Aortic Aneurysms: Symptoms, Causes & Treatment
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. Seshi Vardhan Janjirala - Consultant Interventional Cardiologist
Overview | Statistics | Types | Symptoms | Causes | Risk Factors | Complications | Diagnosis | Treatment | Prevention | Aortic dissection vs Aneurysm | FAQs | When to consult a Doctor
Aortic aneurysm definition
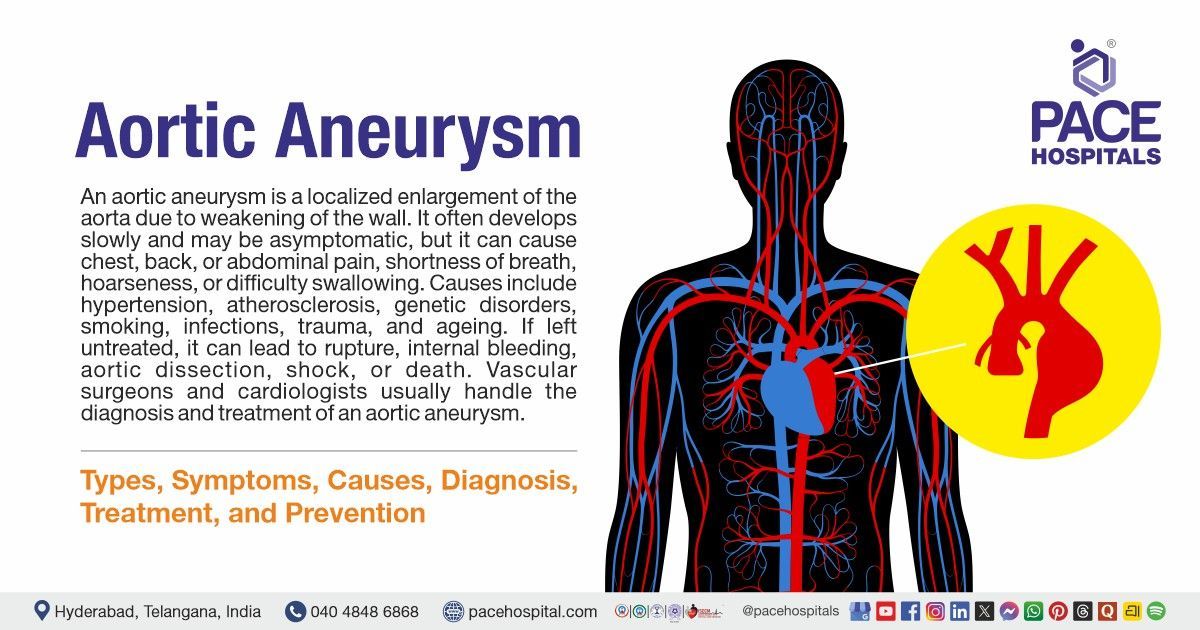
An aortic aneurysm is defined as a medical condition in which there is an abnormal, localised dilation or ballooning of the aorta (the largest artery in the body) due to weakening of the arterial wall. This enlargement may develop slowly and mostly without symptoms, but it can become dangerous if the aneurysm grows large or ruptures. This condition is accompanied by symptoms like deep, persistent chest, back, or abdominal pain, hoarseness, shortness of breath, or difficulty swallowing. In many cases, however, individuals remain asymptomatic until complications occur.
The main causes of aortic aneurysms include long-standing hypertension, atherosclerosis, connective tissue disorders, genetic factors, smoking, infections, trauma, and age-related degeneration of the arterial wall. If left untreated, an aortic aneurysm can lead to serious complications such as rupture, internal bleeding, aortic dissection, shock, and death.
A vascular surgeon and cardiologist can successfully diagnose, treat, and manage the condition.
Aortic aneurysm meaning
The term aortic aneurysm originates from Greek words:
- “Aorta” meaning “great artery”, referring to the main artery that carries blood away from the heart.
- “Aneurysm” meaning “a widening” or “dilation.”
Thus, aortic aneurysm literally means “a dilation or widening of the aorta,” reflecting the condition’s hallmark feature: an abnormal balloon-like enlargement of the aortic wall caused by weakening of the artery, which increases the risk of rupture or other life-threatening complications.
