Atherosclerosis: Symptoms, Causes & Treatment
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. Seshi Vardhan Janjirala - Consultant Interventional Cardiologist
Overview | Epidemiology | Types | Symptoms | Causes | Risk Factors | Complications | Diagnosis | Treatment | Prevention | Atherosclerosis vs Arteriosclerosis | FAQs | When to consult a Doctor
Atherosclerosis definition
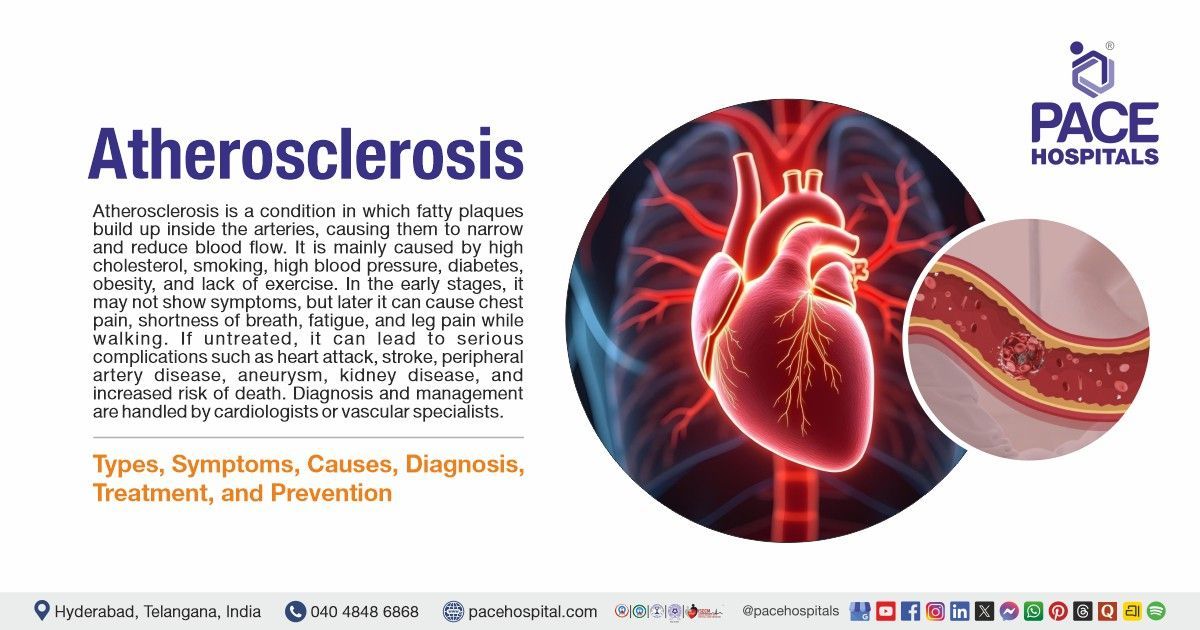
Atherosclerosis is a chronic disease of the arteries in which fatty deposits (plaques) made of cholesterol, calcium, and inflammatory cells gradually build up on the inner walls of blood vessels. This fat buildup causes the arteries to become narrow and harden, hence reducing blood flow to vital organs and tissues. Symptoms depend on the arteries affected. Insufficient blood flow to the heart causes chest pain or shortness of breath; if brain arteries are involved, it may lead to transient ischemic attacks (TIA) or stroke symptoms; and reduced blood flow to the limbs can cause claudication (leg pain during walking).
The causes and risk factors are high cholesterol levels, high blood pressure, diabetes, obesity, smoking, physical inactivity, an unhealthy diet, and a family history of cardiovascular disease. Complications can include acute coronary syndromes, peripheral artery disease, ischemic stroke, aortic aneurysm, chronic kidney disease, and increased cardiovascular mortality.
A
cardiologist or
vascular specialist, a doctor specialised in heart and blood vessel diseases, can accurately diagnose atherosclerosis and guide appropriate treatment and preventive strategies.
Atherosclerosis meaning
The word atherosclerosis comes from Greek words:
- “Athero” means fatty or paste-like material
- “Sclerosis” means hardening
The term describes a condition where fatty deposits build up inside the arteries and make them hard and narrow, which reduces blood flow and can lead to heart disease or stroke.
