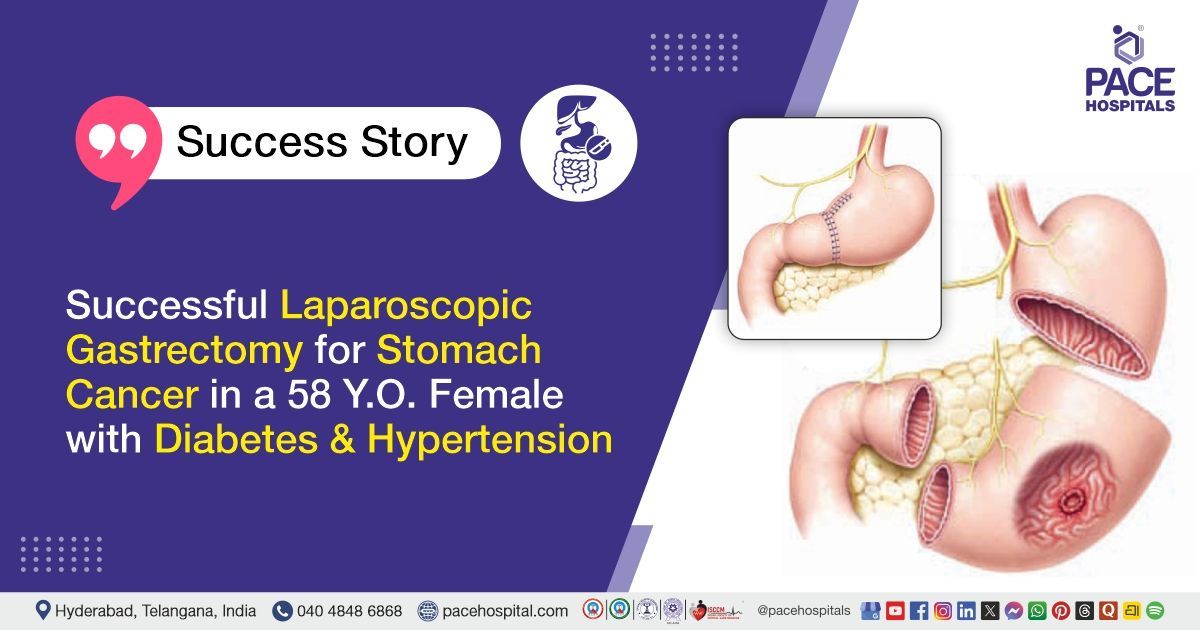
Laparoscopic Gastrectomy for Stomach Cancer in a 58 Y.O. Female
PACE Hospitals
The PACE Hospitals' expert gastroenterology team successfully performed a laparoscopic subtotal gastrectomy on a 58-year-old female patient diagnosed with adenocarcinoma of the stomach. The aim was to remove the cancerous portion with clear margins, prevent disease spread, and preserve healthy tissue for better recovery and digestive function.
Chief Complaints
A 58-year-old female patient with a body mass index (BMI) of 18 presented to the Gastroenterology Department at PACE Hospitals, Hitech City, Hyderabad, with complaints of abdominal discomfort for 3 months, associated with abdominal tightness, loss of taste sensation, and mild epigastric pain. She also reported constipation for 3 months, characterised by incomplete evacuation, hard stools, and the need for straining.
Past Medical History
The patient had a known history of
type 2 diabetes mellitus &
Hypertension and was on regular treatment.
On Examination
On examination, the patient was conscious, coherent, and oriented. Vital signs were stable, with elevated blood pressure noted. Abdominal examination revealed a soft and non-tender abdomen with no significant abnormal findings.
Diagnosis
Upon admission to PACE Hospitals, the patient was thoroughly evaluated by the Gastroenterology team, presenting with a three-month history of abdominal discomfort associated with abdominal tightness, loss of taste sensation, mild epigastric pain, and constipation characterized by incomplete evacuation and hard stools. Based on the clinical presentation, there was a strong suspicion of underlying gastric pathology, particularly a malignant lesion of the stomach.
A comprehensive diagnostic workup was performed. Upper gastrointestinal (UGI) endoscopy revealed a deep, irregular gastric ulcer measuring approximately 4 × 4 cm along the lesser curvature extending to the posterior wall. A biopsy taken for histopathological examination confirmed moderately differentiated tubular adenocarcinoma of the stomach. Colonoscopy was a normal study. A PET-CT scan was performed, which was suggestive of non-metastatic disease. Laboratory investigations - including complete blood picture (CBP), renal function tests (RFT), liver function tests (LFT), serum electrolytes, blood urea, serum creatinine, serum magnesium, bleeding time (BT), and clotting time (CT) - were within normal limits, with mild leukocytosis noted on complete blood picture.
Based on the confirmed diagnosis, the patient was advised to undergo Stomach Cancer Treatment in Hyderabad, India, under the expert care of the Gastroenterology Department.
Medical Decision Making (MDM)
After a detailed consultation with the consultant gastroenterologists, Dr. Govind Verma, Dr. Padma Priya, and Dr. M Sudhir, along with cross-consultation from Dr. Suresh Kumar S, Surgical Gastroenterologist, Dr. Tripti Sharma, Endocrinologist, and Dr. Snigdha Panuganti, General Physician, a thorough evaluation was conducted considering the patient’s complaints of abdominal discomfort, epigastric pain, abdominal tightness, constipation, and loss of taste sensation for three months.
