging. |
| Key Symptoms | The main symptom is stiffness, with a gradual loss of movement in all directions. | Main symptoms are pain and weakness, especially during lifting or reaching. |
| Movement Limitation | Both active and passive movements are restricted because the joint itself becomes stiff. | Main symptoms are pain and weakness, especially during lifting or reaching. |
| Onset & Recovery | Develops slowly over months and may take 1–3 years to fully resolve. | It can start suddenly or gradually; recovery is usually weeks to months, unless a major tear requires surgery. |
| Common In | More common in people with diabetes, thyroid disorders, or those with prolonged immobilization. | Common in athletes, older adults, and people doing repetitive overhead activities. |
Frequently Asked Questions (FAQs) on Frozen Shoulder
What is frozen shoulder?
The condition also known as adhesive capsulitis or frozen shoulder is characterized by thickening, tightening, and inflammation of the connective tissue surrounding the shoulder joint. This leads to pain and a marked reduction in shoulder mobility, often interfering with daily activities. The condition typically develops gradually over several months to years.
How to cure frozen shoulder?
Treatment includes physical therapy to improve flexibility and reduce pain, anti-inflammatory medications, and, sometimes, corticosteroid injections. In some persistent conditions , surgical intervention may be considered. Recovery usually happens in stages over 1 to 3 years with proper care.
What is the main cause of frozen shoulder?
The exact cause is unclear, but it usually follows injury, surgery, or prolonged immobilization reducing shoulder movement. It is linked to inflammation and scarring of the shoulder capsule, sometimes associated with conditions like diabetes or thyroid disorders.
How to prevent frozen shoulder?
Prevention includes keeping the shoulder moving after injury or surgery, regular gentle exercises, and avoiding prolonged immobilization. Managing underlying health issues like diabetes and seeking early treatment for shoulder pain also helps reduce risk.
Is frozen shoulder hereditary?
Frozen shoulder is not generally considered hereditary and is usually linked to medical conditions like diabetes or thyroid disorders, as well as previous shoulder injuries. While family history is not a major factor, certain health conditions or lifestyle factors shared within families may slightly influence the risk.
How much time does it take to cure frozen shoulder?
Frozen shoulder usually takes 1 to 3 years to fully recover, moving through the freezing, frozen, and thawing stages. With consistent treatment, such as physical therapy, stretching exercises, and occasionally steroid injections, many people begin to notice reduced pain and improved mobility even before the condition completely resolves.
How to sleep with a frozen shoulder?
Sleeping is easier by avoiding the painful side, using pillows to support the arm, and maintaining comfortable positions that limit shoulder strain. Some people find relief lying on their back with a pillow under their arm or using a recliner to improve shoulder positioning.
What are the symptoms of frozen shoulder?
Symptoms develop in three stages: pain worsening initially, followed by stiffness with decreased pain, then gradual improvement of motion. Common signs include dull aching shoulder pain, stiffness, and limited range of motion, especially difficulty reaching overhead or behind the back.
Can massage help frozen shoulder?
Massage may provide temporary pain relief and loosen tight muscles, but it is not a primary treatment. It can be helpful when combined with physical therapy to enhance blood flow and reduce muscle tension, but it should be done cautiously under professional guidance.
➡ Read More: How to cure frozen shoulder quickly
What foods are good for frozen shoulder?
Anti-inflammatory foods like fruits, vegetables, omega-3-rich fish, nuts, and whole grains may support healing by reducing inflammation. Maintaining a healthy diet supports overall recovery, though no specific foods cure frozen shoulder (adhesive capsulitis).
What is the best exercise for frozen shoulder?
Gentle stretching exercises such as pendulum swings, wall climbs, and shoulder rolls are recommended. These exercises restore range of motion and mobility and should be performed consistently under physiotherapist supervision to avoid worsening symptoms.
What does the term ‘adhesive capsulitis vs frozen shoulder’ mean?
Adhesive capsulitis and frozen shoulder are the same condition. The term adhesive capsulitis is the medical name describing the thickening and tightening of the shoulder capsule, while frozen shoulder is the common term referring to the symptoms of pain and stiffness.
Is physiotherapy good for frozen shoulder?
Yes, physiotherapy is a key treatment for improving movement, reducing pain, and speeding up recovery. Targeted exercises and therapies effectively restore shoulder function.
Does ankylosing spondylitis lead to frozen shoulder?
Although it doesn't directly cause frozen shoulder, the inflammatory condition ankylosing spondylitis may raise the risk by causing persistent joint stiffness and irritation. The surrounding tissues may be impacted by persistent inflammation, increasing the shoulder's susceptibility to restricted mobility.
When to consult a doctor for frozen shoulder?
Consult a doctor for frozen shoulder if shoulder pain or stiffness persists for several weeks, gets worse, or begins to limit daily activities. Signs that need attention include:
- Difficulty lifting the arm or rotating the shoulder
- Increasing stiffness that restricts movement
- Persistent or worsening shoulder pain
- Pain that disturbs sleep
- Trouble performing routine tasks like dressing or reaching overhead
If these symptoms continue, it is important to consult a frozen shoulder specialist who can evaluate the condition and recommend the right treatment plan. Seek emergency medical attention if the shoulder pain follows an injury, is accompanied by swelling, redness, fever, or sudden inability to move the arm. A general care physician, orthopedic specialist, or physiotherapist can provide the best frozen shoulder treatment to control symptoms and prevent complications.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868