Atherosclerosis Epidemiology
Atherosclerosis epidemiology worldwide
Atherosclerosis is a major global health problem and the leading underlying cause of cardiovascular diseases such as heart attack and stroke. According to the World Health Organisation (WHO), cardiovascular diseases account for nearly 32% of all deaths globally, with atherosclerosis responsible for most of these cases. The highest burden of atherosclerosis-related deaths occurs in low- and middle-income countries, that accounts around 75% of global cardiovascular mortality. Although high-income countries have achieved declining death rates through prevention and advanced care, the prevalence continues to rise worldwide due to population ageing and lifestyle changes.
Atherosclerosis epidemiology in India
Atherosclerosis is the leading cause of death in India, currently accounting for nearly 30–35% of all fatalities. It is uniquely characterised by a premature onset, with heart attacks occurring 5–10 years earlier than in Western populations; notably, 25% of cases strike individuals under the age of 40. The epidemic is driven by a high prevalence of diabetes, hypertension (affecting 1 in 4 adults), and a distinct lipid profile of high triglycerides and low HDL. Prevalence is significantly higher in urban areas (~10–12%) compared to rural regions (~4–6%).

Types of Atherosclerosis
Atherosclerosis is a systemic, progressive disease, but it is described as different types based on the arterial location involved, because involvement of different arteries produces distinct clinical features, complications, and syndromes. This location-based classification helps in understanding disease presentation, diagnosis, and management. The different types of atherosclerosis are discussed below:
- Coronary atherosclerosis
- Carotid artery atherosclerosis
- Atherosclerosis peripheral arterial disease (PAD)
- Atherosclerosis of the renal artery
- Aortic atherosclerosis
- Vertebral artery atherosclerosis
- Intracranial atherosclerosis
Coronary atherosclerosis: The buildup of atherosclerotic plaques in the coronary arteries that supply blood to the heart muscle. As plaques narrow the arterial lumen, due to this oxygen delivery to the myocardium decreases, especially during increased demand such as exercise or stress. Because the heart is highly sensitive to reduced blood flow, coronary involvement is one of the most common site of atherosclerosis.
Carotid artery atherosclerosis: Carotid atherosclerosis involves plaque formation in the carotid arteries, which supply blood to the brain. Progressive narrowing can reduce cerebral perfusion, while unstable plaques may rupture and release emboli that travel to cerebral vessels. This type commonly presents with transient ischemic attacks or ischemic stroke.
Atherosclerosis peripheral arterial disease (PAD): This affects the arteries supplying the lower limbs, and less commonly the upper limbs. This reduces blood flow to skeletal muscles leads to ischemic pain during activity, known as intermittent claudication. In advanced disease, blood flow may be insufficient even at rest, resulting in non-healing ulcers, tissue necrosis, or gangrene.
Atherosclerosis of the renal artery: Renal atherosclerosis occurs when plaques narrow one or both renal arteries, which reduces blood flow to the kidneys. The kidneys release hormones, leading to secondary hypertension that is often resistant to treatment. Chronic reduction in renal perfusion may also cause progressive renal ischemia and loss of kidney function.
Aortic atherosclerosis: Aortic atherosclerosis occurs when fatty deposits build up in the aorta. This buildup happens most often in the lower (abdominal) part of the aorta. At first, it may not cause any symptoms. However, over time, the plaques can weaken the wall of the blood vessel, increase the risk of a bulge or widen, called an aneurysm.
Vertebral artery atherosclerosis: This occurs when fatty buildup develops in the vertebral arteries, which carry blood to the back part of the brain. This area controls important functions such as balance, coordination, and vision. When these arteries get narrowed, less blood reaches the brain, which can cause symptoms like dizziness, spinning sensations, blurred or double vision, trouble with balance or walking, and even fainting.
Intracranial atherosclerosis: Intracranial atherosclerosis refers to the development of atherosclerotic plaques in the arteries located within the cranial cavity and vertebral arteries. Plaque formation in these vessels leads to progressive narrowing of the arterial lumen, reducing blood flow to brain tissue. Clinically, it is a major cause of ischemic stroke and transient ischemic attacks.

Atherosclerosis Symptoms
Atherosclerosis often develops slowly and may cause no symptoms initially. Symptoms usually appear when the arteries become severely narrowed or completely blocked. The signs and symptoms of atherosclerosis depend on which arteries are affected:
Atherosclerosis cardiovascular disease symptoms are:
- Chest pain or pressure (Angina)
- Shortness of breath
- Fatigue
- Heart attack (Myocardial infarction)
Atherosclerosis brain symptoms (carotid arteries) are:
- Sudden weakness or numbness
- Trouble speaking or understanding speech
- Dizziness or sudden vision problems
- Stroke or mini-stroke (TIA)
Atherosclerosis symptoms in the legs
- Claudication (pain or cramping in legs)
- Coldness or numbness in legs
- Slow-healing wounds on feet or toes
Atherosclerosis – Kidney Arteries
- High blood pressure
- Reduced kidney function
Atherosclerosis cardiovascular disease symptoms are:
- Chest pain or pressure (angina): Atherosclerosis narrows the coronary arteries, reducing blood flow to the heart muscle. During exertion or stress, the oxygen supply becomes insufficient, leading to myocardial ischemia and the characteristic pressure-like chest pain called angina.
