Successful Laparoscopic Fundoplication for GERD & Hiatal Hernia in a 31 Y.O. Male
PACE Hospitals
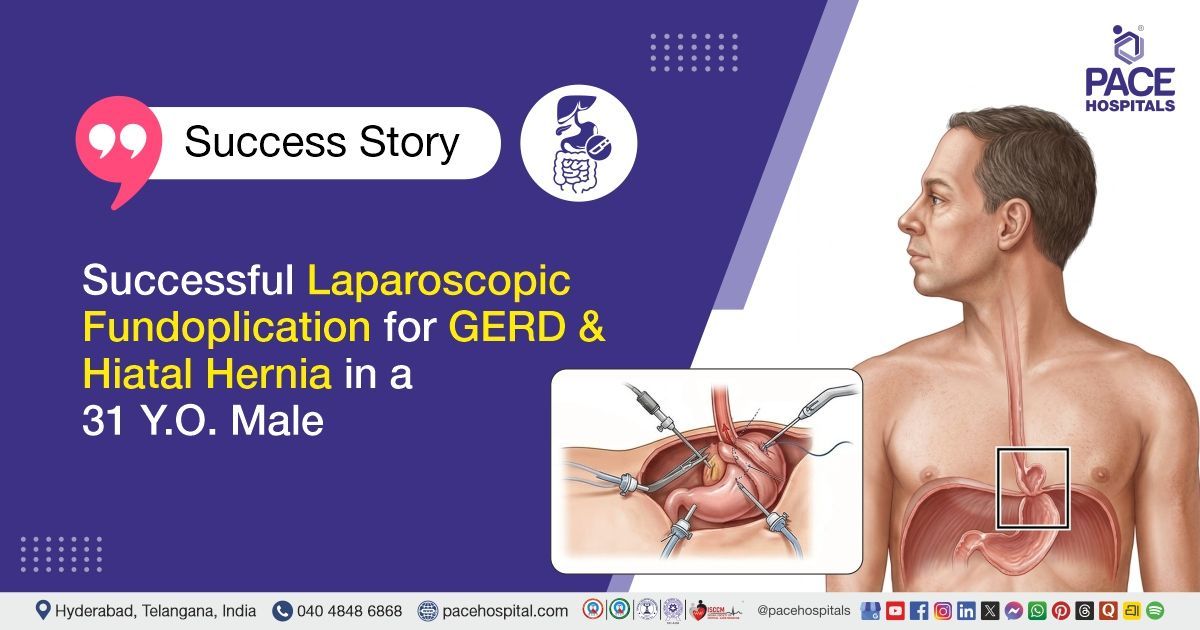
The PACE Hospitals' expert gastroenterology team successfully performed a Laparoscopic Fundoplication on a 31-year-old male patient diagnosed with Gastroesophageal Reflux Disease (GERD) associated with a hiatal hernia and H. pylori gastritis. The primary aim of the procedure was to reinforce the lower esophageal sphincter, prevent acid reflux, and repair the hiatal hernia, thereby alleviating symptoms such as heartburn and regurgitation, improving the patient’s quality of life, and reducing the risk of further complications.
Chief Complaints
A 31-year-old male patient with a body mass index (BMI) of 18 presented to the Gastroenterology Department at PACE Hospitals, Hitech City, Hyderabad, with chief complaints of excessive belching accompanied by regurgitation and reflux for the past 2.5 years, with worsening over the last 1.5 months. He also reported epigastric and retrosternal burning sensation for the same duration, which had similarly aggravated in the past 1.5 months. The symptoms were persistent and did not respond to medical therapy.
Past Medical History
The patient had no significant past medical history and was not known to have any comorbid conditions such as diabetes mellitus, hypertension, cardiovascular disease, or prior gastrointestinal disorders. There was no history of previous surgeries or long-term medication use.
On Examination
On general examination, the patient was conscious, coherent, and oriented. Vital parameters were within normal limits. On systemic examination, per abdomen was soft and non-tender. Overall, the clinical examination findings were within normal limits.
Diagnosis
Upon admission to PACE Hospitals, the patient was thoroughly evaluated by the Gastroenterology and Surgical Gastroenterology teams. He presented with a history of excessive belching associated with regurgitation and reflux for the past 2.5 years, with recent worsening over the last 1.5 months. He also complained of epigastric and retrosternal burning sensation for the same duration, which had aggravated recently. The symptoms were persistent and did not respond to medical therapy. Clinical assessment and history were suggestive of chronic gastroesophageal reflux disease with possible associated hiatal hernia.
The patient underwent further diagnostic evaluation. Upper gastrointestinal endoscopy revealed evidence of hiatal hernia along with erosive pangastritis, and rapid urease test was positive, suggestive of H. pylori infection. Esophageal manometry study was within normal limits but confirmed the presence of hiatal hernia. Routine laboratory investigations, including complete blood picture, were within normal limits except for relative neutrophilia. Overall clinical, endoscopic, and functional findings supported the diagnosis.