Aortic Aneurysm Statistics
Aortic aneurysm statistics Worldwide
Recent Global Burden of Disease (GBD) analyses report that annual deaths from aortic aneurysms increased from about 88,353 in 1990 to over 153,927 in recent years, mainly due to population ageing, despite a decline in age-standardised death rates.
Most deaths (around 75–80%) occur in individuals aged ≥65 years, and mortality is consistently 2–4 times higher in men than women. Abdominal aortic aneurysm (AAA) is the most common type (~90% of cases), with a prevalence of approximately 2–8% in men over 65 years, and about 4–5 times lower in women. Ruptured aortic aneurysms remain highly lethal, with overall mortality rates of 80–90%.
Aortic Aneurysm Statistics in India
The prevalence of abdominal aortic aneurysm is relatively low, at around 0.3–0.5% in the general population, which is lower than in Western countries. This is due to limited screening and late clinical presentation, rather than a true absence of disease. Most Indian patients with aortic aneurysms are older adults (≥60–65 years), with male predominance.
Thoracic and abdominal aneurysms are frequently asymptomatic until rupture, and Indian hospital data indicate that a large proportion of cases present as emergencies, with ruptured aneurysms carrying a very high mortality rate exceeding 80%.
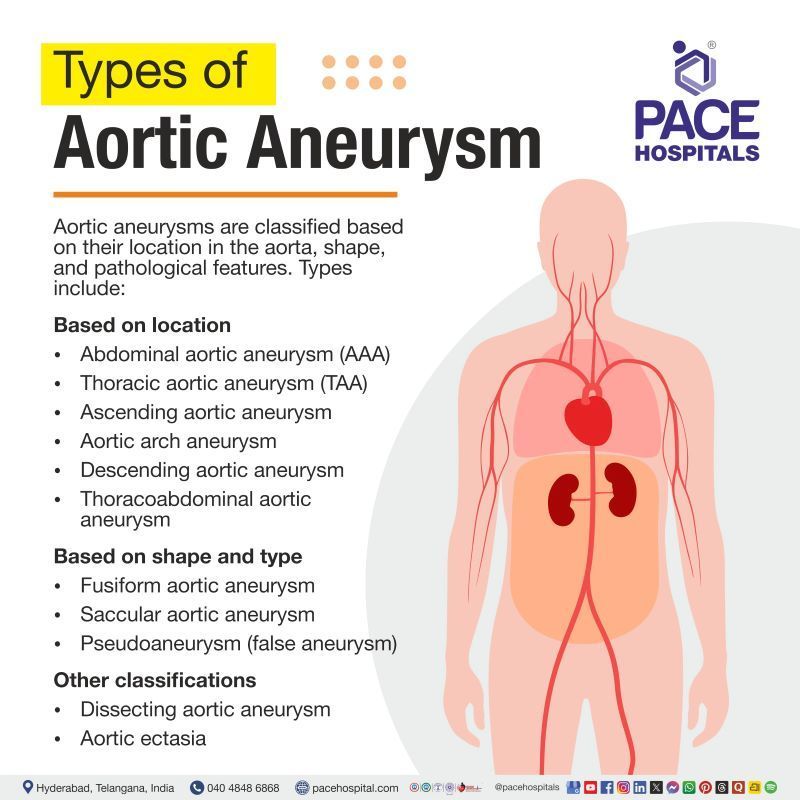
Types of Aortic Aneurysm
The classification is mainly based on the anatomical location of the aneurysm within the aorta, as well as its morphological appearance and pathological characteristics.
Below are the aortic aneurysm classifications:
Based on location
- Abdominal aortic aneurysm (AAA)
- Thoracic aortic aneurysm (TAA)
- Ascending aortic aneurysm
- Aortic arch aneurysm
- Descending aortic aneurysm
- Thoracoabdominal aortic aneurysm
Based on shape and type
- Fusiform aortic aneurysm
- Saccular aortic aneurysm
- Pseudoaneurysm (false aneurysm)
Other classifications
- Dissecting aortic aneurysm
- Aortic ectasia
Based on Location
Abdominal aortic aneurysm (AAA): Abdominal aortic aneurysm is the most common type of aortic aneurysm that occurs in the abdominal portion of the aorta, below the level of the renal arteries. It remains asymptomatic in the early stages, and as the aneurysm enlarges, it may cause abdominal or back pain and a pulsatile abdominal mass. Rupture of an AAA is a medical emergency associated with high mortality.
