Acute Kidney Injury (AKI): Symptoms, Causes & Treatment
PACE Hospitals
Written by: Editorial Team
Medically reviewed by: Dr. A Kishore Kumar - Consultant Nephrologist and Renal Transplant Physician
Acute kidney injury definition
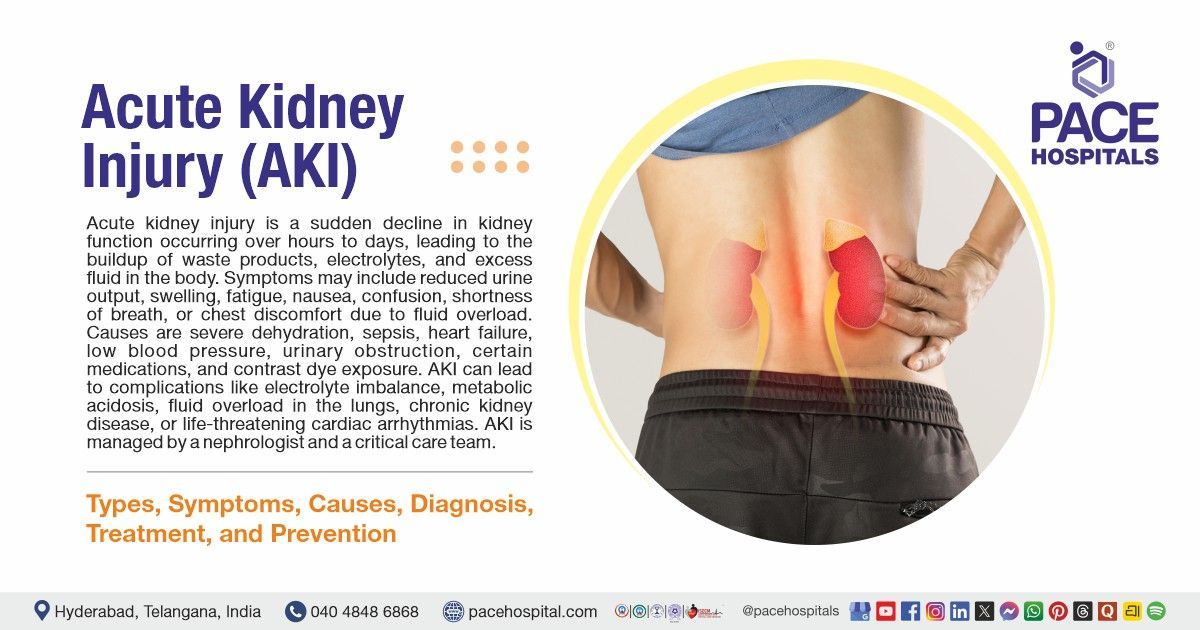
Acute kidney injury (AKI) is defined as a sudden decline in kidney function that develops over hours to days, leading to the buildup of waste products, electrolytes, and excess fluid in the body. It may present with reduced urine output, swelling of the legs or face, fatigue, nausea, confusion, shortness of breath (SOB), or chest discomfort due to fluid overload.
Common causes are severe dehydration, major infections (sepsis), heart failure, low blood pressure, urinary tract obstruction, certain medications (such as some antibiotics or pain relievers), and exposure to contrast dye. If left untreated, AKI can result in serious complications like electrolyte imbalance (high potassium), metabolic acidosis, fluid overload affecting the lungs, progression to chronic kidney disease, or even life-threatening cardiac arrhythmias (abnormal heart rhythm).
Management is usually led by a nephrologist along with critical care specialists in an intensive care unit (ICU), aiming to treat the underlying cause, stabilise fluids and electrolytes, and initiate dialysis when required.
Meaning of acute kidney injury
The term acute kidney injury is derived from Latin and English medical terminology.
- “Acute”: meaning sharp or sudden. In medical terms, it refers to a condition that develops rapidly over hours to days.
- “Kidney”: referring to the organ that filters blood and produces urine.
- “Injury”: meaning harm or damage.
The term acute kidney injury (AKI) replaced the older term “acute renal failure” in the early 2000s to better describe the full spectrum of sudden kidney dysfunction — ranging from mild impairment to complete kidney failure. This terminology was formally standardised by international expert groups such as the Kidney Disease: Improving Global Outcomes (KDIGO) guidelines to promote earlier diagnosis and intervention.
