Sjogren’s Syndrome: Symptoms, Causes, Treatment & Prevention
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. Shweta Bhardwaj - Consultant Rheumatologist and Clinical Immunologist
Sjogren's syndrome definition
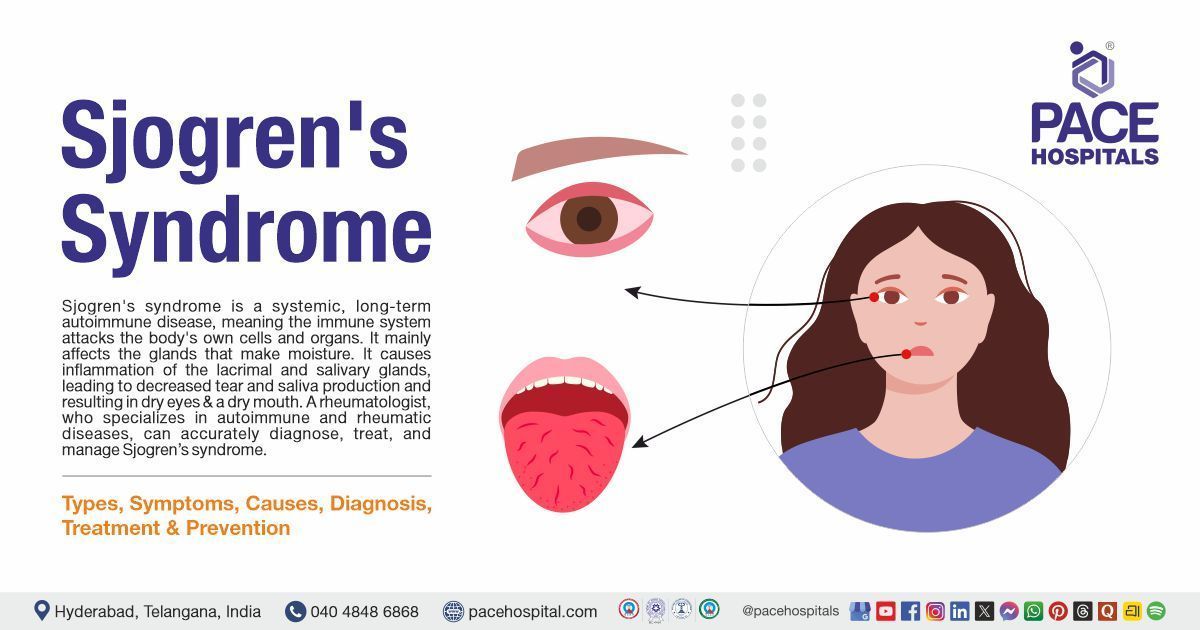
Sjogren's syndrome is a long-term systemic autoimmune disease, meaning the immune system attacks the body's own cells and organs. It damages the glands that produce and control moisture, causing dryness throughout the body, especially the eyes and mouth. This disease causes inflammation of the lacrimal glands (which secrete tears) and the salivary glands (which secrete saliva). This leads to decreased tear and saliva production, causing dryness of the eyes and mouth.
The leading cause of Sjogren's syndrome is unknown; genetic, hormonal, or environmental factors can cause it.
A Rheumatologist, a doctor specialised in autoimmune and rheumatic diseases, can accurately diagnose, treat and manage Sjogren's syndrome.
Sjogren's syndrome meaning
Sjogren’s syndrome is pronounced as ‘show-grins’. It is named after Swedish eye doctor Dr Henrik Sjogren.
Sjogren's Syndrome Prevalence
Sjogren's syndrome prevalence worldwide
Sjogren syndrome is an autoimmune disorder affecting about 0.03%–0.09% of the global population (30–90 per 100,000. It occurs worldwide without any racial or geographic bias and is more common in women than men (≈9:1). Symptoms are most commonly seen between ages 45 and 55, and most of the individuals with this disease also have other autoimmune diseases like rheumatoid Arthritis and lupus.
Sjogren's syndrome prevalence in India
Indian studies show that Sjogren's syndrome is less frequently diagnosed compared to Western countries. Hospital-based studies suggest that Sjogren's syndrome is reported in approximately 0.5–1% of patients attending rheumatology clinics.
Types of Sjogren's Syndrome
Sjogren's syndrome classification is mainly based on the presence of the syndrome alone or in association with other autoimmune diseases. It is classified into two types:
- Primary Sjogren's syndrome
- Secondary Sjogren's syndrome
Primary Sjogren's syndrome
This develops independently without other autoimmune diseases, featuring lymphocytic infiltration of exocrine glands. This syndrome commonly presents with sicca symptoms. Sicca refers to dryness of the eyes and mouth due to inflammation. Most of the affected individuals also have signs and symptoms in organs ranging from the salivary and lacrimal glands to the joints, skin, lungs, nervous system, gastrointestinal tract, and kidneys.