Thoracic aortic aneurysm (TAA): A thoracic aortic aneurysm develops in the section of the aorta located within the chest. TAAs are less common than AAAs and may be associated with genetic connective tissue disorders, hypertension, or degenerative changes. There are different thoracic aortic aneurysm classifications:
- Ascending aortic aneurysm: This involves the portion of the aorta extending upward from the heart. It is the most common subtype of thoracic aortic aneurysm and is frequently linked to conditions such as hypertension, bicuspid aortic valve, and connective tissue disorders. Enlargement in this region increases the risk of aortic dissection, aortic valve dysfunction, and rupture.
- Aortic arch aneurysm: This occurs in the curved segment of the aorta that gives rise to major arteries supplying the head and upper limbs. Because of its location, it may cause symptoms related to compression of surrounding structures.
- Descending aortic aneurysm: This affects the portion of the thoracic aorta that runs downward through the chest. It is commonly associated with atherosclerosis and long-standing hypertension. Patients may experience back pain or chest discomfort, and large aneurysms carry a significant risk of rupture.
Thoracoabdominal aortic aneurysm: A thoracoabdominal aortic aneurysm extends from the thoracic aorta into the abdominal aorta. This type involves multiple segments of the aorta and may affect branches supplying vital organs.
Based on shape and type
Fusiform aortic aneurysm: This is characterised by a uniform, symmetrical dilation involving the full circumference of a segment of the aorta. Fusiform aneurysms usually develop due to chronic conditions such as atherosclerosis, hypertension, and age-related degeneration of the aortic wall.
Saccular aortic aneurysm: This appears as a localised, pouch-like outgrowth on one side of the aortic wall and does not involve the full circumference of the vessel. Saccular aneurysms are often associated with trauma, infection, or penetrating atherosclerotic ulcers.
Pseudoaneurysm (false aneurysm): This type occurs when there is a breach in the aortic wall, and blood leaks out but is contained by surrounding tissues rather than by all layers of the vessel wall. It commonly results from trauma, surgical procedures, and catheter-related injury.
Other classifications
Dissecting aortic aneurysm: This refers to a condition in which a tear develops in the inner layer of the aortic wall, allowing blood to enter and split the layers of the aorta, creating a false lumen. This process weakens the vessel wall and may lead to aneurysmal dilation, rupture, or compromised blood flow to vital organs.
Aortic ectasia: This is characterised by a mild, diffuse enlargement of the aorta that does not meet the size criteria for an aneurysm. It is usually an age-related change and may be associated with hypertension or early atherosclerotic disease.
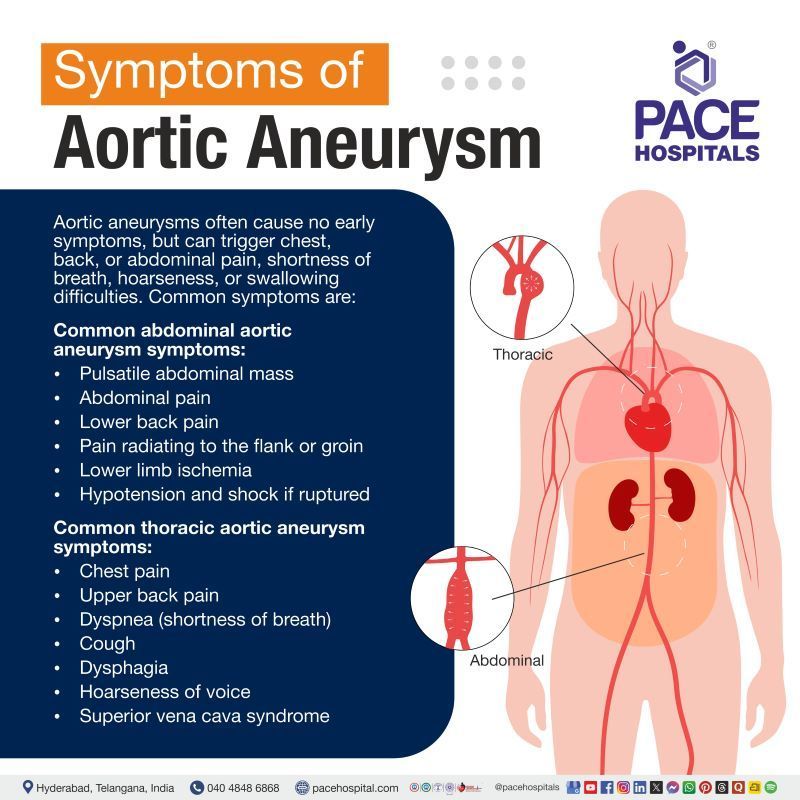
Aortic Aneurysm Symptoms
Aortic aneurysm symptoms arise due to progressive weakening and dilation of the aortic wall, which leads to stretching of pain-sensitive structures, compression of adjacent organs, and altered blood flow. As the aneurysm gets larger, it may press on nearby nerves, airways, esophagus, or veins. The clinical manifestations vary according to the location of the aneurysm, particularly between abdominal and thoracic aortic aneurysms. The signs and symptoms of an aortic aneurysm are:
Common abdominal aortic aneurysm symptoms
- Pulsatile abdominal mass
- Abdominal pain
- Lower back pain
- Pain radiating to the flank or groin