Acute Kidney Injury Epidemiology
Acute kidney injury epidemiology worldwide
AKI is a common and serious condition worldwide. Studies show that AKI affects about 10–20% of hospitalized patients and up to 30–50% of patients in intensive care units (ICUs). Globally, it is estimated that more than 130 lakh people develop AKI each year, with nearly 17 lakh deaths annually, especially in low- and middle-income countries. In high-income countries, AKI usually affects hospitalised patients due to sepsis, major surgery, or medications. In developing regions, it is linked to infections, dehydration, obstetric complications, and toxins.
Acute kidney injury epidemiology in India
In India, AKI is common and remains a major cause of hospital-related illness and death. Studies show that AKI occurs in about 5–7% of hospitalized patients and in 30–40% of ICU patients. In India, sepsis is the leading cause of AKI, especially in critically ill patients. Community-acquired AKI is frequently caused by dehydration, infections, snake bites, obstetric complications, and nephrotoxic drugs, while hospital-acquired AKI is linked to sepsis, major surgeries, and contrast exposure. Mortality in severe AKI cases may range from 20–50%, particularly when dialysis is required.
Types of AKI
Acute kidney injury is classified into three main types based on the underlying cause and where the problem occurs in relation to the kidneys. The following are the types of acute kidney injury:
- Prerenal acute kidney injury
- Intrarenal (intrinsic) acute kidney injury
- Postrenal acute kidney injury
Prerenal acute kidney injury
This type occurs when there is a reduction in blood flow to the kidneys without direct structural damage. Because the kidneys depend on an adequate blood supply to filter waste, any condition that decreases circulation—such as dehydration, severe blood loss, heart failure, low blood pressure, or sepsis—can impair kidney function. The kidney tissue itself is initially normal, and function often improves once blood flow is restored.
Intrarenal (Intrinsic) acute kidney injury
This type develops due to direct damage to the kidney structures, including the tubules, glomeruli, blood vessels, or interstitial tissue. Causes include prolonged reduced blood flow, severe infections, toxins, certain medications, autoimmune disorders, or acute tubular necrosis.
Postrenal acute kidney injury
This type occurs when there is an obstruction to urine flow after it leaves the kidneys. Blockages increase pressure within the urinary system and impair kidney filtration. Common causes are enlarged prostate, kidney stones, tumors, or ureteral strictures.
Acute Kidney Injury (AKI) Symptoms
Acute kidney injury is a sudden decline in kidney function that can range from mild to life-threatening. Symptoms may develop over hours to days, and sometimes are subtle in the early stages. Common signs and symptoms of acute kidney injury include:
- Oliguria (reduced urine output)
- Swelling in the legs, ankles, face, or around the eyes
- Shortness of breath
- Fatigue and weakness
- Nausea, vomiting, and loss of appetite
- Chest pain or pressure
- High blood pressure
- Confusion or mood changes
- Flank pain
Oliguria (reduced urine output): In acute kidney injury, the kidneys lose their ability to filter blood and produce urine effectively. As kidney function declines, urine output decreases because waste products and excess fluid are not properly excreted. Oliguria is often one of the earliest and most important warning signs of AKI, especially in hospitalized or critically ill patients.
Swelling in the legs, ankles, face, or around the eyes: When the kidneys cannot remove excess fluid from the body, fluid accumulates in tissues. This leads to visible swelling, particularly in dependent areas such as the legs and ankles, and sometimes around the eyes.
Shortness of breath (SOB): Fluid overload caused by kidney failure can result in fluid accumulation in the lungs (called pulmonary edema). This makes breathing difficult and may cause rapid or laboured breathing. Shortness of breath in AKI can indicate a serious complication requiring immediate medical attention.
Fatigue and weakness: As waste products such as urea and creatinine build up in the bloodstream, they affect overall body function. Additionally, electrolyte imbalances and anemia may also develop. These changes contribute to generalized weakness, low energy levels, and decreased physical stamina.
Nausea, vomiting, and loss of appetite: The buildup of toxins in the blood (uremia) irritates the gastrointestinal system. This can result in nausea, vomiting, metallic taste in the mouth, and loss of appetite. These symptoms are common when kidney dysfunction becomes more pronounced.