Secondary Sjogren's syndrome
This indicates that Sjogren's syndrome occurs with other autoimmune diseases, such as systemic lupus erythematosus, rheumatoid Arthritis, and scleroderma (a skin disease).

Sjogren's Syndrome Symptoms
The signs and symptoms of Sjogren’s syndrome are different for different individuals. There are two main symptoms:
- Dry mouth (xerostomia)
- Dry eyes
Sjogren's syndrome may also affect other parts of the body, including:
- Vaginal dryness
- Joint pain or muscle weakness
- Heartburn
- Difficulty in breathing/shortness of breath
- Fatigue
- Dry skin
- Swelling of glands
Dry mouth (xerostomia): Dry mouth occurs when the salivary glands are not able to produce enough saliva, which can lead to difficulty swallowing and speaking and may also cause dental cavities and oral thrush (candidiasis, a fungal infection).
Dry eye: Eyes become dry when tear production is reduced, leading to a burning sensation, redness, increased blinking, and sensitivity to light. Blurred vision may also occur.
Vaginal dryness: Women with Sjogren's syndrome have vaginal dryness, which is more common during menopause, causing thinning of pubic hair and decreased vaginal moisture.
Joint pain or muscle weakness: Joint pain, swelling and stiffness of joints in hands and wrists occur. Individuals with Sjogren's syndrome have muscle discomfort.
Heart burn: Heartburn, or acid reflux, is one of the symptoms of Sjogren's disease. If untreated, it may lead to a severe condition called gastroesophageal reflux disease (GERD).
Difficulty in breathing/shortness of breath: A serious complication called Interstitial Lung Disease (ILD), which causes inflammation of the lung parenchyma, the tissue of the lung. When the tissue scars, it becomes stiff and thick, making it difficult for oxygen to be supplied. This causes shortness of breath; this form of lung disease is more common in individuals with Sjogren's syndrome.
Fatigue: It is a symptom of Sjogren's syndrome and can impact the quality of life. This fatigue is severe and persistent, and it causes challenges with daily activities.
Dry skin: Dry skin, or xerosis, is a symptom of Sjogren's disease, which causes the skin to become dry, rough, and scaly.
Swelling of glands: Swelling of the salivary glands, which are presented in the jaw or below the ears, occurs in individuals with Sjogren's syndrome. This causes pain and tenderness in the area.

Causes of Sjogren's Syndrome
The exact cause of Sjogren's syndrome is not known. Some of the factors that cause Sjogren's syndrome are:
- Genetic factors
- Hormonal factors
- Environmental factors
- Other factors
Genetic factors: Sjogren's syndrome is not directly inherited, but it does play a significant role in its pathogenesis. For example, if a person has a defective gene linked to Sjogren's syndrome and then gets an infection, the immune system will respond. WBCs usually attack the infection, but because of the defective gene, they target healthy cells in glands that secrete saliva and tears. This causes Sjogren's syndrome symptoms to keep increasing unless they are treated. People with autoimmune diseases and thyroid diseases have a higher risk of this disease.
Hormonal factors: Hormonal factors can also play an important role in this disease. Women are more affected than men, causing inflammation and gland dysfunction.
Environmental factors: Environmental factors can also trigger this disease. The most common are infectious agents. Environmental pollution, stress, vitamin D deficiency, and silicone are the factors that affect this disease.
Other factors: Viral infections like the hepatitis C virus and Epstein-Barr virus (EBV) may cause autoimmune reactions, which cause the immune system to attack its own healthy tissues.

Risk Factors of Sjogren's Syndrome
Sjögren's syndrome results from complex interactions between hormones, environmental triggers, and genetic predisposition that impair immune tolerance and cause glandular inflammation. Several risk factors may contribute to the development of Sjogren's syndrome. Some of them are:
- Age
- Sex
- Autoimmune diseases
Age: Although Sjögren's syndrome may occur at any age, it usually affects people over 40, especially between the ages of 45 and 55. It is uncommon in children and young adults. Systemic symptoms may be more severe in early-onset cases.
Sex: Women are nine to ten times more likely than men to develop Sjögren's syndrome, most likely as a result of immunomodulatory effects that increase the production of autoantibodies. Changes following menopause may also play a role in the manifestation of disease.
Autoimmune diseases: Some autoimmune diseases also cause Sjogren's syndrome, such as Rheumatoid Arthritis (RA) and Psoriatic Arthritis.