- Lower limb ischemia
- Hypotension and shock if ruptured
Common thoracic aortic aneurysm symptoms
- Chest pain
- Upper back pain
- Dyspnea (shortness of breath)
- Cough
- Dysphagia
- Hoarseness of voice
- Superior vena cava syndrome
Pulsatile abdominal mass: In an aortic aneurysm, the abdominal aorta becomes abnormally dilated and weakened. Because the aorta is a high-pressure artery, this dilated segment expands with each heartbeat. As a result, the transmitted arterial pulsations become exaggerated and can be felt on abdominal palpation as a clearly pulsatile mass, especially in thin individuals.
Abdominal pain: As the swollen part of the aorta slowly gets bigger, it stretches the blood vessel and nearby tissues. This stretching can cause a deep, aching pain in the abdomen. The pain may be mild at first, but it can become more noticeable as the swelling increases.
Lower back pain: The aorta runs close to the spine in the lower back. When it becomes enlarged, it can press on the bones, muscles, and nerves in that area. This leads to lower back pain, which is a classic symptom and may be constant due to ongoing mechanical pressure.
Pain radiating to the flank or groin: Irritation or compression of nearby nerves by the expanding aneurysm can cause referred pain. These nerves supply the flank and groin, causing pain that radiates to these areas. Such radiation often suggests rapid expansion, or which may rupture.
Lower limb ischemia: Blood flow inside the swollen aneurysm can become uneven, allowing blood clots to form. Small pieces of these clots can travel down to the blood vessels of the legs and block them. This may cause leg pain, coldness, numbness, or difficulty in walking due to reduced blood supply.
Hypotension and shock if ruptured: If the aneurysm ruptures, there is sudden and massive internal bleeding, usually into the retroperitoneal space or peritoneal cavity. This rapid loss of blood volume leads to decreased venous return and cardiac output, resulting in severe hypotension and hypovolemic shock, a life-threatening emergency.
Chest pain: Chest pain is common in thoracic aortic aneurysms, which is caused by stretching of the aortic wall or irritation of surrounding tissues as the aneurysm enlarges. This causes pain that is usually deep, dull, or aching and may worsen with expansion, dissection, or impending rupture.
Upper back pain: The thoracic aorta lies close to the spine in the upper back. As the aneurysm enlarges, it can press on the vertebrae and nearby nerves, leading to persistent upper back pain, often felt between the shoulder blades.
Dyspnea (shortness of breath): Dyspnea occurs when a growing aneurysm compresses surrounding respiratory structures, such as the trachea or lungs. Reduced airway space or reduced lung expansion can make breathing difficult, especially during physical activity.
Cough: A chronic cough may develop due to irritation or compression of the trachea or bronchi by the aneurysm. This symptom is often non-productive and persistent and may worsen as the aneurysm increases in size.
Dysphagia: Dysphagia occurs when the aneurysm presses on the esophagus, which lies close to the thoracic aorta. This compression can interfere with the normal passage of food, leading to difficulty or discomfort during swallowing, especially with solid foods.
Hoarseness of voice: A nerve called the recurrent laryngeal nerve controls the vocal cords and runs near the aorta. Pressure from an enlarged aneurysm can damage or irritate this nerve, leading to hoarseness or a weak voice that may develop gradually.