Chest pain or pressure: In severe acute kidney injury (AKI), excess fluid may build up around the heart (pericardial effusion), or electrolyte disturbances such as high potassium may affect heart rhythm. These changes can cause chest discomfort or pressure and may indicate a life-threatening complication.
High blood pressure: The kidneys play a key role in controlling blood pressure by managing fluid balance and hormone release. When kidney function declines, fluid retention and hormonal imbalance lead to higher blood pressure.
Confusion or mood changes: Accumulation of toxins and severe electrolyte imbalances can affect brain function. Patients may experience confusion, reduced alertness, irritability, or altered mental status. In advanced cases, this can progress to severe neurological complications.
Flank pain: Pain in the side of the lower back may occur when AKI is caused by obstruction (such as kidney stones) or inflammation. It can indicate increased pressure within the kidneys or associated infection.
Causes of Acute Kidney Injury (AKI)
A sudden decline in kidney function occurs due to decreased blood flow to the kidneys, direct kidney damage, or obstruction of urine flow. The acute kidney injury etiology is commonly classified into prerenal, intrinsic (intrarenal), and postrenal causes. These categories help identify the underlying factors contributing to kidney injury and guide appropriate management.
Prerenal cause of acute kidney injury
- Severe dehydration
- Major blood loss or trauma
- Low blood pressure (shock)
- Sepsis (severe infection)
- Heart failure or cardiogenic shock
- Severe liver disease
Intrarenal cause of acute kidney injury
- Acute tubular necrosis
- Certain medications
- Autoimmune diseases
- Vasculitis
Postrenal cause of acute kidney injury
- Enlarged prostate
- Kidney stones
- Tumors compressing urinary tract
- Blood clots
- Ureteral strictures
Prerenal cause of acute kidney injury
Severe dehydration: A drop in blood volume reduces blood flow to the kidneys. Since the kidneys need adequate blood flow to filter waste products and balance electrolytes, decreased blood flow lowers the glomerular filtration rate (GFR). This leads to buildup of waste products like urea and creatinine. If prolonged, it can cause prerenal acute kidney injury.
Major blood loss or trauma: Significant hemorrhage reduces blood volume and oxygen delivery to the kidneys. The body prioritises blood flow to vital organs, further decreasing kidney perfusion and causing prerenal AKI.
Low blood pressure (shock): In shock states, systemic hypotension reduces the pressure required to push blood through the glomeruli. Without sufficient perfusion pressure, the kidneys cannot filter blood effectively. Prolonged hypotension may first cause prerenal AKI and, if uncorrected, can progress to intrinsic kidney damage.
Sepsis (severe infection): Sepsis causes widespread inflammation and vasodilation throughout the body, leading to decreased effective circulating blood volume and hypotension. Inflammatory mediators also increase vascular permeability, causing fluid to leak from blood vessels into tissues. These changes reduce blood flow to the kidneys.
Heart failure or cardiogenic shock: When the heart cannot pump effectively, cardiac output decreases. As a result, less blood reaches the kidneys. Reduced renal perfusion lowers GFR and causes retention of nitrogenous waste, leading to prerenal AKI.
Severe liver disease: Advanced liver disease (such as cirrhosis) can cause abnormal blood circulation and reduced effective blood flow to the kidneys. A condition known as hepatorenal syndrome may develop, where kidney function declines despite structurally normal kidneys.
Intrarenal cause of acute kidney injury
Acute tubular necrosis (ATN): This happens when kidney tubular cells are destroyed as a result of chronic low blood flow or toxic exposure. The damaged tubules cannot filter waste correctly, resulting in abrupt kidney failure.
Certain medications: Some medicines can reduce blood flow to the kidneys or directly damage kidney tissues. Drugs such as certain antibiotics, pain relievers (NSAIDs), contrast dyes, and chemotherapy agents may trigger acute kidney injury, especially in high-risk patients.
Autoimmune diseases: In autoimmune conditions, the immune system attacks kidney tissues, causing inflammation of the filtering units. This damage reduces the kidneys’ ability to remove waste and regulate fluids, leading to acute kidney injury.