- Shortness of breath (SOB): This happens because decreased coronary blood flow decreases myocardial contractility, which reduces the heart's capacity to pump effectively. As cardiac output decreases, blood backs up into the pulmonary circulation, causing pulmonary congestion and dyspnea (sensation of breathlessness).
- Fatigue: This is a result of decreased cardiac output caused by chronic myocardial ischemia. When the heart cannot pump sufficient oxygenated blood to meet the body’s metabolic needs, skeletal muscles and other tissues receive less oxygen, leading to early fatigue and reduced exercise tolerance.
- Heart attack (Myocardial infarction): When an atherosclerotic plaque ruptures, a blood clot forms and abruptly blocks a coronary artery. This sudden loss of blood supply causes myocardial infarction, commonly known as a heart attack.
Atherosclerosis brain symptoms (carotid arteries) are:
- Sudden weakness or numbness: Atherosclerotic narrowing or plaque rupture in cerebral or carotid arteries reduces blood flow to specific areas of the brain that control motor and sensory functions. Ischemia of these regions results in sudden weakness or numbness on the opposite side of the body.
- Trouble speaking or understanding speech: When atherosclerosis compromises blood flow to language centres of the brain, such as Broca’s or Wernicke’s areas, speech production or comprehension becomes impaired, leading to difficulty understanding words.
- Dizziness or sudden vision problems: Reduced blood flow to areas that are responsible for balance, coordination, or vision causes dizziness, loss of balance, blurred vision, or sudden visual field defects.
- Stroke or mini-stroke (TIA): Severe or prolonged interruption of cerebral blood flow can result in an ischemic stroke with permanent neurological damage.
Atherosclerosis symptoms in the legs
- Claudication (pain or cramping in the legs): Narrowing of leg arteries can limit blood flow to muscles during walking or exercise. The resulting muscle ischemia causes pain or cramping, which improves with rest.
- Coldness or numbness in the legs: Reduced arterial blood supply decreases skin and nerve perfusion, making the affected limb feel cold and numb compared to the normal side.
- Slow-healing wounds on feet or toes: Poor blood flow reduces oxygen and nutrient delivery needed for tissue repair. Since the blood flow is blocked, even minor cuts or ulcers heal slowly and are prone to infection.
Atherosclerosis – Kidney Arteries
- High blood pressure: When the arteries supplying the kidneys become narrowed, less blood reaches the kidneys. In response, the kidneys release hormones that raise blood pressure and cause the body to retain salt and water. This leads to high blood pressure that is difficult to control with medications.
- Reduced kidney function: Chronic reduction in blood flow to the kidneys causes renal ischemia and progressive damage to kidney tissue. This results in decreased glomerular filtration rate and worsening renal function.
Atherosclerosis Causes
Atherosclerosis is a chronic condition in which the arteries gradually become narrowed and hardened due to the buildup of plaques. This can reduce blood flow to vital organs and tissues, potentially leading to serious cardiovascular problems. It is a progressive disease that often develops silently over many years before symptoms appear. The causes of atherosclerosis are:
- Endothelial injury or dysfunction
- Lipid accumulation
- Chronic inflammation
- Smooth muscle cell migration and proliferation
- Plaque calcification
Endothelial injury or dysfunction
Endothelial injury or dysfunction is the main cause of atherosclerosis by damaging the inner lining of the arteries, making it easier for harmful substances to enter. When this lining gets injured, due to factors like high blood pressure, smoking, or diabetes, it loses its protective barrier function and becomes sticky, which attracts immune cells and allows cholesterol to penetrate into the artery wall. Hence, initiating the disease process.
Lipid accumulation
Atherosclerosis is caused by the deposition of lipid, which happens when excess fats, especially LDL or bad cholesterol, get trapped in the damaged artery wall. These lipids oxidise and form fatty streaks, which attract more immune cells that absorb them up, turning into foam cells that enlarge the deposit. Over time, this growing lipid contributes to plaque formation, stiffening and blocking arteries.