Complications of Sjogren's Syndrome
Sjogren's syndrome is a chronic autoimmune disease, leads to a wide range of complications. The potential complications are recognized for the long-term management. Understanding these outcomes helps reduce and improve the quality of life for affected individuals. Complications of this syndrome include:
- Oral complications
- Eye complications
- Neurological complications
- Haematological complications
- Musculoskeletal
- Dermatologic
- Renal
- Pulmonary
- Non-Hodgkin lymphoma
Oral complications
- Dental cavities: Saliva protects teeth from bacteria, but due to this syndrome, the mouth becomes dry and prone to developing dental cavities.
- Oral infections like candidiasis, which is a fungal infection, are associated with dry mouth.
- A reduction in saliva production causes reduced lubrication, which interferes with speech and swallowing.
- saliva is responsible for taste; reduced saliva alters the taste.
Eye complications
- Vision problems: Dry eyes lead to light sensitivity and blurred vision.
- Keratitis, which is a bacterial infection, can occur due to impaired tear defence
Neurological complications
In Sjogren’s syndrome, both the central and peripheral nervous systems are involved. Numbness, burning sensation, tingling in the hands and feet.
Haematological complications
Patients with Sjogren's syndrome have a lifetime risk of developing non-Hodgkin B-cell lymphoma (Blood cancer).
Some of the less common complications are inflammation of the lungs, kidneys and liver, which leads to pneumonia, kidney dysfunction, hepatitis or cirrhosis.
Musculoskeletal complications
Most of the patients with Sjogren's syndrome have Arthritis (inflammation and stiffness of joints) and myalgia (pain in the muscles).
Dermatologic complications
More common complications of this syndrome include xeroderma (dry skin), eyelid dermatitis, and Raynaud phenomenon (narrowing of blood vessels).
Renal complications
In Sjogren's syndrome, kidney complications are very rare. Those include tubulointerstitial nephritis (inflammation of the kidney and its surrounding tissues), distal renal tubular acidosis (RTA) and membranoproliferative glomerulonephritis.
Pulmonary complications
Lung involvement has a wide range of prevalence in Sjogren’s syndrome. Cough and dryness-related dyspnea are symptoms of this disease.
Non-Hodgkin lymphoma
Non-Hodgkin lymphoma (Blood cancer) is the most serious complication of the Sjogren’s syndrome. Increased risk is seen in patients with this disease when compared to the general population.
Sjogren's Syndrome and Pregnancy Complications
Women with an autoimmune disease like Sjogren's syndrome experience more complications than women without an autoimmune disease. The risk of poor fetal outcome is seen in these patients. Women with this disease should be counselled about the risks and the need to control the disease before planning pregnancy.
Sjogren's Syndrome Diagnosis
To diagnose Sjogren's syndrome, rheumatologists generally use clinical evaluation and some specialised tests.
The following are the steps included in the Sjogren’s syndrome diagnosis criteria:
- Medical history
- Physical examination
- Laboratory investigations: Blood tests include:
- SS-A(Ro) and SS-B (La) antibodies
- Antinuclear antibody (ANA)
- Rheumatoid factor
- Complete Blood Count (CBC)
- Erythrocyte Sedimentation Rate (ESR)
- C-Reactive Protein (CRP)
- Immunoglobulins
- Serum Protein Electrophoresis
- Imaging studies
- Sialogram/sialography
- Diagnostic procedure/ clinical test
- Schirmer tear test
- Ocular surface staining
- Labial gland biopsy
Sjogren's Syndrome Treatment
Non-pharmacological treatment
- Exposure to wind or very dry environments can cause dry eyes; avoiding them helps prevent dryness.
- Sipping water or liquids often maintains hydration
- Drinks containing caffeine, tea or soda are avoided to manage dry mouth
- Tobacco or alcohol, which may dry out the mouth, should be avoided.
- Chew sugarless candy or gums, which stimulate saliva
Pharmacological treatment
Sjogren's syndrome has no cure; the treatment mainly focuses on relieving symptoms. Treatment varies depending on which part of the body is affected.
Eye:
- Artificial tears
- Eye ointments
- Plugs
Mouth:
- Artificial saliva
- Saliva production stimulators
- Antifungal medications
Some of the pain relievers or over-the-counter medications are also used for symptomatic pain relief.
- Over the counter or prescribed pain relievers
- Corticosteroids
- Disease-modifying anti-rheumatic drugs (DMARDs) and anti-malarial drugs
- Acid reflux medications
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support
Sjogren's Syndrome Prevention
There is no cure for Sjogren's syndrome, but it can be managed, and people can live an everyday life. Some of the tips that can make it easier for people with Sjogren's syndrome include:
For dry mouth
- Advised to stop smoking, which can irritate and cause dryness of the mouth.