Vasculitis: Vasculitis causes inflammation and narrowing of blood vessels supplying the kidneys. Reduced blood flow can deprive kidney tissues of oxygen, resulting in sudden impairment of kidney function.
Postrenal cause of acute kidney injury
Enlarged prostate: An enlarged prostate can block the flow of urine from the bladder. When urine cannot drain properly, pressure builds up in the urinary tract and backs up toward the kidneys. This obstruction reduces kidney function and may lead to postrenal acute kidney injury (AKI) if not relieved promptly.
Kidney stones: Kidney stones can obstruct the ureters. A complete or severe blockage prevents urine from passing, causing increased pressure inside the kidneys.
Tumors compressing the urinary tract: Tumors in or near the urinary tract (such as bladder, prostate, or pelvic tumors) may compress or block urine flow. When urine drainage is obstructed, it leads to back pressure in the kidneys, reducing their ability to filter blood effectively.
Blood clots: Blood clots within the urinary tract can block urine flow. Similar to stones or tumors, this obstruction causes urine to accumulate and increases pressure inside the kidney.
Ureteral strictures: These are abnormal narrowing of the ureters, often due to prior surgery, infection, or injury. This narrowing restricts urine flow from the kidneys to the bladder. Continuous obstruction increases pressure within the kidney and can lead to acute kidney injury.
Risk Factors for Acute Kidney Injury (AKI)
Certain patient characteristics, comorbid conditions, and clinical exposures increase the likelihood of developing AKI. Identifying these risk factors is essential for early recognition, prevention, and timely management to reduce morbidity and mortality. The frequent risk factors of acute kidney injury include:
Modifiable risk factors
Factors that can be changed or controlled to reduce the risk of a disease.
- Sepsis
- Major surgery
- ICU admission–related factors
- Use of nephrotoxic drugs
- Severe dehydration
- Exposure to contrast dye
Non-modifiable risk factors
Factors that cannot be changed and are inherent
Modifiable risk factors
Sepsis: Sepsis is a severe, widespread infection that causes inflammation, low blood pressure, and impaired blood flow to vital organs. This lowers kidney perfusion and inflammatory damage make sepsis one of the leading risk factors for AKI.
Major surgery: During major surgeries, fluctuations in blood pressure, blood loss, use of anesthesia, and exposure to certain medications can temporarily reduce kidney blood flow. Cardiac surgeries, in particular, are strongly associated with postoperative AKI.
ICU admission–related factors: Patients admitted to the ICU are usually critically ill and may have unstable blood pressure, severe infections, or multi-organ failure. They often require strong medications and mechanical ventilation, all of which increase the likelihood of kidney injury.
Use of nephrotoxic drugs: Certain medications, such as non-steroidal anti-inflammatory drugs (NSAIDs), some antibiotics, and other toxic agents, can directly injure kidney cells or reduce blood flow within the kidneys.
Severe dehydration: Loss of body fluids from vomiting, diarrhea, fever, or burns reduces circulating blood volume. When kidney blood flow decreases significantly, it can lead to prerenal AKI if not corrected promptly.
Exposure to contrast dye: Contrast agents used in imaging procedures (such as CT scans or angiography) may cause temporary kidney injury, especially in patients with diabetes, CKD, or dehydration. This condition is referred to as post contrast acute kidney injury.
Non-modifiable risk factors
Advanced age: With increasing age, kidney function naturally declines due to reduced kidney blood flow and loss of functioning kidney units (nephrons). Elderly patients also commonly have multiple medical conditions and take several medications, which increases their vulnerability to acute kidney injury during illness, surgery, or dehydration.
Underlying chronic conditions: If a person is suffering from chronic diseases like diabetes, hypertension, and chronic kidney disease (CKD) reduce the kidney’s functional reserve. When an additional stress, such as infection, low blood pressure, or medication exposure occurs, the kidneys may not tolerate it well, which increases the risk.
Patients with heart failure and liver disease: Heart failure reduces effective blood circulation to the kidneys, while severe liver disease alters blood flow and fluid balance. Both conditions affect kidney perfusion and make the kidneys more susceptible to acute damage.