Superior vena cava (SVC) syndrome: Superior vena cava syndrome develops when a large thoracic aortic aneurysm compresses the superior vena cava, which can impair venous return from the head, neck, and upper limbs. This leads to facial swelling, neck vein distension, upper limb edema, and sometimes headache or dizziness.
Aortic Aneurysm Causes
Aortic aneurysms develop as a result of progressive weakening and degeneration of the aortic wall, which reduces its ability to withstand normal arterial pressure. This weakening may occur due to a variety of pathological, genetic, mechanical, and inflammatory factors. Understanding the underlying causes is essential, as they influence the location, rate of progression, risk of rupture, and management strategy of the aneurysm. The most common causes of aortic aneurysms are:
- Atherosclerosis
- Chronic hypertension
- Degenerative changes
- Genetic syndromes
- Vascular inflammation
- Traumatic injury
- Infections
Atherosclerosis: Atherosclerosis is the most common cause of aortic aneurysms. Lipid and fibrous plaque buildup in the aortic wall reduces blood supply and triggers chronic inflammation, leading to degeneration of elastic fibres and smooth muscle cells. This weakens the vessel wall, causing progressive dilation and aneurysm formation.
Chronic hypertension: This exposes the aortic wall to persistently elevated pressure and mechanical stress. Over time, this increased stress accelerates wear and tear on the elastic components of the aortic wall, causing medial degeneration and weakening. The constant force of high blood pressure promotes the gradual expansion of the weakened segment of the aorta.
Degenerative changes: Degenerative changes are related to ageing, involve the gradual breakdown of collagen and elastin within the aortic wall. This process then leads to thinning and loss of structural integrity of the media. As the supportive framework of the aorta deteriorates, the vessel becomes less resistant to intraluminal pressure, predisposing it to aneurysmal dilation.
Genetic syndromes: Certain genetic anomalies, including Marfan syndrome, Loeys-Dietz syndrome (LDS), and Ehlers-Danlos syndrome, cause hereditary deficiencies in connective tissue proteins such as collagen and elastin, which are required for aorta wall strength. In such cases, the aorta is structurally weak from birth and more prone to dilatation, even under normal blood pressure. As a result, aneurysms tend to form at a younger age and might progress quickly.
Vascular inflammation: Inflammatory diseases can cause long-lasting irritation in blood vessels, including the aorta, which is the main blood vessel of the body. Over time, this inflammation allows immune cells to enter the vessel wall and release harmful substances that slowly damage it.
Traumatic injury: Traumatic injury to the aorta, such as from high-speed motor vehicle accidents or severe blunt chest trauma, can directly damage the aortic wall. These partial tears or weakening of the vessel layers may not cause immediate rupture but can later evolve into aneurysms.
Infections: Microorganisms can directly invade the aorta wall, causing mycotic aortic aneurysms. Infectious agents, such as bacteria or fungi, cause severe inflammation, tissue necrosis, and structural layer damage. The aorta wall is vulnerable to dilatation and rupture due to its rapid deterioration.
Aortic Aneurysm Risk Factors
The development of an aortic aneurysm is strongly influenced by the presence of certain risk factors that predispose the aortic wall to weakening and degeneration. These risk factors may be non-modifiable or modifiable. Below are the risk factors of an aortic aneurysm:
- Older age
- Gender
- Smoking
- Family history
- Sedentary lifestyle
- Poorly controlled diabetes
- Hypertension
- Atherosclerosis / coronary artery disease / peripheral artery disease
Older age: Older age increases aortic aneurysm risk as cumulative degenerative changes, such as elastin fragmentation and collagen cross-linking loss in the aortic media, progressively weaken vessel wall integrity, particularly after age 65 for abdominal aneurysms and 70 for thoracic ones.
Gender: Men are more likely than women to develop an aortic aneurysm. This is partly because differences in vascular biology and risk factor exposure can make the aortic wall in men more prone to weakening over time, increasing the risk of an aneurysm.
Smoking: Tobacco smoke causes chronic inflammation, oxidative stress, and direct damage to the endothelial lining of blood vessels. It also speeds up atherosclerosis and promotes the breakdown of elastin and collagen in the aorta wall. These effects dramatically damage the vascular structure, promoting the formation and fast extension of aneurysms.
Family history: A positive family history increases the risk of developing an aortic aneurysm due to genetic predisposition. Close relatives (such as parents and siblings) of affected people are at a higher risk due to hereditary connective tissue deficiencies or genetic disorders. These diseases weakened the aorta wall, making it more susceptible to dilatation and aneurysm formation.