Based on the confirmed diagnosis, the patient was advised to undergo Hiatal Hernia and
Gastroesophageal Reflux Disease (GERD) Treatment in Hyderabad, India, under the expert care of the Gastroenterology Department to control reflux, repair the hiatal hernia, and provide long-term symptomatic relief while preventing further complications.
Medical Decision Making (MDM)
After a detailed consultation with the consultant Gastroenterologist, Dr. Govind Verma, Dr. M Sudhir, Dr. Padma Priya, along with cross-consultation from Dr. Suresh Kumar S, Dr. Krishna Prasad Chowdary MB, Surgical Gastroenterologists, a thorough evaluation was conducted considering the patient’s complaints, and all relevant laboratory and imaging investigations, including complete blood picture, upper gastrointestinal endoscopy, esophageal manometry, and Helicobacter pylori testing, were reviewed.
Based on the clinical and diagnostic evaluations, it was determined that laparoscopic fundoplication was identified as the most appropriate intervention to correct the hiatal hernia, strengthen the lower esophageal sphincter, manage the patient’s complaints, and prevent potential complications such as esophagitis or Barrett’s esophagus.
The patient and his family members were counselled regarding the diagnosis, the surgical procedure, associated risks, expected postoperative recovery, and the potential to improve quality of life.
Surgical Procedure
Following the decision, the patient was scheduled for Laparoscopic Fundoplication Surgery in Hyderabad at PACE Hospitals, under the expert care of the Gastroenterology Department.
The procedure involved the following steps:
- Anesthesia and Positioning: The patient was placed under general anesthesia with endotracheal intubation. He was positioned supine on the operating table, with slight reverse Trendelenburg to allow optimal visualization of the upper abdominal structures.
- Port Placement and Laparoscopic Access: A standard 4-5 port technique was used. Pneumoperitoneum was created with carbon dioxide to allow a working space in the abdominal cavity. The laparoscope and surgical instruments were introduced through the ports to access the esophageal hiatus and upper stomach.
- Hiatal Dissection and Hernia Reduction: The esophageal hiatus was carefully dissected, and the stomach and esophagus were mobilized. The hiatal hernia was identified, and the herniated portion of the stomach was reduced back into the abdominal cavity. Adhesions around the hiatus were carefully released to prevent injury to surrounding structures.
- Fundoplication: The fundus (upper part of the stomach) was wrapped around the lower esophagus to reinforce the lower esophageal sphincter. This 360-degree (Nissen) wrap was secured with sutures to prevent reflux. The wrap was calibrated to allow passage of the esophagus without obstruction while preventing reflux.
- Closure: The hiatus was reinforced with sutures to prevent recurrence of herniation. Pneumoperitoneum was released, ports were removed, and incisions were closed with absorbable sutures.
Postoperative Care
The procedure was uneventful. During the postoperative period, the patient was closely monitored and received supportive therapy including intravenous fluids for hydration, medications for infection prevention, agents to reduce gastric acid secretion, and other supportive treatments as indicated. The patient tolerated recovery well, remained hemodynamically stable, showed gradual improvement in symptoms, and was discharged in a clinically stable condition with advice for follow-up care.
Discharge Medications
Upon discharge, the patient was advised to continue medications for prevention of infection, management of gastric acid secretion, healing and protection of the stomach lining, symptomatic relief of pain as needed, and support for bowel regularity. These were prescribed with specific durations and timing instructions to ensure optimal recovery and to prevent postoperative complications.
Advice on Discharge
The patient was advised to start the Helicobacter pylori eradication kit at the follow-up visit. A liquid diet was recommended for the first seven days, followed by a semisolid diet for the subsequent two weeks.
Emergency Care
The patient was informed to contact the emergency ward at PACE Hospitals in case of any emergency or development of symptoms such as fever, abdominal pain, chest pain and vomiting.
Review and Follow-up Notes
The patient was advised to return for a follow-up visit with the Gastroenterologist in Hyderabad at PACE Hospitals, after 3 weeks, to review his condition.
Conclusion
This case highlights a patient with gastroesophageal reflux disease associated with a hiatal hernia, unresponsive to medical therapy. Following thorough evaluation and cross-consultation with gastroenterology and surgical teams, laparoscopic fundoplication was performed successfully. The procedure was uneventful, and the patient showed symptomatic improvement during the hospital stay. He was discharged in stable condition with appropriate postoperative care and follow-up plans.
Multidisciplinary Approach in Managing GERD with Hiatal Hernia
Management of gastroesophageal reflux disease with hiatal hernia often benefits from a multidisciplinary approach, involving a Gastroenterologist / Gastroenterology doctor, surgeons, and internal medicine specialists. Persistent or complicated cases require thorough evaluation with endoscopy, esophageal function testing, and relevant laboratory investigations to guide treatment. Surgical interventions, such as laparoscopic fundoplication, are considered when medical therapy fails or anatomical correction is needed. Minimally invasive procedures offer the advantage of reduced complications and faster recovery. Postoperative care focuses on symptom monitoring, infection prevention, and promoting healing. Coordinated care and individualized treatment planning are key to achieving optimal outcomes and improving quality of life for patients with these conditions.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868