Complications of Acute Kidney Injury (AKI)
Acute kidney injury can lead to multiple systemic complications due to the sudden decline in renal function and the accumulation of metabolic waste products, fluid, and electrolytes. The complications associated with acute kidney injury include:
- Fluid overload
- Electrolyte imbalance
- Metabolic acidosis
- Uremia (accumulation of waste products)
- Cardiac arrhythmias
- Need for dialysis
- Increased risk of infections
- Progression to chronic kidney disease (CKD)
- Multi-organ failure
- Increased mortality
Fluid overload: When the kidneys fail to remove excess fluid, it accumulates in the body. This can cause swelling in the legs, face, and lungs (pulmonary edema), leading to breathing difficulty and worsening heart function.
Electrolyte imbalance: The kidneys regulate electrolytes such as potassium. In AKI, potassium levels may rise dangerously (hyperkalemia), which can cause life-threatening heart rhythm disturbances.
Metabolic acidosis: AKI reduces the kidney’s ability to remove acids from the blood. This leads to metabolic acidosis, a condition where the blood becomes too acidic, causing rapid breathing, fatigue, and worsening organ function.
Uremia (accumulation of waste products): Waste products like urea and creatinine build up in the bloodstream when kidney function declines. Uremia can cause nausea, vomiting, confusion, itching, and in severe cases, altered consciousness.
Cardiac arrhythmias: Prolonged electrolyte disturbances and acid-base imbalance can affect the heart’s electrical activity, leading to irregular heartbeats that may be dangerous.
Need for dialysis: In severe cases of AKI, the kidneys may stop functioning adequately to remove waste products, excess fluid, and electrolytes from the blood. In such situations, dialysis may be required temporarily to perform the filtering function of the kidneys until kidney function improves.
Increased risk of infections: Patients with AKI, especially those in the ICU or on dialysis, have weakened immunity and a higher risk of hospital-acquired infections.
Progression to chronic kidney disease (CKD): Some patients do not fully recover kidney function after AKI. Persistent damage can lead to CKD or even end-stage kidney disease over time.
Multi-organ failure: Severe AKI often occurs as part of critical illness and may contribute to failure of other organs such as the heart, lungs, or liver.
Increased mortality: AKI significantly increases the risk of death, particularly in critically ill patients or those requiring dialysis.
Acute Kidney Injury (AKI) Diagnosis
The diagnosis of acute kidney injury (AKI) focuses on identifying a sudden decline in kidney function at an early stage. Since symptoms may not appear immediately, doctors rely mainly on blood tests and urine output monitoring to detect changes in kidney performance. Early diagnosis is important to determine the cause, assess severity, and start timely treatment to prevent serious complications.
The following are the steps involved in the diagnosis of acute kidney Injury (AKI):
- Medical history
- Physical examination
- Confirm AKI using laboratory criteria (acute kidney injury definition KDIGO)
- Serum creatinine
- Urine output
- Laboratory investigations
- Blood tests
- Blood urea nitrogen (BUN)
- Estimated glomerular filtration rate (eGFR)
- Comprehensive metabolic panel
- Serum electrolyte
- Acid–base balance
- Urine examination
- Urine electrolytes
- Urine studies
- Urine microscopy
- Protein/ creatinine ratio
- Advanced labs (selected patients)
- Serum & urine protein electrophoresis (especially in older adults)
- Novel biomarkers
- Imaging studies
- Renal ultrasound
- Computed tomography (CT scan)
- Invasive studies (rare)
- Kidney biopsy
Acute Kidney Injury (AKI) Treatment
Management of Acute kidney injury (AKI) primarily focuses on identifying and treating the underlying cause, maintaining fluid and electrolyte balance, preventing further kidney injury, and initiating renal replacement therapy when indicated. Treatment options for acute kidney injury include the following:
Immediate assessment and stabilization
- Assess airways, breathing and circulation
- Hemodynamic optimisation (vasopressors for shock)
- Continuous monitoring (e.g., serum creatinine, urine output, AKI staging)
Non-pharmacological management
- Identify & treat the underlying cause
- Fluid management
- Electrolyte & metabolic monitoring
- Dietary management
- Avoiding nephrotoxic drugs
Pharmacological management
- Management of hyperkalemia (Emergency if K⁺ >6.5 mmol/L)
- IV Calcium gluconate
- Shift potassium into cells
- Remove potassium through loop diuretics or dialysis
- Fluid overload
- IV loop diuretics
- Metabolic acidosis
- IV sodium bicarbonate (if severe, pH <7.1)
- Specific cause-based treatment
- Glomerulonephritis: Steroids / immunosuppressants
- Rhabdomyolysis: aggressive IV fluids
- Sepsis: IV antibiotics + supportive care
- Hypertension: calcium channel blockers and beta blockers (dose-adjusted)
Procedural management
- Renal replacement therapy (RRT)
- Hemodialysis
- Continuous renal replacement therapy (CRRT)
- Urinary catheterization
Surgical management
- Relief of obstruction
- Ureteric stenting
- Percutaneous nephrostomy
- Surgery for:
- Prostatic enlargement
- Tumors
- Renal stones causing obstruction
Why Choose PACE Hospitals?