Sedentary lifestyle: A sedentary lifestyle promotes conditions like obesity, hypertension, and dyslipidemia. Lack of regular physical activity can impair heart health and accelerate vascular ageing. These factors increase mechanical stress on the aortic wall and speed up degenerative changes.
Poorly Controlled Diabetes: Chronic high blood sugar damages blood vessels, causing inflammation and stiffening of the aortic wall, which increases vulnerability to aneurysms.
Hypertension: Persistently high blood pressure puts extra mechanical stress on the aortic wall, stretching and weakening it, making aneurysm formation more likely.
Atherosclerosis / coronary artery disease / peripheral artery disease: Plaque buildup in arteries weakens the structural integrity of the aortic wall, and systemic atherosclerosis, as seen in CAD or PAD, further raises the risk of aneurysm.
Aortic Aneurysm Complications
Aortic aneurysms may remain asymptomatic for long periods; however, as they enlarge, the risk of serious and potentially life-threatening complications increases. These complications arise from progressive weakening of the aortic wall and the aneurysm’s effect on surrounding structures, making early detection and careful management critical. The following are the complications of an aortic aneurysm:
- Aortic rupture
- Aortic dissection
- Thrombus formation and embolization
- Compression of adjacent structures
- Distal ischemia
- Infection of the aneurysm
- Heart failure (in thoracic aneurysms)
Aortic rupture: Rupture is the most serious and life-threatening complication of an aortic aneurysm. As the aneurysm enlarges, the aortic wall becomes progressively thinner and weaker, eventually tearing open. This leads to massive internal bleeding, a rapid drop in blood pressure, shock, and often sudden death if immediate medical intervention is not provided.
Aortic dissection: An aortic aneurysm can predispose the aorta to dissection, where a tear develops in the inner layer of the vessel wall. Blood then flows between the layers of the aorta, separating them and further weakening the vessel. This can compromise blood flow to vital organs and may progress to rupture.
Thrombus formation and embolization: Blood flow within an aneurysm is often turbulent, promoting the formation of blood clots along the aneurysm wall. These thrombi can break off and travel as emboli to distant arteries, causing ischemia or infarction in organs such as the brain, kidneys, or limbs.
Compression of adjacent structures: Large aortic aneurysms may compress nearby organs and structures. This can lead to symptoms like chest or back pain, difficulty breathing, hoarseness due to pressure on the recurrent laryngeal nerve, or difficulty swallowing from esophageal compression.
Distal ischemia: An aneurysm can reduce effective blood flow beyond the affected segment of the aorta. This decreased perfusion may result in ischemia of tissues and organs supplied by branches of the aorta, leading to complications such as renal failure, bowel ischemia, or limb ischemia.
Infection of the aneurysm: An existing aneurysm may become infected, resulting in an infected (mycotic) aneurysm. Infection causes rapid weakening of the aortic wall, increases the risk of rupture, and is associated with high morbidity and mortality.
Heart failure (in thoracic aneurysms): Thoracic aortic aneurysms can affect the aortic valve, leading to aortic regurgitation. This places extra volume load on the left ventricle, which, over time, may result in left-sided heart failure.
Aortic Aneurysm Diagnosis
Aortic aneurysms are often clinically silent and discovered incidentally during imaging performed for other conditions. Timely diagnosis is crucial to evaluate the extent of aortic dilation and to determine the risk of progression or rupture.