Chronic inflammation
Atherosclerosis is caused by chronic inflammation. Foam cells, endothelial cells, and other immune cells release inflammatory mediators such as cytokines and growth factors. These substances attract more inflammatory cells and maintain a continuous inflammatory response, leading to further damage of the arterial wall and progression of the plaque.
Smooth muscle cell migration and proliferation
Inflammatory signals stimulate smooth muscle cells from the arterial media to migrate into the intima. These cells proliferate and produce collagen and extracellular matrix components. This results in the formation of a fibrous cap over the lipid core, contributing to plaque enlargement and narrowing of the arterial lumen.
Plaque calcification
Calcium deposits form within atherosclerotic plaques after prolonged inflammation and plaque maturation. This calcification makes the artery wall harder and less elastic, exacerbating luminal narrowing. This raises the risk of decreased blood flow, plaque rupture, thrombosis, and significant clinical events.
Atherosclerosis Risk Factors
The development of atherosclerosis is not sudden; it progresses gradually as a result of various risk factors that damage the arterial walls, alter lipid metabolism, and promote chronic inflammation. These risk factors can be categorised as non-modifiable and modifiable. Together, they increase the likelihood of plaque formation and the risk of cardiovascular disease. The following are the major risk factors of atherosclerosis:
Atherosclerosis non modifiable risk factors
- Older age
- Gender
- Family history of atherosclerosis or heart disease
- Ethnicity
- Certain medical conditions
Older age: The risk increases with advancing age because arteries gradually lose elasticity and are exposed to the long-term effects of lipid accumulation and inflammation. Over time, this repeated endothelial injury allows plaques to develop and progress, making older individuals more susceptible to arterial narrowing and cardiovascular events.
Gender: Males are generally at a higher risk of developing atherosclerosis at an earlier age compared to females. Female hormones in premenopausal women have a protective effect by improving lipid profiles and maintaining endothelial function. After menopause, this protection declines, and the risk in women increases significantly.
Family history of atherosclerosis or heart disease: A family history indicates a genetic predisposition to conditions such as hyperlipidemia, hypertension, or diabetes. These inherited traits increase the likelihood of endothelial dysfunction and lipid accumulation, raising the risk of early-onset atherosclerosis.
Ethnicity: Certain ethnic groups have a higher prevalence of atherosclerosis due to genetic factors, socioeconomic conditions, and lifestyle patterns. These factors may influence cholesterol levels, blood pressure regulation, and susceptibility to metabolic disorders.
Certain medical conditions: Conditions such as diabetes mellitus, high blood pressure, and genetic lipid disorders accelerate atherosclerosis.
Modifiable risk factors of atherosclerosis
- Physical inactivity
- Unhealthy diet
- Smoking and other tobacco use
- Excessive alcohol consumption
- Excess weight or obesity
Physical inactivity: Lack of regular physical activity causes obesity, insulin resistance, and affects cholesterol levels. It reduces high-density lipoprotein (HDL) cholesterol and increases low-density lipoprotein (LDL) cholesterol, which promotes lipid accumulation and endothelial dysfunction.
Unhealthy diet: Diets that are high in saturated fats, trans fats, salt, and refined sugars raise LDL cholesterol, blood pressure, and inflammation, which accelerate lipid deposition in arteries and promote plaque formation.
Smoking and other tobacco use: Smoking directly damages the endothelium, increases LDL oxidation, and promotes inflammation, which reduces oxygen delivery and increases blood clot formation.
Excessive alcohol consumption: Chronic excessive alcohol intake raises blood pressure, triglyceride levels, and body weight, and these changes contribute to endothelial injury, inflammation, and lipid imbalance.
Excess weight or obesity: Obesity is associated with dyslipidemia, hypertension, and insulin resistance. Excess adipose tissue releases inflammatory mediators that promote chronic inflammation and endothelial dysfunction.

Complications of Atherosclerosis
Atherosclerosis leads to serious complications due to progressive narrowing of arteries, reduced blood flow, and plaque rupture with thrombosis. The major complications of atherosclerotic disease include the following:
Heart-related complications
- Coronary artery disease (CAD)
- Heart failure
- Aortic aneurysm
- Arrhythmia
- Cardiac arrest
- Heart attack (myocardial infarction)
Brain-related complications
- Stroke
- Transient ischemic attack (TIA)
- Vascular dementia
Peripheral vascular complications
- Peripheral artery disease (PAD)
- Critical limb ischemia
- Acute limb ischemia
Other complications
- Chronic kidney disease
- Mesenteric artery ischemia
- Organ failure
Heart-related complications
Coronary artery disease (CAD)
When atherosclerosis affects the coronary arteries, plaque buildup narrows the blood vessels and reduces oxygen supply to the heart muscle. This results in myocardial ischemia, leading to chest pain and increasing the risk of myocardial infarction.