Expert Super Specialist Doctors
Advanced Diagnostics & Treatment
Affordable & Transparent Care
24x7 Emergency & ICU Support
Prevention of Acute Kidney Injury
Acute kidney injury is largely preventable if risk factors are identified early and appropriate precautions are taken. The main aim of prevention is to maintain adequate renal perfusion, avoid kidney toxins, and promptly manage underlying conditions. This includes:
- Maintaining proper hydration
- Managing chronic conditions
- Avoiding nephrotoxic substances
- Early management of infections & sepsis
- Avoiding contrast dyes
- Proper perioperative care
- Prevent postrenal obstruction
Maintaining proper hydration: It is essential to ensure adequate blood flow to the kidneys. Dehydration from vomiting, diarrhea, burns, or blood loss needs to be corrected promptly with oral or intravenous fluids, while avoiding fluid overload.
Managing chronic conditions: Conditions like diabetes, hypertension, chronic kidney disease (CKD), and heart failure all reduce vulnerability to AKI. Proper blood sugar and blood pressure control, as well as regular monitoring of renal function, all contribute to kidney health.
Avoiding nephrotoxic substances: Medications like NSAIDs, aminoglycosides, certain antifungals, chemotherapy drugs, and radiographic contrast agents are important. If these drugs are necessary, they need to be used in the lowest effective dose with dose adjustment according to renal function.
Early management of infections and sepsis: This helps to prevent kidney damage caused by hypotension and inflammation. Prompt antibiotic therapy, adequate fluid resuscitation, and maintenance of blood pressure are crucial.
Avoiding contrast dyes: Avoiding unnecessary contrast dyes, especially in high-risk patients, reduces the risk of contrast-induced kidney injury. Adequate hydration before and after procedures further reduces the risk.
Proper perioperative care: This includes maintaining blood pressure and adequate fluid balance, which helps to prevent reduced kidney blood flow and ischemic injury.
Preventing postrenal obstruction: Early detection and treatment of urinary retention, prostate enlargement, or kidney stones also protects against AKI.
Acute kidney injury vs Chronic kidney disease
Both Acute kidney injury (AKI) and chronic kidney disease (CKD) affect how well the kidneys filter waste and balance fluids, but they differ mainly in how quickly they develop, how long they last, and whether they are reversible. The table below discusses about the differences between AKI and CKD:
| Parameters | Acute kidney injury (AKI) | Chronic kidney disease (CKD) |
|---|---|---|
| Definition | Acute kidney injury is a sudden decline in kidney function that occurs over a short period of time. | Chronic kidney disease is a gradual and progressive loss of kidney function that occurs over months or years. |
| Onset | It develops rapidly, usually within hours to days. | It develops slowly over a long period, typically months to years. |
| Duration | It develops gradually over time, usually months to years. | The condition is long-term and usually irreversible. |
| Causes | It is commonly caused by dehydration, severe infections, shock, certain medications, or urinary obstruction. | It is most commonly caused by long-standing diabetes, hypertension, chronic glomerulonephritis, or inherited disorders. |
| Kidney size | The kidneys are usually normal in size or slightly enlarged. | The kidneys are usually small and shrunken in long-standing disease. |
| Urine output | Urine output is often reduced suddenly, though it may sometimes remain normal. | Urine output is usually normal in the early stages but decreases in advanced stages. |
Frequently Asked Questions (FAQs) on Acute Kidney Injury (AKI)
What is acute kidney injury (AKI)?