- Increase in fluid intake to maintain hydration
- Dry mouth can cause dental cavities, so brush your teeth after every meal.
- Chewing gum or sugar-free candy can stimulate saliva production, helping prevent dry mouth.
- Consult the physician if any symptoms of oral thrush (candidiasis), such as soreness, burning, or white patches, are seen.
For dry eyes
- To relieve dry eyes, use artificial tears or lubricants.
- Increase humidity: To prevent the eyes and mouth from drying out, raise indoor humidity and avoid exposure to blowing air.
- If any symptoms of blepharitis (inflammation of the eyelids) are seen, use warm compresses to relieve discomfort.
For dry skin
- Avoid hot water baths to prevent dry skin.
- Apply moisturiser to prevent dryness of the skin
For vaginal dryness
- Vaginal moisturisers or lubricants are used to prevent dryness of the vagina.
Difference between Mikulicz Disease and Sjogren's Syndrome
Mikulicz disease vs Sjogren's syndrome
Both are autoimmune diseases that affect the lacrimal and salivary glands, causing enlargement and dryness. Despite similar clinical features, they differ in their pathophysiology, immunologic markers, and treatment. Below are the key differences between Mikulicz disease and Sjogren's syndrome.
| Parameters | Mikulicz disease | Sjögren's syndrome |
|---|---|---|
| Definition | Chronic autoimmune disease causes swelling of the salivary and lacrimal glands. It can also affect other parts of the body. | Chronic autoimmune disease that damages the moisture-producing glands, such as the lacrimal glands (glands that secrete tears) and the salivary glands (glands that secrete saliva). This leads to decreased tear and saliva production, causing dryness of the eyes and mouth. |
| Etiology | The cause is unknown; scleroderma, Sjogren's syndrome, and tuberculosis may cause this disease. | Genetic, environmental, and autoimmune diseases |
| Pathophysiology | IgG4-related autoimmune disease that causes infiltration of IgG4 plasma cells into salivary and lacrimal glands, which causes swelling of these glands. | Attacks on exocrine glands lead to dryness of the eyes and mouth. |
| Symptoms | Swelling and dryness of the eyes and mouth. | Dry eyes, dry mouth, fatigue and dry skin |
| Diagnosis | Different for different individuals includes autoantibody testing, serum IgG4 levels, and other tests. | Different to different individuals Example: Sialogram, Schirmer test |
| Treatment | Artificial tears, eye drops, and symptomatic treatment. | Artificial tears, Eye ointments, plugs |
Difference between Sjogren's Syndrome and Systemic Lupus Erythematosus
Sjogren's syndrome vs Systemic Lupus Erythematosus
Both are autoimmune diseases, but they differ in their targets and systemic involvement. Sjogren's syndrome affects exocrine glands like lacrimal and salivary, whereas Systemic Lupus Erythematosus effects on multiple organs, including the joints, skin, joints, blood, and kidneys. Distinguishing between the two is essential for treatment strategies. Below are the key differences between Sjögren's syndrome and Systemic lupus erythematosus.
| Parameters | Sjögren's syndrome | Systemic lupus erythematosus |
|---|---|---|
| Definition | Long-term autoimmune disease that damages the moisture-producing glands, such as the lacrimal glands (glands that secrete tears) and the salivary glands (glands that secrete saliva). This leads to decreased tear and saliva production, causing dryness of the eyes and mouth. | A long-term autoimmune disease that can affect all parts of the body. The immune system attacks its own body cells, causing inflammation and damage to the tissues affecting the skin, heart, kidneys, joints, lungs and brain. |
| Etiology | Genetic, environmental, and autoimmune diseases | Genetic, environmental, and autoimmune disease |
| Pathophysiology | Attacks on exocrine glands lead to dryness of the eyes and mouth. | Loss of self-tolerance causes chronic inflammation and tissue damage |
| Symptoms | Dry eyes, dry mouth, dry skin, fatigue | Butterfly rash, Arthritis, fatigue, swollen glands |
| Diagnosis | Different to different individuals Example: sialogram, Schirmer test | Different to different individuals Example: ANA with autoantibodies |
| Treatment | Artificial tears, Eye ointments, plugs | Pain management and immunosuppressants |
Frequently Asked Questions (FAQs) on Sjogren’s Syndrome
What is Sjogren's syndrome?