Heart failure
Blocked heart arteries from plaque reduce blood flow to the heart muscle over time. Muscle weakens, and the heart can't pump well, leading to heart failure.
Aortic aneurysm
Atherosclerosis weakens the arterial wall of the aorta by chronic inflammation and degeneration of elastic tissue. This weakening causes abnormal dilation of the vessel, forming an aneurysm, which may rupture and cause fatal internal bleeding.
Arrhythmia
Arrhythmia occurs due to reduced blood flow to the myocardium, which can damage the heart’s electrical conduction system. Ischemic myocardial tissue becomes electrically unstable, leading to abnormal heart rhythms.
Cardiac arrest
Severe atherosclerosis can lead to sudden cardiac arrest caused by acute myocardial ischemia, fatal arrhythmias, or massive myocardial infarction, resulting in a sudden loss of effective heart function.
Heart attack (myocardial infarction)
Rupture of an atherosclerotic plaque in a coronary artery leads to thrombus formation and complete arterial occlusion. This abruptly cuts off the blood supply, causing irreversible death of heart muscle tissue.
Brain-related complications
Stroke
Plaque in neck/brain arteries breaks off and blocks smaller brain arteries, or severe narrowing cuts off brain blood flow. Both cause stroke.
Transient ischemic attack (TIA)
Atherosclerosis of the carotid or cerebral arteries may temporarily reduce cerebral blood flow due to blockage or embolisation. This causes short-lived neurological deficits that resolve within 24 hours but signal a high risk of stroke.
Vascular dementia
Chronic reduction of cerebral blood flow due to widespread atherosclerosis leads to repeated small ischemic injuries in the brain. Eventually, this results in progressive cognitive decline and memory impairment.
Peripheral vascular complications
Peripheral artery disease (PAD)
Atherosclerosis in limb arteries, particularly in the legs, reduces blood flow and causes muscle ischemia. This leads to intermittent claudication, characterised by pain during walking.
Critical limb ischemia
Advanced PAD causes a severe and persistent reduction in blood supply, resulting in rest pain, non-healing ulcers, tissue necrosis, and increased risk of limb loss.
Acute limb ischemia
Sudden occlusion of an artery due to plaque rupture or embolism causes abrupt cessation of blood flow. This is a medical emergency that can rapidly lead to gangrene (tissue death) if not treated promptly.
Other complications
Chronic kidney disease
Atherosclerosis of the renal arteries reduces blood supply to the kidneys, which impairs the filtration function. Persistent ischemia leads to progressive kidney damage and ultimately leads to renal failure.
Mesenteric artery ischemia
When atherosclerosis affects the arteries supplying the intestines, it causes abdominal pain, especially after meals. Severe or sudden blockage can lead to intestinal infarction.
Organ failure
Prolonged ischemia due to arterial narrowing deprives organs of oxygen and nutrients. This results in tissue damage and loss of function, ultimately leading to organ failure.