All relevant clinical findings, including vital signs, systemic examination, laboratory investigations (complete blood picture, renal function tests, liver function tests, serum electrolytes, serum magnesium, bleeding time, clotting time), imaging (PET-CT), endoscopy, colonoscopy, and histopathology, were reviewed.
Based on this comprehensive assessment, it was determined that laparoscopic subtotal D2 gastrectomy was identified as the most appropriate intervention to remove the malignant lesion in the stomach, achieve oncological clearance, and prevent disease progression. The surgical gastroenterology team provided cross-consultation to ensure procedural feasibility, safety, and optimal lymph node dissection.
The patient and her family members were counselled regarding the diagnosis of
adenocarcinoma of the stomach (non-metastatic), the surgical procedure, potential risks, post-operative care, dietary modifications, blood sugar and blood pressure management, and the expected improvement in symptoms and overall prognosis following the intervention.
Surgical Procedure
Following the decision, the patient was scheduled for Laparoscopic subtotal gastrectomy Surgery in Hyderabad at PACE Hospitals, under the expert care of the Gastroenterology Department.
The procedure involved the following steps:
- Pre-peritoneal Dissection and Abdominal Inspection: Under all aseptic precautions, the peritoneal cavity was accessed laparoscopically. A thorough inspection of the entire abdomen was performed to evaluate the extent of disease and rule out any metastasis. The omentum was mobilized carefully along the transverse colon to provide adequate access to the stomach and surrounding structures.
- Mobilization and Ligation of Vessels: The right and left gastroepiploic veins were identified and ligated to control vascular supply. The left gastric artery was dissected and ligated, ensuring safe removal of the tumor-bearing portion of the stomach while minimizing intraoperative bleeding.
- Gastric Resection with Endoscopic Guidance: Endoscopic guidance was utilised to confirm accurate transection of the stomach. The diseased segment along the lesser curvature, including all lymph nodes up to station 9, was resected. A linear stapler was applied at the duodenal end to complete the resection safely and maintain gastrointestinal continuity.
- Specimen Retrieval and Drain Placement: The resected gastric specimen was removed through a small incision near the umbilicus. A surgical drain was placed in the abdominal cavity to monitor postoperative fluid collection and ensure early detection of any complications.
- Hemostasis and Closure: Hemostasis was meticulously achieved to prevent postoperative bleeding. The abdominal wall was closed, and the skin was secured using skin staplers.
Postoperative Care
The patient’s postoperative period was uneventful. She was closely monitored in the Surgical Intensive Care Unit (SICU) for respiratory status to prevent aspiration, vital signs, and drain output, which was removed once minimal, indicating satisfactory healing. Referrals were taken with a physician for management of newly diagnosed hypertension, and an endocrinologist for uncontrolled blood sugars, and all recommendations were implemented.
She received treatment for hydration, infection prevention, gastric acid suppression, pain management, blood sugar control, and bowel regulation. The patient remained hemodynamically stable, symptomatically improved, tolerated diet and activity, and exhibited no postoperative complications, allowing for safe transfer to the ward and eventual discharge with instructions regarding medications, diet, and follow-up.
Discharge Medications
The patient was advised treatment for infection prevention for a short duration, suppression of gastric acid, management of pain as needed, and supplementation to support general health. She was prescribed therapy for blood pressure control and ongoing management of blood sugar, including both long-acting and mealtime control, along with additional medication to maintain adequate blood sugar levels. Measures were also advised to ensure regular bowel movements and gastrointestinal comfort. All treatments were to be taken as per the prescribed schedule, with follow-up monitoring to adjust therapy as needed.
Dietary Advice
The patient was advised to follow a high-fiber diet, including green leafy vegetables, with meals prepared in a normal to moderately spicy manner, and to include one fruit per day to support digestive health and overall nutrition.
Emergency Care
The patient was informed to contact the emergency ward at PACE hospitals in case of emergency or having any symptoms like fever, vomiting, chest pain and abdominal pain
Review and Follow-up Notes
The patient was advised to return for a follow-up visit with the Gastroenterologist in Hyderabad at PACE Hospitals after 1 week. Additionally, follow-up visits were recommended with the Surgical Gastroenterology and Endocrinology departments after one week to monitor recovery, manage ongoing health concerns, and adjust treatment as needed.
Conclusion
This case highlights a patient with localized gastric adenocarcinoma and comorbid diabetes and hypertension. She underwent a successful laparoscopic subtotal gastrectomy with complete lymph node clearance. Postoperative recovery was stable with multidisciplinary management for blood pressure and blood sugar. The patient was discharged hemodynamically stable with instructions for diet, medications, and follow-up.
Multidisciplinary Management in Localized Gastric Cancer
Management of localized gastric cancer benefits significantly from a multidisciplinary approach. Early diagnosis and accurate staging by a gastroenterologist guide the choice of surgical and medical interventions. Careful surgical planning and technique are essential to achieve complete tumor removal while minimizing complications. Postoperative monitoring of vital signs, nutrition, wound healing, and comorbid conditions supports optimal recovery.
Coordination with a
gastroenterologist/gastroenterology doctorand other specialists for blood sugar, blood pressure, and systemic issues ensures holistic care and reduces postoperative risks. Patient education, diet counseling, and structured follow-up further enhance outcomes and long-term wellbeing. Integration of oncologists, gastroenterologists, endocrinologists, and dietitians ensures that both disease-specific and general health aspects are addressed, improving quality of life and prognosis.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868