The following are the steps commonly included in the aortic aneurysm diagnosis criteria:
- Medical history
- Physical examination
- Laboratory tests (not routine for diagnosis of aortic aneurysm)
- Complete blood count (CBC)
- Inflammatory markers [C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR)]
- Renal function tests
- Coagulation profile
- Imaging studies
- Ultrasound
- Computed tomography (CT) scan / CT angiography
- Magnetic resonance imaging (MRI) / MR angiography
- Chest or abdominal X-ray
- Echocardiography
Aortic Aneurysm Treatment
The aortic aneurysm management aims to prevent expansion and rupture while minimising treatment-related risks. Treatment strategies are based on the aneurysm's size, location, growth rate, and the patient's overall health. Options range from conservative medical management and regular surveillance to surgical or endovascular intervention for high-risk aneurysms. Treatment of aortic aneurysm includes:
Non-pharmacological management
- Regular imaging surveillance
- Controlling blood pressure
- Lifestyle modification
- Smoking cessation
Pharmacological management
- Blood pressure–lowering medications
- Beta-blockers
- ACE inhibitors/angiotensin receptor blockers
- Cholesterol-lowering therapy (statins)
- Antiplatelet agents (if indicated)
Surgical interventions
- Open aortic aneurysm repair
- Endovascular aortic aneurysm repair
- Thoracic endovascular aortic repair (TEVAR)
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support
Aortic Aneurysm Prevention
Prevention of aortic aneurysm focuses on reducing factors that weaken the aortic wall and increase stress on it over time. Since many aneurysms develop silently and progress gradually, adopting healthy lifestyle practices and controlling underlying medical conditions can significantly lower the risk of aneurysm formation, slow its growth, and prevent life-threatening complications such as rupture. Below are the preventive steps to reduce the risk of aortic aneurysm:
- Stopping smoking
- Managing high blood pressure and cholesterol
- Ensuring a healthy diet
- Regular exercise
- Controlling stress
- Regular check-ups and screenings
Stopping smoking: Quitting smoking is one of the best ways to protect the aorta. When a person stops smoking, inflammation decreases, and the aortic wall can better maintain its strength, slowing or preventing aneurysm growth.
Managing high blood pressure and cholesterol: Effective control of high blood pressure reduces the continuous mechanical stress exerted on the aortic wall, thereby preventing weakening and dilation. Also, managing high cholesterol levels slows the progression of atherosclerosis, which otherwise contributes to inflammation and degeneration of the aortic wall.
Ensuring a healthy diet: A healthy diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats supports overall cardiovascular health. This type of diet helps to control body mass index (BMI), blood pressure, cholesterol, and blood sugar levels. Reducing vascular inflammation and atherosclerotic plaque through nutrition lowers the risk of aortic wall degeneration and aneurysm formation.
Regular exercise: Regular moderate physical activity improves cardiovascular function, helps maintain healthy blood pressure, and enhances circulation. Exercise also aids in weight control and reduces inflammation, which decreases stress on the aortic wall and slows degenerative changes.
Controlling stress: Chronic stress causes chronic elevations in blood pressure and increased release of stress hormones, which can damage blood vessels over time. Relaxation techniques help to normalise blood pressure and reduce vascular strain.
Regular check-ups and screenings: Regular medical check-ups allow early detection and management of risk factors. Screening, especially in high-risk individuals such as older adults and smokers, enables early identification of aortic aneurysms before complications arise.
Difference between Aortic Dissection and Aortic Aneurysm
Aortic dissection vs aneurysm
Aortic aneurysm and aortic dissection are two serious but distinct disorders of the aorta. Although both involve weakening of the aortic wall and can be life-threatening, they differ in their underlying pathology, mode of development, clinical presentation, and complications. Below are some of the parameters that help in differentiating aortic dissection and aneurysm:
| Parameters | Aortic dissection | Aortic aneurysm |
|---|---|---|
| Definition | A tear in the inner layer of the aorta allows blood to pass between the layers of the wall | A localised, permanent dilatation of the aorta due to weakening of the vessel wall |
| Pathology | Sudden separation of the aortic wall layers creates a false lumen | Gradual thinning and degeneration of the aortic wall |
| Onset | Sudden and acute | Usually slow and progressive |
| Main cause | Hypertension, connective tissue disorders, trauma | Atherosclerosis, ageing, hypertension, and genetic disorders |
| Pain | Severe, sudden, tearing or ripping chest/back pain | Often asymptomatic; may cause dull chest, back, or abdominal pain |
Frequently Asked Questions (FAQs) on Aortic Aneurysm
What is an aortic aneurysm?
An aortic aneurysm is a localised widening of the aorta, the main blood vessel carrying blood from the heart to the body. It happens when the vessel wall becomes weak and stretches over time. Aneurysms often grow slowly and may not cause symptoms. The main concern is rupture, which can be life-threatening.
How dangerous is a 4 cm aortic aneurysm?
A 4 cm aortic aneurysm is generally considered small to moderate in size. The risk of rupture at this size is low, usually less than 1% per year. Most people do not have symptoms. Doctors usually recommend regular monitoring with imaging rather than surgery.