Atherosclerosis Diagnosis
Atherosclerosis is a silent disease in its early stages and is usually diagnosed through a combination of clinical evaluation, laboratory tests, and imaging studies. The goal of diagnosis is to detect plaque buildup, assess the severity of arterial narrowing, and identify complications. Below are the atherosclerosis tests and diagnosis:
- Medical history
- Physical examination
- Screening tests
- Blood pressure check-up
- Record body mass index (BMI)
- Laboratory examinations
- Blood tests
- Lipid profile
- High-sensitivity C-reactive protein (hs-CRP)
- Renal function tests (RFT)
- Fasting blood glucose
- Non-invasive diagnostic tests
- Vascular function tests
- Ankle-brachial index (ABI) test
- Electrocardiogram (ECG/EKG)
- Echocardiogram
- Exercise stress test
- Imaging studies
- Carotid/Doppler ultrasound
- Coronary artery calcium (CAC) score (CT-based)
- Computed tomography angiography (CTA)
- Cardiac magnetic resonance imaging (MR angiography)
- Cardiac positron emission tomography (PET) scanning
- Invasive diagnostic tests
- Conventional angiography
- Genetic testing (selected high-risk cases)
Atherosclerosis Treatment
Management of atherosclerosis aims to slow disease progression, prevent complications, improve blood flow, and reduce cardiovascular risk. Management of atherosclerosis includes lifestyle modification, medications, and interventional or surgical procedures, depending on disease severity. Atherosclerosis treatment options include the following:
Non-pharmacological treatment of atherosclerosis
- Lifestyle modification
- Regular physical activity
- Weight reduction
- Stress management
Pharmacotherapy of atherosclerosis
- Lipid-lowering therapy
- Antiplatelet therapy
- Blood pressure control
- Glycemic control (in diabetes)
- Antianginal therapy
- Vasodilators
- Thrombolytic medicines
Surgical management of atherosclerosis
- Percutaneous coronary interventions (PCI)
- Coronary artery bypass grafting (CABG)
- Coronary endarterectomy
- Carotid endarterectomy
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support

Atherosclerosis Prevention
Atherosclerosis is a preventable disease because many of its major risk factors are related to lifestyle and long-term health behaviours. Early and consistent prevention can significantly reduce the development and progression of atherosclerosis and its complications. Important preventive steps are:
- Ensuring a healthy diet
- Performing physical activity regularly
- Managing lifestyle habits
- Reducing stress levels
- Controlling medical conditions
- Taking medications as prescribed
Ensuring a healthy diet: It is the primary prevention of atherosclerosis. A healthy diet rich in fruits, vegetables, whole grains, lean chicken, and healthy fats helps lower LDL cholesterol and reduce inflammation. Limiting saturated fats, trans fats, salt, and added sugars prevents lipid accumulation in arterial walls and protects endothelial function.
Performing physical activity regularly: Regular physical activity helps to improve blood circulation, increases HDL cholesterol, and lowers LDL cholesterol and triglycerides. Exercise also helps control blood pressure, body weight, and blood glucose levels, all of which reduce artery damage and slow the progression.
Managing lifestyle habits: Managing lifestyle habits like avoiding smoking and limiting alcohol consumption are crucial preventive steps. Smoking damages the endothelium, promotes LDL oxidation, and increases plaque development, whereas chronic alcohol intake contributes to hypertension and dyslipidemia. These important lifestyle tips reduce vascular injury and chronic inflammation.
Reducing stress levels: Chronic stress increases blood pressure and stress hormone levels, which can damage blood vessels and promote inflammation. Effective stress management via relaxation techniques, adequate sleep, and mindfulness helps maintain vascular health and lowers the risk of atherosclerosis.
Controlling medical conditions: Proper management of medical conditions such as high blood pressure, diabetes mellitus, and cholesterol is essential in preventing atherosclerosis.
Taking medications as prescribed: Adherence to prescribed medications such as statins, antihypertensives, antidiabetic drugs, and antiplatelet agents helps maintain optimal cholesterol levels, blood pressure, and blood glucose.
Difference between Atherosclerosis and Arteriosclerosis
Atherosclerosis vs arteriosclerosis
Both atherosclerosis and arteriosclerosis affect the arteries and are major contributors to cardiovascular disease. Because they are closely related and often discussed together, these terms are frequently confused or used interchangeably. However, they are not the same condition. Distinguishing between atherosclerosis and arteriosclerosis is essential for understanding the disease.
Atherosclerosis and arteriosclerosis differences are discussed below:
| Parameters | Atherosclerosis | Arteriosclerosis |
|---|---|---|
| Definition | Atherosclerosis is a specific pathological condition characterised by the formation of lipid-rich, fibrofatty plaques within the arterial wall, leading to narrowing of the arterial lumen. | Arteriosclerosis is a broad term that refers to generalised thickening, hardening, and loss of elasticity of arteries, usually associated with ageing. |
| Primary causes | Caused by endothelial injury, hyperlipidemia, smoking, diabetes, hypertension, and chronic inflammation. | Caused mainly by ageing, loss of elastic fibers, increased collagen deposition, and vascular stiffening. |
| Plaque formation | Present | Absent |
| Type of arteries affected | Mainly large and medium-sized arteries such as the coronary, carotid, cerebral, and peripheral arteries. | Can affect arteries of all sizes, including small arterioles. |
| Complications | Thrombosis, embolism, aneurysm formation, tissue infarction, and sudden death. | Mainly contributes to chronic hypertension and end-organ strain. |
Frequently Asked Questions (FAQs) on Atherosclerosis
What is atherosclerosis?
Atherosclerosis is a long-term disease in which fatty substances, cholesterol, calcium, and inflammatory cells gradually build up inside the arteries. It is a slow inflammatory process that begins early in life and progresses silently for years.