Acute kidney injury (AKI) is a condition in which the kidneys suddenly stop working properly over a short period, usually within hours or days. The kidneys normally remove waste products from the blood, balance body fluids, and regulate the excretion of important minerals. When AKI occurs, waste products accumulate in the body, and urine output may decrease. Some people may notice swelling, tiredness, shortness of breath, or reduced urination. In many cases, kidney function improves once the underlying problem is treated.
Can pneumonia cause acute kidney injury?
Yes, Pneumonia, which is a lung infection, can sometimes lead to AKI, especially if the infection is severe. Although pneumonia starts in the lungs, a serious infection can affect the entire body. It may lower blood pressure, reduce oxygen levels, and cause widespread inflammation. These changes can reduce blood flow and oxygen supply to the kidneys, leading to temporary or sometimes more serious kidney injury.
How does sepsis cause acute kidney injury?
Sepsis is a severe and life-threatening reaction to infection that can affect multiple organs, including the kidneys. During sepsis, blood pressure may fall, and the body releases substances that cause inflammation. This inflammation and reduced blood flow can damage kidney cells or prevent them from working properly. Sepsis is one of the most common causes of AKI in hospitalised patients.
How to differentiate acute kidney injury vs diabetic ketoacidosis?
AKI is a condition characterised by a sudden decline in kidney function, leading to the accumulation of waste products (such as urea and creatinine) and disturbances in fluid and electrolyte balance. Patients may have oliguria (reduced urine output), swelling, fatigue, nausea, and abnormal blood test results showing elevated creatinine and electrolyte imbalances.
Diabetic ketoacidosis (DKA) is an acute complication of diabetes caused by insulin deficiency in the body. It leads to very high blood glucose levels, and the production of acidic substances called ketones, leading to metabolic acidosis. Patients typically present with excessive thirst, frequent urination, vomiting, abdominal pain, fruity-smelling breath, and deep, rapid breathing (Kussmaul respiration).
What are the common symptoms of acute kidney injury?
Common symptoms of AKI can vary depending on how severe the condition is. In many cases, especially early on, there may be no obvious symptoms, and it is detected through blood tests. When symptoms do appear, they may include reduced urine output, swelling in the legs or around the eyes, tiredness, and shortness of breath, confusion, nausea, or chest discomfort. These symptoms happen because the kidneys are not removing waste and extra fluid properly. As waste builds up in the blood and fluid accumulates in the body, different organs can be affected.
What does kidney pain feel like in AKI?
Kidney pain in AKI is not very common. Most people with AKI do not feel direct kidney pain. If pain is present, it is usually felt in the lower back or on the sides, just below the ribs. The pain may feel dull or aching. However, pain is more commonly associated with conditions like kidney stones or kidney infections rather than typical AKI caused by dehydration or low blood pressure.
What is contrast-induced AKI?
Contrast-induced AKI is a type of kidney injury that can occur after receiving contrast dye used in certain imaging tests, such as CT scans or angiography. Contrast dye helps doctors see blood vessels and organs more clearly, but in some people, especially those who already have kidney problems, diabetes, or dehydration, it can temporarily reduce kidney function. This usually happens within a few days after the procedure. Generally, most of the cases are mild and improve with proper hydration, but in rare situations, kidney function may worsen significantly.
How does rhabdomyolysis cause AKI?
Rhabdomyolysis is a condition in which muscle tissue breaks down rapidly, releasing substances such as myoglobin into the bloodstream. Myoglobin is a muscle protein that can be harmful to the kidneys when present in large amounts. When this substance reaches the kidneys, it can block small kidney tubes and cause direct damage to kidney cells. Severe muscle breakdown can lead to dehydration and reduced blood flow to the kidneys. These combined effects can result in acute kidney injury.
What is ICU-associated AKI?
ICU-associated acute kidney injury refers to kidney injury that develops in patients who are admitted to the intensive care unit (ICU). It is common in critically ill patients because they often have severe infections, low blood pressure, major surgery, trauma, or require strong medications. In these situations, the kidneys may receive reduced blood flow, be exposed to inflammation, or be affected by medications that stress kidney function. This is associated with longer hospital stays and higher risk of complications.
What is metabolic acidosis in AKI?