What causes abdominal aortic aneurysm?
Long-term damage to the artery wall is the main cause of abdominal aortic aneurysm. The risk factors are smoking, ageing, high blood pressure, and hardening of the arteries. Genetics can increase risk, especially in close relatives. Most abdominal aortic aneurysms develop slowly over many years without early warning signs.
Is an aortic aneurysm hereditary?
Aortic aneurysms can be partially inherited. People with a close family member affected are at a higher risk than the overall population. Certain hereditary connective tissue disorders raise risk by weakening arterial walls. However, the majority of aneurysms are caused by a mix of genetics and lifestyle factors, such as smoking and high blood pressure.
What foods should be avoided in individuals with an aortic aneurysm?
Patients need to avoid foods that cause high blood pressure or aggravate arterial damage. Foods needed to be avoided may include salty foods, processed meats, fried foods, and saturated fat-rich foods. Excess sugar may also cause inflammation. Alcohol should be limited. A diet rich in fruits, vegetables, whole grains, and lean meats promotes blood vessel health.
What is a dissecting aortic aneurysm?
A dissecting aortic aneurysm, more commonly called aortic dissection, occurs when a tear forms in the inner layer of the aorta. Blood then flows between the layers of the vessel wall, forcing them apart. This is a medical emergency and can block blood flow to vital organs or cause rupture.
How to prevent an aortic aneurysm?
Avoiding smoking is the most important step. Keeping blood pressure and cholesterol under control lowers stress on the aorta. Regular physical activity and maintaining a healthy weight are helpful. Conditions such as diabetes should be well-managed. In people with a family history, screening tests can detect early changes and allow monitoring before serious problems develop.
Can a car accident cause an aortic aneurysm?
Car accidents rarely cause an aortic aneurysm, but can trigger tears or bursts in those with existing weak spots from age or smoking. High-impact crashes may damage the aorta directly through blunt force. Healthy aortas seldom develop aneurysms from trauma alone.
Can pregnancy cause an abdominal aortic aneurysm?
No, pregnancy rarely causes an abdominal aortic aneurysm. Hormonal changes and increased blood volume may place extra stress on blood vessels, especially in women with inherited vessel weakness.
How serious is an ascending aortic aneurysm?
An ascending aortic aneurysm is considered serious because it affects the part of the aorta closest to the heart. It has a higher risk of rupture or dissection compared with aneurysms in other areas.
What are the early warning signs of an aneurysm?
Early warning signs of an aortic aneurysm often go unnoticed as it grows silently, but some people experience the following:
- Deep, constant pain in the abdomen, chest, or back
- Pulsating feeling near the belly button (abdominal aneurysm)
- Shortness of breath due to pressure on airways
- Persistent back or side pain lasting several hours
- Sudden severe pain suggests rupture and is a medical emergency
What are the signs of a dissecting aortic aneurysm?
A dissecting aortic aneurysm, also called aortic dissection, usually causes sudden and severe symptoms. Signs are:
- Sudden, intense chest or upper back pain, often tearing or sharp
- Pain may spread to the neck, jaw, or abdomen
- Shortness of breath
- Fainting or loss of consciousness
- Weakness or confusion
- Sudden drop in blood pressure
What is a syphilitic aortic aneurysm?
A syphilitic aortic aneurysm is a complication of untreated syphilis infection, where bacteria weaken the aorta's middle layer over the years. It mainly affects the ascending aorta near the heart, causing slow bulging and valve issues.
When to consult a doctor for an aortic aneurysm?
Consult a doctor if you have risk factors for an aortic aneurysm or experience symptoms that persist or worsen over time. Early evaluation is important to prevent serious complications. Signs that need medical attention include:
- Deep, persistent pain in the chest, back, or abdomen
- A pulsating sensation near the belly button
- Shortness of breath or difficulty swallowing
- Hoarseness or chronic cough
- Back or side pain lasting several hours or days
If these symptoms persist, it is important to consult an aortic aneurysm specialist who can evaluate the cause and recommend the proper treatment plan. Seek immediate medical attention if you experience sudden, severe chest, back, or abdominal pain, fainting, sudden weakness, or a rapid drop in blood pressure, as these may indicate aneurysm rupture or dissection, which are life-threatening emergencies. A cardiologist, or vascular specialist, can provide the best aortic aneurysm treatment and prevent complications.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868