Sjogren's syndrome is an autoimmune disease that damages the glands that produce and regulate moisture in the body. It is a chronic disease that causes the inflammation of the glands that produces saliva and tears.
Is Sjogren's syndrome hereditary?
The inheritance of Sjogren's syndrome is unknown, but genetics plays a significant role. Autoimmune diseases can pass through generations in families; relatives of autoimmune disease patients are at higher risk.
What are the symptoms of Sjogren's syndrome?
Symptoms of Sjogren's syndrome are different for different people. Dry mouth, dry eyes, dry skin, fatigue, vaginal dryness in women, and other symptoms are the most common.
Who has Sjogren's syndrome?
Sjogren's syndrome can be seen in all age groups, including children, but is most commonly seen in women over the age of 40.
Is Sjogren's syndrome curable?
There is no cure for this disease; treatment of Sjögren's syndrome mainly depends on the symptoms. Some over-the-counter or prescribed medications are used for symptomatic relief.
Is Sjogren's syndrome life-threatening?
Sjogren's syndrome is a lifelong disease; there is no cure for this disease. However, you can prevent this disease from getting worse by avoiding some medications that increase the symptoms, alcohol, caffeine and preventing exposure to dry environments.
What does Sjogren's syndrome do to the body?
As it is an autoimmune disease, WBCs target and attack glands that produce moisture, such as the lacrimal glands (tear-producing glands) and salivary glands (saliva-producing glands). So the damaged glands no longer produce saliva and tears, leading to dryness of the mouth and eyes.
What are the risk factors of Sjogren's syndrome?
Some of the risk factors that increase Sjogren's syndrome include age, sex, and autoimmune diseases. People of all age groups can have this disease, but mostly those over 40. Females are more likely to have this disease than men. Some of the autoimmune diseases, like rheumatoid Arthritis and lupus, can cause this disease.
Can a person with Sjogren's syndrome have other autoimmune diseases?
Many autoimmune diseases overlap and share symptoms. Sjogren's syndrome is an autoimmune disease associated with other autoimmune diseases, such as Rheumatoid Arthritis and systemic lupus erythematosus, and can cause the same symptoms as joint pain and fatigue.
What is the difference between primary and secondary Sjögren's syndrome?
In primary Sjogren's syndrome, the disease occurs in the absence of other autoimmune diseases. In contrast, in secondary Sjogren's syndrome, it occurs along with autoimmune diseases such as scleroderma, rheumatoid Arthritis, and systemic lupus erythematosus.
Why is Sjögren's disease more common in women?
Sjogren's syndrome mostly occurs in women than in men. Most cases of Sjogren's syndrome in women occur after menopause, over the age of 55-60. Estrogen and androgen are the hormones responsible for protecting exocrine glands against inflammation. In menopause, there is a decline in these hormones, leading to an increased risk of Sjogren's syndrome.
Can environmental factors worsen Sjogren's syndrome?
Yes, several environmental factors are involved in Sjogren's syndrome; the most common are infectious agents. Environmental pollution, stress, vitamin D deficiency, and silicone are the factors that affect this disease.
Is Sjogren's syndrome an autoimmune disease?
Sjogren's syndrome is a long-term autoimmune disease in which the immune system attacks its own body cells and organs. Sjogren's syndrome damages the glands that produce and regulate moisture in our bodies, causing dryness throughout the body, especially the eyes and mouth.
What are the complications of Sjogren's syndrome?
A decrease in saliva and tear output can lead to severe complications, including dental cavities, oral infections, and vision problems. A reduction in saliva also interferes with swallowing and speech problems. Several neurological problems, such as numbness and tingling, can be observed. People with haematological problems, like those with Sjogren's syndrome, have a lifetime risk of developing non-Hodgkin B-cell lymphoma (Blood cancer).
When to consult a doctor for Sjögren syndrome?
Consult a doctor for Sjögren syndrome if dryness of the eyes or mouth continues for several weeks, worsens, or begins to affect everyday activities. Signs that need attention include:
- Persistent dry eyes with burning, redness, or foreign body sensation
- Chronic dry mouth causing difficulty in chewing, swallowing, or speaking
- Frequent dental caries, oral ulcers, or gum infections
- Unexplained fatigue, joint pain, or muscle stiffness
- Swelling of salivary glands near the jaw or ears
If these symptoms continue, it is important to consult a Sjogren syndrome specialist who can evaluate the cause and confirm Sjögren syndrome. Seek emergency medical attention if you experience sudden vision loss, severe eye pain, shortness of breath, or neurological symptoms. A rheumatologist, ophthalmologist, dentist, or general physician can provide the best Sjogren syndrome treatment to control the disease and prevent complications.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868