Metabolic acidosis is a condition in which too much acid builds up in the blood. The kidneys normally remove acid from the body and help maintain a healthy acid–base balance. When acute kidney injury occurs, the kidneys cannot remove acid, which can lead to acid accumulation. This may cause symptoms like rapid breathing, tiredness, confusion, or weakness. And in severe cases, it may affect heart function. Treatment focuses on correcting the underlying kidney problem and, if needed, giving medications such as bicarbonate to help neutralize excess acid.
How does obstruction cause postrenal AKI?
Postrenal AKI occurs when there is a blockage in the urinary system that prevents urine from flowing out of the body. This blockage may be caused by kidney stones, an enlarged prostate, tumors, or scarring in the urinary tract. When urine cannot drain properly, pressure builds up inside the kidneys. This pressure reduces their ability to filter blood and remove waste.
What is the most common cause of acute kidney injury?
The most common cause of acute kidney injury is reduced blood flow to the kidneys. This happens due to dehydration, severe infection (sepsis), major blood loss, heart problems, or low blood pressure. When the kidneys do not receive enough blood, they cannot filter waste properly. This “pre-renal” cause accounts for the majority of AKI cases, especially in hospitalised patients.
How does AKI affect electrolyte balance?
Acute kidney injury disrupts the body’s electrolyte balance because the kidneys are responsible for maintaining proper levels of minerals such as potassium, sodium, and phosphate. When kidney function declines, potassium can rise to dangerous levels, which may affect heart rhythm. Sodium levels may become too high or too low, causing confusion or swelling. Fluid retention is also common. These imbalances can develop quickly, requiring close monitoring and timely medical management.
Can UTI cause AKI?
Yes, a urinary tract infection can sometimes lead to acute kidney injury, especially if the infection spreads to the kidneys. When bacteria travel from the lower urinary tract to the kidneys, it can cause a kidney infection known as Pyelonephritis. Severe infections may cause inflammation and damage to kidney tissues, reducing the kidneys’ ability to filter waste from the blood. In elderly patients or those with weakened immunity, the infection can also lead to Sepsis, which can decrease blood flow to the kidneys and result in AKI.
What is AKI Stage 3?
AKI Stage 3 is the most severe stage of acute kidney injury. It occurs when kidney function is critically reduced. In this stage, serum creatinine levels increase to more than three times the normal baseline or rise above 4.0 mg/dL, and urine output may drop to very low levels (less than 0.3 mL/kg/hour for 24 hours) or stop completely for about 12 hours.
Patients in Stage 3 may develop serious complications such as fluid overload, electrolyte imbalance, and toxin buildup in the blood. In severe cases, treatment may require kidney support such as dialysis until kidney function improves.
Can steroids cause AKI?
Steroids (corticosteroids) usually do not directly cause acute kidney injury, but in certain situations, they may contribute to it. Long-term or high-dose steroid use can increase the likelihood of infections, fluid retention, and high blood pressure, which may indirectly affect renal function.
In very rare situations, steroids may worsen existing kidney problems or contribute to complications that lead to AKI. However, steroids are also commonly used in medicine to treat certain kidney diseases, especially inflammatory conditions affecting the kidneys.
When to consult a doctor for Acute Kidney Injury (AKI)?
Consult a doctor for acute kidney injury if symptoms such as a noticeable decrease in urine output, swelling in the legs or around the eyes, or unusual tiredness occur. Early medical evaluation is important because kidney problems may worsen quickly if not treated.
Signs that indicate a need for medical assistance are:
- Passing very little or no urine
- Swelling in the feet, ankles, face, or abdomen
- Persistent nausea or vomiting
- Shortness of breath
- Confusion or unusual drowsiness
- Chest discomfort or irregular heartbeat
- Dark, foamy, or bloody urine
If these symptoms persist, it is best to see an acute kidney injury specialist for an accurate diagnosis and treatment. Seek emergency care immediately if there is severe shortness of breath, chest pain, seizures, extreme weakness, or complete absence of urine, as these may indicate serious complications. A primary care doctor or kidney specialist (nephrologist) can provide the right acute kidney injury treatment to prevent long-term damage.
Share on
Request an appointment
Fill in the appointment form or call us instantly to book a confirmed appointment with our super specialist at 04048486868