Can atherosclerosis be reversed?
Atherosclerosis cannot be completely reversed once plaques are well-formed, but its progression can be slowed or partially improved through lifestyle changes such as healthy eating, regular physical activity, and stopping smoking, which stabilise plaques and reduce inflammation. Atherosclerosis medication, like cholesterol-lowering drugs, can shrink plaque size slightly and lower the risk of rupture.
How to avoid atherosclerosis?
Atherosclerosis can be prevented by controlling risk factors. This may include eating a diet low in saturated fat and high in fruits, veggies, and protein, regular physical activity, maintaining a healthy weight, and avoiding tobacco. Managing medical conditions like blood pressure, blood sugar, and cholesterol levels is also important. These measures reduce artery inflammation and plaque formation.
What causes atherosclerosis?
The etiology of atherosclerosis begins with damage to the inner lining of arteries. This damage is commonly caused by high cholesterol (especially high LDL), smoking, high blood pressure, diabetes, obesity, and chronic inflammation. Once the lining is injured, cholesterol enters the artery wall and triggers an inflammatory response, leading to plaque formation.
Which layer of the artery wall thickens most in atherosclerosis?
The inner layer of the arterial wall, also known as the intima, thickens the most during atherosclerosis. Saturated fat, cholesterol, inflammatory cells, and calcium build-up in this layer, producing plaques. As the intima thickens, the artery's inner opening narrows, decreasing blood flow. This process explains why atherosclerosis leads to reduced oxygen supply to important organs and increases the risk of blockage.
Can someone live a long life with atherosclerosis?
Yes, many people live long lives with atherosclerosis, especially when it is detected early and well-controlled. If a person controls their risk factors greatly reduces atherosclerosis- related complications. Lifestyle modifications and appropriate medications help prevent plaque growth and rupture.
Is atherosclerosis hereditary?
Yes, atherosclerosis can be partly hereditary. Genetic factors can influence how the body handles cholesterol, inflammation, and blood vessel health. People with a family history of heart disease have a higher risk of developing atherosclerosis at a younger age. However, genes alone do not cause the disease; lifestyle factors and medical conditions strongly affect it.
Who is at risk for atherosclerosis?
People who are at risk for atherosclerosis include those with high blood pressure, high cholesterol, obesity, diabetes, or a family history of heart disease or stroke. Lifestyle choices such as smoking, physical inactivity, unhealthy eating habits, and chronic stress can also increase the risk. In addition, older adults are more likely to develop atherosclerosis, and men tend to be affected earlier than women, although women’s risk rises after menopause. Certain medical conditions, including chronic kidney disease and inflammatory disorders, may further contribute to the development of atherosclerosis.
How does diabetes cause atherosclerosis?
Diabetes accelerates atherosclerosis by damaging the inner lining of blood vessels. Chronic high blood glucose increases inflammation and oxidative stress, making arteries more vulnerable to cholesterol buildup. Diabetes also alters fat metabolism, raising harmful LDL cholesterol and lowering protective HDL cholesterol. These changes enhance plaque formation and rapid artery narrowing.
Can atherosclerosis cause hypertension?
Yes, atherosclerosis can lead to hypertension by making arteries stiffer and narrower. Healthy arteries stretch easily to handle blood flow, but plaque-filled arteries lose elasticity. As a result, the heart must pump harder to push blood through, increasing blood pressure.
How does LDL cause atherosclerosis?
Low-density lipoprotein (LDL) cholesterol plays a major role in atherosclerosis. LDLs are the particles that enter the inner artery wall and get oxidised. This triggers inflammation and attracts immune cells, which absorb LDL and form fatty plaques. Eventually, these plaques grow, harden, and narrow the artery. High LDL levels directly increase plaque formation and raise the risk of heart attack and stroke.
What is premature atherosclerosis?
Premature atherosclerosis (PreAS) is the early development of artery plaque at a younger age than expected, before the age of 40-45. It is linked to strong risk factors such as genetic disorders, diabetes, smoking, obesity, high cholesterol, and chronic inflammation. Because it develops silently, symptoms may appear suddenly as a heart attack or stroke.
What are the symptoms of atherosclerosis?
Atherosclerosis often causes no symptoms in its early stages. Symptoms appear when arteries become significantly narrowed or blocked. These depend on the affected artery and may include chest pain, shortness of breath, leg pain while walking, numbness, or weakness. If plaques rupture and form clots, sudden events like a heart attack or stroke can occur.
What are the external markers of atherosclerosis?
External markers of atherosclerosis are physical signs that suggest underlying artery disease. Some findings include xanthelasma (yellow cholesterol deposits around the eyes), tendon xanthomas (slowly enlarging subcutaneous nodules), and reduced or absent pulses in limbs. In some cases, a carotid bruit (abnormal sound over neck arteries) may be detected during examination.
What is atherosclerosis, and how does it affect the body?
Atherosclerosis is a condition where the blood vessels become narrowed and hardened due to a build-up of plaque. This plaque is made up of fat, cholesterol, and other substances found in the blood. Over time, this narrowing makes it harder for blood to flow through the arteries, which can lead to problems in vital organs, like the heart and brain. When the blood flow is restricted, the organs don’t get the oxygen and nutrients they need, which can lead to serious health problems such as heart disease, stroke, or kidney damage.
Are atherosclerosis and arteriosclerosis the same?
No, atherosclerosis and arteriosclerosis are related but not the same. Both affect the arteries, but in different ways:
- Atherosclerosis is the build-up of plaque (fat, cholesterol, and other substances) inside the arteries, which causes them to narrow and stiffen.
- Arteriosclerosis, on the other hand, refers to the general hardening and thickening of the arterial walls, this happen due to aging or other factors. While atherosclerosis is a type of arteriosclerosis, not all arteriosclerosis is caused by plaque build-up
What are atherosclerotic plaques made of?
Atherosclerotic plaques are composed of fat, cholesterol, calcium, and cellular waste, which accumulate within the arterial wall. As these fatty streaks develop, they are capped by fibrous tissue, and inflammatory cells can make them unstable and prone to rupture, leading to potential heart attacks and stroke.
Can atherosclerosis cause a heart attack?
Yes, atherosclerosis can cause a heart attack. When plaque builds up in the coronary arteries, it can eventually rupture or break open. When this happens, a blood clot can form at the site, completely blocking blood flow to the heart. Without proper blood supply, the heart muscle starts to die, leading to a heart attack. It’s important to manage the risk factors for atherosclerosis, such as high cholesterol, high blood pressure, and smoking, to reduce the chance of a heart attack.
Can atherosclerosis go away?
Atherosclerosis is a progressive condition, meaning it generally worsens over time if not managed properly. While it can’t be fully reversed, it can be slowed or managed with lifestyle modifications and medications. With the right treatment, the progression of the disease can be halted, and in some cases, plaque build-up can be reduced or stabilized. However, it's important to make long-term changes to diet, exercise, and other risk factors to keep it under control.
Is atherosclerosis curable?
Currently, there is no cure for atherosclerosis, but it can be managed and treated. Early detection and lifestyle changes, such as improving diet, increasing exercise, smoking cessation, and managing stress, can significantly reduce the progression of the disease. Some drugs and medical procedures, including as angioplasty or bypass surgery, may be required to control problems or reduce plaque buildup. The main goal is to prevent severe health problems, such as heart attack or stroke, by controlling risk factors and maintaining a healthy lifestyle.
What kind of food causes atherosclerosis?
Certain foods can contribute to the development and worsening of atherosclerosis, especially those that increase cholesterol and inflammation in the body. These foods include:
- Trans fats: Found in many processed and fried foods (like baked goods, fast food, and margarine).
- Saturated fats: Found in fatty cuts of meat, full-fat dairy products, butter, and lard.
- Refined carbohydrates: Such as white bread, sugary snacks, and sodas, which can lead to high blood sugar and inflammation.
- Excess salt: Found in processed foods, which can increase blood pressure.
- Red and processed meats: These can be high in saturated fats and sodium, both of which can contribute to plaque build-up.
When to consult a doctor for atherosclerosis?
Consult a doctor for atherosclerosis if there are symptoms that suggest reduced blood flow to the heart, brain, or limbs. Many people have no early warning signs, so medical evaluation is important when risk factors are present. Signs that indicate a need for medical attention are:
- Chest pain, chest pressure, or discomfort during activity
- Shortness of breath or unusual fatigue
- Pain, cramping, or weakness in the legs while walking
- Numbness, weakness, or sudden difficulty speaking or seeing
- Coldness or poor wound healing in the feet or toes
If these symptoms continues, it is recommended to see a atherosclerosis doctor, who can assess in cardiovascular risk and start appropriate treatment. Seek emergency medical care for sudden angina, stroke-like symptoms, or severe breathlessness, as these may indicate life-threatening complications. A cardiologist can provide the right atherosclerosis treatment to manage symptoms and reduce long-term risks.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868